Playlist
Show Playlist
Hide Playlist
Blepharitis – Diseases of the Eyelids
-
Slides External Eye Diseases Diseases of the eyelids.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
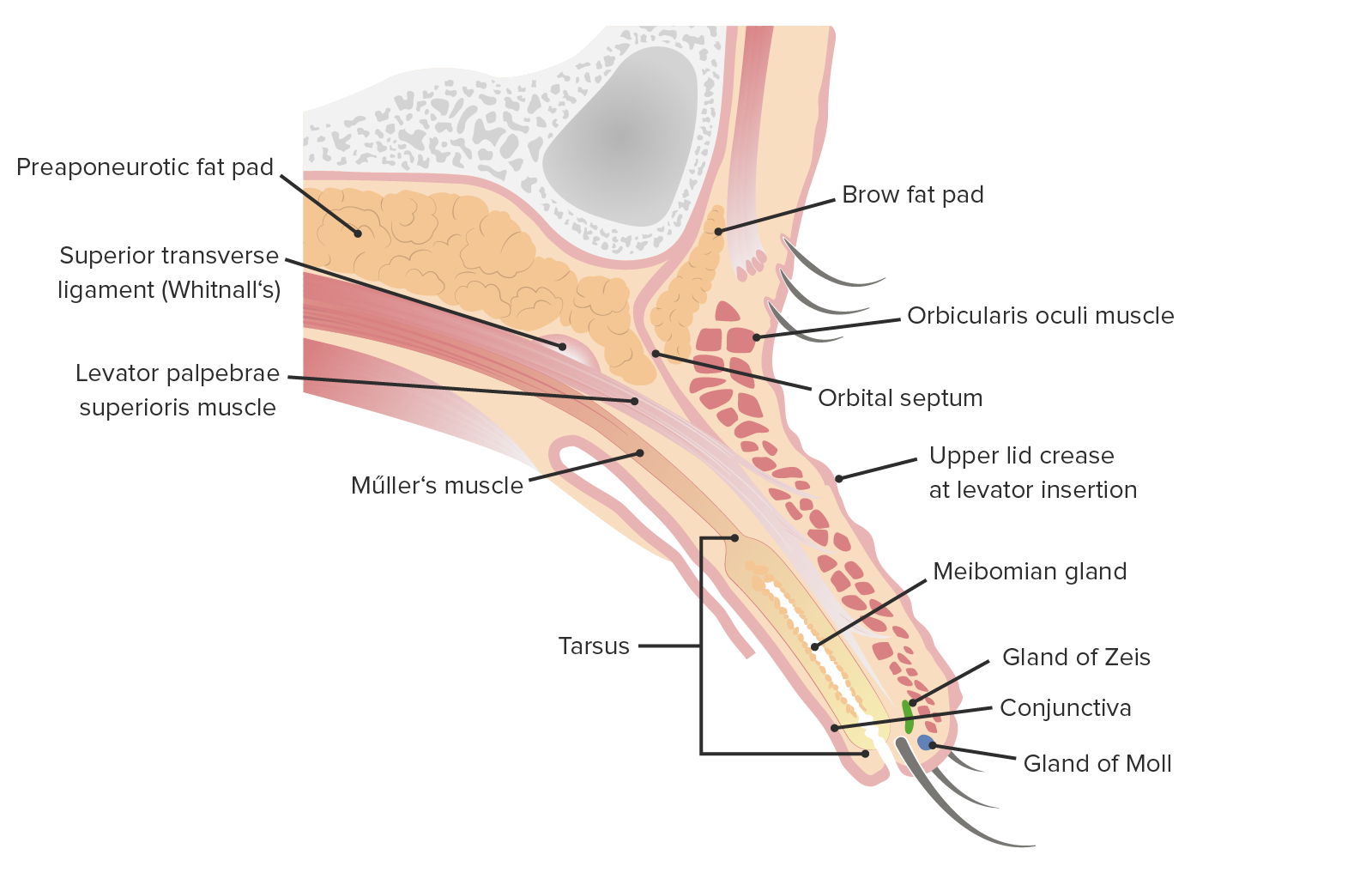
00:02 Ok, now that we've been all oriented to the structures of the eyes and we kind of have a good sense of where things are, what they're made up of, let's start getting into some of the ophthalmologic pathology. 00:15 And we're going to start with the outside and work our way all the way in, diseases of the eyelids as first. 00:23 Let's start with the upper lid and lower lid, the upper and lower palpebrae, so the lids. 00:29 And we're going to talk about diseases that are blepharitis, chalazion, and hordeolum okay, or stye. 00:39 Inflammation of the lid margins is blepharitis. 00:42 And it can involve a number of structures, so basically it's inflammation. 00:47 kind of at the edges of the eye, including some of the glands and some of the muscles and skin that are there. 00:55 Blepharitis. 00:56 So inflammation of the blephs, if you will. 01:00 So signs and symptoms of blepharitis, you're looking at it right here. 01:02 This does not look like a happy guy at all. 01:06 And that lid is swollen. 01:09 I'm sure it's very tender. 01:11 You don't want to rub it at all, and it's red. 01:13 So you're looking at the hallmarks of inflammation: erythema, edema, and there's also pain here. 01:23 There will be an itchy gritting or burning sensation so the eye is not innervated, but the lid is. 01:31 And it will as a result of all the inflammation that's going on there, It will feel tender or burning, he'll have a variety of sensations. 01:39 It will be very, very uncomfortable. 01:42 The eyes are excess, there's excess watering, and this is because of the activity. 01:46 The inflammation is driving various glands to secrete more fluids. 01:50 Some of this, especially if it's extending out into the lacrimal glands, we will have inflammation that may secondarily involve that. 01:56 So we will get increased watery eyes from the increased drainage. 02:02 The inflammation causes vasodilation, increased vascular permeability of the conjunctiva and in the lid margins. 02:09 And that conjunctiva, becomes red and injected, so instead of having nice white sclera, we are beginning to see the vessels that are normally relatively inapparent in the conjunctiva. 02:20 And with the materials that are being released by the glands and then when they condense, aggregate, crosslink, etcetera, we will get skin crusting and scaling. 02:32 So there are going to be inflammatory cells that have crawled out. 02:35 They will form kind of a crust or a scale on the eyelid margin eyelashes. 02:40 And again, that will be contribute to some of that gritty sensation that's there. 02:45 So a number of things and a little bit of inflammation goes a long way when it involves the eye. 02:53 Because of all this excess fluid, the vision will tend to be blurred and because of inflammation, light shining into the eye, when you want to actually have undergo miosis and mydriasis, you'd want to kind of expand the eye or contract the eye, actually hurts because we're pulling on smooth muscle and there are nerves that are there. 03:18 Okay, so the anatomical structures that are involved in blepharitis. 03:21 We've looked at these previously and we're going to talk specifically about some of them. 03:26 But basically it's the muscles, the levator palpebrae superioris that keeps the lid up. 03:34 The orbicularis oculi muscle, that's the one that allows you to close your eyes, your eyelids. 03:40 And then there's going to be the underlying structures. 03:42 The tarsus, remember, this is the connective tissue that gives integrity, kind of a framework, scaffolding upon which we're going to have the levator in the orbicularis sit. 03:53 The tarsus also has within it glands that are going to be part of the lubrication of the eye. 04:00 Meibomian glands and then glands that are associated with the eyelashes. 04:05 We've talked about these previously, but the gland of Moll and the gland of Zeiss, great names. 04:09 I don't know who Moll and Zeiss were, but they got their name, these particular glands, and they're basically just sebaceous glands or modified sebaceous glands that sit attached to the hair follicles that form the eyelashes. 04:26 Anterior blepharitis is that mainly centered around the skin and the skin structures, the eyelashes, a little bit of hair follicles that sit over the front of the lid or at the end of the lid. 04:38 And then you can have a posterior blepharitis. 04:40 Obviously, if there's anterior, there's got to be the posterior. 04:43 Posterior blepharitis, it's going to involve the structures of the tarsus, in particular the Meibomian glands. 04:50 Okay, so these are the structures that are there and they are inflamed, hence blepharitis. 04:58 Let's look at these things in a little bit more details. 05:01 So what causes blepharitis, many, many different causes. 05:05 And some of these may be systemic, as we'll see. 05:07 Some of these may be very focal and just hit the eye because of things we do to your eye. 05:12 Okay, so seborrheic dermatitis is a chronic inflammation of sebaceous glands It can be very focal, but seborrheic dermatitis can happen everywhere and if you've if you've had flaky, itchy, oily scalp that's seborrheic dermatitis. 05:26 Anywhere that there's hair, that can happen because there are sebaceous glands associated with that hair. 05:33 You're going to have chronic inflammation due to increased immune response. 05:36 It's basically an exaggerated inflammation out of control, that's rosacea. 05:41 Again, it can be systemic. 05:43 It can be focal, can be in any particular area, but if it involves the eyelid, you'll get blepharitis. 05:49 You can have atopic, otherwise known as contact dermatitis. 05:53 And that is things that you might rub on your eye, makeup and other things like that, even just what is in the detergent that you clean your eyes with or on a towel or whatever. 06:06 You can get a delayed-type hypersensitivity to that. 06:09 And that inflammation of the lid will cause blepharitis You can have psoriasis, which is an autoimmune disorder. 06:19 Many of the immunologic mechanisms are going to be akin to delayed-type hypersensitivity but this one is driven by specific adaptive immune elements that are recognizing elements of the skin. 06:32 And again, it tends to be systemic, tends to be everywhere on the skin, but can particularly affect the eyes, eyelids. 06:40 Bacterial infections are probably going to be a major driver for blepharitis There's a lot of bacteria on our skin, the eyelids are no exception. 06:49 And Staphylococcus is going to be the most common bacterial infection, Staph aureus in particular. 06:54 Then you can have a variety of viral infections - molluscum, varicella zoster, herpes simplex, etc. 07:00 You can have parasitic infections. 07:02 So this sounds incredibly distasteful, but you can have little parasites that live within the hair follicles that eat dead skin - Demodex. 07:11 And they can elicit inflammatory responses and give you a blepharitis. 07:19 So cosmetics and pollen. 07:21 So other irritants and allergens specifically can do that just because there is a particular element that may be inflammatory and then some medications and retinoids in particular. 07:33 If we give Accutane, for example, for people who have chronic acne, what that elevated retinoid level does is change the nature of the epithelium in the glands from something that's more cuboidal or columnar into something that's more squamous. 07:49 And so we don't get the normal production or movement of the various components. 07:55 And the retinoids may actually cause a significant amount of inflammation. 08:02 Okay, those are causes. 08:04 How do we diagnose it? Well, you saw it. 08:07 You diagnosed it on that very first slide. 08:08 That kind of swollen eyelid looks painful. 08:11 There's you know, there's blurring. 08:13 Its clinical symptoms, okay. 08:15 And the treatment? It's mainly keeping the eyelid clean, getting rid of the bacteria, not rubbing things that are particularly inflammatory on top of that. 08:25 If there is infection, then we may need to provide antibiotics. 08:30 It can be topical, it can be systemic. 08:32 And then warm compresses help because when we put on a warm compress, we're causing increased vascular flow. 08:40 We're actually causing vasodilation, which will help to clear some irritants, but will also help to bring in inflammatory elements if we need to treat an infection. 08:50 So warm compresses are frequently very good, just kind of over the counter sorts of things that you can do to treat this. 08:59 Okay, so that's blepharitis and it's mostly the upper lid, it's mostly the kind of inflammation of those structures.
About the Lecture
The lecture Blepharitis – Diseases of the Eyelids by Richard Mitchell, MD, PhD is from the course External Eye Diseases.
Included Quiz Questions
What structure is involved in blepharitis?
- Eyelid margin
- Sebaceous glands
- Tarsus
- Levator palpebrae superioris
- Cilia
What is the clinical presentation of a patient with blepharitis?
- Itchy, gritty, or burning sensation
- Purulent discharge from the eye
- Yellow discoloration of the sclera
- Upward and outward rotation of the eyeball
- Temporary paralysis of the eye
What structure is affected by posterior blepharitis?
- Meibomian gland
- Gland of Moll
- Gland of Zeiss
- Lacrimal gland
- Orbicularis oculi
What organism most commonly causes blepharitis?
- Staphylococcus
- Mycobacterium
- Streptococcus
- Varicella
- Candida
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |