Playlist
Show Playlist
Hide Playlist
Adaptive Immunity: T Cells
-
Slides Adaptive Immunity.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
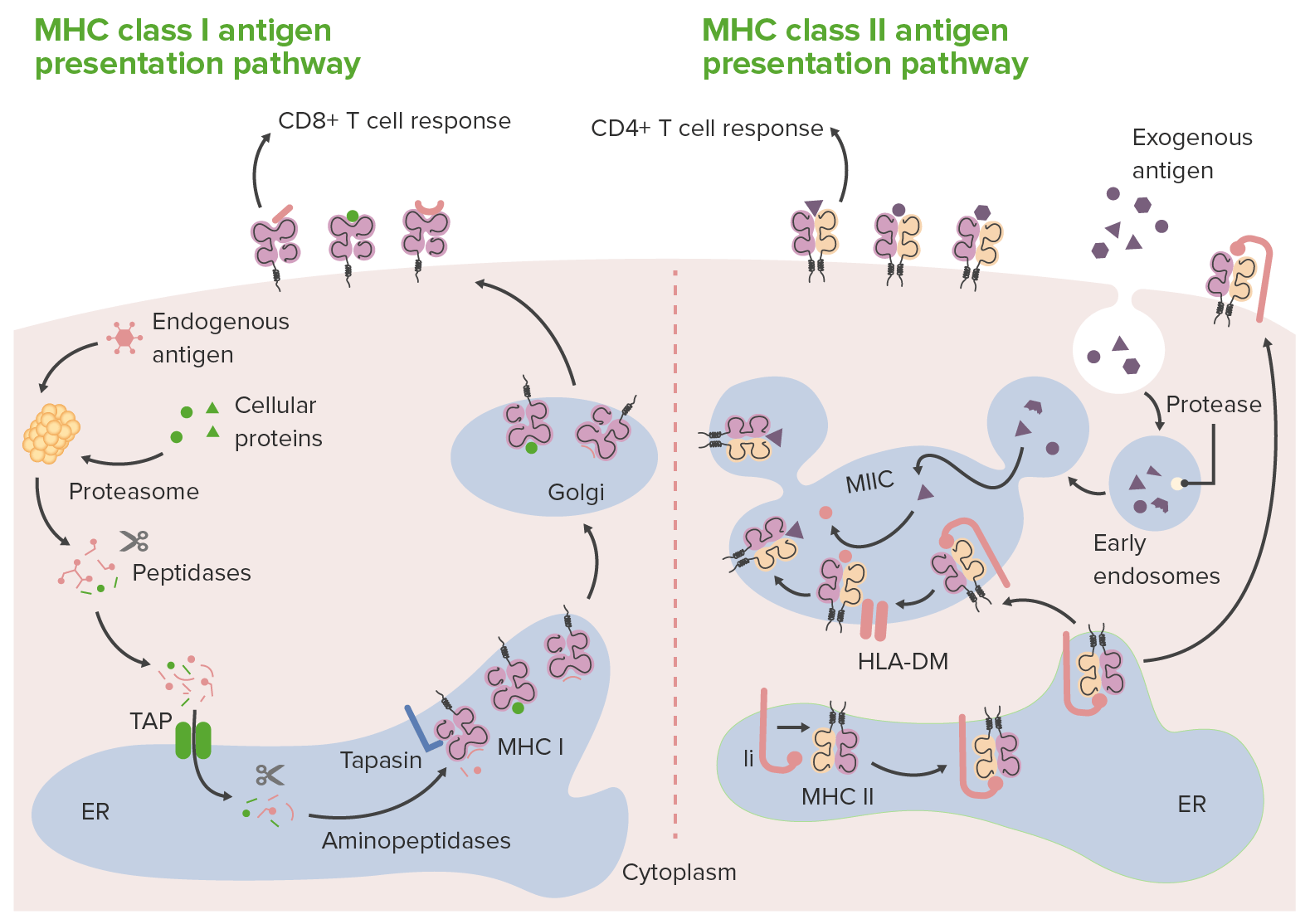
00:01 So let's talk about the effector functions from T cells. 00:05 And there are going to be two flavours of T cells that we need to deal with. 00:08 There are cytotoxic T cells and there are helper T cells. 00:12 And they will respond in different ways to dealing with infectious agents. 00:18 So, the first thing we have to deal with our infectious agents that are intracellular. 00:25 Viruses, certain intracellular bacteria, we need to be able to kill the cell that is harbouring them. 00:31 That's our only way to respond. 00:33 To kill an infected cell, we bring in cytotoxic T lymphocytes, killer T cells. 00:40 They are identified on their surface by a marker called CD8. 00:46 And I apologise for the immunologists, who named these various markers. 00:51 CD stands for cluster of differentiation. 00:54 And just knowing the number doesn't help you figure out what cell type it is. 01:00 You just have to memories it. 01:02 So cytotoxic T lymphocytes or killer T cells are also CD8+. 01:08 So that's how we recognise them. 01:11 So that CD8+ T cell needs to somehow recognise that that orange blob on the left hand side has become infected with a virus and to kill it. 01:21 How does it do that? Well, that blob on the left, any any cell in the body, is constantly surveilling its internal environment. 01:31 It's constantly breaking down proteins into peptides, and then presenting them out on their surface. 01:38 If everything that's inside the cell is normal, and is self, we leave it alone. 01:42 However, if there's an invading pathogen, an intracellular virus, those viral proteins will be broken down into little peptides, and they're presented on the surface of that cell via MHC class 1. 01:59 MHC stands for major histocompatibility complex, and it's class 1. 02:05 It's a specific kind of the MHC molecules. 02:10 So that infected orange blob is now expressing on surface MHC class 1 a normal molecule, but in it, bound to it, is a little tiny peptide that is derived from the virus. 02:22 And now specific cytotoxic T lymphocytes can recognise it. 02:27 And when they do, what they do is they release in a vectorial way vacuoles that contain granzyme and perforin. 02:38 The perforin punches holes in the target cell and the granzymes induce a proptosis. 02:44 So, the goal here is that we need to be able to recognise intracellular pathogens. 02:51 We do so via the generation of peptides bound to class 1 that can be recognised by CD8 cytotoxic T lymphocytes that will kill. 03:01 Great. Now we've identified a way to deal with intracellular pathogens. 03:05 What about extracellular pathogens? That's on the right hand side. 03:10 In this particular case, there are cells that run around the body, macrophages, dendritic cells, some endothelial cells a variety of antigen presenting cells. 03:22 So their job is to surveil the extracellular space and look for pathogens, look for microbes, look for invaders, and they're constantly surveilling the extracellular environment. 03:36 Everything that they swallow, gulp, eat, they will process into peptides that they will express on their surface with MHC class II. 03:46 So major histocompatibility complex class two molecules. 03:50 And those little peptides bound to MHC class II potentially allow helper T cells to recognise it. 03:57 If the outside world doesn't contain any new molecules, no new microbes, then all the proteins that are presented ourself, and we leave them alone. 04:08 However, if there's a microbe out there, a bacterium or fungus or whatever, the antigen presenting cell will gobble that up, sample it, put the peptide on MHC class two and display it so that helper T cells can come along. 04:23 So remember we said there are two flavours of T cells: the cytotoxic T lymphocytes on the left hand side, the helper T cells in the right hand side. 04:32 The marker for helper T cells or TH cells is CD4. 04:37 That's a way that we can tell when we do even a histochemical staining or flow cytometry, which population we're talking about. 04:45 Now the helper T cells recognise this newly processed peptide in association with MHC class II and will respond. 04:55 Now we don't want to kill the messenger. 04:56 We don't want to kill the antigen presenting cell. 04:59 Antigen presenting cell just saying, "Hey dude, there's infection going on out here." So, we want to have the T cell respond when it sees that process peptide plus class II, we want it to make cytokines, that will bring in other inflammatory cells. 05:15 So, the cytokines that are elaborated by that helper T cells are going to coordinate, regulate, activate macrophages and neutrophils and other elements of the immune system to go after that extracellular pathogen. 05:30 So two different flavours: killer T cells - recognising peptide plus class 1 on target cells and killing them. 05:39 And helper T cells CD4+, that are recognising extracellular peptide on edge of presenting cells and then orchestrating a response through cytokine production. 05:55 Cytotoxic T lymphocytes. 05:57 So they are recognising intracellular pathogen plus MHC class 1 and will kill. 06:04 And that's their major job in life, but they also will do additional things such as making cytokines. 06:13 Important point about the cytotoxic T lymphocyte is its specific killing. 06:19 Only the target will die as a result of the T cell interacting with it. 06:25 As opposed to the helper T cells. 06:28 So the helper T cells recognising extracellular pathogen peptide, in association with MHC class II on an antigen presenting cell make a whole variety of cytokines. 06:39 Those cytokines, however, just turn on the macrophages and neutrophils. 06:44 They're very potent, but they're pretty dumb. 06:47 And potentially once they get turned on, turn all their activities towards itself. 06:53 So you can have a lot of innocent by standard damage. 06:57 So the cytokines produced in this process will activate macrophages and neutrophils will recruit those effectors but there's potentially important nonspecific killing that's going on.
About the Lecture
The lecture Adaptive Immunity: T Cells by Richard Mitchell, MD, PhD is from the course Immune-mediated Diseases.
Included Quiz Questions
What is the function of cytotoxic T lymphocytes?
- Killing infected cells with intracellular pathogens
- Interacting with plasma cells to produce antibodies
- Recognizing infected cells by proteins presented via MHC II
- Releasing histamine and serotonin to kill infected cells
- Nonspecific killing of pathogens
What is the function of helper T lymphocytes?
- Orchestrating an immune response through cytokine production
- Recognizing infected cells with intracellular pathogens
- Specific killing of pathogens
- Recognizing microbial proteins presented on APCs via MHC I
- Releasing granzymes and perforin to kill infected cells
Which of the following are examples of APCs?
- Dendritic cells
- Neutrophils
- Mast cells
- Cytotoxic T lymphocytes
- Helper T lymphocytes
What is the mechanism by which cytotoxic T lymphocytes kill infected cells?
- Apoptosis
- Atrophy
- Necrosis
- Autolysis
- Opsonization
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |