Playlist
Show Playlist
Hide Playlist
Hypertrophic Obstructive Cardiomyopathy (HOCM)
-
Slides Obstructive heart disease and detour defects.pdf
-
Reference List Pediatric Nursing.pdf
-
Download Lecture Overview
00:01
Moving on to the next type of obstructive heart disease -
and this one is another one that can present in adulthood -
is hypertrophic obstructive cardiomyopathy or HOCM.
00:16
This is also called subaortic stenosis.
00:20
In this case, there is a bulge in the septum -
and you can see this on the right side of the slide here in the green area -
this bulging septum, which can cause an obstruction of blood
coming out of the left ventricle.
00:36
Usually, it's asymptopmatic.
00:38
They've got this bulge, not much is going on.
00:42
But if this patient is in a situation of, for example, exercise
or some situation where they have increased blood return on the right side,
they can get in trouble.
00:53
Basically, what happens is that blood comes back up to the right side,
the pressures increase on that right side
because of the pumping action of the legs,
and that causes that bulge to bend over into left ventricle.
01:09
Now, the blood coming out of the left ventricle is truly obstructed.
01:14
Two things are important.
01:16
One, blood supply to the brain is important,
and within seconds, this patient can lose consciousness.
01:22
But also remember, the coronary arteries are coming off the base root of that aorta.
01:28
Now, this patient is not having coronary perfusion
and the patient will have an acute myocardial infarction or sudden death.
01:36
This is a condition that can present with sudden death during exercise.
01:43
However, when looking at patients as a whole, it turns out that most patients who die suddenly
actually don't die during exercise, but rather at rest. The reason for this is unclear.
01:54
This disease happens very uncommonly.
01:57
One in 500 people walking down the street have this condition.
02:01
Many don't know they have it.
02:04
It's primarily a genetic condition
and there's a long list of genes that can result in it.
02:09
But most often, it's asymptomatic.
02:12
In fact in the elderly, in autopsy,
you can frequently find this and say,
"Oh, look, this guy lived his whole life
with obstrutive cardiomyopathy and nobody knew."
The challenge is it can also result in heart failure.
02:27
In severe cases, this often happens in their 30s.
02:30
In very severe cases, it can even happen in infancy.
02:35
The problem with this condition is the physical exam can be normal.
02:40
There may not be a murmur, or there's a benign sounding murmur,
which many people get, which is just a general flow murmur.
02:49
You may hear that systolic murmur - it's going to be low-pitched.
02:53
If it's severe, you'll certainly recognize the heart failure on exam
with rales and congestive heart failure.
03:01
The challenge with diagnosing this condition is that,
EKG abnormalities are seen,
but EKGs themselves have high false positive rates.
03:13
So universal screening is right now not recommended and is fairly controversial.
03:20
People have asked,
"Maybe we should routinely screen all athletes with EKGs
because we would hate to have an athlete die
of hypertropic obstructive cardiomyopathy
when you could have made the diagnosis and known they had the condition."
There's some famous athletes who died on the court of basketball with this condition.
03:39
The problem is that because of the false positive rate,
which is so high in EKGs - upwards of 5-10 percent -
there would be an enormous number of echocardiograms done
for the vast majority of people who are normal.
03:54
If you suspect this disease in a patient -
let's say you happen to get an EKG and see an abnormality,
or you hear a suspicious murmur -
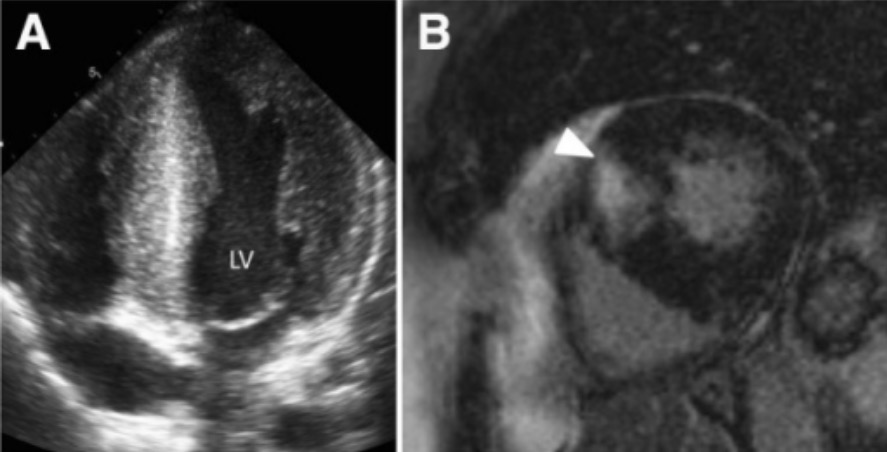
the best way to make the diagnosis is certainly through an echocardiogram.
04:09
MRI may be helpful for more accurate assessment of muscle movement
to really understand what's going on,
but it's probably not the best screening option
mostly because of expense and time.
04:22
There's no therapy for asymptomatic individuals.
04:26
People with this condition, remember,
the majority will have their whole lives with it.
04:31
Patients with heart failure tend to respond to medical therapy,
or a septal myectomy, where they remove some of that cardiac tissue.
04:40
An ICD implantation is generally indicated.
04:45
These patients will have an internal device
that's going to shock them out of an abnormal rhythm should something bad happen.
04:53
In infants with the disease, who are very severe,
they may have metabolic disease or other causes of cardiomyopathies,
such as infection that are driving this.
05:03
Mortality overall for all the patients with this problem
is about 1 percent per year of life.
05:09
But if they make it into adulthood,
prognosis is usually excellent.
05:14
For relatives or children of this condition,
remember in most cases, it's genetic -
screening echos are indicated.
05:23
If you have this condition,
your child should probably get screened for it as well.
About the Lecture
The lecture Hypertrophic Obstructive Cardiomyopathy (HOCM) by Brian Alverson, MD is from the course Pediatric Cardiology. It contains the following chapters:
- Pathology
- Clinical Presentation
- Diagnosis
- Management
Included Quiz Questions
Which of the following is TRUE about hypertrophic obstructive cardiomyopathy (HOCM)?
- There is no therapy for asymptomatic patients
- All athletes are screened with an ECG.
- It occurs in 1:10,000 patients presenting to the primary care physician.
- Most often it presents with unexplained dizziness and syncope.
- Death most commonly occurs in infancy.
You suspect an athlete to have hypertrophic obstructive cardiomyopathy. Which of the following tests would help you confirm the diagnosis?
- Echocardiography
- Electrocardiography
- Chest X-ray
- Cardiac catheterization
- Carotid duplex ultrasound
What is the approximate frequency of hypertrophic obstructive cardiomyopathy in the general adult population?
- 1:500
- 1:100
- 1:200
- 1:1000
- 1:10
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Excellent lecture as usual. I did not know the frequency in the general population was so high. Thank you!