Playlist
Show Playlist
Hide Playlist
DiGeorge Syndrome
-
Slides DiGeorgeSyndrome Pediatrics.pdf
-
Download Lecture Overview
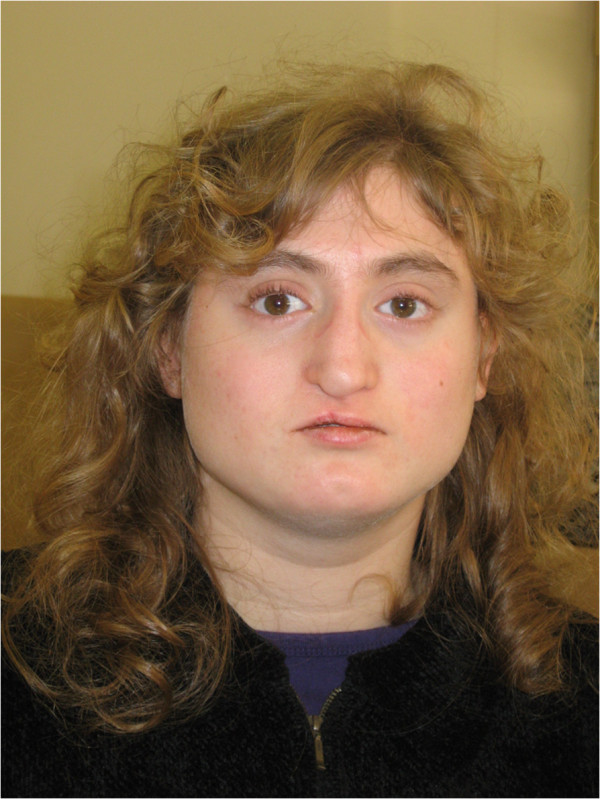
00:01 In this lecture, we will discuss DiGeorge Syndrome. 00:04 So DiGeorge Syndrome is a deletion of the 22q11 section of a chromosome. 00:10 It's a microdeletion. Most cases are de novo mutations. 00:14 They just precursely happen but 7% are inherited from an infected parent in an autosomal dominant manner. 00:22 This happens between 1 in 4,000 and 1 in 6,000 live births and it is also called velocardiofacial syndrome. 00:30 Let's go through it in detail. What are the symptoms? Patients most importantly perhaps can have thymic hypoplasia. 00:39 Basically, they have a failure of development of the third and fourth pharyngeal pouches. 00:44 This can result in a lack of thymus. 00:47 The lack of thymus then results in a T-cell deficiency and these patients with a loss of T-cell mediated immunity can suffer from infectious diseases that are taking advantage of their weakened immune system. 01:02 Also, they can have congenital heart defects and problems with the great vessels. 01:09 The way I like to think of these patients is midline defects right around the face and the chest wall. 01:15 The glands, the structures and the abnormalities all land in that central area. 01:21 So let's review the facial features and abnormalities of patients with DiGeorge Syndrome. 01:26 They can have hooded eyelids, a tubular-looking nose. 01:30 They may have hypertelorism where they are too wide apart. 01:34 The features can be subtle. 01:36 Remember in DiGeorge Syndrome there is a wide variability of penetrance. 01:41 A patient for example may only have a heart defect or may only have thymic hypoplasia but usually it's a constellation of symptoms. 01:50 So there's wide variability in their severity of presentation. 01:54 So let's review the systemic features of the problem. 01:59 I mentioned the immune deficiency already and that's the one that's often is the most concerning. 02:04 They also may have learning difficuties. 02:07 This happens in 70 to 90% of patients. 02:10 About three quarters of patients will have congenital heart disease and this can really be any kind of congenital heart disease but it's often seen. 02:20 About half of patients will have a period of hypocalcemia. 02:24 This maybe from their lack of parathyroid gland. 02:28 Remember, those central glands that are involved and a quarter will be at increased risk for psychotic disorders later in adolescence. 02:37 The reason for this isn't totally understood. 02:39 So if we suspect that the patient has DiGeorge Syndrome, how do we test for it? Well, we used to do FISH but right now in the United States, pretty much nobody is doing FISH for any reason at all. 02:54 We've moved on to a slightly less expensive microarray genetic testing. 02:59 We often are able to make a prenatal diagnosis in patients where there was a previous history of a child with DiGeorge and deletion may not be seen by karyotype so that microarray is important. 03:15 So what labs do we get in patients where we've made a diagnosis of DiGeorge syndrome? Well, the first is they really deserve an echocardogiam. 03:25 We'll do an EKG and an echo to have complete understanding of the cardiac physiology. 03:30 Remember, half of these patients will have an abnormality. 03:33 We will also assess their thyroid gland and their parathyroid gland by checking a serum calcium, a serum phosphate and a thyroid hormone panel. 03:46 Remember, those midline hormones are affected. 03:49 We will do an immune function evaluation to see if their thymus is aproblematic. 03:56 A CBC may show lymphopenia. 03:59 We can test directly for T and B cell subsets and we can check immunoglobulin levels. 04:06 Also, a chest x-ray may be valuable in that if we see a lack of thymus on that chest x-ray, that's a clue that that child may have a T-cell involvement. 04:14 Lastly, we'll screen the kidneys. 04:17 These patients can have abnormal kidneys as well. 04:20 How do we treat these patients? First of all, if they have a T-cell abnormality, we're going to avoid live vaccines just like with other patients with T-cell deficiencies. 04:33 We're going to treat any abnormal structure or anomalies as needed and if needed and early intervention and developmental evaluation is very important because of the high instance of problems with learning. 04:48 So we need to address those early and often and frequently. 04:51 That's my review of DiGeorge's Syndrome in children. 04:56 Thanks for your time.
About the Lecture
The lecture DiGeorge Syndrome by Brian Alverson, MD is from the course Pediatric Genetics.
Included Quiz Questions
Which of the following findings is most consistent with DiGeorge syndrome?
- Hypertelorism
- Hypercalcemia
- Multigenerational family history of DiGeorge syndrome
- Hyperthyroidism
- Increased bone mineral density
Which of the following is not a feature of DiGeorge syndrome?
- Humoral immune deficiency
- An incidence of about 1 in 6000 live births
- Microdeletion of 22q11.2
- About 7% inherited from affected parent
- Thymic hypoplasia
A child presents with ocular hypertelorism, tubular nose, cleft palate, hypocalcemia, and thymus hypoplasia. Which of the following diagnostic tests is most likely to confirm the diagnosis?
- Microarray genetic testing
- Biopsy of thymus
- Karyotyping
- Fluorescence in situ hybridization (FISH)
- Chest CT scan
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |