Playlist
Show Playlist
Hide Playlist
Anemia in Children: Pathology and Diagnosis
-
DLM 09-65 Anemia Alverson v011.pdf
-
Download Lecture Overview
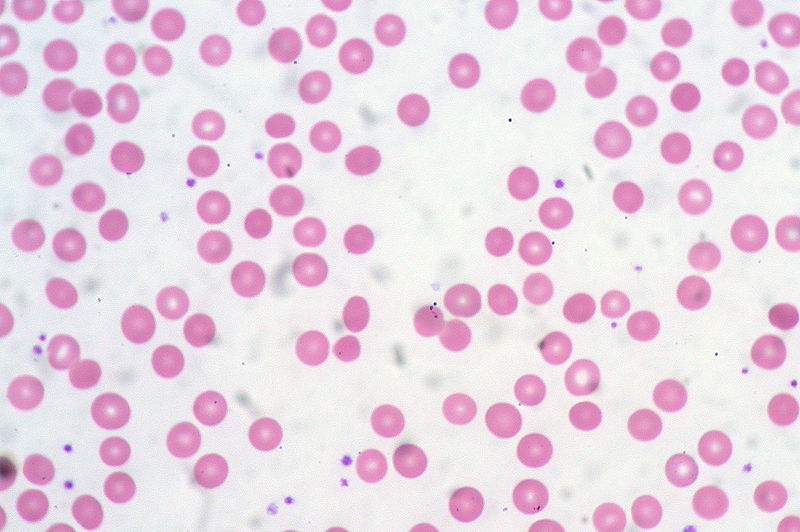
00:01 Another valuable thing, test that we do when patients with anemia is we can actually look at the blood under the microscope, and the blood under the microscope, it's hard to say whether the blood cells are small or big or have a normal distribution, that's what the machine is for but the blood cells can give us clues to what's going on. 00:20 You see this picture here. This is a patient who's having an acute hemolytic anemia, that's an intravascular problem. 00:27 They got helmet cells, and cells are being clearly ripped apart. 00:31 Here is an example of a patient with a multilobular white blood cell. 00:37 That's gonna tell me a little bit of this patient may have B12 deficiency. 00:41 Here is another example of where the picture might help us. 00:45 Look at this slide carefully, and you can see especially on the top right next to that one little purple dots, this is called basophilic stippling. 00:54 We sometimes see this in lead poisoning. 00:57 If I saw this under the microscope, I'd know, uh-oh better worry about lead poisoning. 01:01 Here's another example of a picture. This patient has very abnormal shape cells. 01:07 Here's the last one. This one should be pretty obvious to you. 01:13 If you look at it carefully, you can see that some of the cells are long and thin instead of round. 01:19 Yeah, this person has Sickle cell disease. 01:23 And you can see it, if you step back even, if you look at the -- farther away view, you can see lots of little sickled cells. 01:31 This even looking at this mirror might tell you how bad off they are right now, how much sickling is going on. 01:38 Okay, so we've got a CBC, we know that they're reticulocyte and we know their MCV. 01:46 And we have a sense of the RDW as well. 01:49 Let's break it down in terms of what might be going on. 01:52 Anemia's can be classified in three categories based on the mean corpuscular volume or MCV. 02:00 If the MCV is low, the anemia is called microcytic. 02:04 The most common causes of microcytic anemias are iron deficiency anemia, alpha and beta thalassemia, anemia of chronic disease and sideroblastic anemia. 02:16 If the MCV is high the anemia is termed macrocytic. 02:21 This is usually megaloblastic anemia due to folate or vitamin B12 deficiency. 02:27 If the anemia is normocytic, then we need to calculate the reticulocyte count in order to determine if the anemia is caused from under production of red blood cells or their peripheral destruction. 02:39 If the reticulocyte are low, this means that the ideology of the anemia is under production from the bone marrow. 02:47 The most common causes are shown in the slide and include aplastic anemia, leukemia and renal failure. 02:53 Other causes that may appear in the pediatric population are Diamond-Blackfan anemia which is a rare congenital anemia caused by increase apoptosis of red blood cells in the bone marrow and the transient erythroblastopenia of childhood which is cause by suppression of erythropoiesis often after a viral infection. 03:13 If the reticulocyte count is high, this means that the bone marrow response to the peripheral destruction of red blood cells, the most common causes includes sickle cell anemia, G6PD deficiency, hereditary spherocytosis, autoimmune hemolytic anemia and paroxysmal nocturnal hemoglobinuria. 03:34 You can see how these values are gonna start to tweak our understanding or guessing of what things are, and if you understand the disease you'll be able to put it together. 03:45 So knowing that lead poisoning causes microcytic anemia and is a long indolent thing and prevents the production of reticulocyte counts you can predict where it falls in this table.
About the Lecture
The lecture Anemia in Children: Pathology and Diagnosis by Brian Alverson, MD is from the course Pediatric Hematology. It contains the following chapters:
- Anemia – Pathology
- Anemia – Diagnosis
Included Quiz Questions
Which of the following is the most likely diagnosis in a child with microcytic anemia and basophilic stippling on peripheral blood smear?
- Lead poisoning
- Folate deficiency
- Hereditary eliptocytosis
- G6PD enzyme deficiency
- Sickle cell disease
Which finding is most likely on a peripheral blood film from a patient with microangiopathic hemolytic anemia?
- Helmet cells
- Hypersegmented neutrophils
- Red blood cells with basophilic stippling
- Howell-Jolly body
- Sickle shaped cells
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |