Playlist
Show Playlist
Hide Playlist
Pain Management: Peptic Ulcer Disease, Kidney Disease, and Coronary Heart Disease
-
Slides Pain ChronicCare.pdf
-
Download Lecture Overview
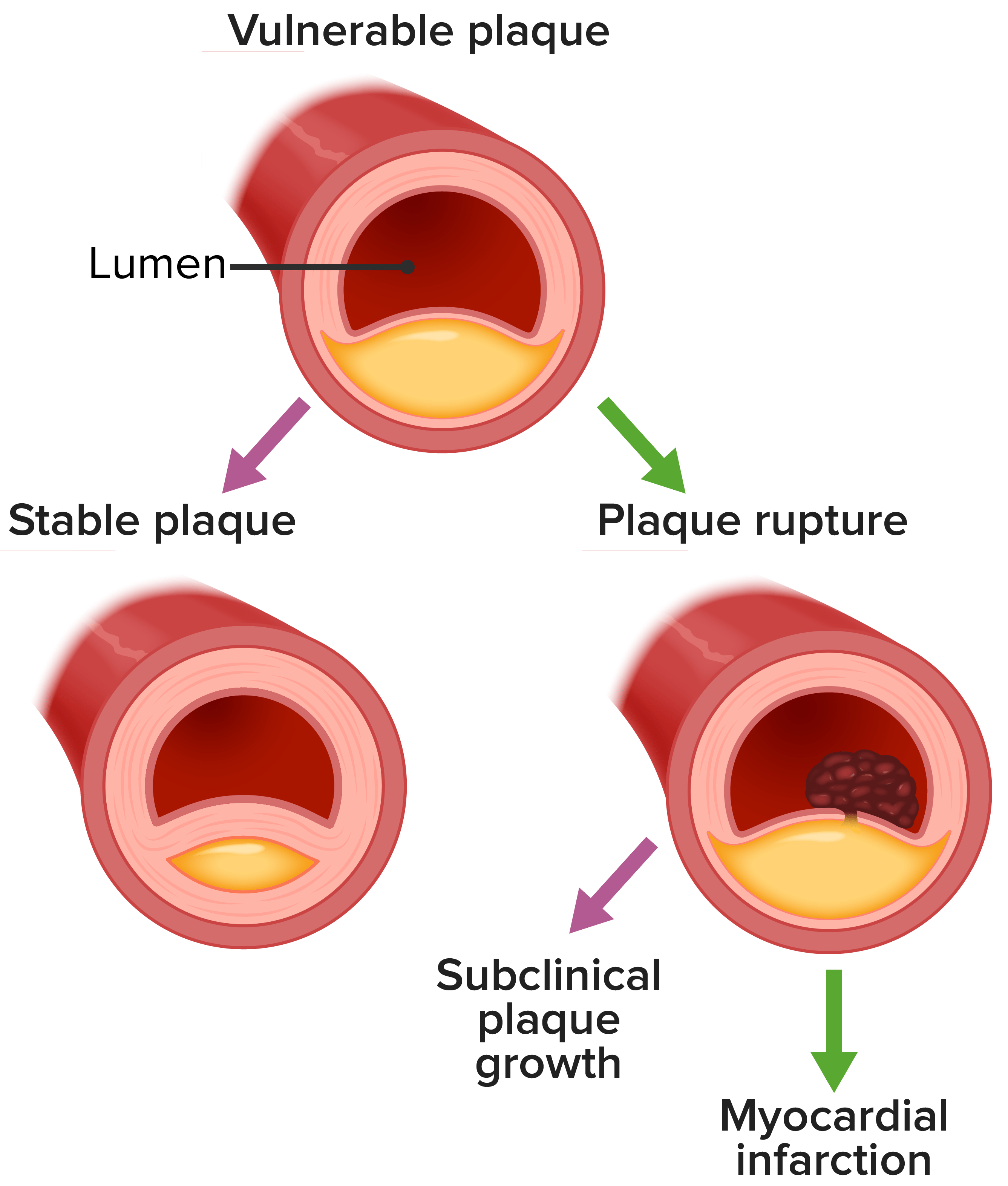
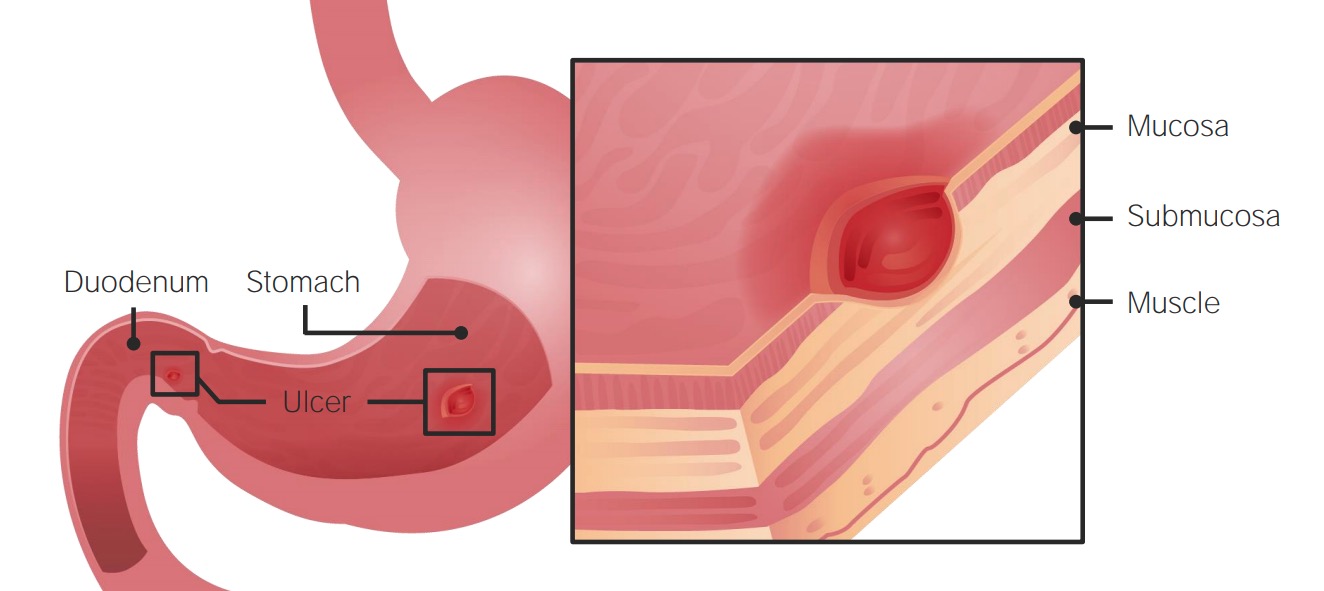
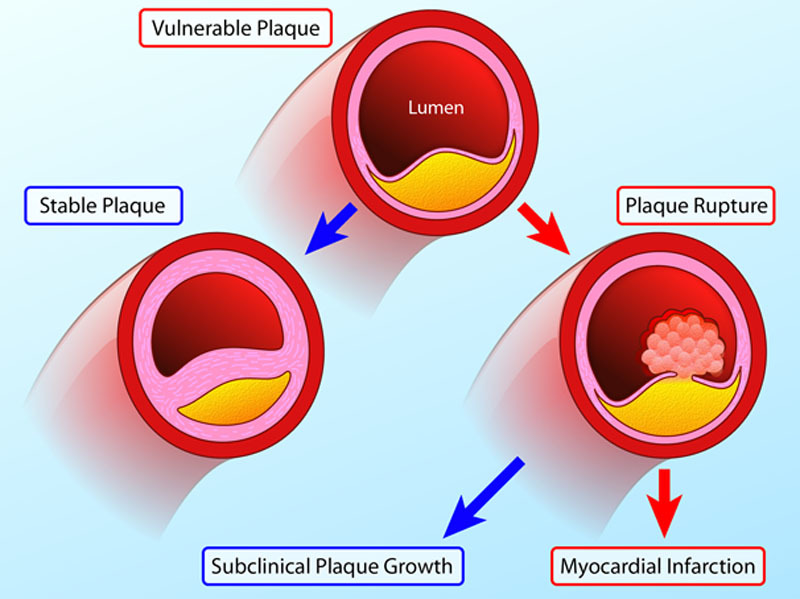
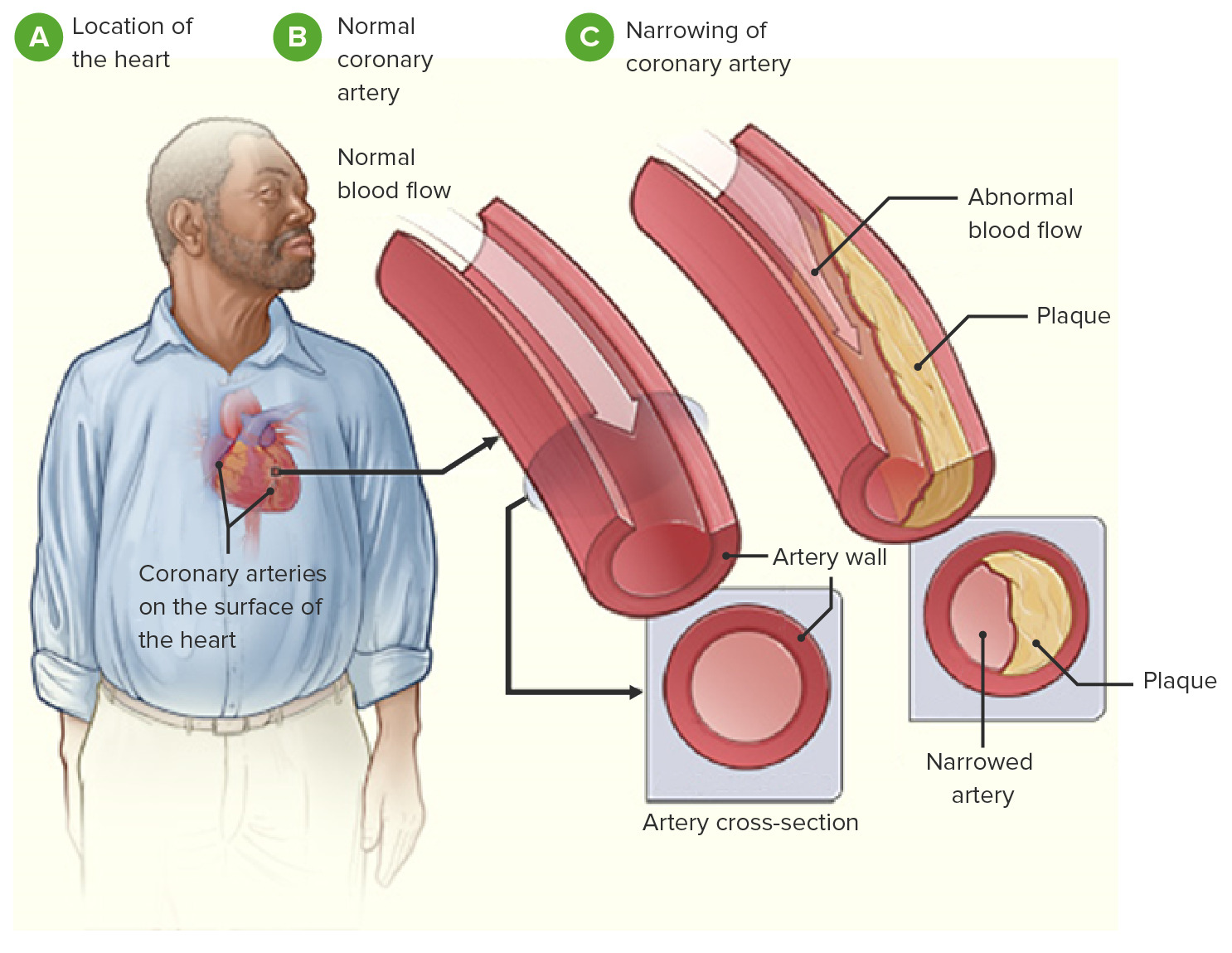
00:01 And just to pay attention to a few critical illnesses, as we think about treatment of mild to moderate pain, one is gastric ulcers. 00:09 There was a classic study that performed endoscopy on patients who have been taking NSAIDs, they found that there was some evidence of gastric ulceration in 30% of those patients. 00:20 Those aren't usually serious gastric ulcers that produce symptoms, but nonetheless we always have to be aware of chronic NSAID use and the risk for a gastrointestinal ulcer and gastrointestinal bleeding. 00:31 There is two opposing trends. 00:33 First of all, H. pylori has been more recognized and now more is being treated. 00:38 So, that's driving the rate of peptic ulcers down. 00:41 However, more people are using NSAIDs on a chronic basis, particularly older adults who are already at risk for ulcer. 00:48 That's driving the risk of ulcers up. 00:50 So, overall, the prevalence of ulcers has remained about the same. 00:56 They account for up to 2.5% of all admissions. 01:00 But if you talk to patients and ask them, has a doctor ever told you had peptic ulcer in the past? About 10% will say that they had that diagnosis in the past. 01:10 So, there’s a disconnect there between admissions and a broader number of patients who've been diagnosed with PUD. 01:17 Risk factors for peptic ulcer include older age, low educational attainment, low family income, history of smoking and, as I mentioned, chronic NSAID use. 01:26 And the one I think we can do most about as clinicians is chronic NSAID use. 01:32 What about kidney disease? So, there is a link between NSAID use and kidney disease, but that doesn’t mean that if you're a 28-year-old playing basketball and you sprain your wrist and you take ibuprofen for a week that you’re going to have a significantly increased risk of kidney disease. 01:52 That's not going to happen. 01:53 Young healthy people, it’s pretty safe to take intermittent NSAIDs. 01:56 However, among patients who are over 65, taking NSAIDs, instead of acetaminophen, is associated with 34% increase in the risk of renal impairment, and that is dramatically increased if coronary artery disease is also present. 02:13 So, really, be cognizant of older adults and adults with comorbid conditions that are frequently associated with kidney disease. 02:21 NSAIDs can really do damage to the kidney in those patients. 02:26 What about coronary heart disease? So, this is a study of nearly 62,000 adults, all of whom had a first-time myocardial infarction. 02:34 So, mostly men, mostly older, as you'd expect. 02:37 And so, what they're looking for here were two rates. 02:40 Among those patients with a myocardial infarction, what were the rates of bleeding among those who did and did not receive an NSAID after their myocardial infarction? What were the rate of cardiovascular events among those who did and did not receive an NSAID? And so, what they found not shockingly, their bleeding is in green here, that there was about twofold risk in the risk of bleeding among patients with -- who received an NSAID and had a history of myocardial infarction, but there was also a 40% increase in the rate of recurrent cardiovascular events associated with NSAID use as well. 03:18 So, this makes it appear that NSAIDs may promote a higher risk of repeat cardiovascular events among patients with known myocardial infarction.
About the Lecture
The lecture Pain Management: Peptic Ulcer Disease, Kidney Disease, and Coronary Heart Disease by Charles Vega, MD is from the course Chronic Care.
Included Quiz Questions
Which of the following is NOT a known risk factor for peptic ulcer disease?
- Chronic acetaminophen use
- Alcohol
- Helicobacter pylori infection
- Smoking
- Chronic NSAID use
Which of the following patients is at highest risk of developing renal impairment due to NSAID use?
- A 66-year-old woman with coronary artery disease who takes NSAIDs for shoulder osteoarthritis
- An 18-year-old soccer player using NSAIDs for pain relief for a sprained ankle
- A 60-year-old woman with on selective serotonin reuptake inhibitors for depression who uses NSAIDs for back pain
- A previously healthy 68-year-old Chinese immigrant who uses NSAIDs for intermittent headaches
- A 35-year-old man who drinks alcohol moderately and takes NSAIDs for tension headaches
Which condition is NOT at increased risk of developing because of chronic NSAID use?
- Stroke
- Peptic ulcer disease
- Coronary heart disease
- Renal impairment
Which of the following statements is LEAST ACCURATE?
- NSAIDS improve glomerular filtration rate.
- NSAIDS are associated with an increased risk of cardiovascular disease events in patients with cardiovascular disease.
- NSAIDS are associated with an increased risk of cardiovascular disease events in patients without cardiovascular disease.
- Peptic ulcer disease is associated with the consumption of NSAIDs.
- Aspirin use increases the risk of peptic ulcer disease.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |