Playlist
Show Playlist
Hide Playlist
Cushing Syndrome and Cushing Disease
-
Slides 01-02-01 Adrenal Pituitary.pdf
-
Reference List Endocrinology.pdf
-
Reference List Pituitary and Hypothalamic Disorders.pdf
-
Download Lecture Overview
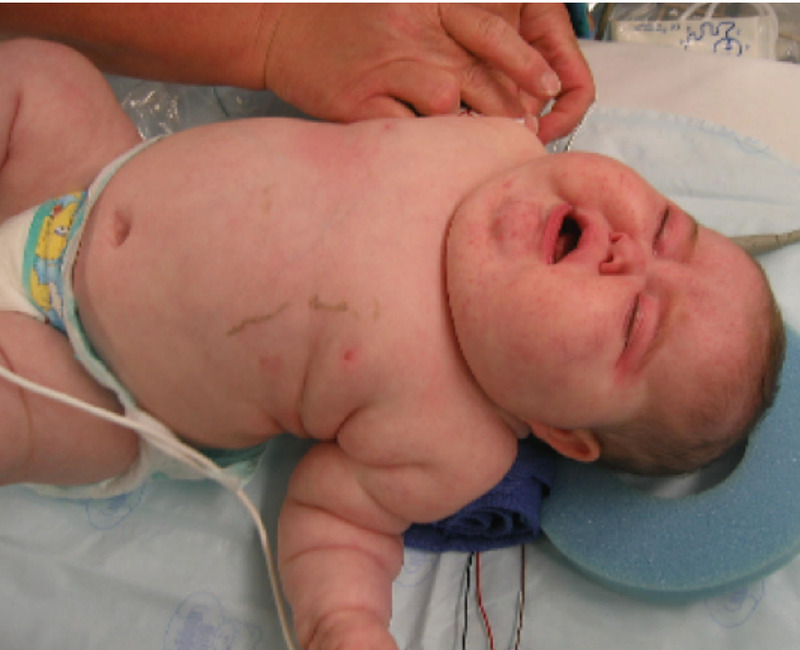
00:01 In this image, you can see some of the clinical findings we discussed. 00:05 On the left, we see her face, which is moon shaped. 00:09 She has evidence of hirsutism on her chin and on her cheeks. 00:14 On the image on the right, we see these reddish stretch marks in her lower abdomen, otherwise known as livid striae. 00:23 Striae are very specific, especially when they’re red, for the presence of Cushing syndrome. 00:29 What they signify is that the skin of the abdomen is stretching very rapidly, mostly related to the centripetal or central redistribution of fat in the abdomen causing the abdomen to distend acutely. 00:45 When this happens, the skin stretches, and as a consequence, stretch marks appear. 00:51 The red color is from damage to the capillaries as they expand rapidly producing the classic red or livid color. 01:00 Let's go through some of the classic findings in Cushing syndrome. 01:05 First of all, patients may present with weight gain, slow healing of cuts, an increase in the risk of infections, and fatigue, as well as glucose intolerance. 01:17 Psychological conditions that may accompany Cushing syndrome include depression, anxiety, irritability, loss of emotional control, and cognitive difficulties, and reduced libido. 01:31 As we saw in the prior image, a moon face may appear because of fat deposition around the face. 01:38 They may also manifest headaches. 01:42 The stem of the prior question talked about fat redistribution in the neck. 01:47 This is commonly called a buffalo hump. 01:51 Muscle weakness is a feature as well of the condition because of excess of cortisol. 01:58 In the skin, likewise, there is thinning, fragility. 02:02 There is the presence of acne on the face, and excessive hairiness otherwise known as hirsutism. 02:08 We've already addressed the striae and their etiology. 02:13 In terms of vascular conditions associated with Cushing syndrome, new or worsening of blood pressure is often noted. 02:22 The bones had also increased risk for fractures because of cortisol-mediated osteoporosis. 02:29 The reproductive system can also be affected, in which case, irregular or absent menstrual periods may manifest in females, and erectile dysfunction in males. 02:41 It's important to differentiate Cushing disease on the one hand from Cushing syndrome. 02:45 Crushing disease, which is pituitary in origin, is ACTH dependent where the ACTH causes excess cortisol production. 02:55 Cushing syndrome, on the other hand, is adrenal and ACTH is not responsible for excess cortisol production, as in the case we just saw where the patient's ACTH level was below five picograms per ml. 03:11 So, the patient in the prior example had Cushing syndrome as opposed to Cushing disease. 03:19 Excess cortisol production due to ACTH-secreting pituitary adenomas. 03:24 When undiagnosed, Cushing disease is associated with long-term morbidity such as diabetes, morbid obesity, hypertension, infertility, and osteoporosis. 03:39 Clinical features of Cushing syndrome include specific findings, less specific findings, and associated findings. 03:47 Starting with the specific findings, centripetal obesity, facial plethora which is redness of the face, supraclavicular fat pads, dorsocervical fat pads, and these wide violaceous or livid striae are pretty specific for the condition. 04:04 Some less specific findings from cortisol excess include easy bruising, excessive skin fragility, proximal muscle weakness, impaired memory, temporal balding, hirsutism or abnormal hair growth in women, and finally, menstrual abnormalities. 04:23 Associated conditions with the Cushing syndrome include osteoporosis, hypertension, diabetes mellitus, the presence of obesity, depression, electrolyte abnormalities such as hypokalemia, nephrolithiasis which are kidney stones, and the increased propensity to develop venous thromboembolism and pulmonary embolus. 04:48 Confirming the diagnosis of Cushing disease. 04:51 Dexamethasone is administered at 11 PM and cortisol is tested at 8 AM. 04:57 A pituitary source of ACTH will respond to negative feedback from high doses of dexamethasone suppressing cortisol to less than five micrograms per deciliter. 05:08 Ectopic sources of ACTH do not have suppression of cortisol. 05:15 This test has a relatively low sensitivity and a specificity of only 57% for Cushing disease. 05:23 Here is an algorithm that will help you confirm the diagnosis of Cushing syndrome. 05:28 We always start clinically where we suspect Cushing syndrome based on our history and physical exam. 05:34 The next step is to exclude that the patient is not taking exogenous glucocorticoids for some reason such as for severe asthma or in cases of intraarticular injections for joint pain. 05:47 Once this is excluded, perform initial lab testing with a 24-hour urine free cortisol, a one milligram dexamethasone suppression test, and a late night salivary cortisol level. 06:00 If these are abnormal, it is important to exclude the presence of physiologic hypercortisolism. 06:06 Once physiological hypercortisolism is confirmed, no further testing needs to be done. 06:13 If, however, physiological hypercortisolism is excluded, then additional testing should be performed, and this may take the form of additional imaging. 06:23 If these are abnormal, then we confirm Cushing syndrome. 06:26 If the additional testing is normal, repetition of the initial abnormal tests is indicated to rule out spurious positive results. 06:35 Alternatively, going back to the top of the algorithm, if the initial testing is all normal, Cushing syndrome is very unlikely. 06:44 Once ACTH-dependent Cushing syndrome is confirmed by chemically, a pituitary MRI should be obtained. 06:50 If no pituitary tumor or a tumor less than six millimeters is visualized, an MRI and an eight milligram dexamethasone suppression test is used to differentiate Cushing disease from an ectopic source of ACTH. 07:05 This is the so-called high-dose dexamethasone suppression test. 07:10 Ectopic ACTH production from a non pituitary tumor most often in the lung, pancreas, or thymus is still very uncommon. 07:19 Going through the treatment of Cushing disease. 07:22 Transsphenoidal pituitary tumor resection is probably the most curative plan. 07:28 Beware, however, of endogenous ACTH production in the remaining normal pituitary gland which will be suppressed after the removal of the tumor due to long-standing hypercortisolism, and that may require additional glucocorticoid replacement. 07:44 It may take up to one year for endogenous ACTH production to return to normal, and sometimes the hypothalamic-pituitary-adrenal axis does not recover. 07:56 If surgical cure is not achieved, pituitary radiation may be required. 08:01 Medical therapy requires the inhibitors of adrenal enzyme synthesis of cortisol like ketoconazole or metyrapone. 08:10 Dopamine agonists like cabergoline may be used and somatostatin analogues like pasireotide. 08:18 Medical cure of Cushing disease has a relatively low success rate. 08:22 But hypercortisolism symptom control is an achievable goal in all patients with endogenous Cushing syndrome.
About the Lecture
The lecture Cushing Syndrome and Cushing Disease by Michael Lazarus, MD is from the course Pituitary and Hypothalamic Disorders. It contains the following chapters:
- Cushing Syndrome
- Cushing Disease
Included Quiz Questions
Which of the following clinical features are most suggestive of Cushing syndrome?
- Moon facies, hirsutism, and livid striae
- Malar rash, hirsutism, and livid striae
- Moon facies, hirsutism, and exophthalmos
- Moon facies, exophthalmos, and livid striae
- Peritibial myxedema, malar rash, and livid striae
Which of the following clinical features are more characteristic of Cushing syndrome?
- Centripetal obesity and wide purple striae
- Centripetal obesity and impaired memory
- Centrifugal obesity and facial plethora
- Temporal balding and facial plethora
- Temporal balding and impaired memory
Which of the following tests may be used to screen for Cushing syndrome?
- Overnight dexamethasone suppression test
- Oral glucose tolerance test (OGTT)
- Water deprivation test
- Radioactive iodine uptake test
- Liver function tests (LFTs)
Where do the abnormalities causing Cushing disease and Cushing syndrome originate, respectively?
- Cushing disease: pituitary | Cushing syndrome: adrenal
- Cushing disease: adrenal | Cushing syndrome: pituitary
- Cushing disease: adrenal | Cushing syndrome: adrenal
- Cushing disease: pituitary | Cushing syndrome: pituitary
Customer reviews
3,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
1 |
Makes something hard easier. It is a good explanation and the presentation represents the most important points.
makes the topic way harder to understand even with the easiest topics.