Playlist
Show Playlist
Hide Playlist
Development Regression, Neurocutaneous Disorders and Tuberous Sclerosis
-
Slides 13 PediatricNeuropathology Neuropathology II.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
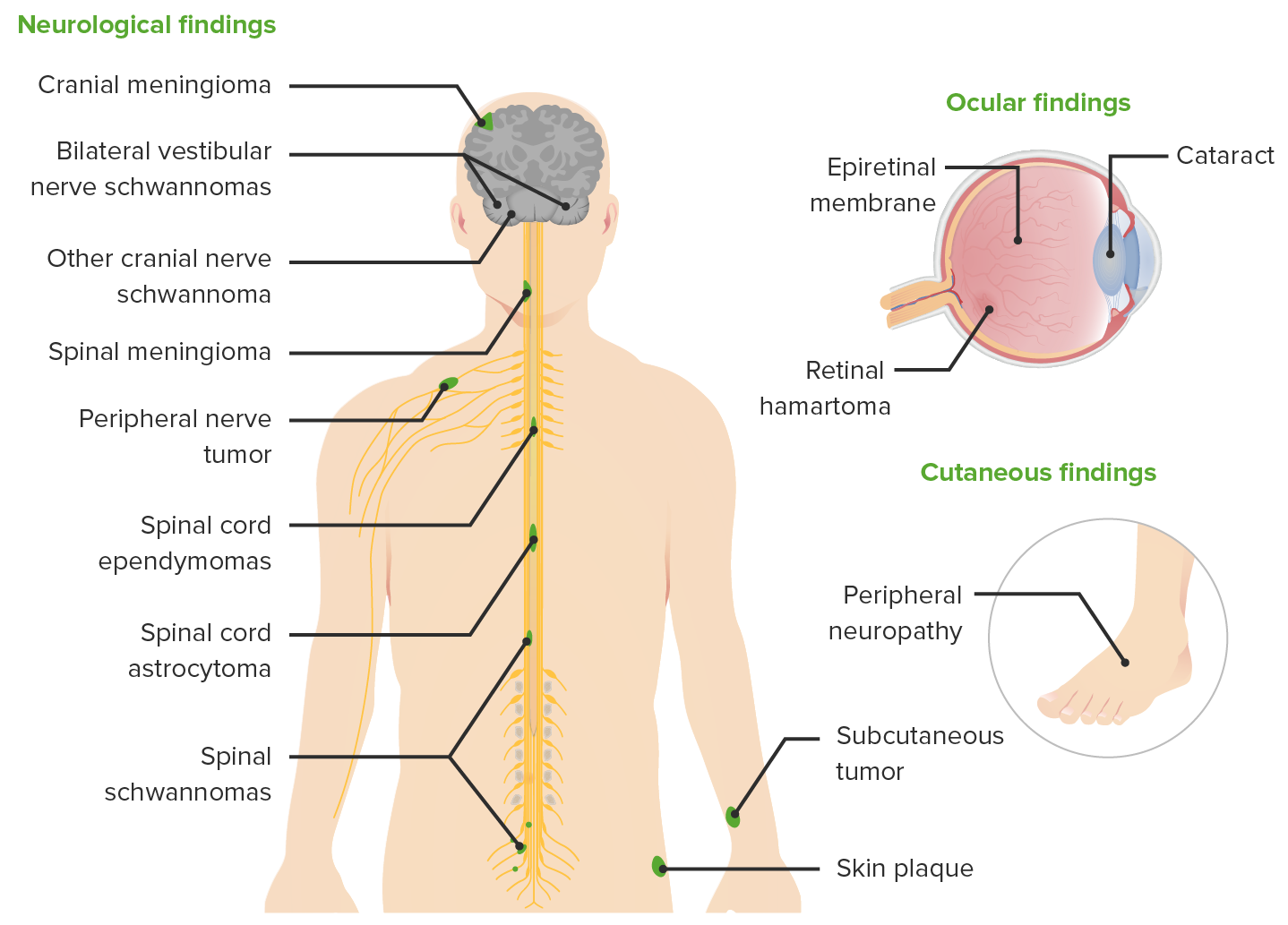
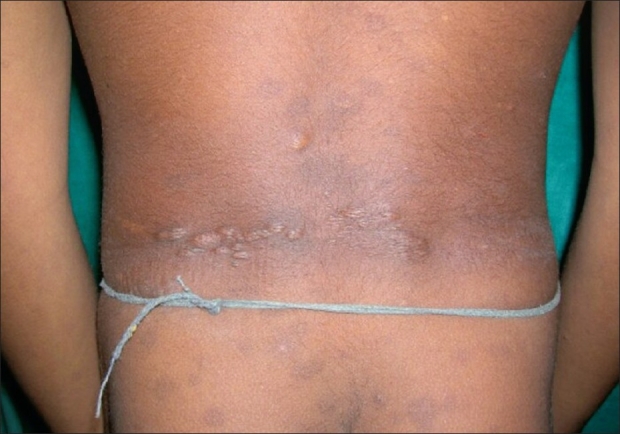
00:01 Developmental regression: Loss of previously attained developmental milestone. 00:06 So we’re going back from that milestone, back towards a primitive type of behavior. 00:11 Almost always has a bad prognosis, keep that in mind. 00:15 Onset age, before 2. 00:18 Here, you might be thinking about mitochondrial disorders including your mitochondrial encephalopathy, lactic acidosis, and stroke-like symptoms. 00:27 Hypothyroidism, cretinism. 00:30 Neurocutaneous disorders such as neurofibromatoses. 00:34 And gray matter disorder. 00:35 Remember, bad prognosis. 00:37 Onset before age of two. 00:39 White matter disorder, metachromatic leukodystrophy. 00:43 Amino acid metabolism such as PKU or phenylketonuria. 00:47 And enzymatic disorders. 00:49 These are developmental regression. 00:52 Clinical pearl, bad prognosis, here, referring to those differentials before the age of 2. 01:00 The neurocutaneous disorders that we’ll walk through quickly. 01:03 It’s called tuberous sclerosis complex. 01:06 Not tuberculosis, but tuberous sclerosis. 01:09 This is an inherited, hereditary issue. 01:13 Neurofibromatosis, specially we have neurofibromatosis type 1, which is known as your neurofibromin protein or neurofibromin 1 protein. 01:23 And with this, you’ve heard of Café au lait spots and so on and so forth. 01:28 Sturge-Weber. 01:29 In vascular pathology, with Sturge-Weber, you’ve talked about port wine syndrome. 01:35 Remember with Sturge-Weber, it’s a problem with the leptomeningeal blood vessels, and therefore may result in new onset seizure in this patient. 01:43 Familial telangiectasia or you’ve heard of hereditary, hemorrhagic telangiectasia, Osler–Weber–Rendu. 01:51 Von Hippel-Lindau disease. 01:52 Remember with Von Hippel-Lindau disease, you could have bilateral renal cell carcinoma in a very young patient. 02:00 Along with this, there could be hemangioblastomas of the cerebellum and the retina. 02:05 And we have incontinentia pigmenti. 02:08 And ataxia telangiectasia. 02:12 Let’s talk about tuberous sclerosis. 02:14 Autosomal dominant disorder To begin with, please understand that this has nothing to do with an infection. 02:21 Incidence: 1 in 10,000. 02:23 There are two gene loci. 02:25 You have TSC1 on chromosome 9. 02:28 Please memorize hamartin. 02:31 Now, with hamartin, you can play with that a little bit more and this is what I recommended to do. 02:36 You’ve heard of, in pathology, hamartomas and hamartoma would mean increased proliferation of cell, but completely, completely, non-neoplastic by definition. 02:47 With tuberous sclerosis, there are important hamartomas that may be seen. 02:53 And one of these hamartoma could be seen, well, perhaps in the heart. 02:57 What I’m saying is hamartin chromosome 9, at least know TSC1. 03:04 TSC2, T as in two and use that to your advantage with the gene tuberin, T. 03:13 At least know hamartin with TSC1 at this juncture. 03:18 The classic Vogt triad of syndrome include the skin lesions. 03:23 Our topic is under neurocutaneous and skin lesions include something like your ash-leaf spots, shagreen spots. 03:31 There might be convulsions and these are your tubers that you might find in the brain and there might be intellectual disability. 03:39 With tuberous sclerosis, things that you’re paying attention to, the primary symptoms cluster. 03:45 Remember that skin? In the skin, it’s called adenoma sebaceum, ungual fibroma, cortical tubers. 03:52 Those tubers will be found in the brain. 03:54 And we have subependymal nodules and multiple retinal astrocytomas. 04:01 The secondary symptoms: Infantile spasms. 04:04 The ash-leaf spot, as the name implies, will be white and it’s hypomelanotic macule. 04:13 And of course, that’s referring to blanch – I shouldn’t use the word blanch, but we’ll say pale and it would be hypopigmented. 04:23 In the heart, we have these rhabdomyomas. 04:26 Remember, in the heart, in cardiology, very rare that you might have a cancer in the heart. 04:33 However, if by chance you think of a benign tumor that might be located in it, and it’s a rhabdomyoma, then please know that this could be part of tuberous sclerosis, which is my topic. 04:45 Renal angiolipoma in the kidney. 04:48 And first degree relative with tuberous sclerosis complex or TSC. 04:54 And keep in mind once again, at least know TSC1, which then represents hamartin. 04:59 There is no condition that we see here, either primary or secondary, in terms of symptom that truly would be malignant, is there? No.
About the Lecture
The lecture Development Regression, Neurocutaneous Disorders and Tuberous Sclerosis by Carlo Raj, MD is from the course Pediatric Neuropathology. It contains the following chapters:
- Developmental Regression
- Neurocutaneous Disorders
- Tuberous Sclerosis
Included Quiz Questions
Which of the following conditions is associated with a spectrum of benign and malignant tumors, including clear cell renal cell carcinoma and hemangioblastoma?
- Von Hippel–Lindau disease
- Neurofibromatosis
- Osler-Weber-Rendu disease
- Hemorrhagic telangiectasia
- Tuberous sclerosis
Tuberous sclerosis may be caused by a mutation of TSC1 on which of the following chromosomes?
- Chromosome 9
- Chromosome 13
- Chromosome 22
- Chromosome 14
- Chromosome 8
The TSC1 gene codes for which of the following proteins?
- Hamartin
- Tuberin
- Fibrillin
- Neurofibromin
- Merlin
Which of the following is a tumor associated with tuberous sclerosis?
- Cardiac rhabdomyoma
- Angiosarcomas
- Fibrosarcoma
- Myxosarcomas
- Cardiac rhabdomyosarcomas
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |