Playlist
Show Playlist
Hide Playlist
Examination of the Skin and the Mucosal Surfaces
-
Reference List Physical Examination.pdf
-
Download Lecture Overview
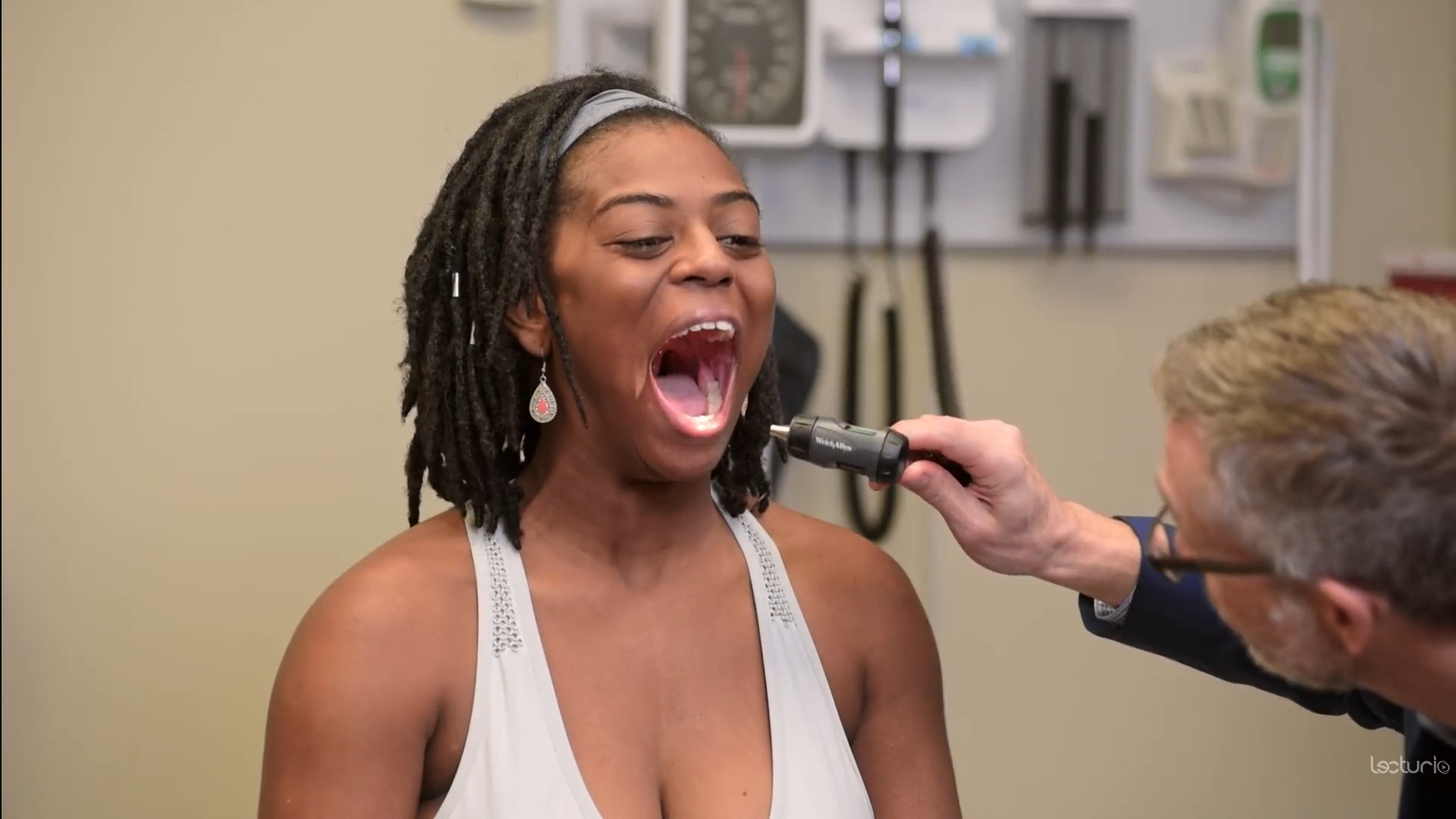
00:00 Next, we're going to move on with the dermatologic exam. Now this is, as you might imagine, a potentially very sensitive part of the exam because we really need to see every square inch of our patient's skin. So top to bottom, front to back including orifices and any crevices to make sure that there's no pathology in those areas depending of course on what exactly you're looking for. That will also include the scalp, the nails, the mucosal surfaces, etc. So, turning over to our patient, I would have her fully gowned and comfortable. While we're walking through each part of the exam, I wouldn't just have her sitting naked on a table, we would instead just look at each area as we need to protect our patient's modesty. So we'll go ahead and start with just looking at the arms, so putting the arms out to the sides. 00:48 I'm looking at the flexor surfaces of the arm and then I'll flip around and look at the extensor surfaces of the arm. Knowing the regional anatomy in which particular disease processes may afflict certain areas can help you to focus on the focal versus the global part of the dermatologic exam. So if I saw just some papules or macules with some excoriations in her antecubital fossa, I'd be thinking about atopic dermatitis whereas on the extensor surfaces I may be thinking more about something like psoriasis. So, attending to those areas is important. 01:19 It's also really important that we look in the interdigital spaces there, sometimes people could even have a melanoma brewing in there. And down at the toes that's where you may find evidence of a fungal infection, tinea pedis with interdigital maceration between the 5th and 4th or 4th and 3rd toes. We're also going to be looking at her nail beds themselves. It's important to take a look at the nail beds and the nail plates as they may be harbingers of systemic disease. You can find half-and-half nails there in the setting of kidney disease, Terry's nails in the setting of cirrhosis, Muehrcke's lines in the setting of hypoalbuminemia. 01:55 There are really a lot of different things that you could find if you go looking for it there. 02:01 I will do the same thing with her right arm then her left leg and her right leg and I already mentioned the toes as well. Next up, we'll take a look at mucosal surfaces and if the patient was concerned about a sexually transmitted infection or if there were concerns in that regard then of course we would perform a mucosal exam involving the vagina and the intergluteal cleft posteriorly. In this case, we're just going to focus on looking at the mucosal surfaces of the mouth and the eyes. So just grab my light. Open up, great. I'm looking at the buccal surfaces, the upper palate, the uvula. And your tongue you can stick out please too, great. And then I would likewise look under her conjunctivae, bottom, and top. There are a lot of different things that may present on the skin, but actually may have more clues if you look in the mucosal surfaces. Things like Stevens-Johnson syndrome, bullous pemphigoid and pemphigus vulgaris can be distinguished by the fact that the latter is more likely to have mucocutaneous involvement so it's really important to not neglect looking at the mucosal surfaces. Next up, let's make sure that we can use the right language to describe what we find. So, in this case I can tell you that we're right down here on her foreleg identifying a flat, hyperpigmented lesion. We're obviously not going to just use the term lesion, we need to be more descriptive than that. So the proper terminology for a non-palpable lesion that is smaller than a centimeter is a macule. If it's larger than a centimeter we would, instead of using macule, we would refer to it as a patch. If, on the other hand, I ran my thumb over this and it was palpable instead of using the word macule we would call it a papule. Greater than a centimeter, it's called a plaque. If, on the other hand, I rubbed it again and it had fluid in it so it's both palpable and appears to be fluid-filled the proper term is a vesicle. You could also use the term blister to describe that. Greater than a centimeter, we would use the term bullae. If it was not only enlarged, but it was very firm and appeared to have a subdermal component, at that point we would use the term nodule. And if greater than a centimeter, we would use the term tumor though it may delay the term tumor has a lot of baggages that comes along with it so sometimes we don't certainly use that term, we would just describe the size of the lesion. Lastly, I should mention that certainly people can have evidence of bleeding into the skin and there are different terms to describe that as well. A lesion that is smaller than 3 mm is referred to as a petechiae whereas if it's larger you can use either the term ecchymosis or a purpura which is just a larger area of bleeding into the skin. If somebody has an inflammatory lesion involving like a vasculitis with inflammation of blood vessels with extravasation of blood into the skin, we could call that palpable purpura because normally a purpura is just flat and you don't feel it under your fingertips. So those give us the right language to be used to describe different lesions that we may find. And I just want to add 3 specific maneuvers that you can do at the bedside in specific circumstances depending upon what sort of lesions you're looking at. So, let's say that Shayla had evidence of bullous lesions on her arms or elsewhere in her body and if right here there was one bullous lesion, we would want to see whether or not there is a defect in the epidermis. Remember there is an epidermis and then a dermis and there are some diseases that specifically attack the interconnections within the layers of the epidermis. And when that's the case, the skin gets very friable and it's easy to separate and cause blisters. And that's a classic feature, for example, of pemphigus vulgaris. You can also see it though in toxic epidermal necrolysis and Stevens-Johnson syndrome. So a test is called the Nikolsky sign where I'm simply pulling on the skin and if there was disease within the epidermis, simply pulling on the skin like that in an area adjacent to where there's a blister may cause further tearing of the skin and it would really help to clench your diagnosis. In contrast, bullous pemphigoid involves the defect at the junction between the epidermis and the dermis. The skin is much stronger and so doing that Nikolsky test would not yield any further breaks in the skin. So that's the Nikolsky test. The next one that I want to demonstrate is simply called dermatographism and there were some very specific diseases that are associated with dermatographism. What I typically would do is I can use the back of my thumb, you actually just basically scrape the skin like that and you can even make a small symbol just to make sure that you know what you're drawing on. A patient with dermatographism within a matter of 30 seconds to a few minutes you'll actually see a wheel or hives appear just in the area where I have put some stress on the skin. And that's why it's called dermatographism, which means drawing on the skin. And you can actually, you know, spell out letters if you were to do so.
About the Lecture
The lecture Examination of the Skin and the Mucosal Surfaces by Stephen Holt, MD, MS is from the course Examination of the Skin.
Included Quiz Questions
Scraping a client’s skin with a fingernail to see whether it produces urticarial erythema in a linear distribution is called...
- ...dermatographism.
- ...Nikolsky sign.
- ...Murphy’s sign.
- ...McMurray’s test.
- ...Auspitz sign.
What is the definition of a macule on skin exam?
- A flat, non-palpable skin lesion smaller than 1 cm in size
- A blister
- A raised, palpable skin lesion smaller than 1 cm in size
- A raised, palpable skin lesion greater than 1 cm in size
- A flat, non-palpable skin lesion greater than 1 cm in size
What is the definition of a papule on skin exam?
- A raised, palpable skin lesion smaller than 1 cm in size
- A flat, nonpalpable skin lesion smaller than 1 cm in size
- A blister
- A raised, palpable skin lesion greater than 1 cm in size
- A flat, nonpalpable skin lesion greater than 1 cm in size
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
1 customer review without text
1 user review without text