Playlist
Show Playlist
Hide Playlist
Acute Mesenteric Ischemia: Diagnosis
-
Emergency Medicine Bord Mesenteric Ischemia.pdf
-
Download Lecture Overview
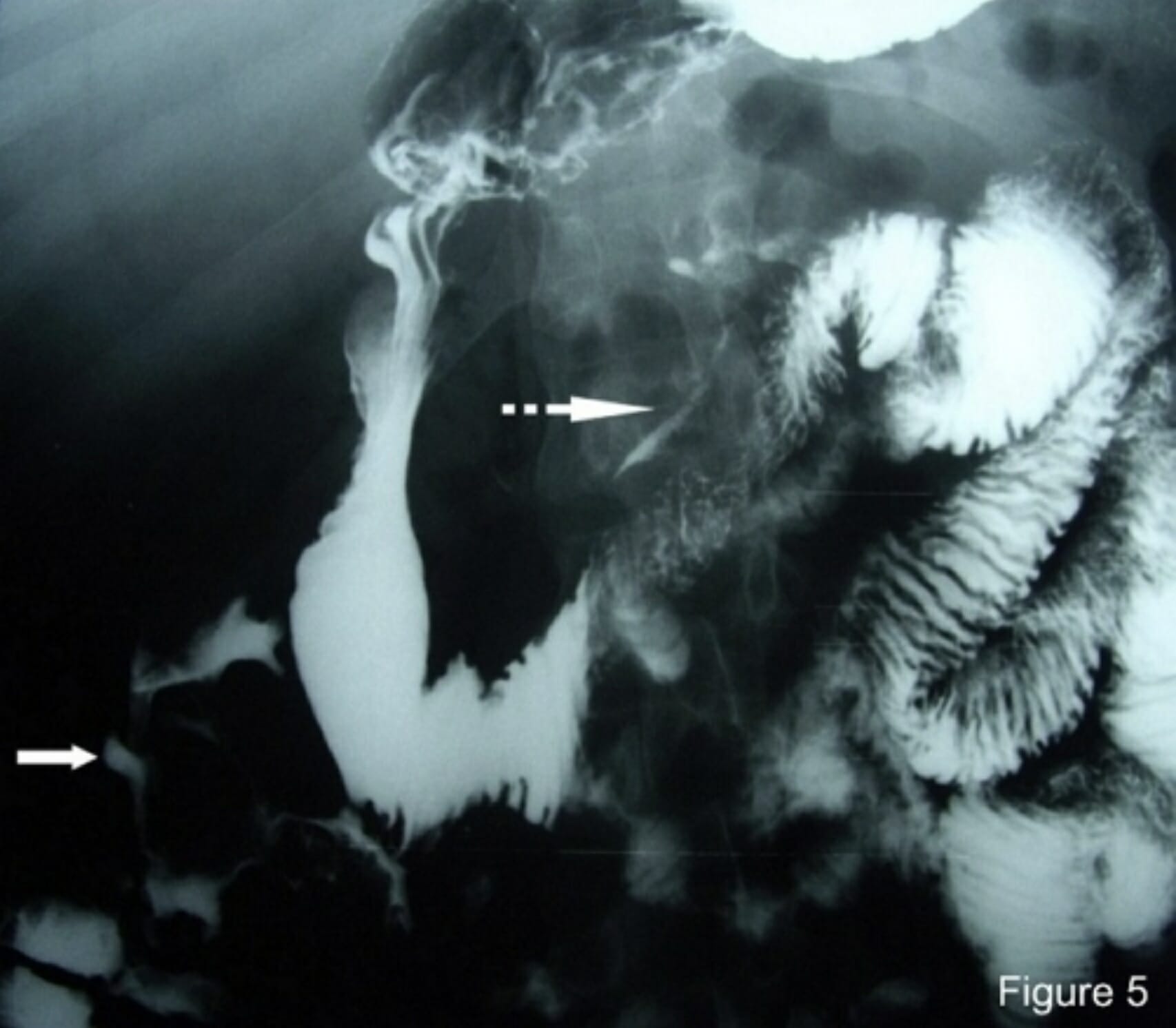
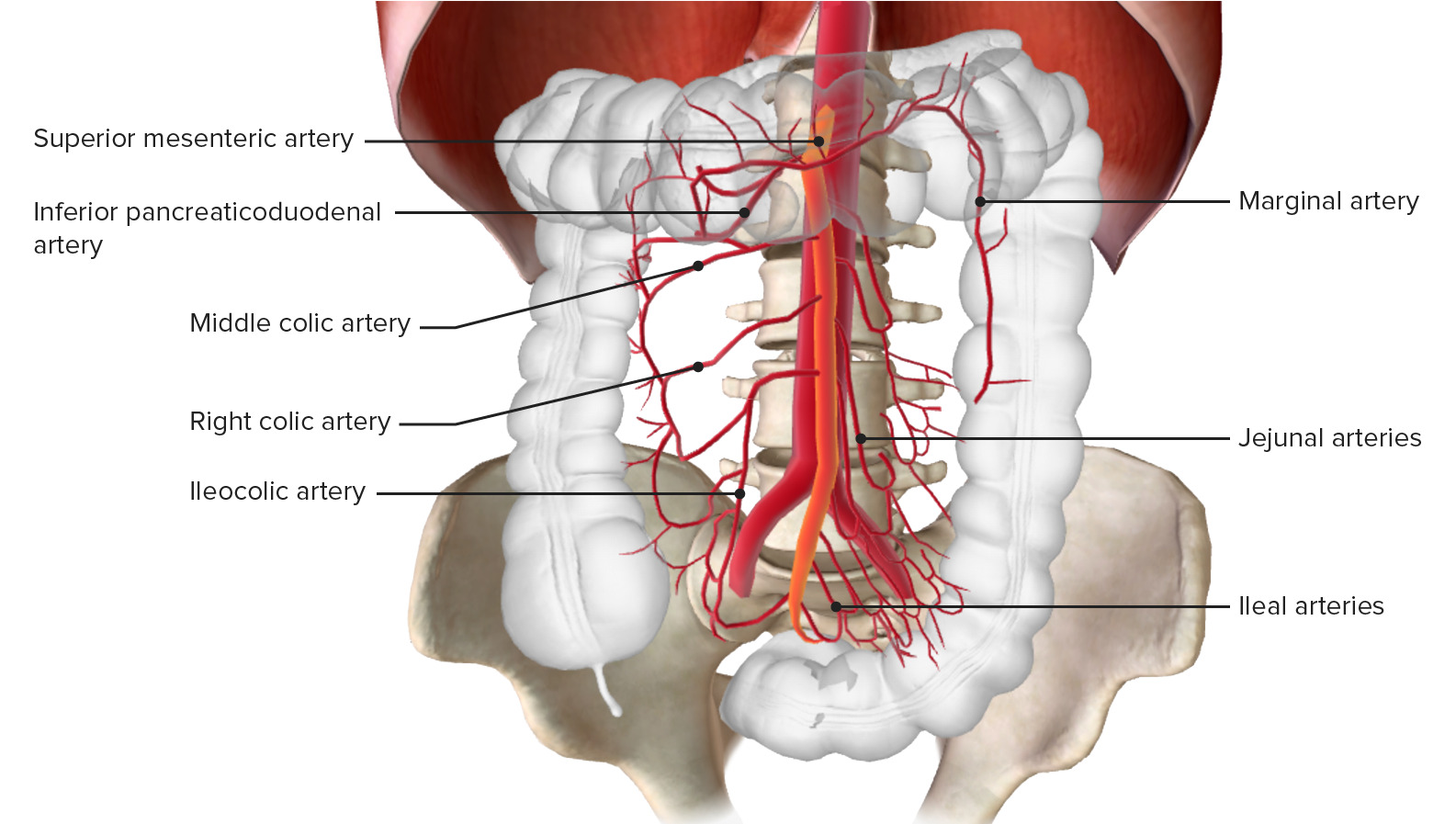
00:01 How do we diagnose it? No lab tests really have been shown to be very specific for the diagnosis. 00:07 There’s nothing where if your labs reveal something, that that will automatically mean that there is mesenteric ischemia present. 00:13 The lactic acid level may be helpful. 00:16 You can check serial levels especially in the setting of ischemia and prolonged ischemia, and ischemia that keeps going on, those lactic acid levels are gonna keep increasing, so they’re gonna keep rising. 00:27 If you have a very high suspicion for this diagnosis, go ahead and check preoperative labs. 00:33 So that means adding on additionally like a type and screen or a type and cross. 00:37 If you think your patient’s going to the OR, checking coagulation studies again if you think your patient’s going to the operating room. 00:44 And then, you wanna get an EKG and your EKG is mainly looking for dysrhythmia so you’re looking to see if there is any abnormality in the rhythm. 00:53 If it’s atrial fibrillation, you’re looking to see if it’s normal sinus rhythm, and that can be very helpful again in figuring out if there is concern for an embolic event. 01:02 What additional testing can we get? So we’re gonna wanna start working on getting some imaging. 01:08 A plain film x-ray can be an okay starting point here. 01:12 In advanced disease, so as the disease process again goes on, it may show something called thumb printing which is evidence that there has been decreased blood flow to the bowel wall, or potentially as the process goes on, you can maybe see air in the bowel wall. 01:28 Ultrasound is specific but not super sensitive for the diagnosis. 01:33 Ultrasound has the benefit of being easy to obtain, it’s generally relatively cheap, but potentially, won’t be super helpful in making this diagnosis. 01:45 Moving along to the tests that are really gonna help us out the most. 01:50 So there’s two options here. 01:52 One is a mesenteric angiogram. 01:54 The advantage here is that you can treat and you can diagnose at the same time. 01:58 So if when you’re doing the study you see or the radiologist sees that there’s a blockage in a specific location, they can go in and they can help dissolve the clot, or suck out the clot, or do something to help treat it. 02:11 CT angiography has the advantage that it’s widely available. 02:15 This is basically a CT scan you’re getting that’s gonna be timed with IV contrast to be able to light up or visualize the vessels in the abdomen. 02:26 This is a pretty widely available study. 02:28 It’s something that you can obtain at almost every institution and it can give you your diagnosis. 02:34 Now, the cons with these studies for the mesenteric angiogram is that it requires IV dye. 02:40 So if your patient does in fact have renal insufficiency or an allergy to IV dye, that may be a limitation. 02:46 It’s also not widely available. 02:48 So this requires a special interventional radiologist to perform this test and that’s not gonna be available at every institution. 02:56 That’s not gonna be available at every location. 02:58 So that’s something else that you wanna make sure that you keep in mind. 03:02 The cons for CT angiography again, it does require IV dye as well. 03:07 So we’ll have similar limitations to the angiogram. 03:10 And you’re unable to treat concomitantly. 03:13 So let’s say you do the CT angiography and you see that there’s a blockage. 03:18 There’s no way for you to go in and intervene on that blockage at the same time. 03:24 This is a picture of a CT angiography that’s showing a blockage of a vessel. 03:30 So the bright white color or that kind of brighter white color or greyish color should indicate that there is blood flow going through that. 03:38 Now, the green arrow here points to the area where there is a blockage in the vessel. 03:43 That’s an area where the vessel should be getting blood flow to it distally and it should be lighting up with contrast but it’s not lighting up with contrast.
About the Lecture
The lecture Acute Mesenteric Ischemia: Diagnosis by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
What imaging modality has the advantage of both being able to diagnose and treat mesenteric ischemia at the same time?
- Mesenteric angiogram
- CT angiogram
- Ultrasound
- Plain film x-ray
- MRI
What is the purpose of requesting an EKG when evaluating patients with suspected mesenteric ischemia?
- To check for dysrhythmia that may suggest an embolic event
- To check for heart rate
- To check for bradycardia
- To check for ventricular enlargement
- To check for ventricular tachycardia
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |