Playlist
Show Playlist
Hide Playlist
Medium Vessel Vasculitides: Polyarteritis Nodosa
-
I Rheumatology 05 Vasculitis.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
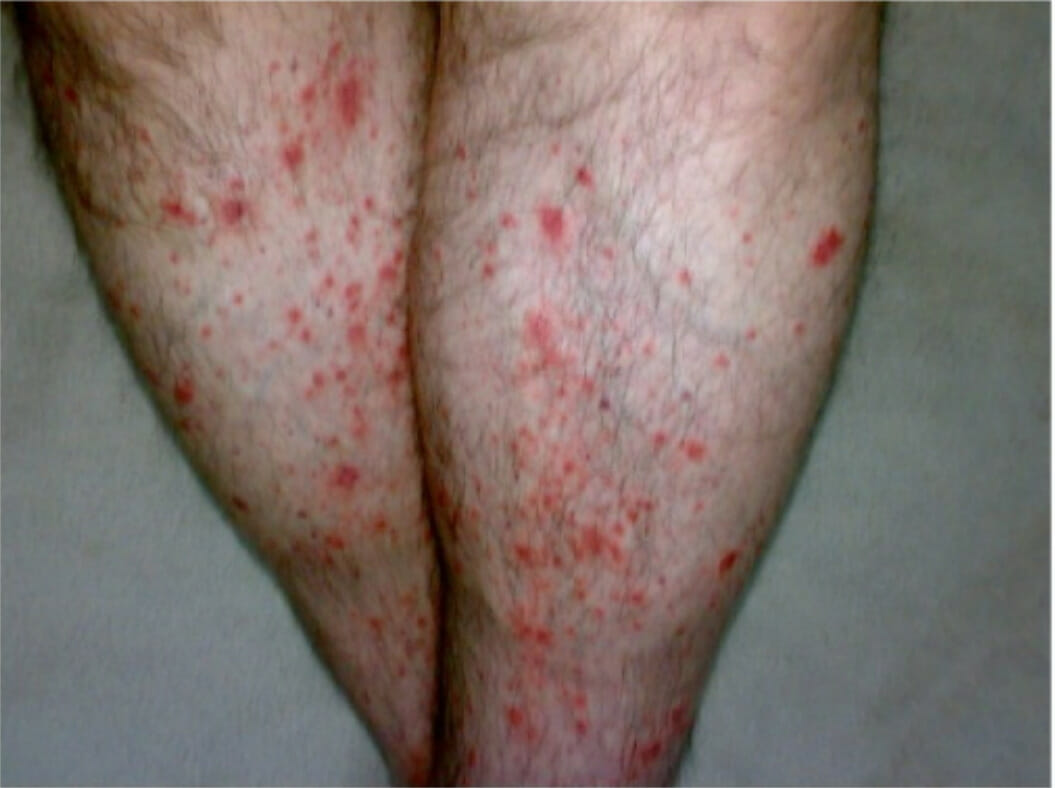
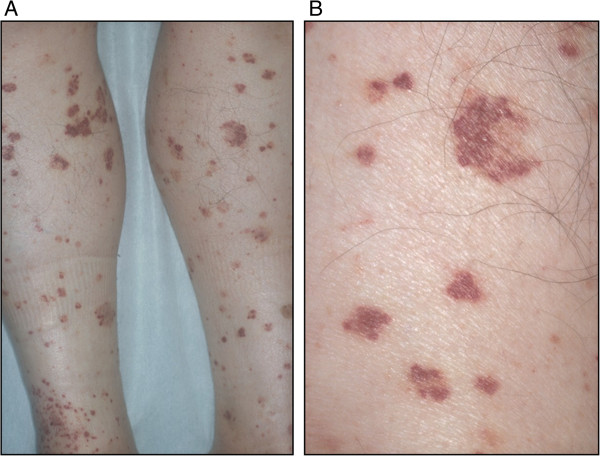
00:01 From here, we’re going to move on to our next organization of our vasculitides and these are medium vessel diseases. 00:10 Now the medium vessel vasculitides I want you to, once again, pay attention to the fact that does it always have to be medium blood vessel? Not necessarily. It could be a small vessel. 00:20 Now I don’t want you to be contained in that aspect, but you’re going to be paying attention to who’s your patient walking through the door? With polyarteritis nodosa, most commonly, the patient is presenting with abdominal pain, and that’s because the mesenteric arteries are undergoing inflammation. 00:38 In addition, there also might be issues with hematuria, and that’s because the renal blood vessels are being affected. 00:45 Also, the patient may have maybe foot drop, in other words, mononeuritis multiplex. What’s that mean? Well if its foot drop, maybe the common peroneal nerve has been affected resulting in foot drop or maybe wrist drop because of radial never issues. 01:02 So you have 1 nerve, mononeuritis, in multiple systems called mononeuritis multiplex. 01:12 Now in terms of, once again, the organs that you’re paying attention to mesenteric and the renal. 01:18 Could it be elsewhere? Absolutely. The patient presents with fever remember, -itis, and wheneve you see the term –itis, you can pretty much assume that with that inflammatory process that the patient is going to present with fever. 01:32 That’s important. 01:34 Diagnostic: What are you going to do? Gold standard is biopsy here as well on necrosis. 01:39 The type of inflammation that you’re going to find is going to be, what’s known as, transmural. That’s important. 01:47 Look for that description. 01:49 Number 2: Mesenteric blood vessel; thus, the patient presenting with abdominal pain and maybe GI bleeding. Correct? Ischemia. 01:57 Number 2: On, what’s known as, your angiography. 02:01 Alright? So let’s say that you do magnetic resonant angiography I’ll show you a picture coming up—in which, you’re going to be looking for innumerable microaneurysms. 02:12 Now with those microaneurysms taking place in the renal region, no doubt, that there’s a possibility of hematuria taking place. 02:19 Now be careful. Polyarteritis nodosa, especially with a fever and such, could be—could be confused with infectious vasculitis, but one has nothing to do with the other. 02:29 Management: Steroids. Well, most of these cases, we’re thinking about steroids, maybe cyclophosphamide for organs that are threatened by the disease. 02:40 There is approximately 30%, I repeat—there’s an approximate 30% association with hepatitis B. 02:48 So if you’re able to properly, properly manage a patient with polyarteritis nodosa, then there’s every possibility that hepatitis B, and then symptoms and such, might also subside; but if there’s hepatitis B then you’re thinking about drugs to combat this including lamivudine, [Inaudible 00:03:05] steroids, and plasmapheresis obviously to address the polyarteritis nodosa. Keep that in mind. That’s important in terms [Inaudible 00:03:11]. 03:15 Now in this picture that I’m going to show you in a second, is the renal blood vessel of polyarteritis nodosa, in which, what do you find? Innumerable microaneurysms is what the [Inaudible 00:03:28], the flock of arrows that you’re seeing here are pointing to little bitty aneurysms that are taking place in the picture of angiography. 03:40 Thus, the patient presenting with hematuria. 03:43 This is for polyarteritis nodosa. 03:47 Continue our discussion of medium vessel disease. 03:51 In polyarteritis nodosa, that’s a patient that is a young adult, maybe 20’s and such, polyarteritis nodosa is to an adult or a young adult, as Kawasaki is to a child. 04:07 So now, some of the symptomology that you find with Kawasaki, you could perhaps find with polyarteritis nodosa; however, I told you to focus upon the most common symptoms. 04:21 And polyarteritis nodosa, you as a doctor, he signs that you would see, obviously would be the abdominal pain or the patient will complain of abdominal pain. 04:31 You might notice GI bleed and hematuria. 04:35 In Kawasaki, sure, that might also occur; however, in Kawasaki, this is what you’re going to be paying attention to. 04:42 Number 1: That child—that child must have a fever. 04:48 That child, when you observed the tongue of this child, it looks like the peel of a strawberry. 04:55 So strawberry tongue in pathology is going to be Kawasaki whereas strawberry tongue in microbiology could be something like Scarlet fever. 05:05 So now we have fever and now we have the strawberry tongue. 05:08 Next, you’re going to be looking for the rash, and that rash is called desquamation type of rash, maybe perhaps on the palms and maybe on the soles of the foot. 05:19 That rash is important. That fever is a must. You cannot even diagnose Kawasaki without the fever. Remember, this is of vasculitis. 05:28 It’s an anti-endothelial antibody disease, isn’t it? Most feared, however, is the fact that it is the most common acquired cause of coronary arterial disease in a child. What does acquired mean? Not genetic and not congenital. 05:46 And also, you’re going to be looking for that cervical lymphadenopathy. 05:50 So things that you’re looking for here, let me recap—you have the fever; you have the desquamating rash; you have the tongue, the mucous membrane here looks like the peel of a strawberry, literally. 06:00 If you take a look at the eyes, both bilateral in this child, they are red injected—so bilateral injected conjunctivitis. 06:09 And we talked about the coronary arteries could be affected, and the child unfortunately, could be suffering from cardiac disease. 06:16 Diagnostically, what are you looking for? Fever, fever, fever must be seen more than 5 days, and 4 of the 5 should be found—here we go: First beginning with that tongue that I was talking to you about, mucous membrane, but in addition to the mucous membrane of the tongue, you have the conjunctiva, bilateral conjunctivitis. 06:37 The strawberry tongue, which is the changes in the orad that rash that I was referring to known as a desquamating rash found in the palms and soles, and cervical lymphadenopathy. 06:50 You must find 4 of the 5, and they will give it to you—they have to, so that you can diagnose properly your patient with Kawasaki. 06:57 Management: Now this gets really interesting which is IV immunoglobulin, as your preferred method of treatment, you must also have aspirin in the mix. Keep that in mind. 07:08 This then reduces, especially the coronary manifestations, in this child with Kawasaki. 07:13 These are the big points of Kawasaki.
About the Lecture
The lecture Medium Vessel Vasculitides: Polyarteritis Nodosa by Carlo Raj, MD is from the course Vasculitis: Basic Principles with Carlo Raj. It contains the following chapters:
- Medium Vessel Vasculitides - Polyarteritis Nodosa
- Medium Vessel Vasculitides - Kawasaki Disease
Included Quiz Questions
A 65-year-old man has had fatigue, weight loss, weakness, fever, arthralgias, and abdominal pain for several weeks. Further investigation shows skin lesions, hypertension, hematuria, and chronic kidney disease. An angiography reveals microaneurysms of blood vessels in the renal circulation. What is the most likely diagnosis?
- Polyarteritis nodosa
- Takayasu arteritis
- Giant cell arteritis
- Kawasaki disease
- Granulomatosis with polyangiitis
What virus is associated with about 30% of patients who have polyarteritis nodosa?
- Hepatitis B
- Borrelia burgdorferi
- Human immunodeficiency virus
- Epstein-Barr virus
- Cytomegalovirus
A 5-year-old boy presents with 5 days of fever and bilateral conjunctival injection, strawberry tongue, edema of hands, and cervical lymphadenopathy. What is the most likely diagnosis?
- Kawasaki disease
- Polyarteritis nodosa
- Dermatitis
- Giant-cell arteritis
- Takayasu arteritis
What organ may be affected as a complication of Kawasaki disease in children?
- Heart
- Lungs
- Kidneys
- Brain
- Liver
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Carlo Raj, make easy everything, I appreciate that. Thankss ss