Playlist
Show Playlist
Hide Playlist
Causes and Symptoms – Heart Failure
-
Slides 08 Cardiology Alpert.pdf
-
Reference List Cardiology.pdf
-
Download Lecture Overview
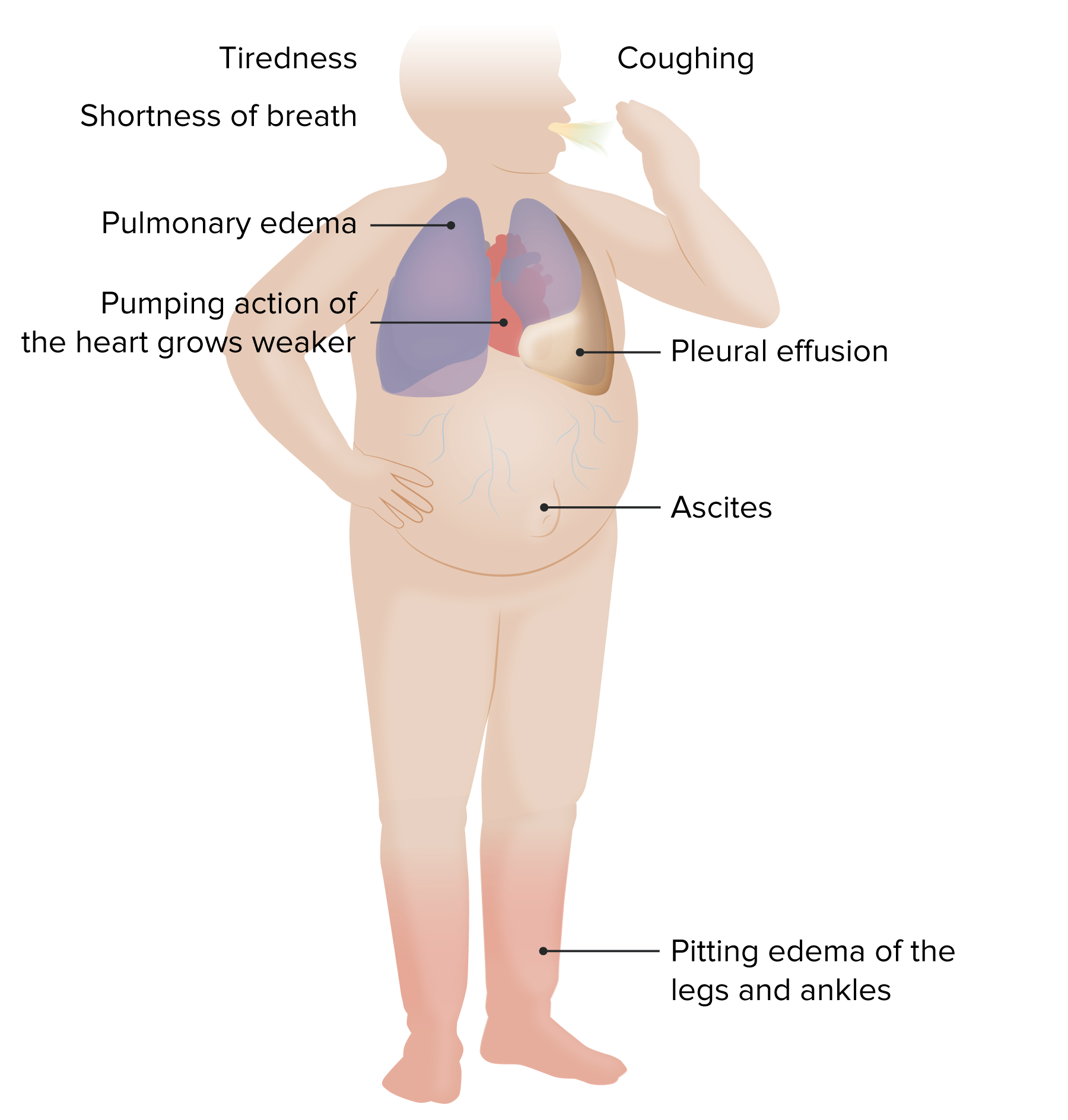
00:00 Now, it’s important to remember that heart failure relates to atherosclerosis, in the majority of cases who present to the cardiologist with heart failure. No surprise. Remember we talked about the last time, I spoke to you about the typical patient? That’s the commonest patient that comes to the cardiologist, the patient with atherosclerotic heart disease. 00:25 When that disease is advanced, particularly if the patient has had previous myocardial infarcts or heart attacks, the ventricular function is compromised and the patient shows up with heart failure. So, what are the risk factors for heart failure? They are the risk factors for atherosclerotic heart disease. They are hypercholesterolemia, hypertension, cigarette smoking, diabetes, all the things we talked about before that can lead to atherosclerosis. And you can see that the commonest ones, you know, are... problem leading to heart failure is ischemic heart disease, but there’s a number of other factors that are involved as well, but ischemic heart disease, the number one cause of death in the world, number one cause of heart failure. There are a number of rarer causes of heart failure. I’m not going to go into this in any detail, but for example, in the United States, one of the commonest causes of cardiomyopathy is excessive alcohol intake. Alcohol is a poison for the myocardium. Taking in small amounts, it’s good. Increases the HDL level, can be very pleasant in a social setting, but excessive alcohol can lead to cardiomyopathy and of course, a lot of other problems, liver failure from cirrhosis, etcetera, etcetera. 01:39 There are other things that can cause heart failure. We’ve talked about this before. 01:44 Cardiomyopathy from a chronic viral infection, certain drugs can do it. One of the favorite drugs for chemotherapy for breast cancer also damages the heart and some drugs… other drugs can do the same thing. And of course, arrhythmias with long standing fast heart rate that’s uncontrolled can also lead to cardiac fatigue. These things are much rarer. 02:05 Remember, ischemic heart disease is number one public enemy. 02:11 And here you just see all of the symptoms that patients will have with heart failure. 02:18 They will be dyspneic, that is they’ll be short of breath. You will find maybe their lips are blue because they’re not pumping enough oxygenated blood around. There may be heart murmurs as we had in the patient in the last lecture with aortic stenosis. 02:34 Sometimes on physical exam, you will hear a loud extra heart sound that says the ventricle’s really hurting. The patient’s breathing fast. You may hear actually sounds from fluid in the lungs and so forth. There’s a whole variety of physical findings that the doctor finds that confirms the diagnosis of heart failure. Remember from the last lecture, the most important thing are the symptoms, they give you the clue. 90% of the answer of the diagnosis is in the history, you then move to the physical exam. Oh yes, I’m hearing things, I’m seeing things that suggest that the reason the patient is tired, the reason the patient is short of breath, the reason the patient has swelling in their legs is because of heart failure. Right ventricular heart failure alone can cause a different set of symptoms and signs. Of course, the edema, the extra fluid is in the legs and you will remember that you may have problems in the abdomen because the increased venous pressure backing up is not only in the legs, but it’s also in the abdomen, the liver swells, there’s also swelling in the… fluid in the abdomen, patients may find their waist size gaining, they become very, very tired and often, you can even feel on physical exam this bulging abdomen that’s full of fluid. 03:59 Remember again, right heart failure? Much less common than left heart failure. Commonest cause of left heart failure - ischemic heart disease that is previous heart attacks. So, here’s a few diagrams that just show you what the cardiologist sees when they see a patient usually with very clear and significant heart failure. And you can see their pupils may be dilated from the adrenaline that’s circulating, the skin may be gray or pale or even blue, cyanotic and a whole bunch of things. They may be short of breath, breathing fast, they may be uncomfortable lying back and feel more comfortable breathing sitting up. There may actually be sounds in the lungs from fluid in the lungs, crackles or so called rales. 04:46 They may have a cough from the excess fluid that’s in their system. There is often increased pressure in the veins and you can actually see that in the neck. I’m going to show you a picture of that and the blood pressure maybe decreased because the cardiac output is down. And also, the patient may even have some discomfort in the abdomen, swelling and nausea and so forth. And of course, you may see bulging of the abdomen as I mentioned and edema that is swelling in the legs. All of these are not seen necessarily in one patient, but in individuals, you may see a number of these findings. And of course, patient's anxiety level is increased, of course, because they’re short of breath. One of the worst things that can happen to you is to be suffocated. It activates anxiety in a huge way. And again, you may see the fact that the patient has decreased oxygen saturation. Often we can test that with a little finger thing or an ear thing to see that the oxygen level in the blood is going down. The patients in advanced heart failure may be confused, particularly in elderly patients. There may be, as I’m going to show you a picture in a moment, the jugular vein is distended because of high filling pressures in the right atrium transmitted back to the jugular vein. There can… if the patient's had a heart attack, there may be chest discomfort in association with this. Of course, the patient is markedly fatigued and you may hear the heart sounds that I mentioned before. This extra heart sound, the heart may be increased in rate and again, you may feel swelling of the liver or the spleen from the venous congestion that goes back there. And of course, there’s decreased cardiac output if you measure that often with an echo and the pulse may be therefore weak. The patient is often cool… cool, the skin may be sweaty. 06:49 So, here’s a picture, that’s a lovely picture of a distended internal jugular vein. 06:56 You can see it rising up from just above the clavicle, the bone that’s right here on the front of the chest and you can see rising up almost to the level of the jaw. So, this is a patient with quite advanced heart failure. In this case, it’s a finding of right ventricular failure, but the commonest cause of right ventricular failure is often left ventricular failure that increases pressure in the lungs, increases the work of the right ventricle which eventually fails. So, this could be a patient with left ventricular and right ventricular failure or it could be somebody with isolated right ventricular failure. 07:31 And here, we see an example of peripheral edema, you can see you push into the soft tissue of the leg and you’ll notice that the impression stays when you take your finger away. So, this is a patient with advanced peripheral edema. It also looks to me like the skin doesn’t have its normal tone, its normal color. It looks gray and mottled and often this is because of decreased cardiac output.
About the Lecture
The lecture Causes and Symptoms – Heart Failure by Joseph Alpert, MD is from the course Cardiac Diseases.
Included Quiz Questions
Which of the following is the most common cause of heart failure?
- Ischemic heart disease
- Hypertension
- Valvular heart disease
- Endocarditis
- Arrhythmias
Which of the following is least likely to be seen in a patient with heart failure?
- Increased appetite
- Decreased urine output
- Dyspnea
- Heart murmurs
- Cyanosis
Which of the following is most likely in a patient with right-sided heart failure?
- Bilateral leg swelling
- Enlarged apex beat
- Pulmonary edema
- Narrow pulse pressure
- Aortic stenosis
Which of the following is least likely to be seen in a patient with heart failure?
- Jugular vein collapse
- Pulmonary congestion
- Decreased BP
- Ascites
- Anorexia
Customer reviews
4,7 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
This lecture is good because of in depth explanation of the signs and symptoms.
Excellent lecture! Very clear and easy to understand. Explanation easy to follow.
This was an excellent video! It was easy to understand and the professor did not overcomplicate what he was teaching.