Playlist
Show Playlist
Hide Playlist
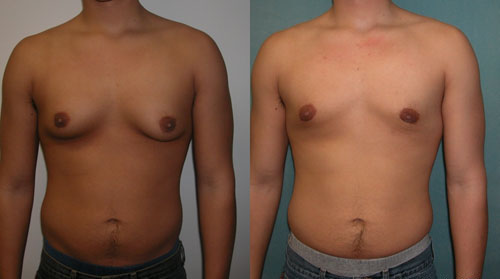
Gynecomastia in Adolescent Males
-
Slides Gynecomastia Pediatrics.pdf
-
Download Lecture Overview
00:01 In this lecture, we will review gynecomastia which is a common problem in adolescent males. 00:07 Basically, the pathophysiology of standard gynecomastia in males is a result of excess estrogen compared to androgens in the blood. This transient imbalance between estrogen and androgens occurs commonly in early puberty in males. We see spontaneous regression of this gynecomastia when the androgen levels rise and counter the estrogen effects. However, there are some pathologic causes of gynecomastia which the practitioner should be aware of and rule out in a patient who complains of unilateral or bilateral breast development. One is they can be drug induced. 00:51 So specifically, anabolic steroids, antipsychotics, spironolactone, marijuana, and ketoconazole are all implicated in the development of gynecomastia. Tumors may result in gynecomastia, in particular testicular tumors or adrenal tumors. Patients with hyperthyroidism may develop gynecomastia or primary hypogonadism, the classic example being Klinefelter syndrome. 01:20 Patients may have organ dysfunction resulting in gynecomastia, things such as cirrhosis or renal insufficiency. If you see a patient with gynecomastia, it’s important to ask a few questions. 01:36 First, pubertal gynecomastia may be painful or slightly tender. If there has been nipple discharge, consider a pathologic pituitary cause such as a pituitary adenoma. You should review the progression of the breast development and how that has been going. It’s important to ask about marijuana. 01:57 Marijuana use in teens is common and a lot of marijuana use may be the cause of that patient’s gynecomastia. 02:04 Also, ask if the patient has noted any abnormalities on testicular self-exam which they should be counseled to be doing anyway. On physical exam, you will generally notice in gynecomastia a firm, rubbery mobile mass of breast tissue just beneath the areola. Check for galactorrhea. This is present in high prolactin use or in marijuana use. Examine the testes for masses and asses the patient’s Tanner stage. 02:33 Review for signs of thyroid, liver, or renal disease. Lab testing is generally not required. 02:43 We sometimes will do a workup on gynecomastia if the duration is more than two years, if puberty has completed and then it shows up, or if there are some sort of abnormalities on either history or physical exam that are keying you off that there might be a systemic problem. 03:00 We may check thyroid function test for patient who we suspect thyroid disease or testosterone levels or we can also check estradiol levels. LH is a signal that goes down then to the testicle and signals testosterone development. If we’re concerned about low levels of testosterone being centrally mediated, we may check levels of gonadotropin hormones. LFTs may be helpful in a patient with suspected liver disease. So, testing is really directed at the concern we’re finding on history and physical exam. Our treatment of gynecomastia is really not much. 03:37 We generally have to just reassure the patient that this will gradually go away and that’s all you need. 03:42 We do recommend seizing any contributing medications, any of those drugs that we mentioned that can cause problems. There is limited data to support use of pharmacological therapy. 03:53 We don’t usually give testosterone injections for example for a patient with gynecomastia. 03:59 However, if there is no regression of the lesion, we can do surgical intervention for cosmetic purposes. 04:06 That’s a review of gynecomastia in adolescent males. Thanks for your time.
About the Lecture
The lecture Gynecomastia in Adolescent Males by Brian Alverson, MD is from the course Adolescent Medicine.
Included Quiz Questions
Which of the following does NOT cause gynecomastia?
- Tamoxifen
- Cocaine
- Marijuana
- Benzodiazepines
- Spironolactone
Which of the following is NOT a cause of gynaecomastia?
- Ovarian cancer
- Testicular tumor
- Adrenal tumor
- Hyperthyroidism
- Klinefelter syndrome
Which of the following is an indication for further workup in a prepubertal boy with bilateral gynaecomastia of approximately 3 cm for 6 months?
- Age
- Bilateral involvement
- No nipple discharge
- Size
- Duration of symptoms
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Good overview of a disease that is not often talked about in pediatrics. Thank you!