Playlist
Show Playlist
Hide Playlist
Approach to Arthritis: Review
-
Slides Approach to Arthritis.pdf
-
Reference List Rheumatology.pdf
-
Download Lecture Overview
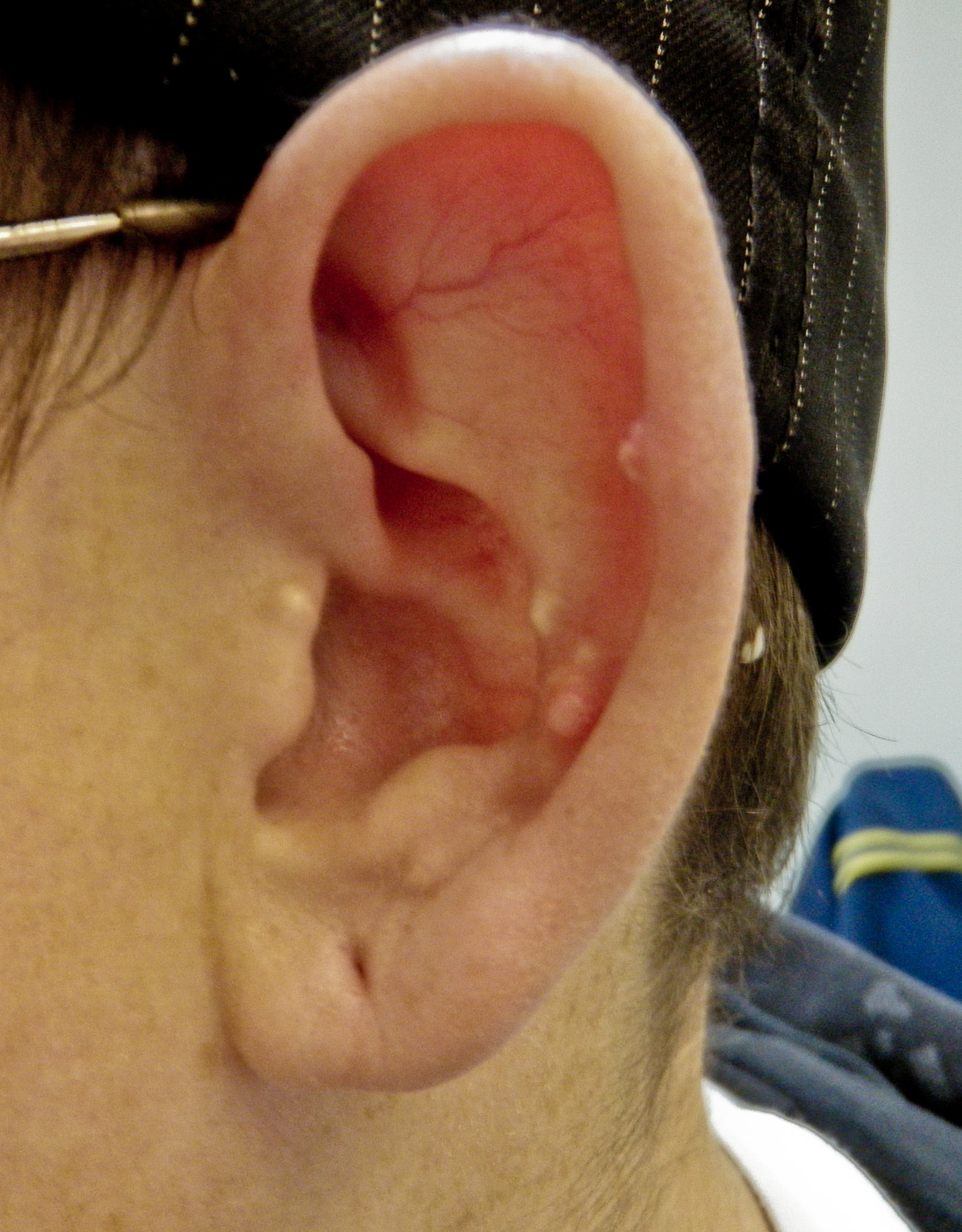
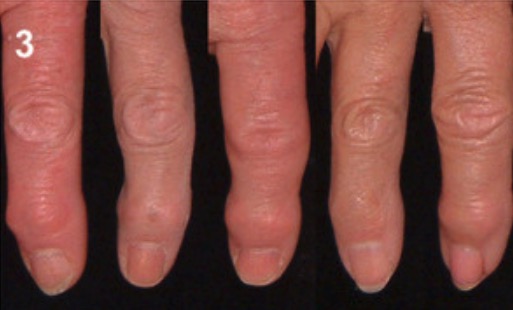
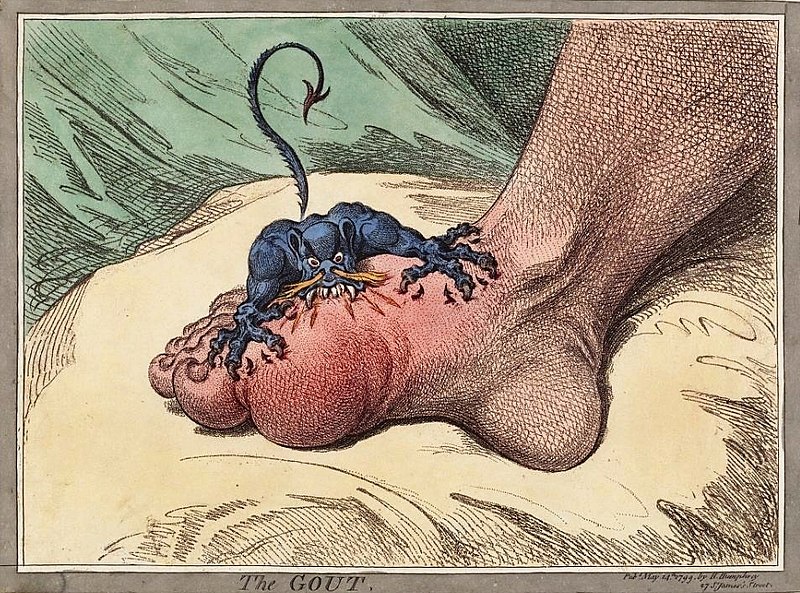
00:00 So to review this section, the variables that you always want to get when you're looking at patients with joint pain are what's the time course, what's the pattern of joint involvement, is there any evidence of inflammation when examining that joint, and is there evidence of other systems involved. Having done that, let's take a look at an overview of the types of conditions that you might see in our section on arthritis. We can think of the causes of arthritis broken up into 4 major categories, 3 of which are in 1 category. We'd call them autoimmune conditions. These include connective tissue diseases. Shown here is a picture of rheumatoid arthritis. The seronegative arthritides also called axial spondyloarthritides. Shown here is someone with inflammation in the Achilles tendon at enthesitis in this area of the back of the heel. And then our vasculitides and this is polyarteritis nodosa which can have a lot more things going on than just joint disease. 00:57 And then the non-autoimmune arthritides, we'll talk about as well. Shown here is just basal joint arthritis just common manifestation of osteoarthritis. So, rheumatoid arthritis, classic example of a connective tissue disease. We also have lupus, systemic lupus erythematosus or the drug-induced lupus pictures. Shown here is the classic malar rash of lupus. And then Sjogrens. These are just representative examples of some of the connective tissue diseases that can manifest with joint disease. Systemic sclerosis, this is another example and shown here is just Raynaud's phenomenon. 01:33 Part of the CREST acronym when we think about systemic sclerosis. And then inflammatory myositis, which is another topic that we'll cover on another day which also falls into this category of autoimmune diseases. The next broad category is the spondyloarthritides. These include IBD or inflammatory bowel disease related arthritis, ankylosing spondylitis, reactive arthritis, and psoriatic arthritis. And the next large category, which is a very complicated category, is the vasculitides of which there are a number of vasculitis patterns. We typically break them up into 3 large categories; small, medium, and large. And within the small category, we have immune complex mediated and shown here is a picture of what used to be called Henoch-Schönlein purpura now called IGA vasculitis with some palpable purpura and ANCA-associated vasculitis and this is a picture of granulomatosis polyangiitis also previously known as Wegener's, a renal biopsy from that disease. Secondly are the medium vessel vasculitis, which this is a picture of polyarteritis nodosa. And then thirdly are large vessel vasculitis and this is a picture of a temporal artery biopsy from giant cell arteritis or temporal arteritis. Now let's talk about the non-autoimmune causes of arthritis. 3 categories here as well. The first of which is the crystalline arthropathies. 03:00 The most notable is gout, uric acid crystals depositing in joints. Pseudogout also known as CPPD. Septic joint, again typically monoarticular and most common organism involved is <i>Staph aureus</i>. 03:17 And then, just degenerative joint disease most commonly osteoarthritis. It's important for us to remember those 4 large categories of arthritis. Again, the autoimmune group and then the non-autoimmune arthritis. But keep in mind there's also a number of miscellaneous causes of joint-related disease. These are basically a group of conditions where the patient may not actually have a joint problem but they're presenting with pain in their joints. An example of this would be something like sarcoidosis which has involvement in a number of different sites and a person may certainly present with arthralgias. Fibromyalgia, which is a condition we'll talk about at some length but involves pain in the joints and to the muscles but there's actually no objective evidence of joint or muscle disease. And then thirdly, myofascial pain syndrome which is related to fibromyalgia. It's just important for us to keep these types of diseases in mind as they are essentially soft tissue causes of joint pain even if the joint itself is not strictly involved. 04:26 Again, to review, we started with the 4 features that we're going to be looking for when looking through a new case; the time course, pattern of joint involvement, evidence of inflammation, and systemic involvement.
About the Lecture
The lecture Approach to Arthritis: Review by Stephen Holt, MD, MS is from the course General Approach to Arthritis and Joint Pain.
Included Quiz Questions
Which of the following microorganisms is most associated with septic arthritis?
- Staphylococcus aureus
- Pseudomonas aurgenosa
- Escherichia coli
- Salmonella typhi
- Streptococcus pneumonia
Spondyloarthritides include all of the following conditions EXCEPT...?
- ...gout.
- ...psoriatic arthritis.
- ...ankylosing spondylitis.
- ...reactive arthritis.
- ...inflammatory bowel disease-related arthritis.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |