Playlist
Show Playlist
Hide Playlist
Congenital Adrenal Hyperplasia (CAH) in Children
-
Slides CAH Pediatrics.pdf
-
Download Lecture Overview
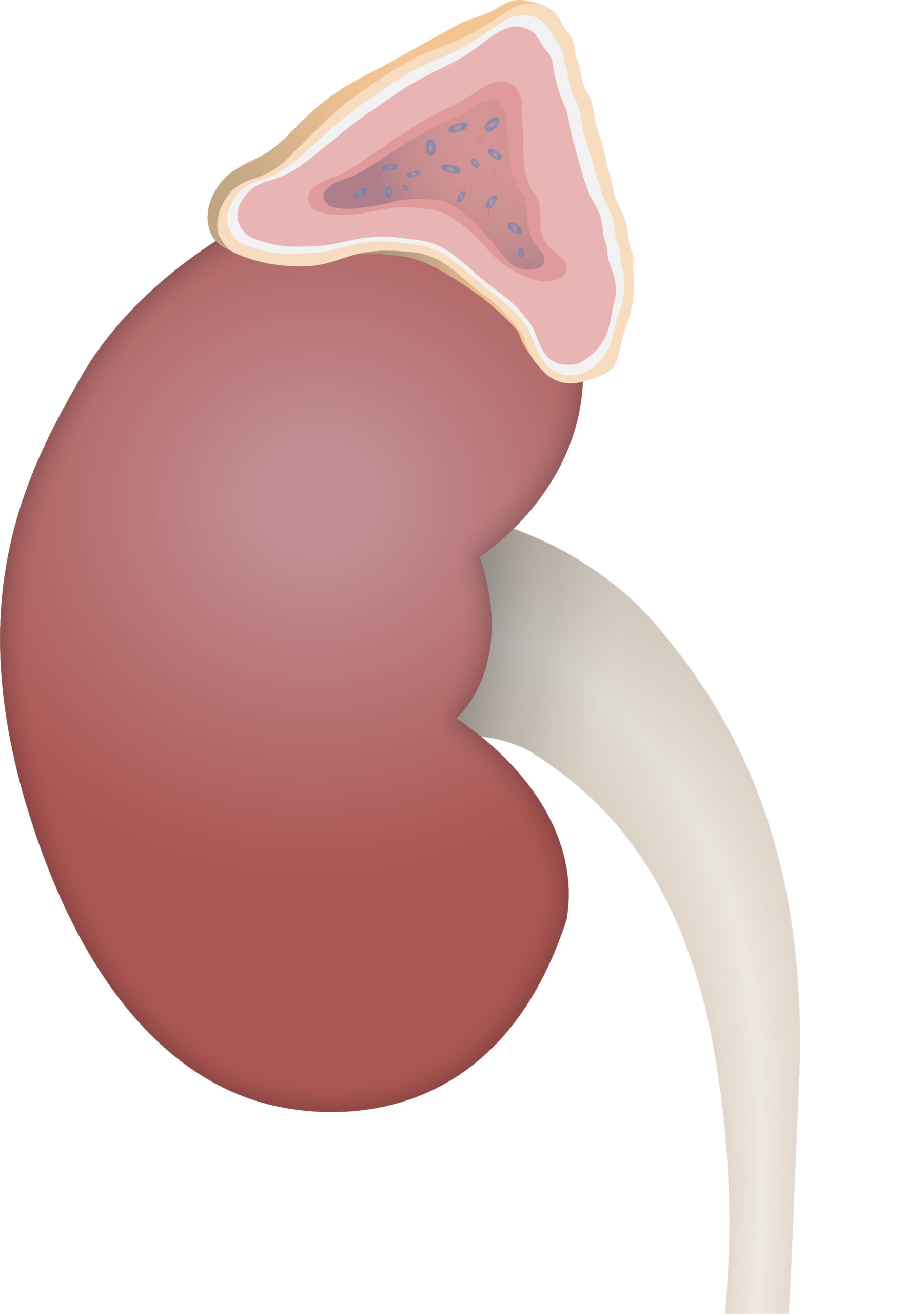
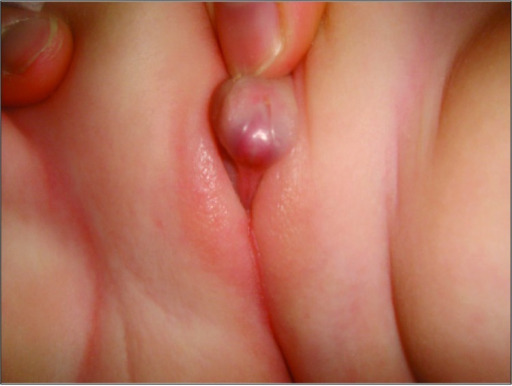
00:01 In this lecture, we're going to discuss Congenital Adrenal Hyperplasia. 00:06 Here's the classic case. A baby is born to a G1P1 completely healthy mother. 00:12 And on exam, you happen to notice this. 00:15 On your exam, the genitalia are abnormal looking. 00:20 What do you suspect? So this is a classic case of a female infant with congenital adrenal hyperplasia. 00:28 You can see that their genitalia are masculinized. 00:30 She has a large clitoris and she has a partly fused labrum. 00:36 So what's your next step? Well, let's pause first and ask ourselves, what exactly is congenital adrenal hyperplasia? Well, the cells are hyperplastic. So it's a large adrenal gland, but the problem is a deficiency of an enzyme. 00:54 This is a lot to remember from your basic physiology course. 00:58 But as we can remember the pathway is steroid synthesis includes these three main branches. 01:06 A branch which is going towards your glucocorticoids. 01:11 A branch that is going to your mineralocorticoids. 01:14 And a branch that is going on the right side of the slide to the sex hormones. 01:21 The most common enzyme that is deficient in these patients, is 21-alpha-hydroxylase deficiency. 01:28 So these patients are going to have an inability to move hormones in their development down towards the glucocorticoid and mineralocorticoid area. 01:39 And as a result, these steroids will get shunted over into the sex steroids synthesis pathway, and these patients will have excessive testosterone. 01:49 So less cortisol, less mineralocorticoid and more sex hormone. 01:55 When we see these kids, there's really two aspects to them that we have to worry about. 02:01 The most surprising and immediate when they come out of the womb, especially if it's a girl, would be any genitalia malformation. 02:08 As a result of being exposed to too much testosterone in urethra. 02:12 But the most concerning thing is the lack of mineralocorticoid. 02:17 In that these patients will become salt wasters. 02:21 They will be losing sodium. 02:23 Let's just remember for a second how mineralocorticoid works. 02:28 Remember mineralocorticoid will cause a retention of sodium into the blood, and will spit up potassium into the urine as a counter exchange, because after all we have to keep ourselves electrically neural. 02:45 That potassium, because there's three sodium is going out, and only two going in, in that pump which is powered by ATP. 02:52 An extra potassium will go through into the cell from the blood to maintain electrical neutrality. 03:00 These sodium?s and potassium?s are then freely exchange into the urine as well. 03:06 So the pump which is driven by ATP and stimulated by mineralocorticoid is really doing the whole thing. 03:13 So there are a couple of different ways these children can typically present. 03:18 The classic form is one in 15,000 and these patients can present either a salt wasters, which is about 75%, or simple virilizing, where they have less of the mineralocorticoid effect, and mostly are just virilized as a result of the sex hormone. 03:40 The non-classic form is typically milder, a little bit later onset, and they can have virilization even after birth. 03:49 So let's get into the clinical presentation of these patients. 03:55 Like I said, most common of these patients have 21-hydroxylase deficiency. 04:01 They may have a mutation in the CYP21A2 gene. 04:05 Generally, the shunt of hormone into that testosterone pathway causes virilization. 04:13 This means that males may be missed, because they're already virilized. 04:18 And females may look like males or have fused labia and clitoromegaly. 04:24 The salt wasting if present can be severe. 04:28 It's usually seen in the first 4 weeks of life with profound dehydration and maybe even shock. 04:34 What's also key and this makes sense if you think about it, is these patients may become hyperpigmented, from an increase expression of ACTH, because they're lacking the negative feedback loop of the steroids on their brain. 04:50 So how do we know they have this disease? Well, on electrolytes, we will see as you might expect a low sodium, they are wasting their sodium. 05:01 A high potassium, they are retaining their potassium. 05:04 And sometimes a metabolic acidosis, mostly because of severe dehydration. 05:10 They may have ketones from starvation or they might just have lactic acid from inadequate perfusion of any organ tissues. 05:18 Their hormone levels, they should have an elevated 17-hydroxyprogesterone. 05:23 They should have elevated androstenedione. 05:26 And they should have elevated adrenal androgens, such as testosterone. 05:31 If they fit this picture, we can then send a generic profile and see that they in fact have a CYP21A2 mutation. 05:40 We will also want to image these children to see to what extent they're having problems with their genitalia and the development of those genitalia. 05:48 So we'll generally get an MRI, where an ultrasound of the genitalia to look for Mullerian duct malformations. 05:54 For older children with later onset congenital adrenal hyperplasia, we need to check for increase growth, precocious puberty. 06:02 And often, in older kids, we'll get a bone age as well with hand x-ray to correlate their growth spurt and their bone age. 06:11 In congenital adrenal hyperplasia, the management, we need to replace the steroids. 06:17 These patients will go on glucocorticoid replacement therapy and mineralocorticoid replacement therapy. 06:24 We often ask patients add extra salt to food for those who were salt-wasters. 06:32 We need to give stress dose steroids for all these children when they become sick. 06:38 Let me be clear, the issue is, is that when we are normally sick, normal, healthy individuals, we raise our indigenous steroid levels for a variety of reasons. 06:50 If we are incapable of raising those steroid levels, we're at risk for shock. 06:54 So these patients who cannot make their own steroids need to have their steroids artifically raised by increasing their medication when they're feeling sick, or they are at risk for shock. 07:07 In patients, we will often do surgery, to try and fix the genitalia abnormalities that are present. 07:15 Girls will have a feminizing genitoplasty as needed. 07:20 Careful monitoring of steroid levels is important, because if we over treat we put these children at risk for Cushing's syndrome. 07:28 So these patients are usually followed by an endocrinologist to monitor and make sure things were going okay. 07:34 That's everything I have for you today, about congenital adrenal hyperplasia. 07:39 Thanks for listening.
About the Lecture
The lecture Congenital Adrenal Hyperplasia (CAH) in Children by Brian Alverson, MD is from the course Pediatric Endocrinology. It contains the following chapters:
- Case Study
- Pathology
- Diagnosis & Clinical Presentation
- Management
Included Quiz Questions
Which enzyme is MOST COMMONLY deficient in a patient with congenital adrenal hyperplasia?
- 21-alpha-hydroxylase
- 11-deoxycorticosterone synthetase
- Pregnenolone lyase
- 17-hydroxy pregnenolone synthetase
- Androstenedione synthetase
Which of the following is the most likely combination of laboratory test findings in congenital adrenal hyperplasia?
- Decreased serum sodium, increased serum potassium, metabolic acidosis
- Decreased serum sodium, increased serum potassium, metabolic alkalosis
- Decreased serum sodium, decreased serum potassium, metabolic acidosis
- Increased serum sodium, increased serum potassium, metabolic acidosis
- Increased serum sodium, decreased serum potassium, metabolic alkalosis
Which of the following is NOT seen in congenital adrenal hyperplasia?
- Newborn gynecomastia
- Mullerian duct malformations
- Salt-wasting
- Hyperpigmented skin
- Metabolic acidosis due to dehydration
A 10-year-old girl comes in with a sudden growth spurt, as indicated by her mother. She also says her daughter's breasts have started to develop. You suspect late-onset congenital adrenal hyperplasia. Which of the following should be the next step?
- Check bone age with hand X-ray
- Obtain X-ray of the knee joint
- Order a bone scan
- Schedule a hysterosalpingography
- Reassure the mother
Which of the following is NOT a management option for congenital adrenal hyperplasia?
- ACE inhibitors for salt wasters
- Mineralocorticoid replacement therapy
- Adding salt to food
- Stress steroids
- Feminizing genitoplasty
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
It really clarifies a topic which was not clear for me before. Now I have a clear concept of it in my head. Thank you!
This lecture is very clear. It helps to understand the physiology of the disease