Playlist
Show Playlist
Hide Playlist
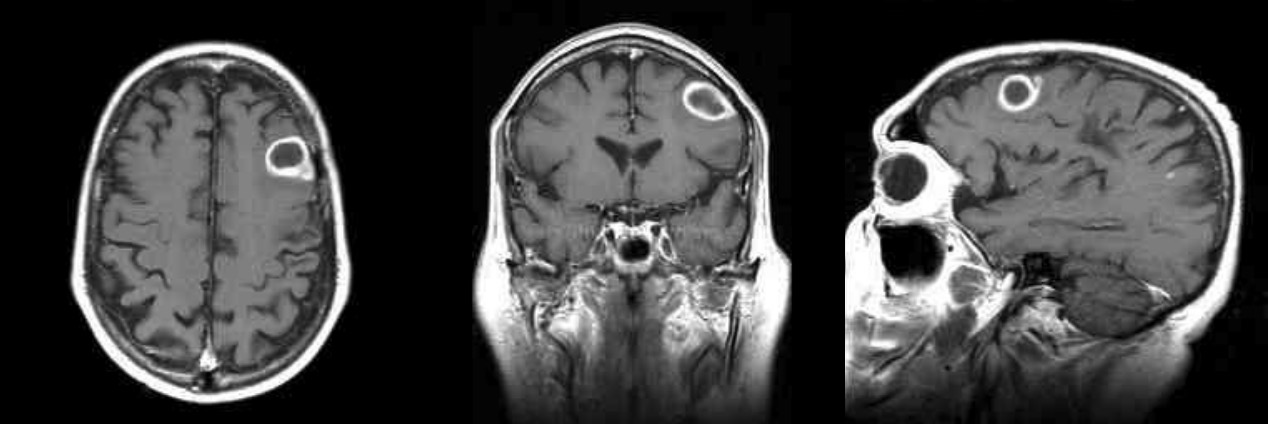
Brain Abscess: Signs & Symptoms
-
Slides BrainAbscess InfectiousDiseases.pdf
-
Reference List Infectious Diseases.pdf
-
Download Lecture Overview
00:01 So, let's talk about the clinical features of brain abscess. 00:06 It can be an indolent sneaky infection or fulminant symptoms and signs depending upon the size and location of the abscess and what it's pushing on or what it’s destroying. 00:19 Another determining factor is the virulence of the infecting organism. 00:25 Most of the patients will present with headache. 00:28 It can be on one side of the brain and it usually is on the same side of where the brain abscess is. 00:37 And so, it can be a generalized headache or hemi-cranial. 00:42 There are really no distinguishing factors, and so that often results in a delay in diagnosis. 00:52 But if a patient has sort of an indolent course and then becomes suddenly very ill, that suggests that the brain abscess has ruptured into the ventricles and is causing now meningitis. 01:11 So, various pathogens produce brain abscess. 01:18 We started earlier talking about Nocardia. 01:22 And I should point out at this point that about 10% of the patients who develop a Nocardio lung abscess also have a brain abscess. 01:35 This is a very abscessogenic organism. 01:38 So, if you diagnose lung abscess due to Nocardia, the incidence of brain abscess is so high that those patients should have imaging of their brain, symptomatic or not. 01:54 The zygomycetes, they are angioinvasive. 01:59 These are the bread molds. 02:01 And angioinvasive means that they invade blood vessels and they then can occlude those blood vessels and disseminate. 02:12 And most of the time, it's in and around the paranasal sinuses. 02:18 And most of the time it’s associated with diabetic ketoacidosis. 02:22 The absolute worst case of this I've ever seen is a man that was treated at an outside hospital for some kind of infection on the skin, a cellulitis. 02:34 He was given antibacterial antibiotics. 02:38 And during the course of that hospitalization, his glucose was out of control and he developed diabetic ketoacidosis in the other hospital. 02:48 He then began to complain of nasal congestion and trouble with his vision. 02:56 And they then transported him to the Medical College of Georgia, where I work, and at the time he arrived he was absolutely sightless in both eyes. 03:10 He had no light perception in either eye. 03:14 His face was swollen and you could almost demarcate where the infection was. 03:21 He had essentially caused an infarction of his face. 03:26 This organism had invaded all of the blood vessels in and around his sinuses and face. 03:32 And it had spread already to his brain, and so emergency surgery was done because you have to cut this infection out. 03:42 Remember, if the blood vessels are occluded, then how are antifungals even going to get there. 03:48 So, you’ve got to cut this entire infection out. 03:52 And the neurosurgeons and ENT physicians, when they cut, they kept finding fuzzy mold beneath the skin and deep into the sinuses. 04:04 And the patient literally had his face taken off by the surgeons. 04:13 And he was about to be fitted with a mannequin like mast to place over his face, but unfortunately he died of a bacterial meningitis because of the proximity of all this surgery to his brain. 04:28 But I'll never forget that patient. 04:30 And the main reason I want you never to forget it, anything – in a diabetic with ketoacidosis, anything suspicious about the sinuses, those patients need an emergency workup by ENT for invasive mucormycosis. 04:51 And then, we’ve already talked about the association of near-drowning with Scedosporium. 04:59 Toxoplasma encephalitis in brain abscess will present usually with confusion. 05:05 We’re usually talking about an HIV patient and the patient may have extrapyramidal findings because the basal ganglia are frequently involved in abscesses due to Toxo. 05:19 In a patient with aspergillosis, this, like mucor and like the bread molds, is angioinvasive. 05:28 And the main patients at risk for this infection are patients with neutropenia. 05:35 Indeed, the most common fungal infection in a patient with leukemia and neutropenia is aspergillosis. 05:43 And a patient may actually present as if they've had a stroke, and so stroke in a leukemic victim should be considered to possibly be Aspergillus until proven otherwise.
About the Lecture
The lecture Brain Abscess: Signs & Symptoms by John Fisher, MD is from the course CNS Infection—Infectious Diseases. It contains the following chapters:
- Signs/Symptoms – Clinical Features
- Various Pathogens
Included Quiz Questions
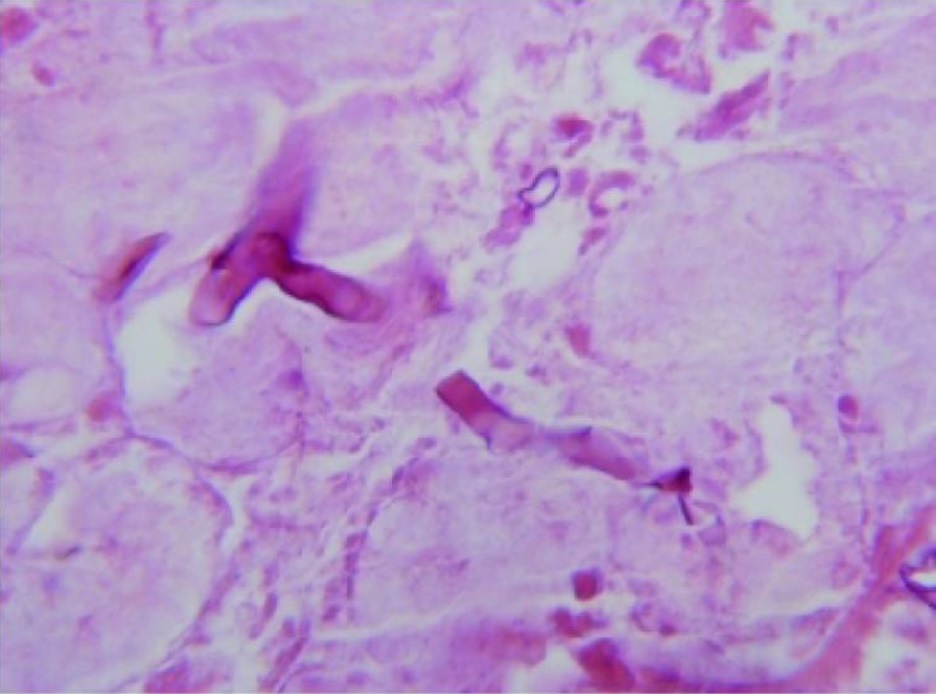
Samples from a brain abscess in a patient with neutropenia reveal hyphae with dichotomous branching that is progressive and primarily at acute angles of around 45°. Which of the following organisms is the most likely cause?
- Aspergillus spp.
- Toxoplasma gondii
- Mucormycetes
- Nocardia spp.
- Scedosporium apiospermum
Which of the following pathogens is a common cause of brain abscess in immunocompromised hosts with a lung infection?
- Nocardia
- Klebsiella pneumoniae
- Streptococcus milleri
- Schistosoma japonicum
- Entamoeba histolytica
which of the following is the most common symptom of brain abscess?
- Headache
- Fever
- Neck stiffness
- Mental status changes
- Seizure
Which organism is notorious for causing severe infections of the paranasal sinuses in poorly controlled diabetic patients which requires surgical intervention?
- Zygomycetes
- Streptococcus pneumoniae
- Staphylococcus aureus
- Mycoplasma pneumoniae
- Nocardia
Which of the following locations in the brain is most commonly affecte by toxoplasma-induced brain abscess?
- Basal ganglia
- Cerebellum
- Inferior temporal lobe
- Medulla
- Frontal lobe
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |