Playlist
Show Playlist
Hide Playlist
Acute Mesenteric Ischemia
-
Emergency Medicine Bord Mesenteric Ischemia.pdf
-
Download Lecture Overview
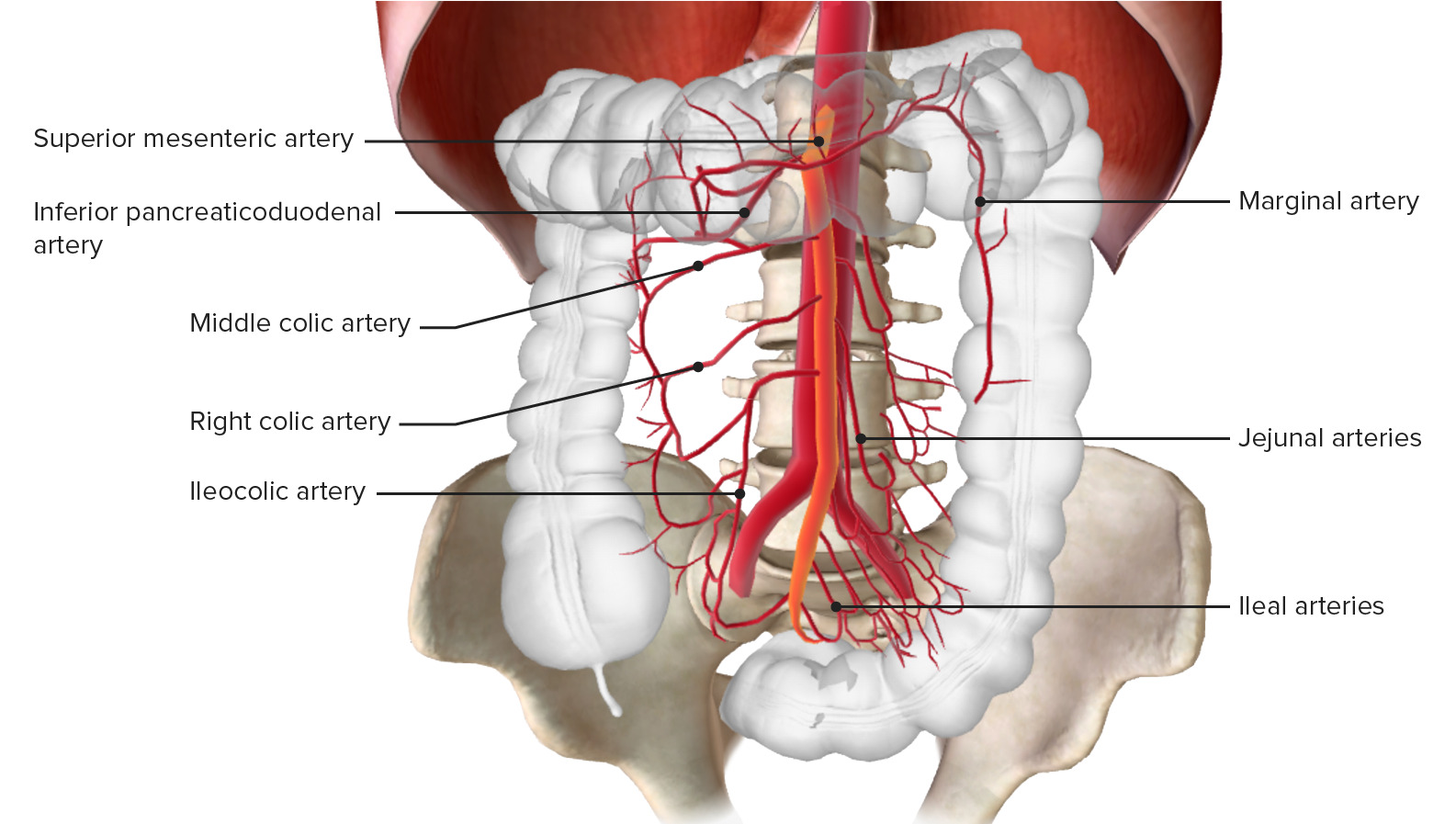
00:02 Hi. We’re gonna be talking about mesenteric ischemia. 00:05 Before we get started, we’re just gonna take a quick moment to review the anatomy. 00:09 So the mesentery which are your intestines, your small intestine and your large intestine, are all supplied by blood vessels that are offshoots from the aorta. 00:19 What happens in mesenteric ischemia is that there is something that decreases that blood flow. 00:25 There’s either a blood clot there or there is a low flow through those vessels, and we’ll be exploring that further. 00:30 And when you have that decreased blood flow, there’s a high metabolic demand of those intestines. 00:37 Decreased blood flow can lead to mucosal sloughing in the first three hours, and then in the first six hours, it can lead to necrosis and bowel necrosis is something that can be very bad and dangerous for a patient. 00:50 So this is a diagnosis where you wanna make sure that you’re thinking about it, you’re considering this in the appropriate patient population, and that you’re keeping this diagnosis in mind. 01:02 There’s four different pathophysiologic processes here and we’re gonna talk a little bit about each one of these. 01:10 So the first is mesenteric arterial embolism. 01:13 This is the most common making up 50% of the cases of mesenteric ischemia. 01:19 There’s also mesenteric arterial thrombosis, non-occlusive mesenteric ischemia, and then mesenteric venous thrombosis. 01:28 Like I said, mesenteric arterial embolism represents 50% of these cases and is the most common cause of mesenteric ischemia. 01:38 The median age for presentation of this is 70 years of age and a majority of patients, so two thirds of these patients are gonna be females. 01:47 Most of the time, the embolus comes from the heart. 01:52 So the emboli are cardiac in origin and that’s oftentimes due to an atrial dysrhythmia, so due to the fact that the patient has atrial fibrillation or something that causes the blood to sit around the heart. 02:03 So an atrial fibrillation is kind of one of the classic examples and in atrial fibrillation, the atria are doing what we call fibrillating. 02:11 So they’re basically just sitting there and they’re not effectively pumping the blood out of the heart. 02:15 And as the blood sits there, it has the tendency to cause clots. 02:19 This is one of the reasons that many patients who have atrial fibrillation are on anticoagulation because the blood clot that forms in the heart can go to the intestines, it can also go to the brain and cause a stroke, so this is one of the reasons for anticoagulating those patients who have that condition. 02:36 Sometimes, patients may not be compliant with their treatment or they may not recognize that they have atrial fibrillation. 02:43 So those might be reasons that patients may not be on anticoagulation.
About the Lecture
The lecture Acute Mesenteric Ischemia by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
What is the most common pathophysiologic process involved in mesenteric ischemia?
- Mesenteric arterial embolism
- Mesenteric arterial thrombosis
- Non-occlusive mesenteric ischemia
- Mesenteric venous thrombosis
- Idiopathic ischemia
What is the most common source of emboli in mesenteric arterial embolism?
- Heart
- Lungs
- DVT
- Liver
- Carotid
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
What a great lecturer. Very confident and clear to the point.
Very clear and to the point with the pertinent information.