Playlist
Show Playlist
Hide Playlist
Hereditary Liver Diseases
-
Slides GD liver disease.pdf
-
Download Lecture Overview
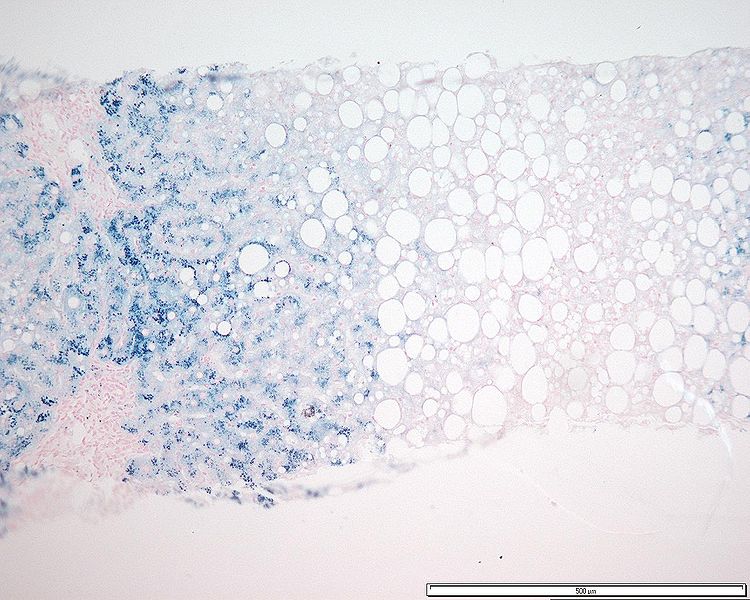
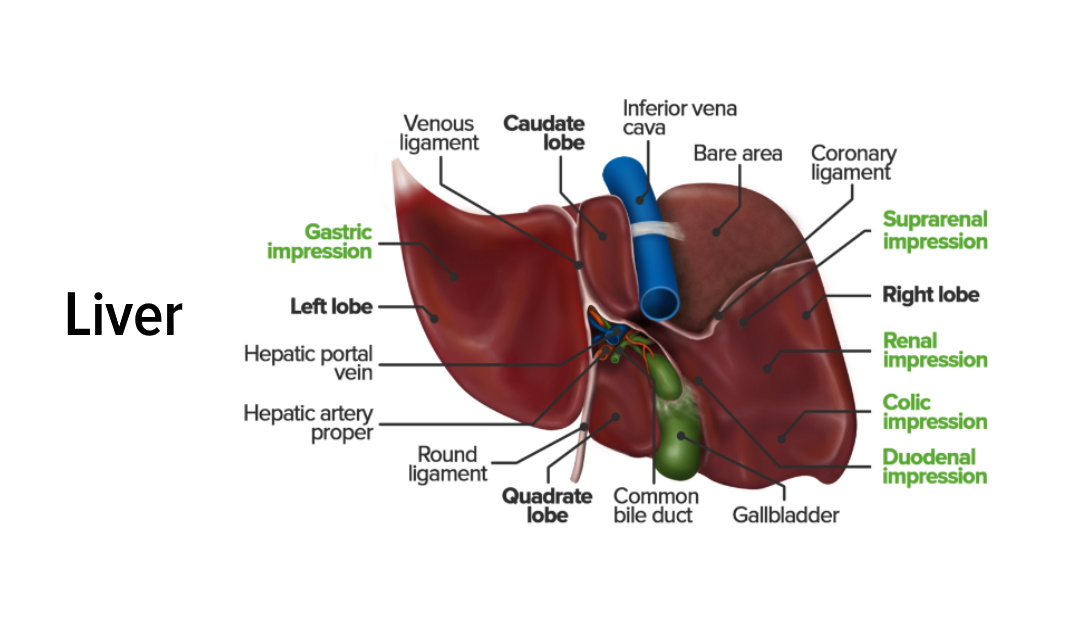
00:01 Move on to hereditary liver diseases, and the differentials that you find with hereditary liver disease include hereditary hemochromatosis, Wilson's disease, big time. 00:13 You need to know about alpha-1 anti-trypsin deficiency. How come? How common might you find cystic fibrosis in the Caucasian population? Quite common. 00:22 How often can you find Down's Syndrome in the Caucasian population? Unfortunately, quite common. 00:28 The third most common genetic disease in the US in the Caucasian population is alpha-1 anti-trypsin deficiency. 00:38 So, if you did not pay attention to it in med school, oh my goodness, pay attention to me now and I’ll walk you through. 00:45 Remember, not only you can have alpha-1 anti-trypsin deficiency causing damage to the liver, but obviously, you've heard of panacinar emphysema. We've talked about that in pulmonology.
About the Lecture
The lecture Hereditary Liver Diseases by Carlo Raj, MD is from the course Liver Diseases: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following is NOT an example of hereditary liver disease?
- Budd-Chiari syndrome
- Alpha-antitrypsin deficiency
- Hemochromatosis
- Wilson disease
- Cystic fibrosis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |