Playlist
Show Playlist
Hide Playlist
Cardiac Case: 19-year-old Man with Central Chest Pain Worsening when Breathing
-
Cardiac Case 19-year-old Man with Central Chest Pain Worsening when Breathing.pdf
-
Reference List Cardiology.pdf
-
Download Lecture Overview
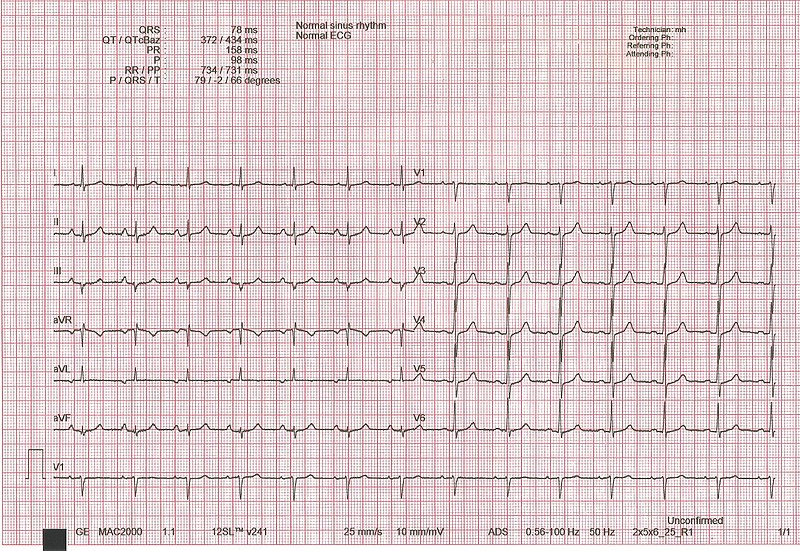
00:00 A 19-year-old college student comes to the emergency department complaining of severe central - that is right here in the center of the chest -- chest pain for the last 2 days. 00:10 It worsens whenever she takes a deep breath or when she lies down. 00:15 Personal history: there's no previous cardiac history, she's a vigorous exerciser 4 times per week for the last 2 years with no symptoms during or after exercise. 00:26 Her laboratory test shows slightly elevated white blood count. 00:31 The normal white blood count is less than 10,000. 00:33 She's slightly elevated at 11,200 and she has 10% of her lymphocytes are atypical. 00:40 Atypical lymphocytes imply a viral infection and she has a slightly elevated blood troponin. 00:46 Troponin being one of the parts of the myocardial machinery, contractile machinery. 00:52 When the heart's injured, troponin is released into the blood stream. 00:56 It can happen with a heart attack; it can happen because there's a car accident where the heart is bruised, or from many other things that can damage the heart. 01:05 So, what's critical in this history first of all, persistent chest pain which is pleuritic. 01:12 It's worse when she takes a deep breath and worse when she lies down. 01:15 And the laboratory is suggesting an infective or an inflammatory process. 01:21 And here's her electrocardiogram. 01:24 Please look at it and see what you believe is abnormal about this cardiogram. 01:36 In fact, this cardiogram shows diffuse ST segment elevation. In Lead 1, there's ST elevation. 01:44 Lead 2, there's ST elevation. Lead 3, there's ST elevation. 01:47 And also, in AVF and then across the precordium there's ST elevation. 01:52 So almost all the leads have ST elevation and there's no reciprocal ST depression implying ischemia. 01:59 The diagnosis is pericarditis probably following a viral infection. 02:06 Acute viral pericarditis, she had little echo that showed a little bit of pericardial effusion. 02:12 Generally, the echo is done to make sure there's not a large pericardial effusion but it's quite common to have a small pericardial effusion with viral pericarditis. 02:22 Turns out, there were no major findings of too much fluid on the echo. 02:30 If there were a lot of fluid, it can sometimes compress the heart and decrease the blood pressure and we would have to drain the fluid. 02:36 And the treatment is non-steroidal anti-inflammatories such as indomethacin or ibuprofen and colchicine as well. 02:45 And generally, the patients do extremely well over the next week or two. 02:49 If we had seen a lot of fluid and there was evidence that the heart was tamponading, that is the fluid was squeezing the heart and decreasing cardiac output, this would require a trip to the cath lab to drain the fluid from the heart so that the heart function would improve. 03:04 That's pretty rare. Almost always we're able to handle this with the drugs.
About the Lecture
The lecture Cardiac Case: 19-year-old Man with Central Chest Pain Worsening when Breathing by Joseph Alpert, MD is from the course Cardiovascular Cases.
Included Quiz Questions
A 19-year-old male is found to have viral pericarditis, with atypical lymphoctyes on peripheral blood smear. The atypical lymphocytes seen in this case imply which of the following?
- Infectious or inflammatory process
- Autoimmune disorder
- Myocardial infarction
- Cardiac tamponade
- Rhabdomyoma
Which of the following statements is incorrect?
- Outcomes for pericarditis are typically poor
- Troponin levels can increase any time there is damage to the cardiac tissue, even if it is secondary to trauma
- Cardiac tamponade would be treated with pericardiocentesis
- The typical treatment for uncomplicated pericarditis is an NSAID, such as indomethacin
- Pericarditis is often secondary to a viral etiology
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Dr. Alpert provides such a clear & concise overview about high-yield diagnosis & management strategies! Thank you for creating this very helpful lecture series!