Playlist
Show Playlist
Hide Playlist
Epidural Hematoma: Etiology, Clinical Presentation, and Diagnosis
-
Slides Head Trauma Epidural Hemorrhage.pdf
-
Download Lecture Overview
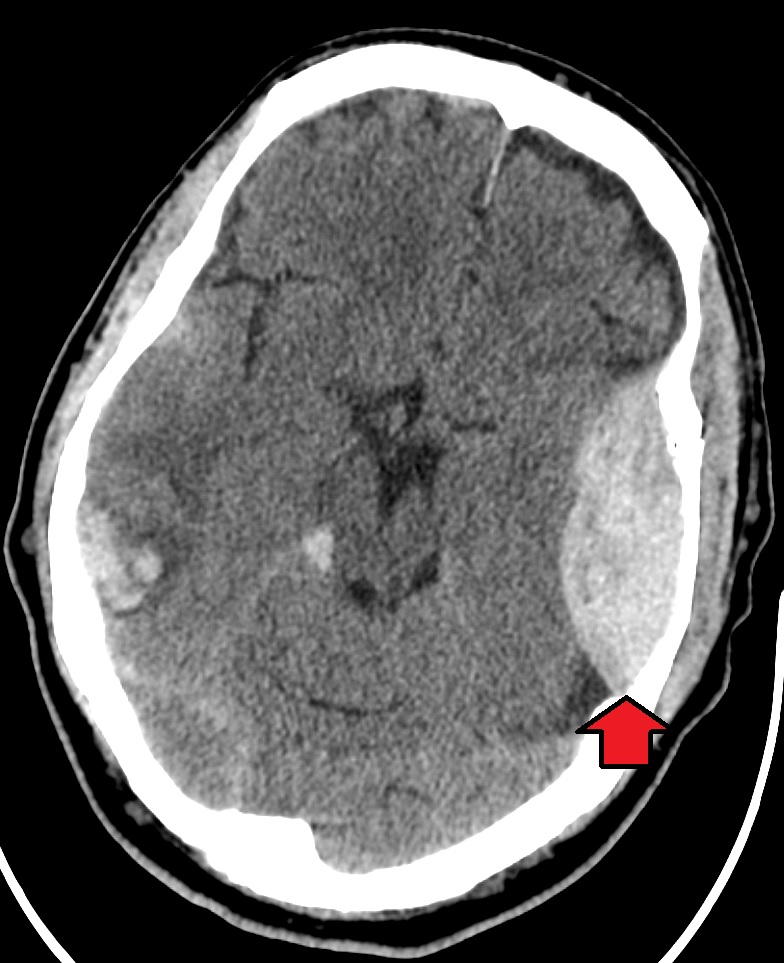
00:01 So let's talk a little bit more about epidural hematoma and start with a definition. 00:06 Epidural hemorrhage or epidural hematoma is a bleeding event where bleeding occurs into the epidural space between the dura layer of the meninges and the skull usually caused by trauma. 00:19 As we think about what's happening, I think it's helpful to look at the layers of the brain and skull. 00:24 So here we're looking at the skull bone going all the way down into the brain. 00:27 And we see that epidural space is a potential space between the bone and the dura mater. 00:34 And that's really where an epidural hemorrhage occurs. 00:37 This is the development of blood within that potential epidural space. 00:41 Importantly, the dura is affixed to the bone at suture lines and so we don't see epidural hematomas extend beyond suture lines, and the result is a pinching of blood on two sides and a lens shaped a deformity that we see on imaging. 00:58 What about the epidemiology? Epidural hematomas are estimated to have an incidence of 1-4% of traumatic head injuries. 01:07 They may be accompanied by a skull fracture and 75% of cases. 01:11 Skull fracture is common. 01:12 If we see a skull fracture, let's look for epidural hematoma. 01:15 And alternatively, if we see an epidural hematoma, we need to evaluate for the potential of a skull fracture. 01:21 Peak incidence is in young adults ages 20 to 30s as a result of trauma in those ages, and it's really rare to see this in individuals over the age of 50. 01:31 And older individuals we tend to see subdural hematomas more commonly than epidural hematoma. 01:38 Let's talk about the etiology. 01:39 What's going on how does this developed and what occurs in the development of an epidural hematoma? Head trauma is the most common cause of an epidural hematoma. 01:52 Trauma causes injury to the vascular structures that course between the dural meningeal layer and the skull. 01:59 The trauma transmit forces from the skull base into the brain and causing injury to underlying structures. 02:06 One that I want you to remember is the middle meningeal artery and you can see that here. 02:11 It is on a course right beneath the temporal bone and is subject to injury with lateral head trauma. 02:19 Rupture of the middle meningeal artery results in an epidural hematoma formation. 02:23 And this is the most common cause of epidural hematoma and one to remember. 02:28 We can also see injury to the anterior meningeal artery to the dural sinuses and others. 02:33 But that injury to the middle meningeal artery resulting in epidural hematoma from trauma is one to commit to memory. 02:42 How about etiology? We can see epidurals from any cause of trauma, motor vehicle accidents, falls, assaults, any injury that could put stress and strain on the skull and transmit that into those epidural arteries. 02:57 In terms of clinical presentation and neurologic symptoms, the nature of the neurologic symptoms and signs depends on the following characteristics. 03:05 And I like to think of four. 03:06 One is the location of the injury. 03:08 Two is the size of the blood. 03:10 Three is the rate of growth or more rapid the rate of growth of the blood. 03:14 The shorter that lucid interval, and the more significant the neurologic deficits. 03:19 And the acuity of the associated injury. 03:23 So we think about each of those in terms of the types of symptoms the patient may present with. 03:29 So let's look at the time course of what's happening with an epidural hematoma. 03:33 This begins with a traumatic event. 03:35 And typically it's a significant at traumatic event, enough to contribute to momentary or perhaps more persistent loss of consciousness for a period of minutes. 03:44 Typically, we hear from patients who have suffered an epidural hematoma, a period of spontaneous recovery for some period of time, that may be short minutes, it may be hours. 03:53 It's usually not longer than days. 03:56 And this is followed by progressive neurologic deterioration, often focal neurologic deficits and impaired consciousness over time. 04:05 And that lucid interval that period of spontaneous recovery is an important contributing factor to epidural hematoma presentation and something we should key into when we're listening to the history for these patients. 04:17 It's observed in roughly 50% of cases of epidural hematomas. 04:21 This is often from an arterial bleed, and that initial arterial bleed takes time to develop and once it does, there's progressive neurologic deterioration, again, occurring in hours that contributes to this presentation. 04:34 That's different from subdural hematomas, which typically come from venous bleeding, which take days two weeks to develop, and we hear a more progressive course over time, and that story can help to differentiate epidural and subdural hematomas. 04:48 Other symptoms including headache, nausea, vomiting, drowsiness, confusion from increased ICP can also be present in these patients. 04:56 How about the diagnostic investigation? What do we do to work this up? Well, first is a noncontrast head CT which we're going to do for any patient presenting with moderate to severe TBI. 05:06 The imaging modality is the choice modality to look at acute head trauma, acute loss of consciousness and suspected epidural as a result of the trauma or other intracranial bleeds. 05:17 What we're looking for as we see on this noncontrast head CT is a lens-shaped deformity, does not extend beyond suture lines, and we see the appearance of hyper density on the CT as a result of the underlying bleeding. 05:31 Acute epidurals are this high density lens-shape, which is very specific for a diagnosis of epidural hematoma. 05:39 The fresh blood appears as a high density on CT and so we're looking for that on the noncontrast scan. 05:45 The acute blood collection sometimes is easily distinguishable from the surrounding edema. 05:50 But in less than 10% or roughly 10% of cases, it's really hard to see that underlying epidural blood early in the course of the bleeding and so we need to look at this closely in patients presenting soon after an event and with minor injuries and minor symptoms.
About the Lecture
The lecture Epidural Hematoma: Etiology, Clinical Presentation, and Diagnosis by Roy Strowd, MD is from the course Head Trauma.
Included Quiz Questions
What is caused by trauma and results in bleeding between the dura mater and the skull?
- Epidural hematoma
- Subdural hematoma
- Subarachnoid hemorrhage
- Intraventricular hemorrhage
- Subgaleal hematoma
What clinical finding often correlates strongly with an epidural hematoma?
- Skull fracture
- Otorrhea
- Gaze palsy
- Resting tremor
- Ataxia
Traumatic injury to which artery is most likely to cause an epidural hematoma?
- Middle meningeal artery
- Basilar artery
- Vertebral artery
- Internal carotid artery
- External carotid artery
How long might a clinician expect the lucid interval to last in a patient with an arterial source of intracranial hematoma?
- Hours
- Minutes
- Days to weeks
- Up to a year
- Up to three months
What is the initial imaging modality of choice in evaluating a suspected epidural hematoma, and what is the typical finding?
- Non-contrast head CT; lens-shaped opacity
- CT head with contrast; lens-shaped opacity
- T2-weighted MRI; lens-shaped opacity
- Non-contrast head CT; crescent-shaped opacity
- CT head with contrast; crescent-shaped opacity
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |