Playlist
Show Playlist
Hide Playlist
Gout: History, Pathophysiology
-
Slides Gout.pdf
-
Reference List Rheumatology.pdf
-
Download Lecture Overview
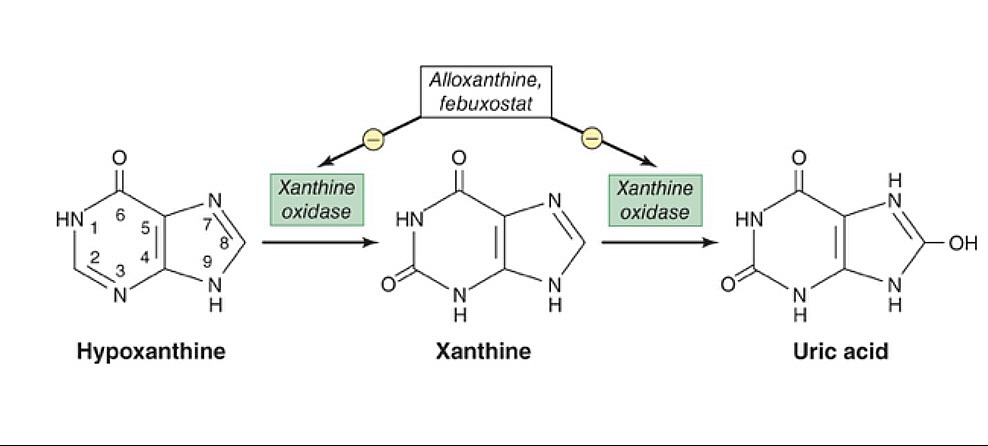
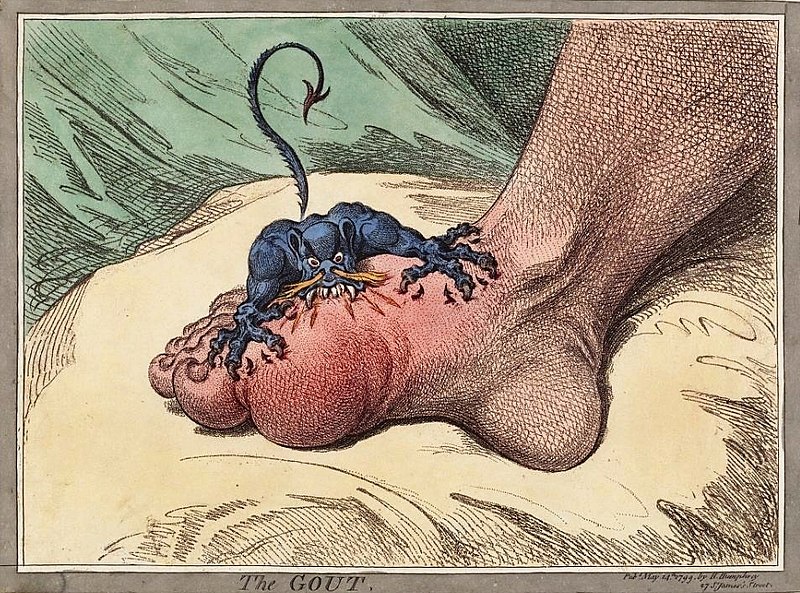
00:00 So let's take a step back and talk about what is gout. 00:04 We'll talk about the pathophysiology in a moment but actually the history can help us to remember some things about the disease as well. 00:10 This is a picture of a classic 18th century depiction of gout, specifically podagra. 00:17 Podagra is the term that we use to describe gout when it afflicts the 1st MTP and that just happens to be the most common place that people have their first episode of gout. 00:27 The word gout comes from an old Latin term, "gota", which simply means, drops. 00:32 The thought was that gout was essentially an accumulation of toxic humourous inside an afflicted joint. 00:38 In fact, when you use the term "insulin drip" in the hospital and you write "gtt" which is sort of how we use to write orders on paper, that "gtt" means "gota", so it means drops when you're ordering a drip. 00:49 Same thing with guttate psoriasis where we see guttate being used to describe little dew drops on the skin. 00:55 So the etymology can help us here. 00:57 Podagra comes from 2 Greek words, "pod, podus" which means foot and "agrar" which means to seize or to bite, which is what we're seeing in this picture. 01:06 Those who have ever had an acute flare of gout, they know there is an intense onset of pain can come on in span of hours with heat, redness, tenderness, swelling, the works. 01:19 and that's exactly what's captured in this 18th century picture. 01:23 To continue with our history lesson for just a moment, gout used to be called the "disease of kings". 01:28 But because it was only people who were affluent and wealthy and had access to have seafood and high protein, meats, alcohol, those were the folks who were likely to get gout. 01:39 And that tells us a little bit about the pathophysiology. 01:41 We know that gout is associated with purine rich foods: meat, seafood, alcohol and also it's associated with obesity and hypertension which is also something you would see in the affluent who could afford to be obese. 01:56 So let's talk now about the pathophysiology of gout. 01:59 Specifically, when we're talking about what causes gout, we're talking about hyperuricemia, how much uric acid is in the body. 02:06 To start this off, I'd like you to think of that circle in the middle that says urate as essentially the total body content of urate in our body. 02:14 I'll interchangeably go between saying urate and uric acid, just so you're aware. 02:19 So on the left of that circle, think of that as a faucet. 02:23 Those are things that are pouring uric acid into our body, which think of that like a bathtub. 02:28 So for stuff on the left is your dietary purine load, how much purine rich substances you're consuming and then endogenous purine synthesis. 02:37 If for some reason there's increase cell turnover or cell death, there's gonna be a release of purines into the bloodstream and that's also gonna lead to increased urate. 02:46 On the right hand side, think of that like a drain, draining stuff out of your bathtub. 02:50 So, renal excretion, how effectively are you getting urate out and same thing with gut excretion as well. 02:56 Turns out there's a lot of different factors which contribute to these things, turning the faucet on or increasing the activity of the drain or clogging the drain. 03:05 Ultimately, as the bathtub of uric acid increases, we have urate supersaturation, crystallization in joints and boom, a gout flare. 03:16 Let's look at some of those specific factors. 03:19 First off, I mentioned dietary purine load. 03:21 Things like meat, seafood, that's gonna increase purines coming into your body. 03:26 Obesity, we know that that's associated with increased endogenous purine synthesis. 03:31 Pancreatitis, this simply is meant to represent any number of different types of chronic inflammatory states or acute inflammatory states that just increase protein catabolism and they're gonna lead to increased purine synthesis. 03:45 Likewise, a lymphoproliferative disease or lymphoma or leukemia, those kinds of cancers, lots of increased purine synthesis there. 03:53 And lastly, a hospitalized patient. 03:56 Someone who comes in septic shock or has a massive surgical procedure, there's gonna be some tissue necrosis, tissue ischemia is gonna lead to cell death and again, a load of purines being released into the blood stream. 04:09 So that's the faucet, now let's focus on the drain. 04:12 And it's important to think about the drain because it turns out that 85% of the contributing causes of uric acid or hyperurecemia is really the drain problems, clogging the drain. 04:24 Chronic kidney disease, our patient's got CKD stage III, He's gonna have a lot of trouble getting all that urate out of his body. 04:31 Likewise, there's certain medications which can compromise our ability to get urate out, classically, diuretics. 04:37 Turns out that diuretics while they may help with salt excretion, they can also contribute to uric acid reuptake and prevent us from getting urate out of our bodies. 04:47 Other medications to think about are also things like cyclosporine which can also impede the flow of urate excretion via the kidneys. 04:57 Thirdly, the ovaries. 04:59 It turns out that having ovaries is protective. 05:02 That's why men are more likely to get gout than women. 05:05 But as soon as a woman becomes as post-menopausal, either surgically or just in menopausal period with age, that woman now is gonna become susceptible to hyperuricemia. 05:17 It turns out that estrogen in ovaries was promoting urate excretion. 05:21 Once the ovaries are not doing that anymore then uric acid starts to build up. 05:26 And lastly, diseases like hypertension have been associated with impaired renal excretion as well.
About the Lecture
The lecture Gout: History, Pathophysiology by Stephen Holt, MD, MS is from the course Non-Autoimmune Arthritis.
Included Quiz Questions
Which of the following is the most common site of gouty arthritis?
- First metatarsophalangeal joint
- Ankle joint
- Knee joint
- Shoulder joint
- Wrist joint
Which of the following drugs is considered a risk factor for developing gout?
- Cyclosporine
- Febuxostat
- Acetaminophen
- Montelukast
- Zileuton
Which of the following is NOT considered a risk factor for gout?
- Coffee intake
- Hypertension
- Obesity
- Diuretics
- Alcohol consumption
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
history lesson helps retention. and his energy keeps the audience engaged.