Playlist
Show Playlist
Hide Playlist
Latent Syphilis, Tertiary Syphilis, Syphilitic Meningitis & Meningovascular Syphilis
-
Slides Syphilis InfectiousDiseases.pdf
-
Reference List Infectious Diseases.pdf
-
Download Lecture Overview
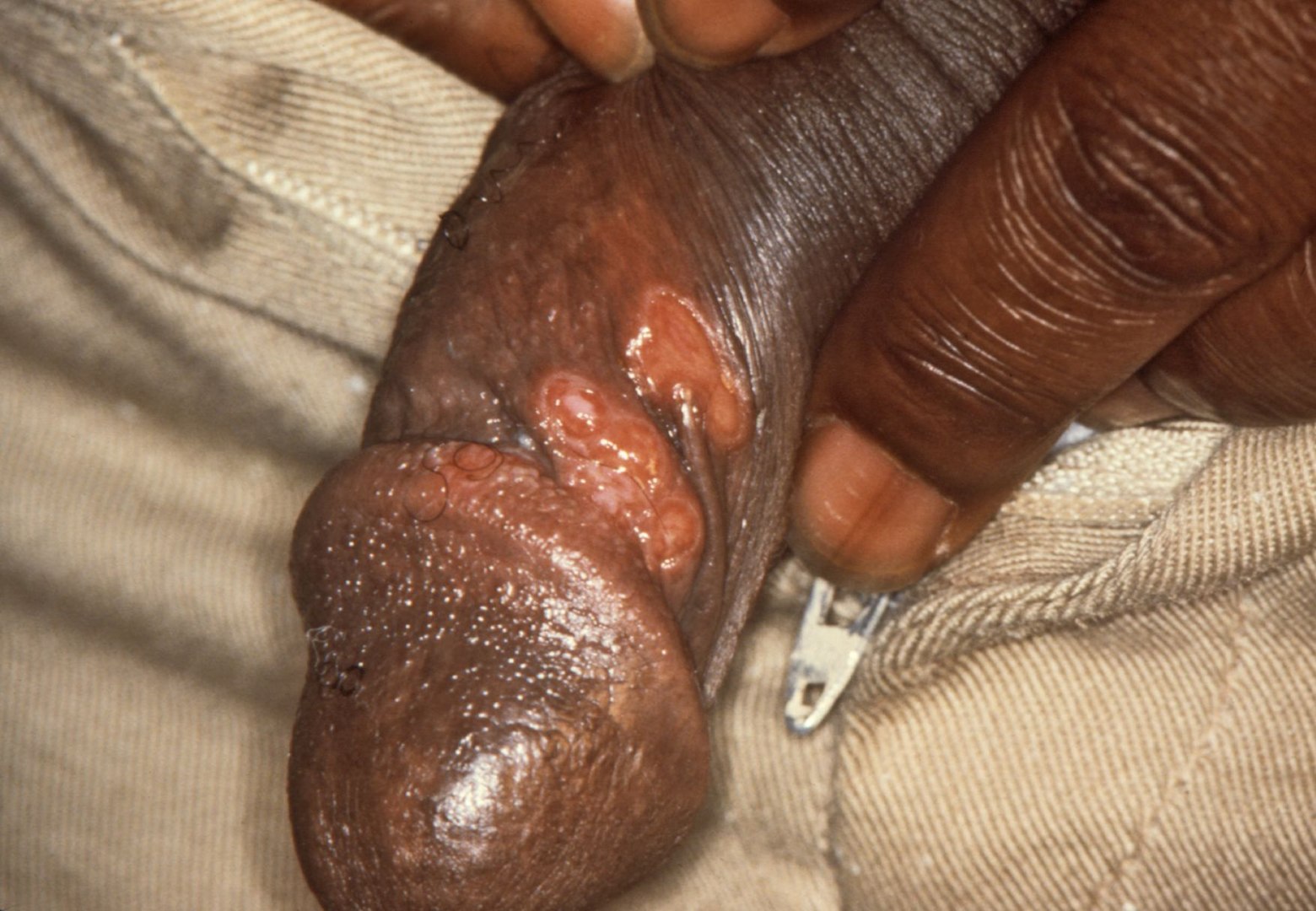
00:01 Then we come to, what I would say, is the majority of patients. 00:06 They don't remember having a chancre, and they've got a positive serologic test for syphilis. 00:14 But they have no recollection of any illness, and so they have no clinical manifestations. 00:21 But the point that this disease is not quiescent. 00:27 There's something going on. 00:29 So all they've got to show for it is a positive serologic test for syphilis. 00:34 Here we're showing you the classic positive rapid plasma reagin or RPR. 00:42 Furthermore, the disease can relapse, and when it relapses with inadequate therapy, it is also possible to transmit the disease because these lesions are highly contagious. 01:01 It's less florid than secondary syphilis. 01:04 You find the mouth and the genital areas affected most frequently, and sometimes the lesions are sort of rounded or annular. 01:17 And then the worst possible manifestation and these are obviously old photographs, are the lesions of tertiary syphilis, which is a slowly progressive destructive inflammatory process. 01:33 It can involve any organ in the body and usually doesn't occur till at least 5 but up to 30 plus years after the initial infection. 01:44 So as I mentioned, this disease is not quiescent - it's ongoing. 01:54 So let's talk for a minute about neurosyphilis, and first talk about asymptomatic neurosyphilis. 02:02 That can be expected in about 10% of individuals who contract syphilis in the first place. 02:12 And so they're asymptomic, they have a positive serology, and they often undergo analysis of the cerebrospinal fluid because of their positive serology. 02:28 What's found is a pleocytosis -- a mixture of round cells and neutrophils, an elevated protein in almost everybody, and a positive CSF VDRL. 02:47 But they have no neurologic signs or symptoms. 02:52 So they usually have one or more of those findings in the CSF, but they have no neurologic findings of any kind, no symptoms and no signs. 03:03 Now the ones who become symptomatic, all of them had preceding asymptomatic neurosyphilis. 03:12 So if a patient presents with asymptomatic neurosyphilis unless you treat them, they're going very likely to develop symptomatic neurosyphilis. 03:30 And that brings us to a discussion of syphilitic meningitis. 03:35 About 50% or more recall having had a chancre or some kind of rash that was consistent with secondary syphilis, or they may have had both. 03:47 The classic findings are signs of increased intracranial pressure such as nausea, vomiting, headache. 03:55 And sometimes the vomiting is projectile, sort of effortless vomiting. 04:02 That's a sign of increased intracranial pressure. 04:06 Or they may have acute hydrocephalus without any focal signs. 04:11 And some patients may have meningitis and it tends to involve the meninges of the vertex of the top of the head. 04:20 Many of these patients will present for the first time with a seizure, or with a focal neurologic deficit, such as hemiplegia, aphasia, or some altered consciousness. 04:34 Syphilis can also infect the base of the brain where the cranial nerves are, and give craniel nerve dysfunction. 04:41 For example, III, VI, VII, and VIII can be infected. 04:45 And it can be unilateral or bilateral in nature. 04:49 Now meningovascular syphilis implies involvement of the blood vessels. 04:55 And so when you involve the blood vessels, sometimes you get clots. 05:02 And when these blood vessels are occluded, you get stroke. 05:09 Now this usually occurs later than most manifestations of neurosyphilis. 05:15 And so what happens because the middle celebral artery and its tributaries are involved, you get a contralateral hemiparesis, you may get homonymous hemianopsia or aphasia. 05:34 And a little pearl is, young people don't get strokes. 05:39 So if a physician encounters stroke in a very young person who's had no history of hypertension or any other predisposing factor, you ought to think of syphilis as one of the causes of that stroke.
About the Lecture
The lecture Latent Syphilis, Tertiary Syphilis, Syphilitic Meningitis & Meningovascular Syphilis by John Fisher, MD is from the course Genital and Sexually Transmitted Infections. It contains the following chapters:
- Latent Syphilis
- Tertiary Syphilis
- Neurosyphilis
- Syphiltic Meningitis
- Meningovascular Syphilis
Included Quiz Questions
A 32-year-old HIV positive male with no prior history of hypertension or diabetes presents with new sudden onset hemiparesis. If this is due to meningovascular syphilis, which of the following is the most characteristic finding on cerebrospinal fluid analysis?
- Pleocytosis and elevated protein
- Pleocytosis and elevated glucose
- Normal white cell count and decreased glucose
- Pleocytosis and decreased protein
- A non-reactive venereal disease research laboratory test
Which of the following statements regarding latent syphilis is MOST ACCURATE?
- It is asymptomatic.
- Serologic testing is non-reactive.
- The disease is quiescent.
- Most patients are aware of their primary infection.
- Painless ulcers persist through the latent phase.
Gummatous syphilis is characteristic of which of the following types of syphilis?
- Tertiary syphilis
- Primary syphilis
- Secondary syphilis
- Latent syphilis
- Gummatous syphilis occurs in any type of syphilis.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
He is a good educator.voice is so clear and not too fast or too slow.Best wishes sir.
Really thorough lectures. Helpful pathophysiology and lots of helpful pictures. I wish every other lecture from other speakers could be like this! Thanks!