Playlist
Show Playlist
Hide Playlist
Acute Mesenteric Ischemia: Epidemiology
-
Emergency Medicine Bord Mesenteric Ischemia.pdf
-
Download Lecture Overview
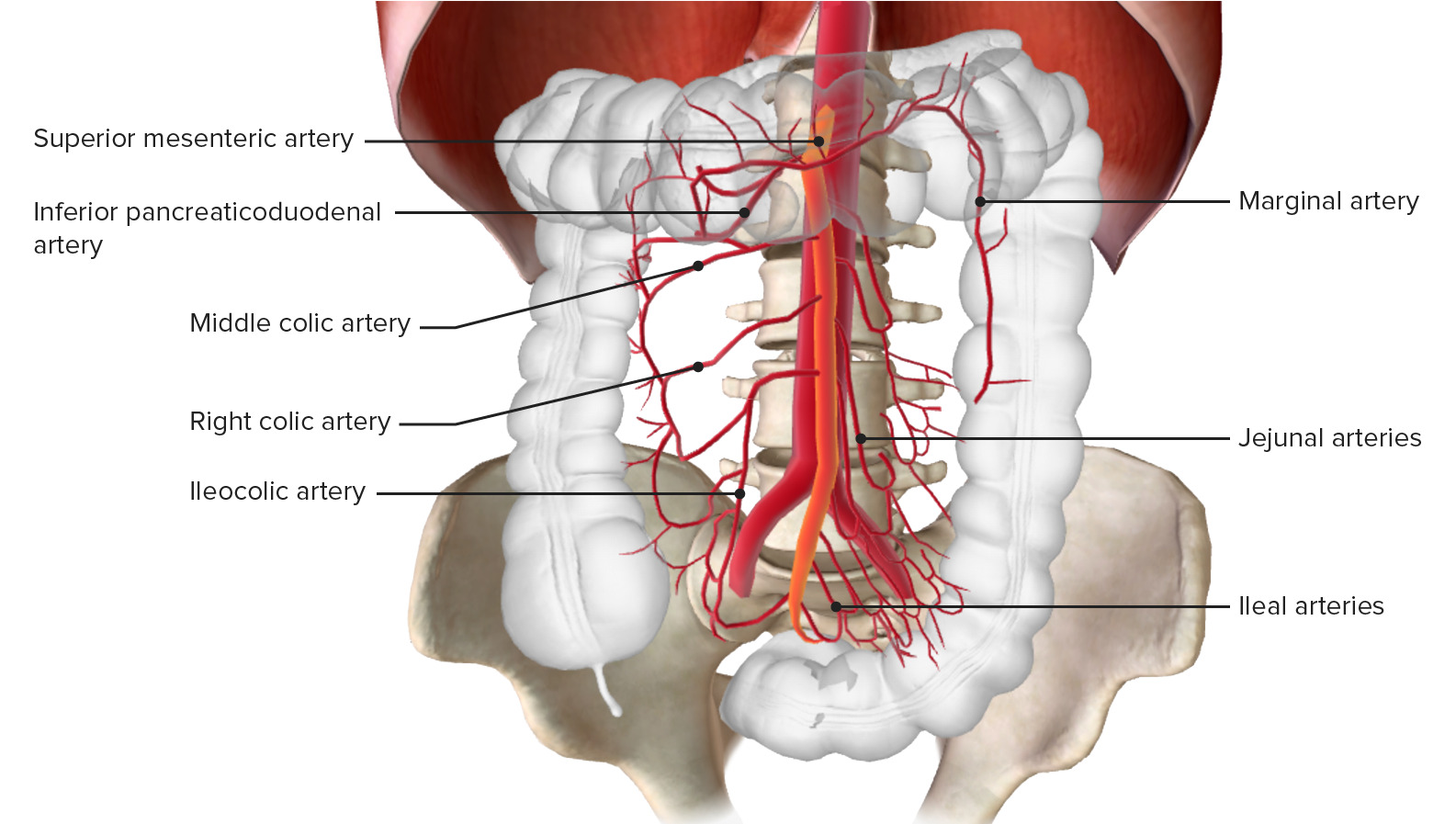
00:01 Now, what are our risk factors? There’s risk factors for myocardial ischemia so if you’ve ever had a heart attack before that puts you at risk for mesenteric arterial embolism, if you have a history of endocarditis, part of the endocarditis that’s attached to the valve can go ahead and cause the clot to go to the mesenteric vessels. 00:23 A ventricular aneurysm can cause a blood clot as well, so if you have an aneurysm in the blood kind of just sits there in that aneurismal component of the ventricle of the heart that can lead to the blood clot going to the vessels; and then atrial dysrhythmias. 00:40 So does the patient have atrial fibrillation which can go ahead and lead to the blood clots going to the mesenteric vessels as well. 00:48 Now, the most frequent vessel involved in mesenteric arterial embolism is the SMA, the superior mesenteric artery. 00:57 Clots, when they go here, they lodge generally distally; and when SMA is affected, the jejunum which is the second portion of the small intestine, is the most commonly affected portion of the small intestine. 01:10 You know it’s important to know that the SMA is the furthest vessel from the collaterals so patients who have a problem with their SMA, you’re not gonna be getting blood flow from lots of other areas, so sometimes if you have an occlusion of another one of the blood vessels, there’s a lot of collateral flow -- there’s a lot of other like backup flow that can help supply those areas but the SMA doesn’t necessarily have that. 01:36 Secondly, we can talk about mesenteric arterial thrombus. 01:41 Now, this is one of the second causes for mesenteric ischemia. 01:45 This is due to atherosclerotic disease so the patient has plaque build up, cholesterol build up in the mesenteric vasculature. 01:53 These are more commonly related to chronic mesenteric ischemia, so while mesenteric arterial embolism is an acute process, that’s a, process where you have a blood clot, it goes to a mesenteric vessel, it causes acute decrease in blood supply, this is more of a chronic problem. 02:14 The occlusion here is more commonly at the proximal superior mesenteric artery rather than the distal in the mesenteric arterial embolus. 02:23 You know, what are the risk factors here? Very similar to risk factors for patients who are having myocardial ischemia, for patients who have underlying heart disease, underlying peripheral arterial disease, diabetes is a big risk factor, chronically elevated blood pressure, smoking, and elevated cholesterol. 02:43 So if a patient has a lot of these risk factors, and risk factors for heart disease, that’s something that’s gonna predispose them to a mesenteric arterial thrombus. 02:54 The third cause here is non-occlusive mesenteric ischemia. 02:59 Non-occlusive mesenteric ischemia is kind of just what it sounds like. 03:02 It’s due to vasospasm of the mesenteric vessels so patients who have a spasm of the vessel, there's not gonna be be a good blood flow that goes through there. 03:15 You know this can result in our current and repetitive injury for those patients cuz it might be a recurring issue so they might have vasospasms that make it better then it make it worse again and then it make it better again. 03:26 You know in this situation it’s different than the prior two things we discussed in the sense there’s nothing actually blocking the vessel, this is non-occlusive. 03:33 The risk factors here are hypoperfusion, so patients who are hypotensive, patients who are septic can have hypoperfusion, they cannot get enough blood flow that’s going to those blood vessels. 03:47 So sepsis, hypovolemia, patients who are very dehydrated, hemorrhagic shock in the situation of trauma or someone who’s had a massive GI bleed and then pancreatitis; is the other condition that can sometimes lead to decrease blood flow in those mesenteric vessels. 04:05 You know, nervous systems activity can sometimes also cause vasospasm to those vessels and primarily these are things that increase the sympathetic nervous system activity. 04:15 So CHF is one, vasopressors -- so sometimes, this is iatrogenic, sometimes this is due to medications that we give people, so if someone comes in and they’re very hypotensive, their blood pressure is low, we give them medicine to support their blood pressure. 04:30 Sometimes those medicine can do too good of a job constructing the vessels and can cause decrease blood flow to the intestines. 04:39 And then cocaine is a elicit drug that can cause increase sympathetic stimulation and primarily would cause vasospasms so it would cause those vessels to clamp down inappropriately. 04:51 And last but not least we have mesenteric venous thrombosis. 04:55 Now this is the least common cause of mesenteric ischemia making up about 5 to 15% of cases. 05:01 Most commonly it involves the super mesenteric vein so this is the problem with the venous system rather than the arterial system. 05:10 Often times there’s an underlying thrombotic disorder or a hypercoagulable state that the patient may or may not know about yet. 05:18 Young women who are on oral conceptive agents especially oral conceptive agents that contain estrogen can predispose to clotting. 05:28 If there is venous stasis so the blood is kinda just sitting around there in the portal hypertension in the portal system that can be a risk factor, and then Virchow’s Triad. 05:39 Virchow’s triad is basically immobility, damage to the blood vessel and that can predispose to clotting as well.
About the Lecture
The lecture Acute Mesenteric Ischemia: Epidemiology by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
Which vessel is most frequently involved in mesenteric arterial embolism?
- Superior mesenteric artery
- Middle colic artery
- Right colic artery
- Ileocolic artery
- Superior mesenteric vein
What is the pathophysiology behind non-occlusive mesenteric ischemia?
- Vasospasm of mesenteric vessels
- Atherosclerosis of vessels
- Thrombosis of vessels
- Hypercoagulable state
- Idiopathic cause
Which vessel is most commonly affected in mesenteric venous thrombosis?
- Superior mesenteric vein
- Inferior mesenteric vein
- Left colic vein
- Splenic vein
- Right gastroepiploic vein
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |