Playlist
Show Playlist
Hide Playlist
Hyperlipidemia
-
Slides Atherosclerosis Cardiovascular Pathology.pdf
-
Download Lecture Overview
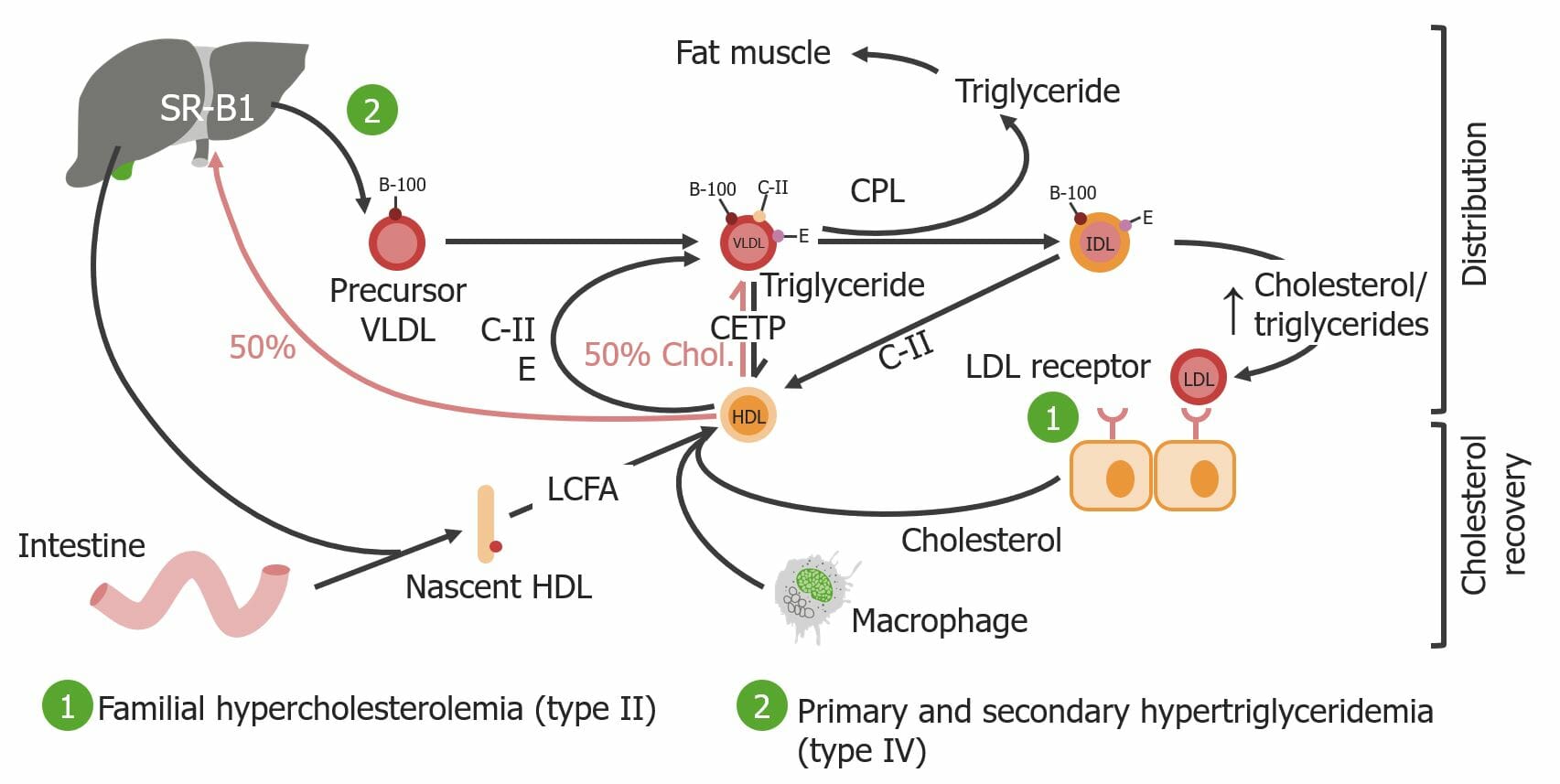
00:00 So to begin at the top, and here, I want you to understand this to, what's going on in this schematic, so that you can clearly see as to what is the normal pathophys and biochemistry of the lipid that we're going to consume, from our mouth, and it's making a way, all way over to the liver. Okay? So, here, let's say that you just had a fatty meal, you just had a bratwurst, you just had a burger from McDonald’s. 00:30 So that means that the fatty meal -- I made a stereotype, but there you have it. 00:35 So now you just ate a fatty meal. 00:37 In terms of effective digestion of your lipid, it begins in the duodenum. 00:41 Is that clear? And the gall bladder contains what? It contains bile. 00:45 Why do you require that bile? Now, we get into the effective, effective, effective lipid digestion. 00:52 So we have this bile which is then being housed in your gall bladder which makes its way to the second part of the duodenum. Are you there? Are you with me? Good. 01:01 And you see this enterocyte, and so, therefore, that bile coming into the second part of the duodenum is going to surround the triglycerides. 01:12 And when you surround your triglycerides with bile, what does it called? You call this a micelle. You call this a chylomicron. What do you call this? You call this a micelle, don't you? So micelle has been formed with emulsification process. 01:24 What it's gonna do? It does exactly that. It emulsifies the triglycerides because a triglyceride can -- can you see those finger-like projections? Those finger-like projections are the brush border of your duodenum, shall we say. 01:38 So you see where it says free fatty acids and glycerol. 01:42 That would be the lumen of the duodenum. Are you with me? And this is now become emulsified with the help of bile. 01:49 Then you're going to create these free fatty acids, FFA, which is then going to make its way through the brush border into the enterocyte. Stop there for a second. 02:00 So we're now inside my enterocyte and we're going to now recreate that triglyceride. 02:06 We are gonna reesterify, is what it's called. 02:08 That's what this is doing. The triglyceride went through the wall. 02:10 At first, it became free fatty acid. Amonotype of glycerol, and then it reformed into triglyceride. 02:15 Here I am. What are you gonna do with me? You're gonna form a chylomicron, a nascent. 02:20 What's nascent mean? Maybe, think neonatal, neonate. It's a nascent chylomicron. 02:26 What kind of apolipoprotein, it'd require? You must memorize ApoB-48. 02:31 It's imperative that you know that. The ApoB-48 is now formed a chylomicron. 02:35 What's a chylomicron have in it? It has what? It has triglycerides. Good. 02:42 What are we trying to get to? What's your objective for this entire illustration? It's the fact that you have lipid that you're consuming from your mouth, making its way to the liver. 02:52 Is that clear? Now, you have a chylomicron. What's the number one method? What's a preferred method of transport of your lipid? It is through your lymphatics. 03:00 Do you see lymphatics? Now, you find this lymphatic and it's going to make its way eventually where? The Lymphatics from the right side of the body lead to the thoracic duct, which then empties into the venous circulation at the junction of the left internal jugular and left subclavian vein. 03:16 Inside that blood vessel there are a couple of things that I wish to bring to your attention. 03:19 So here, you’ll notice that HDL. What's HDL mean to you? It's called "good cholesterol," isn't it? So, that good cholesterol is then going to donate its C-II and E to the nascent chylomicron. 03:35 What's nascent mean? Neonatal, baby. Think of it that way. 03:38 It's naive. It is now -- you have been knighted. What does that mean? HDL comes over to chylomicron and says, "Son, you have now been knighted. 03:46 I am now imparting unto you C-II and E." Now, you have a mature chylomicron. 03:54 Still filled with what please? Triglycerides. Where are you? In your blood vessel. 04:00 You're literally in your circulation. Now, that we have a mature chylomicron. What is its objective? To make its way to the liver. Let's continue. Alright now, there's number two. 04:11 Number two says CPL. That means capillary lipoprotein lipase. 04:16 CPL is capillary lipoprotein lipase. 04:19 Eventually, what are we gonna do here? We're gonna put in -- we're gonna plug in these pathologies. 04:23 But if you don't understand the normal first, it makes it quite impossible for you to understand what's going on with the pathology and you're just memorizing and that's not going to really, it won't be in your best interest. 04:34 So the capillary lipoprotein lipase, you pay attention to lipase, is then going to take the triglyceride from your chylomicron and extract it. 04:42 So now that we have an empty chylomicron, what do you need so that you can be taken up by the liver? It's called an E-receptor. 04:49 You take a look at that three. So number three is dealing with what's known as the E-receptor. 04:54 Now, let's take number one, let's take number two, let's take number three, and now that you've understand the flow of this illustration, you can see how clearly you can understand what's going on with your patient and the presentation. 05:08 The first one, number one is abetalipoproteinemia in which you literally are not able to form a proper chylomicron because apolipoprotein B or ApoB-48 is not present, pathology number one. 05:21 Pathology number two, it's the fact that you need to have C-II. 05:26 That C-II exists to stimulate that CPL. 05:30 What if you're deficient of C-II? Your lipoprotein lipase isn't working. 05:34 If that isn't working, oh my goodness, we're accumulating in your patient. 05:38 Tons of chylomicron. What's chylomicron mean to you in terms of presentation of your patient? Is it triglycerides or cholesterol? Good. Triglycerides. 05:49 Your patient is going to have triglyceride levels out the wazoo. 05:53 In other words, it'll be ridiculously elevated. Even 150 is high. 300 is really high. 06:00 Thousands is what I'm talking about with triglyceride, not a good thing. Is it clear? That's pathology number two. 06:06 Pathology number three, I would like for you to take that capital E at the E-receptor So type III, what's known as hyperlipoproteinemia is actually missing your E-receptor. 06:18 So guess what. You cannot properly pick up your chylomicron remnant into your liver. 06:25 It's called remnant-removal disease, but another name that you wanna know for this is called familial dysbetalipoproteinemia. 06:33 Here we go. Pathology 1, 2, and 3, spent a little bit of time here. 06:36 Everything that you need to know about these pathologies begins with the understanding the biochem, the phys, and then eventually, the disease processes. 06:45 Now, if that was from the mouth to the liver, what are we gonna do next? We're gonna take this lipid and we're going to then deliver it to the tissues. 06:55 So from the liver is where we are, and just like we began in the previous discussion, where we looked at your chylomicron, right? Chylomicron. Where did they come from? The enterocyte, right? What did they require for the formation of a chylomicron, it was ApoB-48. Good. 07:14 Here, the triglycerides being delivered by -- versus VLDL. 07:19 That VLDL is what is going to then transport your triglyceride. Okay Now, you see where this ApoB100? How important is that? Ridiculously important ApoB100 is a component that is required for proper VLDL formation. 07:35 What does it contain? Triglycerides. 07:37 Now, this is at first, a precursor with nascent VLDL. It's young. It's a baby. 07:42 What was it that then matured chylomicron ? Son, you have been knighted. Who knighted that particular baby? Vessel or package. It was called HDL. Here, you have it here again. 07:55 You see where this HDL. HDL is going to then also implant or deliver C-II and E here as well to VLDL. You form a proper and mature VLDL. 08:06 In the meantime, you will see an exchange of what's known as CETP. 08:10 All that is part of biochemistry that we do not have time to go through but it's important that you understand their proper to change between VLDL and HDL. 08:18 So, now they we're in -- where am I now? You're in your circulation. 08:22 Where did VLDL come from? It came from the liver. 08:25 Keep this separate please from your chylomicron that we discussed earlier. 08:29 In the meantime, what you also find from the intestine, it's important for you in biochemistry as well, is some of your long chain fatty acids. 08:39 So, all of this is then going to allow you to properly form your HDL, and what you know about HDL? HDL is a scavenger. Scavenger of what? It's a scavenger of cholesterol. What do we call HDL? We call HDL, good cholesterol. 08:52 Let's continue. So now you have VLDL. What does it contain? Triglycerides. 08:58 So, let me ask you this question. What did the tissue require for proper synthesis of your cell membrane if a tissue required, let's say, a production of your cortisol or -- gonads, you needed to produce what? Testosterone and estrogen. 09:12 It was in triglycerides that you were delivering. It's the fact that you're delivering your cholesterol. 09:18 So, what you're gonna do now? Now, quickly you're going to then go through intermediates. 09:23 So, there now you have capillary lipoprotein lipase, CPL. 09:26 You're taking out the triglyceride and you're forming IDL. What does IDL mean to you? Intermediate density lipoprotein. In this IDL, eventually is going to form your LDL right now for pathology purposes. 09:38 We're going to keep things simple. 09:40 So at this point, for all effective discussion, we've taken triglycerides from the liver and delivered to the tissue in the form of LDL. 09:51 Now, that LDL receptor, what if it was deficient? In this case, if you have an LDL receptor deficiency, you all must know that this is a type II hyperlipoproteinemia. 10:00 So, what might you call? Type I hypertriglyceridemia, is that clear? Do you see as to how it's important? It's important that you pay attention normal so that as you plugged in the pathology, all of this is coming to life. 10:16 Now, let's take a look at number 2. You see number 2. 10:19 Number two, once again the bottom line is this -- there's an accumulation of type IV. 10:25 Accumulation of the VLDL. VLDL has 1, 2, 3, 4 letters in it. 10:31 Thus, accumulation of VLDL, which also contains triglyceride, will be a type IV hyperlipoproteinemia, and this may either be primary or secondary hypertriglyceridemia. Is that clear?
About the Lecture
The lecture Hyperlipidemia by Carlo Raj, MD is from the course Atherosclerosis: Basic Principles with Carlo Raj.
Included Quiz Questions
Which part of the intestine involves an effective metabolism of lipids?
- Duodenum
- Jejunum
- Colon
- Rectum
- Ileum
Which enzyme removes the triglycerides from chylomicrons?
- Capillary lipoprotein lipase
- Hormone-sensitive lipase
- Apolipoprotein B-48
- Pancreatic lipoprotein lipase
- Hepatic lipase
Which lipoprotein scavenges cholesterol and transports it to the liver?
- High-density lipoprotein (HDL)
- Low-density lipoprotein (LDL)
- Very low-density lipoprotein (VLDL)
- Intermediate density lipoprotein (IDL)
- Apolipoprotein B-48
Which lipoprotein is elevated in Type IV hypertriglyceridemia?
- VLDL
- HDL
- IDL
- LDL
- Chylomicron
Which of the following substances reesterifies the triglycerides during their transport across the brush border of the duodenum?
- Apolipoprotein B-48
- Apolipoprotein C-48
- Apolipoprotein A-48
- Apolipoprotein B-100
- Apolipoprotein C-III
Which of the following receptors is deficient in familial dysbetalipoproteinemia?
- E-receptor
- Apolipoprotein B-48 receptor
- C-receptor
- H2 receptor
- M3 receptor
Customer reviews
3,7 of 5 stars
| 5 Stars |
|
7 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
1 |
| 1 Star |
|
3 |
Again an excellent lecture from Dr Raj. I love this man to be honest
Very good class, very dynamic teacher, excellent for learning, 5 stars
making simple subjects more difficult, very bad examples and constant joking which makes understanding hard. the way he explains topics from last to first makes it difficult to follow and remember
Dr. Raj uses a conversational and repetitive lecture style that really helped me actually be able to learn and recall the material. I suppose some people may not like this taking a bit longer, but considering the fact that I was able to remember and learn the entire mechanism and pathology in around 20 minutes I think this style works well for long-term learning.