Playlist
Show Playlist
Hide Playlist
Androgen Insensitivity Syndrome: Complete and Partial AIS
-
Slides Androgen Insensitivity Syndrome.pdf
-
Download Lecture Overview
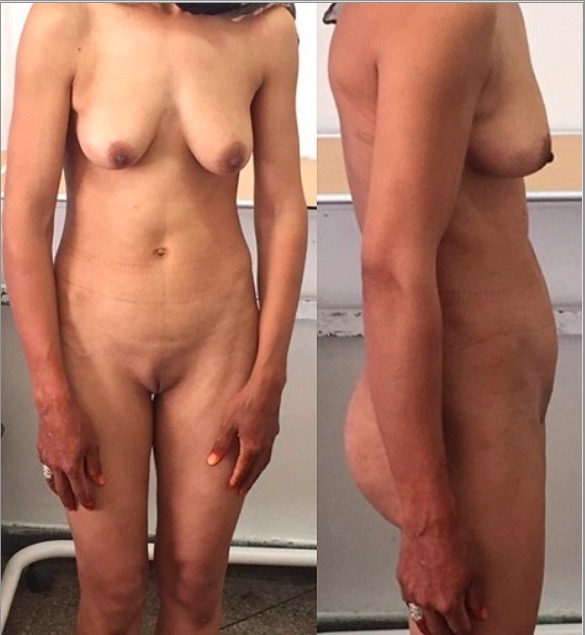
00:00 Hi. Let’s now review androgen insensitivity syndrome. Androgen insensitivity syndrome has two components. 00:09 It can be complete or partial. These patients have normal gonads. They make steroids. 00:14 However, mutations and receptors can mute the effect of steroids on specific tissues. 00:20 Before we review androgen insensitivity syndrome, let’s review the target organs of testosterone. 00:27 So in the skin, it actually influences hair growth. It can cause balding and sebum production. 00:34 In the liver, it can actually promote synthesis of serum proteins. Male sexual organs rely on activated or DHT which is dihydrotestosterone to actually cause penile growth, spermatogenesis after puberty, prostate growth and function. In the female which I don’t have displayed here, it does not affect female sexual organs. In fact, too much testosterone can cause ambiguous genitalia which is seen in another lecture. Bone marrow can also be affected by testosterone. 01:09 You can have stimulation of stem cells. In the brain, testosterone can influence libido in both males and females as well as mood. Muscles are actually increased in strength and volume. 01:23 Kidneys are actually stimulated to perform erythropoietin production. In the bone, testosterone increases accelerated linear growth and closure of the epiphysis. 01:36 Now, let’s go back to androgen insensitivity syndrome. It’s very rare. It occurs in about 1 in 20,000 patients who are live born meaning they’re born live, not a stillbirth. These are XY individuals. 01:51 So, they have normal genetic sex. They’re 46, XY. But 1 in 300 of these patients will have a mutation of the androgen receptor. The androgen receptor is on the X chromosome not the Y. 02:06 Therefore, these mutations follow an X-linked pattern of inheritance. 40% of patients with complete androgen insensitivity will have a de novo mutation which means to say their parents are not carriers. They just have a new mutation that sort of spontaneously occurs. 02:26 The majority of mutations result in single amino acid substitutions which cause a receptor not to function. 02:33 Now, let’s review complete versus partial AIS. Complete AIS sometimes abbreviated CAIS causes unambiguous XY females. So, their genetic sex is 46, XY. However, they look like normal females at birth and onward. Usually, they present to the clinic when they have primary amenorrhea and infertility. 03:00 There is another lecture about primary amenorrhea that you can review. 03:05 Androgen insensitivity syndrome again is partial versus complete. So, the complete referred to here is CAIS is generally associated with incomplete absence of androgen binding and androgen receptor activation. 03:20 So, they have the receptors but the receptors do not work. They make normal testosterone but again, the message is not going where it should go. Patients who have partial AIS or PAIS may present completely differently. They have a male phenotype but you typically will see gynecomastia. 03:40 You can see here in this figure that this man has normal male hair distribution but when you look at the breast tissue, it should not look that way and that is a prime example of gynecomastia. 03:53 This patient can also have hypospadias. So, you can see here that the glans penis has a urethral meatus but there is another additional hole and that is evidence of a hypospadias. 04:04 These patients can also have infertility. Therefore, they have difficulty actually fathering a pregnancy. 04:11 PAIS, partial androgen insensitivity syndrome is very heterogeneous and can present with the following. 04:19 Here, you can see in this picture, you see a micropenis. So, it’s a very, very small penis than a child should have at delivery. They can also have cryptorchidism. So, you’ll see here back to this picture, if you actually palpate the scrotum here, you should be able to feel a testis on either side. 04:39 But with cryptorchidism, the testes do not descend as they typically should into the scrotum. 04:46 They can also have periscrotal hypospadias and this part of a syndrome called Reifenstein syndrome where they have a bifid scrotum and perineoscrotal hypospadias. These patients again, when they present as infants and children, they have unilateral or bilateral hernias. 05:07 So, with partial androgen insensitivity syndrome, these patients can sometimes present as a phenotypic virilized female with fused labioscrotal folds. They may or may not have clitoromegaly. 05:21 You can see in this photograph that this child has fused labioscrotal folds and they do have clitoromegaly. 05:28 A karyotype would be very helpful in diagnosing this patient. PAIS patients also have normal pubic and axillary hair but they’ll have little to no face hair or chest hair. This is because the adrenals will still make androgens that allow for pubic hair which is pubarche or axillary hair. 05:50 But the male distribution of hair may sometimes be compromised in these patients. 05:55 Now, let’s review the laboratory findings with CAIS. Their serum testosterone concentrations are normal or moderately increased in male ranges. But remember, you may not suspect that because they may look phenotypically female. They have normal production of testosterone by the intact testis but remember, their receptors are not getting the message. So, they make androgen but the androgen is not received by the receptor. So the message is in effect being lost, not heard by the receptor. 06:28 This will help you during your exam if you can think of it like this. So, how do we diagnose these patients? Well, the most reliable method for diagnosis of androgen insensitivity is to sequence the androgen receptor using DNA obtained from blood or tissue that's then cross referenced to a database of mutations. 06:48 Remember that the karyotype will also be 46, XY. Complete androgen insensitivity syndrome patients have a very unique body habitus. They typically look female but they’re usually very tall for a female and their weight is usually greater than an average woman. Remember that their breast development occurs normally because the androgens that they are making normally from the testes are aromatized peripherally. So in the CAIS patient, the complete androgen insensitivity syndrome patient, their external genitalia are clearly female. The vagina is either blind or shortened and sometimes described as a dimple. It’s important though that you not say that a patient has a dimple or shortened vagina without attempting to do a complete vaginal exam with either a speculum or digital palpation. Remember that their axillary and pubic hair tend to be scant or absent as that is reliant on an intact androgen receptor.
About the Lecture
The lecture Androgen Insensitivity Syndrome: Complete and Partial AIS by Lynae Brayboy, MD is from the course Normal Puberty and Disorders of Sexual Development. It contains the following chapters:
- Androgen Insensitivity Syndrome (AIS)
- Partial AIS (PAIS) and Complete AIS (CAIS)
Included Quiz Questions
What is the pattern of inheritance in patients with androgen insensitivity syndrome?
- X linked
- Autosomal dominant
- Autosomal recessive
- Mitochondrial pattern of inheritance
- Manifesting heterzygote
Which of the following mechanism is dysfunctional in patients androgen insensitivity syndrome?
- Androgen receptors are dysfunctional
- Inadequate androgen formation
- Dysfunctional release of androgens
- Dysfunctional transport of androgens
- Dysfunctional quantity of androgens
Which of the following is the most reliable method of detection of androgen insensitivity syndrome?
- Sequence the androgen receptor and cross-referencing with mutation database.
- Karyotyping
- PCR
- FISH
- Linkage analysis
What is the karyotype expected in a phenotypical female with complete androgen insensitivity syndrome?
- 46, XY
- 46, XX
- 45, X0
- 47, XXY
- 47, XYY
Which one of the following is NOT associated with partial androgen insensitivity syndrome?
- Accessory nipples
- Gynecomastia
- Hypospadias
- Infertility
- Micropenis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Awesome! I like how fluent the Dr. is. Keep the hard work.