Playlist
Show Playlist
Hide Playlist
Derma Case: 57-year-old Woman with Hypertension and Hair Loss
-
Slides Alopecia.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
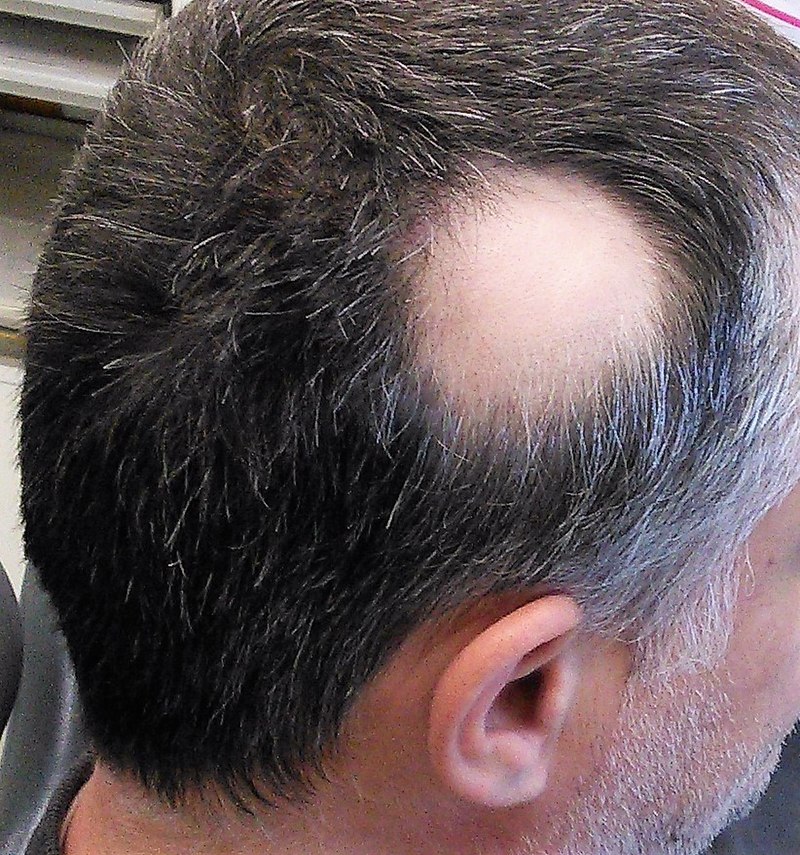
00:01 So let's jump into our case. 00:03 So this is a 57-year old woman with a history of hypertension who presents with a chief concern of hair loss. 00:09 She states that she's seen an increasing quantity of hair shedding once she takes a shower. 00:14 This has been fairly stable over the past 6 months but she's now concerned that her hair is just thinning out particularly on the top of her head. 00:22 Now she denies any pruritus or pain, there's no paresthesias on the scalp No recent trauma or surgery either. 00:28 She is anxious though about her hair loss, but otherwise reports no acute stressors. 00:33 She takes only hydrochlorothiazide and has not started any new medications lately. 00:38 There's no recent weight loss or fever or chills nor myalgias, no arthralgias. 00:42 A pretty benign review of systems. 00:44 Social and family history - there's no history of autoimmune diseases. 00:48 I mentioned the review of systems. 00:49 And when we performed our exam of the scalp, we see mild, diffuse, symmetric thinning of the scalp hair. 00:57 with no evidence of erythema or scaling or scarring. 01:00 A hair pull test that we mentioned before yields 3 hairs which is pretty normal There's no exclamation point hairs present and there are no nail findings. 01:13 So highlighting a few specific features, the time course sounds pretty indolent. 01:18 It's just been slowly stable for the past 6 months - nothing acute. 01:22 The pattern of skin involvement, it appears to be a symmetric involvement the scalp particularly on the top Regions of her scalp were the vertex of the scalp. 01:31 It doesn't look like any systemic involvement based on a completely negative review of systems. 01:37 And in terms of skin inflammation, we have none of those evidence, findings for erythema, scaling or scarring. 01:44 Alright, so which of the following is the most likely diagnosis? First off, alopecia angiogenetica. 01:50 Now that's a very fancy term for one of the most common causes of hair loss that there is. 01:55 Just basic male pattern or female pattern balding or hair loss. 02:00 It is a benign, common pattern of baldness seen in both men and for women. 02:04 With men it's most commonly in the vertical or the vertices of the scalp Whereas for women it may be a bit more diffuse. 02:11 It's mediated by androgens. 02:13 That's why it happens more on men than in women but it does happen over time in women as well. 02:17 As I said, it is the most common cause of hair loss. 02:20 We're certainly gonna consider it in our patient particularly with the lack of any inflammatory findings on exam. 02:27 This is pretty typical picture of a man with alopecia androgenetica. 02:33 So this picture in contrast shows very severe hair loss in just one discreet patch in contrast to the diffuse hair loss that we saw in the prior slide. 02:42 This is called alopecia areata. 02:44 Now this is an immune-mediated destruction of the hair follicles. 02:48 It's associated with a number of other autoimmune diseases, more commonly vitiligo, Hashimoto's thyroiditis or Addison's disease. 02:56 And essentially what's happening is an immune attack on the anagen follicles that are damaged, they transition to telogen phase and then very quickly to the exogen phase, Now you might think with an immune-mediated destruction of hair follicles, that you might see some scalp inflammation but it turns out that it's really happening at a microscopic level. 03:14 So you're not gonna see erythema or scaling or folliculitis or anything like that. 03:19 One thing that you may find on physical exam other than that discreet patch or several patches of hair loss is this finding called exclamation point hairs which is just an indication of deceased, broken hair cells at the site of prior hair follicles. 03:34 While most patients classically just have these little patches of hair loss, it is important to recognize that there are some very severe cases where all the hair cells on the entire body are being attacked and that's a condition called alopecia universalis where every hair cell has been wiped out and there's no eyebrows, no eyelashes, no hair on the scalp either. 03:55 Now our patient has mild diffuse hair loss rather than any dense patches so I think it's safe that we can x-out alopecia areata. 04:06 As we x-out alopecia areata, I do want to just draw your attention to the link between some hair loss etiologies and some nail findings. 04:15 For unclear reasons, you might sometimes see nail pitting or other forms of nail dystrophy in patients with alopecia areata Again, presumably an immune-mediated phenomenon. 04:24 So these nails can provide clues to a number of different diagnoses and we'll see that in one of the next diagnosis on our list. 04:31 Telogen effluvium. 04:33 So telogen effluvium is transient, diffuse hair loss cause by a systemic stressor, a variety of different stressors and we'll talk about in a moment. 04:41 What's happening is a premature shift from the anagen phase to the telogen phase and again to the exogen phase ultimately. 04:48 And usually what's happening is after an inciting event, it's 2-4 months later before you start to see the hair loss which can be very disconcerting for patients because the stressor was months ago and it's hard for them to associate that stressor with what's going on today. 05:01 Importantly however, you can reassure patient that spontaneous recovery should occur if it was simple episodic stressor and a few months after the initial loss of hair, it should start to regrow. 05:14 Most common causes or precipitants for telogen effluvium would be pregnancy, major surgery particularly bariatric surgery, severe illnesses of any sort, malnutrition, iron deficiency. varieties of hypo or hyperthyroidism, severe psychologcial stress not just feeling anxious about hair loss, and a number of different medications can do this as well. 05:37 Now we talked before about the association between nail findings and hair loss. 05:42 The same applies for telogen effluvium. 05:45 While stressors can manifest with telogen effluvium in the hair, it can also manifest as either palpable transverse ridges on the nail plate or what you call Beau's lines or as non-palpable alternating white and red transverse lines depicted here in the nail bed. 06:00 Those are called Muehrcke's line. 06:01 So again, just something else to look for on the physical exam when you're seeing somebody having hair loss. 06:07 Now in our case, our patient again does have diffuse hair loss but we're not getting any obvious precipitants, stil lwe should kepe it on the list for now. 06:17 The next one on our list s called Anagen Effluvium. 06:20 It simply stated this is just an extreme form of telogen effluvium with an abrupt loss of hair. 06:26 In contrast to waiting 1-3 months or 2-4 months after a stressor, this can happen over the span of a few days. 06:33 And the most common etiology is chemotherapies. 06:37 Promising interventions nowadays are to try and actually freeze the scalp during chempotherapy in order to try and avoid hair follicles from absorbing all those toxic chemotherapies, and hopefully mitigating some of the downstream anagen effluvium which used to occur relentlessly. 06:55 And so, we'll take that off of our list, we have to presume she would've told us if she's getting chemotherapy. 07:01 So that brings us to discoid lupus, which gets its own slide. 07:06 Discoid lupus erythematosus is a type of cicatricial alopecia. 07:11 Cicatriacial is a fancy word derived from latin which means scarring, a scarring type of alopecia. 07:18 Now it is a subtype of chronic cutaneous lupus. 07:21 Actually about 15-30% of patients with systemic lupus erythematosus will have discoid lupus. 07:28 And it is of higher risk in women, in African-Americans and in those ages 20-40, which doesn't really meet the demographics for our patient at all. 07:37 Patients with this type of lesion have well-demarcated, erythematous plaques with adherent scale. 07:44 So in contrast to our patient which has no evidence of inflammation, this is an inflammatory leison, it's not subtle. 07:51 It does have a predilection for this scalp but you may also see on the face where there wouldn't be hairloss, there would just be scarring and same wise with the neck. 08:00 What you can see in phyical exam is a slowly-expanding rim of inflammation leaving some depressed areas of central scarring where the hair may not grow back at all. 08:10 So this picture really doesn't look at all like what our patient presents with, so I think we can safely take this one off our list So let's revisit our case and highlight some of the most significant features. 08:22 Her age does support androgenetic causes, That is just female pattern baldness rather than any other immune-mediated etiology. 08:31 The typical location for alopecia androgenetica is again, on the top of her head which is consistent and the absence of pruritus, pain, or paresthesias on the scalp really steers us away from things like tinea or any of those cicatricial alopecias that we mentioned. 08:47 Likewise, we're not seeing any evidence of any stressors. 08:51 No trauma, no surgery, not starting any new medications, no recent weight loss to suggest malnutrition. 08:57 So that's gonna make telogen effluvium less likely. 09:01 And again, the absence of any autoimmune diseases, the absence of any exclamation point hairs, the absence of nail findings,and this diffuse picture, leads us away from alopecia areata, which would not typically look like this. 09:13 So barring any surprises, it looks like she's got a case of basic female alopecia androgenetica. 09:23 So let's talk about the treatment, how are we gonna help our patient out? The treatment for alopecia androgenetica is typically just topical minoxidil, oral finasteride or just reassurance. 09:35 It's obviously a benign condition. 09:38 The treatment for alopecia areata in contrast since this is an immune-mediated condition, would benefit from either topical or intralesional glucocorticoids. 09:46 You can also try Janus kinase (JAK) inhibitors. 09:49 Telogen effluvium, you can check some basic lab test like a TSH, maybe an iron panel but ultimately, you're just gonna avoid further triggers and further stressors and just reassure the patient that your hair's gonna grow back with watchful waiting. 10:04 Tinea captiis in contrast, you're gonna use a topical azole shampoo to try and eradicate the hair follicles there. 10:11 Some of these patients actually require systemic antifungal therapy. 10:16 And lastly, scarring alopecia You really just gonna try and treat the underlying cause, whether it's lupus or something else.
About the Lecture
The lecture Derma Case: 57-year-old Woman with Hypertension and Hair Loss by Stephen Holt, MD, MS is from the course Miscellaneous Skin Disorders.
Included Quiz Questions
Which of the following is a type of cicatricial alopecia?
- Discoid lupus erythematosus
- Alopecia areata
- Anagen effluvium
- Telogen effluvium
- Androgenetic alopecia
Which of the following is used in the management of androgenetic alopecia?
- Topical minoxidil
- Topical mupirocin
- Ketoconazole shampoo 20%
- Hydrochlorothiazide
- Topical corticosteroids
Which of the following is involved in the pathogenesis of alopecia areata?
- Immune-mediated hair loss
- Superficial fungal infection
- Chemotherapy-induced hair loss
- Androgen-mediated hair loss
- A premature shift from the anagen phase to the telogen phase
Which of the following is characteristic of telogen effluvium?
- It has a spontaneous recovery within 2–3 months.
- It has an abrupt onset.
- Well-demarcated erythematous plaques with central scarring is a typical morphologic pattern.
- It is treated with oral finasteride.
- "Exclamation point" hairs are present.
Which of the following is true regarding androgenetic alopecia?
- The vertices of the scalp are the primary sites of involvement in men.
- It is commonly associated with other autoimmune disorders.
- Nail pitting and nail dystrophy are commonly seen in association with androgenetic alopecia.
- Hair pull tests are typically positive in patients with androgenetic alopecia.
- Physical examination reveals signs of erythema, inflammation, and/or scarring.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |