Playlist
Show Playlist
Hide Playlist
Traumatic Brain Injury: Introduction
-
Slides Head Trauma Traumatic Brain Injury.pdf
-
Download Lecture Overview
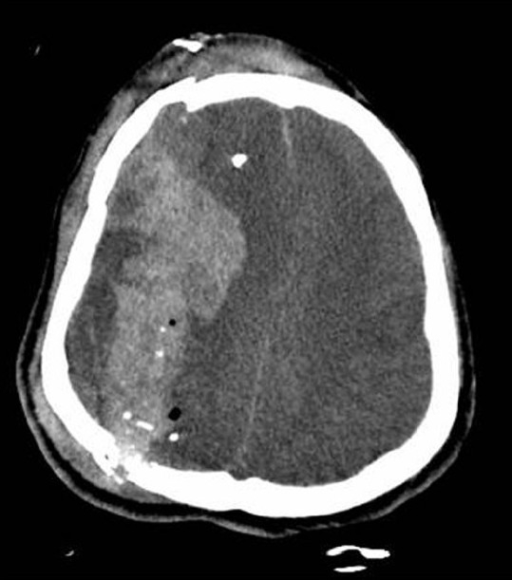
00:01 Now let's talk about traumatic brain injury specifically. 00:05 And let's go back to a case. 00:07 This is a 68 year-old man with no significant past medical history who presents to the emergency department with progressive altered mental status. 00:16 The patient initially fell from a ladder in his home 4 days ago. 00:19 His family says that he appeared normal after the fall, and over the past few days has become progressively weaker, began to trip on his right leg and have difficulty using his right arm. 00:31 Today, the patient became progressively more confused and has not been speaking. 00:36 On examination, he's awake and his eyes are open spontaneously. 00:40 He has a left gaze preference, but is unable to look past the midline. 00:43 He moves his left body with full strength but has severe right hemiparesis and is only able to withdraw to pain. 00:51 So again, with this case, there are a number of key features. 00:53 First is the patient suffered a trauma. 00:56 And this is the inciting nidus of this presentation. 00:59 His core since then has been progressive, steady development of more and more deficit over time, which is consistent with a specific type of hemorrhage that is likely contributing to this patient's problem. 01:11 And then in terms of localization, this patient has a focal neurologic deficit, right hemiparesis what sounds like an aphasia, all from a left hemisphere left cortical problem. 01:23 Patient underwent imaging with noncontrast head CT, which is the initial evaluation of these patients. 01:29 And we see a number of things here. 01:31 First, there's hyper dense blood on the surface of the left convexity extending beyond suture lines in a crescent-shaped appearance. 01:41 We see that both on the axial here on the right and on the coronal on the left. 01:45 And as a result of this increase in total brain contents, there's mass effect on the left side of the brain and some early midline shifts that we see all of which are contributing to this patient's presentation. 01:58 So what's the most likely diagnosis? Is this an epidural hematoma, subdural hematoma, subarachnoid hemorrhage or glioblastoma? Well, this is not a glioblastoma. 02:09 This patient has an intracranial hemorrhage we don't see any underlying lesion. 02:13 This is not the imaging appearance of a subarachnoid hemorrhage, which is on the surface of the brain extending along the course of the surface of the brain or the blood vessels in the subarachnoid space, which is not where this blood is. 02:28 This is not the imaging appearance of an epidural hematoma, which is a lens-shaped lesion on the surface of the brain. 02:34 This is a classic imaging and clinical presentation for a subdural hematoma. 02:42 What is a traumatic brain injury? Simply put it as an injury to the brain. 02:48 When we think about the epidemiology of traumatic brain injuries, it's one of the leading causes of disability. 02:55 There is a male greater than female predominance, a 2 to 1 male predominance. 03:00 And we see a bimodal distribution of traumatic brain injuries in young individuals also often from trauma, motor vehicle accidents or sports-related injuries and an older individuals frequently from falls. 03:13 So we want to think about this in these patient populations.
About the Lecture
The lecture Traumatic Brain Injury: Introduction by Roy Strowd, MD is from the course Head Trauma.
Included Quiz Questions
What might be a sign that a patient has suffered a traumatic brain injury?
- Focal neurologic deficits
- Abrasions on other parts of the body
- Chest pain
- Abdominal pain
- Fever
What is a leading cause of traumatic brain injury in people under the age of 24?
- Motor vehicle accidents
- Falls
- Self-inflicted harm
- Gunshot wounds
- Stabbing
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |