Playlist
Show Playlist
Hide Playlist
Cardiac Anesthesia & Neuroanesthesia – Anesthesia for Special Operations
-
18 -Anaesthesia for special operations.pdf
-
Download Lecture Overview
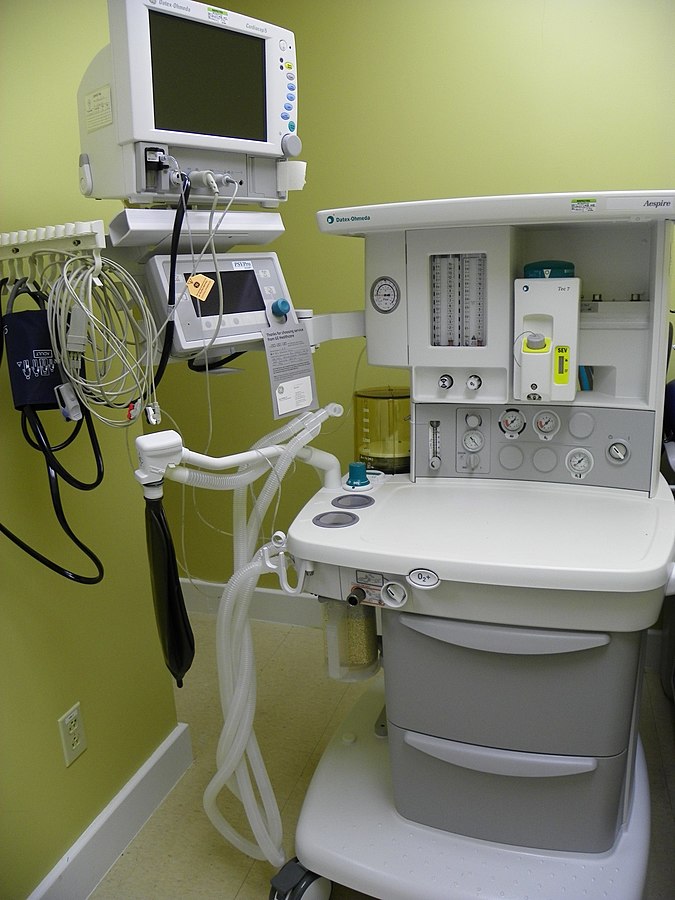
00:00 We're going to move now to Cardiac Anesthesia, which is a very common type of anesthesia nowadays, but is a very unique form of anesthesia. 00:08 In cardiac surgery, in open-heart surgery, the cardio-pulmonary bypass machine, which is shown in this picture, and which is operated by a highly skilled member of the team called a perfusionist, basically bypasses the patient's own heart and lungs. And it takes blood from the central circulation, through the machine, warms it, filters it, oxygenates it, sends it away to the brain, the kidney, the rest of the body, and completely bypasses the lung and the heart. And this leaves the surgeon with a heart that's immobile. And it makes it much easier to do the surgery if the heart is on standby. Some surgeons however prefer to have a beating heart and it is possible, under certain circumstances, to keep the heart beating and still do surgery on it. That's not the commonest way of doing it. The anesthesiologist is responsible for managing the patient while they're on cardio-pulmonary bypass. 01:08 The surgeon is responsible for preserving the myocardium while the patient's heart is at rest. And the way this is done is one of two ways. Either very cold solutions with high potassium are forced through the coronary arteries. This causes cardioplegia, it causes the heart to stop working because of the high potassium. And the cold just cools the heart and reduces its oxygen demand. The other way of dealing with this is, again using high potassium solution, but this time blood, forcing it through the coronary arteries, and that'll stop the heart. And because you're putting blood through the heart, you're actually supplying oxygen to a heart that, because it's immobile, really doesn't have very high oxygen demands. 01:56 The critical phase in cardiac surgery is Coming Off Bypass. 02:02 And this is usually managed by the anesthesiologist, although there tends to be a fair amount of back and forth discussion going on between the surgeon, the anesthesiologist, and the perfusionist at this time. 02:14 So these are just some valves that are replaced during open heart surgery. The top valve is a metal valve. And the advantage of a metal valve is that they're tough and they will last for 20, even 30 years. So, if you're a young person requiring valve surgery, you want a metal valve, because you don't want to come back again for as long as you possibly can. The negative with metal valves is that clots tend to form on the valves, so patients have to be anticoagulated for the rest of their lives. They have to take anticoagulation every day for the rest of their lives. And some people find that a totally intolerable situation. 02:50 The lower two valves in this picture are tissue valves. They could be bovine, or they can be pig valves. And they're much safer in terms of embolic phenomena, they simply don't cause embolic phenomena, so you don't need to take anticoagulation. The negative with these valves unfortunately is they don't last as long as the metal valves. 03:14 And they often need to be replaced every 10 years or so. And repeat cardiac surgery is infinitely riskier and more complex than first time cardiac surgery. 03:26 The scarring that goes on in the chest after cardiac surgery is unbelievable. So getting back in and finding the portion of the heart you need to operate on can be extraordinarily challenging. 03:38 So the anesthesiologist is responsible for protecting the heart prior to cardio-pulmonary bypass, which is particularly critical if the patient has ischemic heart disease, or is unstable. We have to be very careful to control tachycardia, and more importantly, not to cause tachycardia. Because tachycardia increases cardiac work and requires increased oxygen supply to the heart. If you've got ischemic heart disease, it means the vessels into the myocardium are blocked, so you can't increase oxygen supply to the heart. So you must keep the heart rate slow. Frequently, very potent inotropic drugs such as norepinephrine, epinephrine, dobutamine, dopamine and milrinone are given in bypass and coming off bypass. Anticoagulation is required during bypass, because the actual bypass tubing in the cardio-pulmonary bypass machine tends to induce clotting. And the last thing you ever want to see, and I'm thankful I have never seen it, is a generalized clotting forming in your cardio-pulmonary bypass. That's a fatal event. So we give very high doses of anticoagulant. And the drug we use is heparin. So these patients are very prone to bleeding. Once the patient's off cardio-pulmonary bypass, we reverse the heparin. But by then, there's been some damage to platelet, there's been some dilution of clotting factor, so bleeding is not uncommon. When we wean patients from bypass, they are sometimes extremely unstable. And it's our job as anesthesiologists to monitor and manage that during the transfer to the Cardiac Surgical Intensive Care Unit, and usually for the first few hours in that unit. 05:26 Once the patients are stable, we can consider discontinuing ventilation, which has been continued following the surgery. And usually they stabilize over about 4 hours and we can usually extubate them later in the day of their surgery, and have them transferred to the Cardiac Ward the following day. I spent 20 years as a Cardiac Anesthesiologist, and the changes that occurred during that 20 years were phenomenal. 05:56 The rate of damage to patients dropped dramatically, and the preservation of the myocardium improved dramatically. So death on the table and death immediately following, or nearly following surgery has become really quite uncommon.
About the Lecture
The lecture Cardiac Anesthesia & Neuroanesthesia – Anesthesia for Special Operations by Brian Warriner, MD, FRCPC is from the course Anesthesia in Special Situations. It contains the following chapters:
- Cardiac Anesthesia
- Neuro Anesthesia
Included Quiz Questions
Which description applies to cardiac surgery and anesthesia?
- Often requires isolation of the heart and lungs by cardiopulmonary bypass
- Is associated with a high incidence of "death on the table"
- Has never been complicated with "recall"
- Uses anticoagulation to prevent bleeding during surgery
- High doses of calcium are used to stop the heart
Which description applies to neurosurgery?
- Can often be done under local anesthesia and sedation
- Always requires general anesthesia for adequate control of pain and awareness
- Like cardiac surgery, requires intraoperative anticoagulation
- Is never associated with failure to awaken
- Is always associated with recall.
How is myocardial damage prevented in open heart surgery?
- By increasing potassium and cold solutions infused in the coronary artery
- By increasing sodium infusion
- By increasing magnesium infusion
- By increasing calcium infusion
- By increasing potassium and magnesium infusion
Why is a metal valve prosthetic preferred?
- Lasts for 20 years
- Has fewer allergic reactions
- Does not require anticoagulant
- Requires anticoagulant
- Is easy to implant
What is the effect of ketamine on ICP?
- Increases it, which is not beneficial
- Decreases it, which is beneficial
- Increases it, which is beneficial
- Decreases it, which is not beneficial
- Does not affect the ICP
Which of the following is NOT a complication of neuroanesthesia?
- Decreased ICP
- Massive hemorrhage
- Stroke
- Increased ICP
- Failure to awaken from anesthesia
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |