Playlist
Show Playlist
Hide Playlist
Generalized Rashes: Atopic Dermatitis and Viral Exanthems
-
Slides GeneralizedRash AcuteCare.pdf
-
Download Lecture Overview
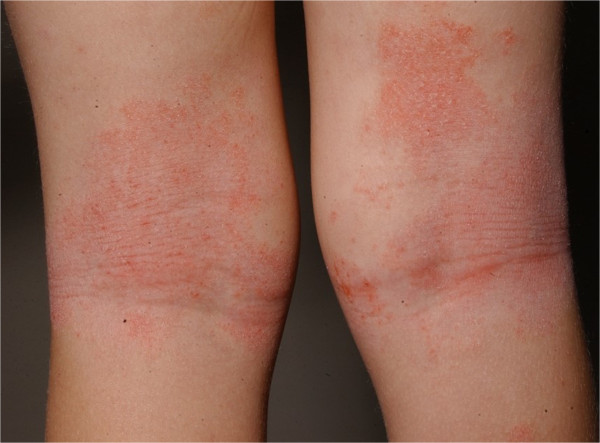
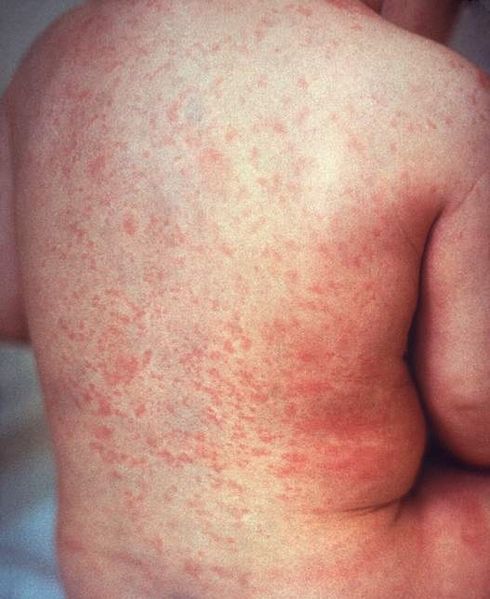
00:01 All right. 00:02 So, now, we’re going to discuss generalized rashes. 00:04 And this is a really important subject, particularly for USMLE and test taking. 00:09 I recertified in my family medicine board exam last year and I remember one of the last things I reviewed before going into the exam was generalized rashes because I knew I was going to see a picture and I knew you have a question associated with it. 00:22 So, I’m going to try to make this very pertinent for you in your exam too, but it's also pertinent for your clinical practice. 00:27 These are all things I see on a routine basis. 00:31 So, we’re going to start with one of the more common ones, atopic dermatitis. 00:35 And so, really when you’re thinking about atopic dermatitis, think about looking for scale and lichenification or dryness with pruritus. 00:44 And it’s more common among children. 00:46 You can see it among adults as well. 00:48 It's associated with a family history of atopy except not every kid has that family history. 00:54 Do remember, though, that these children with atopic dermatitis, about a third of them eventually develop asthma and many of them also develop allergic rhinitis. 01:03 So, that history of atopy, therefore, affects multiple systems at once. 01:09 The distribution you’re going to look for with atopic dermatitis, it's going to be more on your flexor services, on the neck, on the forehead, and definitely the classic is behind the years, particularly among younger children and infants. 01:23 So, start, in terms of management, with some real basics. 01:27 You don’t want to use a lot of heat. 01:29 Heat makes those worse. 01:30 And try to avoid soap, if you can, for these children, in particular. 01:36 And if not, just use a very gentle soap, a moisturizing soap. 01:40 The emollients are the key again. 01:42 And I just keep coming back to that. 01:44 Usually, it’s dryness of the skin which really makes the rash a lot worse, but it can be prevented. 01:51 So, you have to be very consistent with using emollients. 01:55 And I have a son with atopic dermatitis and I know what a challenge that can be, but we've taken it – we’ve taken the challenge and it certainly does a lot better when he’s on the emollients versus not. 02:06 For flares, topical corticosteroids are effective, but they do have side effects in terms of hypopigmentation of the skin, thinning of the skin structures. 02:18 And so, therefore, you really want to use the minimum dose for the shortest amount of time possible when it comes to topical corticosteroids and use them for the inevitable flares that occur. 02:29 Topical calcineurin inhibitors are really considered more of a second line agent for active disease behind corticosteroids. 02:37 They may not be as effective. 02:39 There was concern that these agents promoted higher risk of skin cancer. 02:44 That doesn't seem to be the case. 02:46 And so, they appear to be fairly safe over time, but just don't have the efficacy of topical corticosteroids and, therefore, considered second-line agents. 02:56 All right. 02:56 Let's now move on to viral exanthems. 02:58 And I try to hit the big ones for you with our discussion today. 03:02 We’re going to start with fifth disease. 03:04 So, fifth disease is caused by parvovirus B19. 03:08 Usually a benign course that can be kind of scary, but a lot of – some fever and cough, but also produces these classic rashes. 03:18 And so, if you need to, like a great USMLE question, is you see the picture of the child with a slap cheeks there and what's the causative agent, it's fifth disease and, therefore, it’s parvovirus B19. 03:30 That’s what you want to look for. 03:31 So, the slap cheek appearance appears early in the course of illness and then oftentimes there is also a more generalized rash over the body that has either a fishnet or a lacy appearance. 03:44 That's the other thing you really want to look for with fifth disease. 03:48 But again, usually a benign course with supportive care only. 03:53 Another scary rash and scary illness for parents, but something that kids actually do really well with is roseola. 04:03 So, the classic pattern for roseola is there's a high fever, but it’s fairly short, usually only lasting a couple of days. 04:11 And when the fever breaks, that's when this rash breaks out. 04:14 This is a generalized maculopapular rash. 04:17 It starts centrally, spreads outward more peripherally. 04:21 And importantly, essentially when the rash comes on, the fever starts to go away. 04:26 And it also occurs in young children. 04:29 So, you don't expect to see this in an eight-year-old, but certainly in a nine-month old or in a two-year-old roseolas are very common illness. 04:37 And has a benign course again, resolves usually over a week with the rash itself.
About the Lecture
The lecture Generalized Rashes: Atopic Dermatitis and Viral Exanthems by Charles Vega, MD is from the course Acute Care. It contains the following chapters:
- Generalized Rashes
- Viral Exanthems
Included Quiz Questions
Which of the following conditions is strongly associated with atopic dermatitis?
- Asthma
- Inflammatory bowel disease
- Psoriasis
- Irritable bowel syndrome
- Angioedema
An 11-month-old boy presents with a blanching maculopapular rash that started on the neck and trunk 2 days ago and spread to the face and extremities. He had high fever for 3 days prior to development of the rash. Which of the following is the most likely diagnosis?
- Roseola
- Measles
- Fifth disease
- Rubella
- Mumps
Which of the following best describes the rash that follows the slapped cheek rash in fifth disease?
- Lacelike
- Pustular
- Vesicular
- Bullous
- Nodular
Which of the following is not included in the list of recommendations for maintenance of atopic dermatitis?
- Topical antifungals
- High-potency topical steroids
- Low-potency topical steroids
- Topical emollients
- Topical calcineurin inhibitors
In children with atopic dermatitis, which of the following is NOT a typical location of rash?
- Scalp
- Antecubital fossa
- Volar aspect of the wrists
- Popliteal fossa
- Neck
Which of the following complications is most likely with long-term use of topical steroids for atopic dermatitis?
- Skin atrophy
- Resistance to steroid therapy
- Lichenification
- Skin cancer
- Allergic dermatitis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |