Playlist
Show Playlist
Hide Playlist
Guillan-Barré Syndrome (GBS) and Acute Disseminated Encephalomyelitis (ADEM)
-
Slides GBSandADEM Pediatrics.pdf
-
Download Lecture Overview
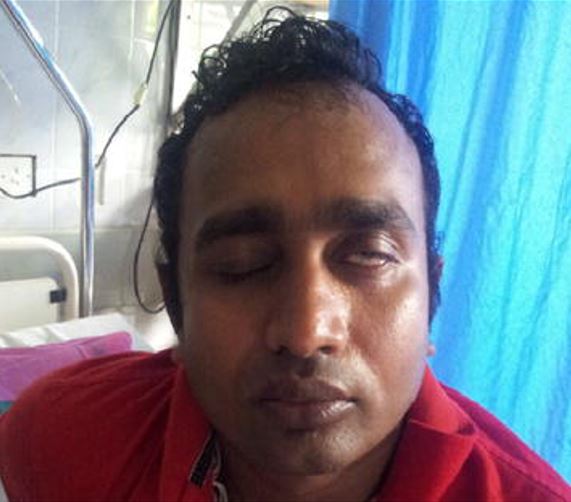
00:01 In this lecture we will discuss autoimmune attacks on the CNS. 00:06 We'll talk about Guillain-Barre Syndrome and Acute Disseminated Encepahlomyelitis. 00:12 Let's start with Guillain-Barre Syndrome. 00:15 So, Guillain-Barre is an autoimmune antibody attack on the peripheral nerve roots. 00:21 Typically, this is an attack on the myelin sheet of the nerve. 00:26 Usually, there is a preceding infection, something like diarrhea. 00:30 Especially, Campylobacter can cause it. 00:33 Also, patients can get mycoplasma pneumonia infections and then subsequently have Guillain-Barre Syndrome. 00:41 General viral respiratory illnesses can trigger the problem. 00:45 And vaccination can to, especially influenza vaccination. 00:52 So, how does Guillain-Barre present? Generally patients have an acute weakness. 00:58 This acute weakness has a typical pattern of ascending. 01:02 It starts with leg weakness, and gradually proceeds up to the body to the arms and eventually to the cranial nerves. 01:10 The progression usually happens over a period of a few days. 01:15 And it may lead to respiratory failure, which is when people really get into trouble. 01:23 The weakness is symmetric in that both legs and both arms should be equally affected. 01:29 Generally, deep tendon reflexes should be diminished or absent. 01:33 Because of the nerve root. 01:35 And pain is common. This can be a very painful condition. 01:39 Autonomic dysfunction is possible and this can be dangerous. 01:44 Patients can develop cardiac arrhytmias They may get urinary retention. 01:48 And they may develop gastroparesis. 01:52 One side type of Guillain-Barre Syndrome is the Miller-Fischer variant of Guillain-Barre Syndrome. 02:00 This may happen as the isolated finding or it may happen in the context of a patient with this gradually ascending paralysis. 02:10 The key for Miller-Fischer variant is opthalmoplegia or paralysis of the eye muscles. 02:17 Here, you can see this child being asked to look about the room is having great difficulty moving his eyes. 02:25 Weakness commonly begins in this case in the cranial nerves. 02:30 And patients may have the triad of Ataxia, and Areflexia, but then also, Ophthalmoplegia but arm and leg weakness occur in the minority of these cases. 02:43 Most just have the eye findings. 02:46 Back to Guillain-Barre Syndrome. 02:49 If we have a patient where we have suspected the key test to get is the spinal tap. 02:54 In patients with Guillain-Barre Syndrome, typically, there will have a normal white cell count and a very elevated protein level. 03:03 This is sometimes called Albuminocytologic dissociation. 03:08 That's a fancy way of saying, the albumin or protein is high but the cell count is normal. 03:14 Remember, normally in meningitis, we see both being elevated. 03:18 If we proceed to MRI because we are suspicious of Guillain-Barre Syndrome, the MRI may well show enhancement of the nerve roots and we can also do if we wish, specific antibody testing to see whether the patient has antibodies directed against to their nerves Additionally, if a diagnosis really needs to be made, in most cases we don't really need to go this far, patients can get nerve conduction studies to try and figure out the speed at which electrical signals are going through those nerves. 03:52 It should be delayed with patients wtih myelin damage. 03:57 Generally for Guillain-Barre Syndrome, steroids are not helpful. 04:03 IVIG is. 04:05 And so we'll give Intravenous Immunogobulin to patients with Guillain-Barre Syndrome. 04:10 This is effective. It slows progression and it speeds up recovery. 04:16 We want to watch these patients very carefully. 04:19 And to do that, we get something called NIFs This is done typically on the wards or in the ICU setting. 04:27 So, what is a NIF? A NIF is a Negative Insperatory Flow. 04:33 The patient is asked to breathe all the way out and breathe in as rapidly as they can. 04:38 This is the measure of the patients ability to sustain respiration. 04:43 And will check baseline NIFs and as they decline, we know we're moving closer and closer towards the need for respiratory support or intubation. 04:54 Pulse oximetry is not effective for screening. 04:57 Because the oxygen is the last thing to go. 05:01 Mechanical ventilation is needed often in these patients who are severe for respiratory failure. 05:08 We will intubate them and generally wait for the illness to resolve and they can be safely extubated and hopefully recover fully. 05:16 And the vast majority do recover fully. 05:19 95% of these patients will eventually make a full recovery. 05:24 But that recovery may take months. 05:27 So, we have to be patient and wait for the child to improve. 05:31 Let's switch gears here to Acute Dissemintated Encephalomyelitis. 05:37 or ADEM. 05:39 ADEM is a brief but intense disease. It is an autoimmune attack on the brain and the spinal cord. 05:47 And these antibodies are against again on myelin. 05:51 It is often preceded by a viral infection usually one or two weeks later. 05:56 And maybe a precursor to multiple sclerosis. 06:00 You can think of this a little bit like MS in children. 06:06 ADEM is usually a rapid onset problem, where patients are fine and then rapidly develop encephalitis or central nervous system symptoms. 06:17 Weakness may be present or a sensation of pain is present. 06:21 If they have spinal cord lesions as well, which they may or may not. 06:26 Sometimes, this can be a confusing picture. 06:29 Because the problem as the name suggests is disseminated. 06:33 And can be spotty. 06:35 So, certain areas of the brain are affected but not others and that could lead to very unique neurologic patterns in terms of symptomatology Optic nerve involvement can happen and patients may have vision problems as well. 06:50 Here you can see a typical brain MR for patients with ADEM. 06:54 And you can see several spots highlighted by the arrows where inflammation is occuring. 07:00 A brain and spine MRI is indicated if you suspect ADEM. 07:05 Because involvement can happen anywhere along the brain and the entirity of the spine. 07:10 The MRI is diagnostic for demyelinization. 07:14 And with a spotty picture the diagnosis is made. 07:17 In ADEM, unlike in Gullain-Barre, steroids are helpful and are the mainstay of treatment. 07:26 IVIG or plasmaphoresis maybe helpful. It is unclear right now. 07:32 Good studies haven't really been done. But in severe cases we may move on to that as an act of desperation to try and help the child improve. 07:41 Recovery usually happens over a period of usually 1-2 months. 07:45 But unlinke Guillain-Barre Syndrome, which has a very high rate of recovery While many children recover, not all do. 07:52 Generally, between 60-80% will have a recovery. 07:56 And a small minority may be at risk for eventually developing multiple sclerosis. 08:02 That's all I have for today about acute disseminated encephalomyelitis and Gullain-Barre Syndrome. 08:08 Thanks for your attention.
About the Lecture
The lecture Guillan-Barré Syndrome (GBS) and Acute Disseminated Encephalomyelitis (ADEM) by Brian Alverson, MD is from the course Pediatric Neurology. It contains the following chapters:
- Guillain-Barré Syndrome
- Miller-Fischer Variant
- Diagnosis and Management of Guillain-Barré Syndrome
- Acute Disseminated Encephalomyelitis (ADEM)
Included Quiz Questions
Which of the following is the best therapy for a patient with Guillain-Barré syndrome (GBS)?
- Intravenous immunoglobulin (IVIG)
- Intravenous steroids
- Oral methotrexate
- Fluorouracil
- Rhogam
Which of the following correctly describes Guillain–Barré syndrome (GBS)?
- Autoimmune attack on the peripheral nerve roots
- Exclusively affects the central nervous system
- Most commonly occurs after a streptococcal throat infection
- Starts with weakness in the arms
- Does not progress
Which of the following is a fatal complication of Guillain–Barré syndrome (GBS)?
- Respiratory failure
- Congestive heart failure
- Ischemic stroke
- Renal failure
- Coma
Which of the following is NOT a feature of Guillain–Barré syndrome (GBS)?
- Asymmetric weakness
- Absent deep tendon reflexes
- Pain
- Urinary retention
- Gastroparesis
Which of the following is the key feature of the Miller-Fischer variant of Guillain–Barré syndrome (GBS)?
- Ophthalmoplegia
- Areflexia
- Ascending paralysis
- Urinary retention
- Ataxia
Which of the following is NOT seen on the cerebrospinal fluid of a patient with Guillain–Barré syndrome (GBS)?
- Elevated glucose
- Normal WBC count
- Elevated protein
- Elevated albumin
- Albuminocytologic dissociation
Which of the following is TRUE regarding Acute Disseminated Encephalomyelitis (ADEM)?
- Antibodies against myelin are created
- Chronic course
- Autoimmune attack on the muscles
- Preceded by fungal infection
- Associated with Guillain-Barré syndrome (GBS)
Which of the following is the mainstay of management of acute disseminated encephalomyelitis (ADEM)?
- Steroids
- Antifungals
- Antiviral
- Supportive only
- Beta-agonists
Guillain–Barré syndrome (GBS) can be triggered by diarrheal illnesses and respiratory tract infections. On rare occasions, which of the following vaccines could cause GBS?
- Influenza vaccination
- Mumps vaccination
- Small pox vaccination
- Measles vaccination
- Polio vaccination
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Excellent lecture as usual. It is very helpful to see all the diseases one has studied for adults, explained for pediatrics. It gives the student more confidence instead of wondering: "well, in adults it's like that, maybe it's the same for children". It gives more certainty.