Playlist
Show Playlist
Hide Playlist
Definition – Heart Failure
-
Slides 08 Cardiology Alpert.pdf
-
Reference List Cardiology.pdf
-
Download Lecture Overview
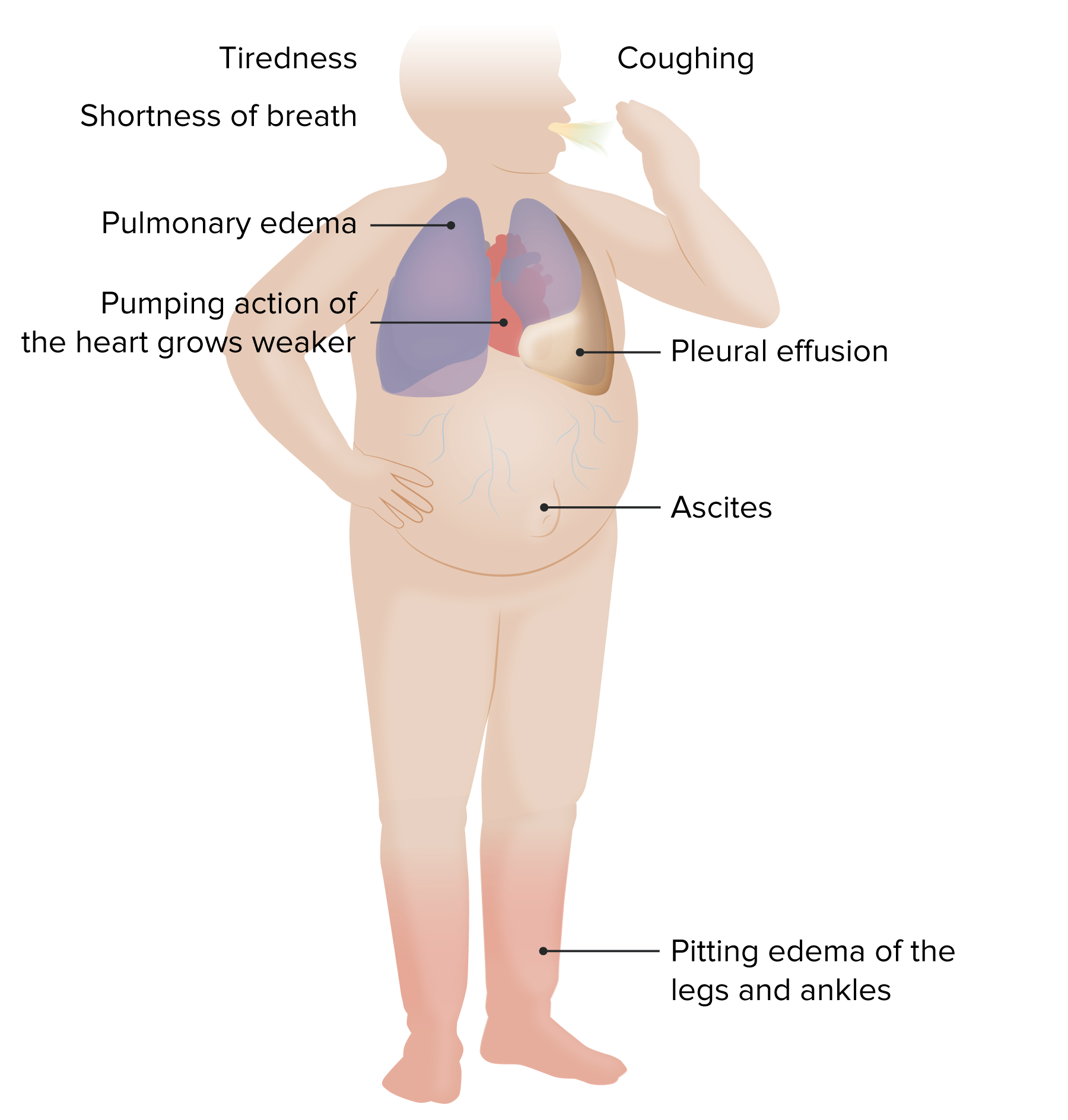
00:08 In this series, we are going to consider one of the most serious problems that faces a cardiologist; the patient with heart failure. 00:17 Heart failure is very common and increasingly common these days. 00:22 It's because it is a common complication of older individuals and of course the older population is increasing throughout North America and Western Europe as well as Asia. 00:33 Heart failure is defined differently in different circumstances by different cardiologist. 00:40 But basically, it's an inability of the heart to pump enough blood to meet the demands of the body. 00:48 In other words, if one exercises, one requires an increase in blood flow to the body. 00:53 And if you can't do that, you may develop the symptoms of heart failure. 00:57 As we're going to see, there are a number of compensatory mechanisms that gets set off in heart failure and some of them actually work to increase symptoms in these patients. 01:09 The major issue here is that the heart has an inadequate or decreased cardiac output. 01:16 Remember, cardiac output that's stroke volume times heart rate that is the amount of blood the heart puts out each beat times the heart rate. 01:25 And in this setting, what you see is that the patient has an increase in blood volume because of compensatory mechanisms that work to correct the heart failure state. 01:40 Unfortunately, this leads to fluid accumulation in the body and even edema; that is swelling in the body. 01:48 This can also be associated with circulatory congestion for example in the lungs, so you have increased fluid in the lungs. So the patients are short of breath. 01:59 And in addition, you may see patients being markedly fatigued because they're not getting adequate heart pumping. 02:08 As I said before, it's a very common problem. 02:10 There are more than 3 million patients in the United States with heart failure. 02:14 There's a number of new patients presenting every year. 02:18 And unfortunately, heart failure has a very poor prognosis. 02:22 Often, a prognosis just as bad as many forms of cancer. 02:27 Heart failure is more common in African-Americans and it's interesting that these patients seem to do better briefly when they're admitted to the hospital but their long term outlook is worse. 02:42 Some of this may be because of lower socio economic conditions in many African Americans. 02:50 The heart failure frequency in the US has been increasing with an increasing population. 02:56 A statistic I like to quote is, "The United States in every 24 hour period more people will become age 85 than will be born." So you can imagine if heart failure is a very common problem in the elderly just as atrial fibrillation is a common problem in the elderly. 03:13 Both of these are what I call "growth industries." And again, women tend to be a little less frequently affected by heart failure. 03:23 Men is a little more common early on. 03:26 But once we get into the geriatric population; above 65 to 70, the amount is about the same. 03:33 There are a number of factors that are referred to when we talk about heart failure and you'll remember some of these factors from the basic lectures on heart function. 03:44 Remember preload. Preload is filling of the heart so that it's a manifestation of the size of the ventricle when it fills up. 03:55 When you have increased blood volume, you increase the preload; that is the amount of volume that the heart has to squeeze out. 04:04 This happens with some of the compensatory mechanisms that increase the blood volume and consequently preload may be increased in the heart. 04:12 And what increased preload leads to is increased filling pressures in the ventricle during diastole, during the rest period. This leads to increased pressures in the ventricle during diastole. 04:23 And those increased pressures are transmitted back to the lungs and even back to the rest of the body leading to fluid accumulation in the tissues of the lung and the rest of the body. 04:36 Afterload is the work of the heart. It's the resistance the ventricle feels when it is pumping out. 04:42 This is usually due to resistance in the vascular system. 04:45 You'll remember that from the basic lecture in cardiology. 04:49 Increased peripheral vascular resistance leads to increased afterload, increased work of the heart. 04:55 You can imagine that's not good in heart failure and in fact, here's a clue. 05:00 When we talk about therapy of heart failure, one of the things is to decrease afterload. 05:05 To decrease the work of the ventricle and hope that it will recover from its depressed state. 05:11 There are two forms of heart failure: systolic and diastolic. 05:16 In other words, sometimes – let's take diastolic first. 05:21 Well, the ventricle squeezes all right, but it fails to relax normally. 05:27 It relaxes slowly or in a stiffened manner leading to increased pressure in there that gets transmitted throughout the circulation and leads to collection of fluid as we talked about before; edema. 05:39 Systolic heart failure is when the ventricle fails to squeeze well that can happen of course with the patient who's had heart attacks, happens to patients with cardiomyopathy, heart muscle disease and often systolic heart failure is associated also with diastolic. 05:55 So most patients with heart failure have both systolic and diastolic, but there is a whole group of patients or minorities you can see from the circle diagram here who have pure diastolic heart failure. 06:07 Interestingly, the long-term prognosis for diastolic heart failure is just as bad as for systolic heart failure. 06:14 Diastolic heart failure tends to occur in older individuals often with thickened heart muscle.
About the Lecture
The lecture Definition – Heart Failure by Joseph Alpert, MD is from the course Cardiac Diseases.
Included Quiz Questions
Which of the following refers to the passive stretching of heart muscle fibers prior to contraction?
- Preload (end diastolic ventricular volume)
- Cardiac inotropy
- Afterload
- Systemic vascular resistance
- Stroke volume
Which of the following statements represent preload most accurately?
- Preload is the passive stretch of the ventricle before contraction.
- Increased blood volume decreases the preload.
- Preload is a force opposing or stretching the heart muscle after contraction.
- Increased preload decreases filling pressure in the ventricle.
- Compliance of the ventricle cannot affect preload.
Which of the following terms describes diastolic heart failure most accurately?
- Heart failure with a preserved left ventricular ejection fraction
- Heart failure with a reduced left ventricular ejection fraction
- Heart failure with an increased left ventricular ejection fraction
- Heart failure with a varied left ventricular ejection fraction
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Clarísimo, la explicación es breve, clara y precisa. Me ha gustado mucho.
Nice topic and the speaker is good , he has the potential that all the listener is willing to hear what is he lecturing because his quality of voice and the quality of his teaching is an example of professional.
Clear voice Excellent expression Excellent representation Pointwise description Evident graphics
The explanations went direct to the point. Yes, I woul recpmment this lecture.
1 customer review without text
1 user review without text