Playlist
Show Playlist
Hide Playlist
Assisted Control – Modes of Ventilation
-
Slides ModesOfVentilation RespiratoryPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
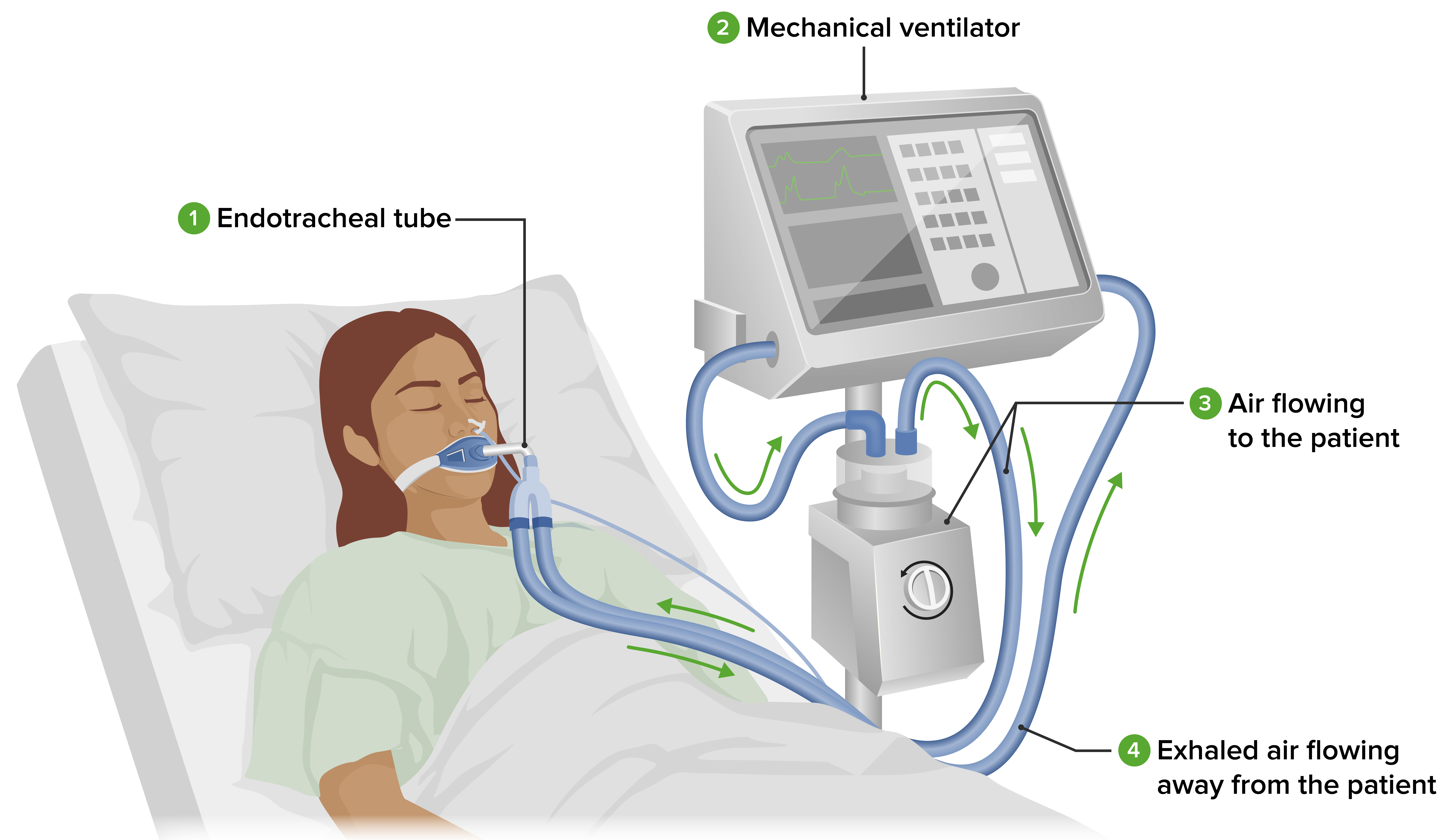
00:02 Let's continue taking a look at respiratory failure and now however, you know how the ECG or EKG was for the cardiovascular system. Well, it’s just as important that you take at look at the graphical presentation of what is known as your ventilation or modes of in respiratory failure. 00:23 We will begin by looking at the foundation of setting up what you want to be very familiar with when you are interpreting graphs of modes of ventilation. What does that even mean? Well, there are two modes, in general, that you would be able to help your patient with respiratory failure. You are extremely familiar with one of them which is the management of a patient that has obstructive sleep apnea. Think about that patient who is obese and maybe has a hard time breathing out and so therefore might be, wow, apart from hypoxemia might also be then retaining carbon dioxide. So with this patient, you might want to think about providing this patient with what is known as a mode of non-invasive ventilation and this is referred to as being CPAP and that you already are familiar with. What CPAP stands for is continued positive airway pressure. 01:19 Now on that note, what we will take a look at is, well, non-invasive versus invasive. 01:25 What, really, what is the difference and how does that then benefit you? Say at some point, you do need to intubate your patient, right, endotracheal. You need to intubate your patient, then here, the graphical representation which will be your ventilation graph through invasive will be quite important for you to interpret. So, just like we looked at pulmonary function test as being non-invasive, let's begin by dissecting our graphs. The graph that you see in the bottom is pressure. And how would you measure pressure in the respiratory system? That will be centimetres of water and then this corresponds to what happens actually in the lung. And so therefore you are looking at volume in the above graph. 02:07 Next, well you bring in your physiology. What does that mean? Well, I want you to pay attention to the bottom graph and take a look at the black solid line. You see the black solid line on the bottom graph of your pressure and you should remember from physio that if you were to breathe in or inhale, then you have your pressure which is then going to become more negative. Do you remember that? You should. So all that physiology or lung mechanics is going to come into play here when dealing with clinics. So we have a negative pressure which is the trigger for you to then, guess what? Go back up to the top graph, you will notice a spike. That spike in which now, the volume, litres per minute, is increasing from 0 towards positive. Now, understand the concept first. At this point, it is not imperative that you memorize the values, understand the concept. Negative pleural pressure, therefore brings about inspiration. Okay, great. Let's say that your patient is having a hard time with breathing. He is not able to properly keep open the alveoli and probably has impairment of gas exchange. So what does that mean to you? Well, if this is impairment in gas exchange and you feel the need to then give your patient some type of ventilatory assisted control and what might you want to do? Well, take a look at the bottom graph. This time, I want you to pay attention to red dashed lines. The red dashed line, represents the fact that the patient wishes to inspire, inhale. During that process of inspiration this will be a trigger in which now, guess what kind of pressure? Do you remember that conversation that you and I had with PEEP, positive end expiratory pressure? It’s positive pressure, isn’t it? And so, what you are doing and how you are introducing air into the alveoli is, remember. You are now the lung. You, the clinician. So therefore you are going to inject “positive pressure” into the respiratory system so you can keep your alveoli open and at this point, if you follow the red dashed line in the bottom graph, you will notice that there is a plateau. It’s nice and uniform and so therefore, just like in EKG, you would have your sinus rhythm and QRS complex. You are going to have this pattern of breathing taking place ever so often, intermittently. This is the foundation in which you want to keep in mind when dealing with expansion and pressure of your lung with, What kind of pressure that you are going to provide? Very good. Positive pressure. Now, a host of side effects or should we say, adverse effects that might have occur when applying such positive pressure. 04:59 All these are discussions to be had as you move forward. Important? Absolutely. This is the evolution of a board exam.
About the Lecture
The lecture Assisted Control – Modes of Ventilation by Carlo Raj, MD is from the course Respiratory Failures.
Included Quiz Questions
Which of the following units is commonly used to express the pressure in a ventilation curve diagram?
- Centimetres of water
- Millimetres of mercury
- Kilo pascals
- Newton
- Millimeters
Customer reviews
1,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
1 |
1 customer review without text
1 user review without text