Playlist
Show Playlist
Hide Playlist
Acute Sinusitis: Management
-
Slides FisherSinusitis InfectiousDiseases.pdf
-
Reference List Infectious Diseases.pdf
-
Download Lecture Overview
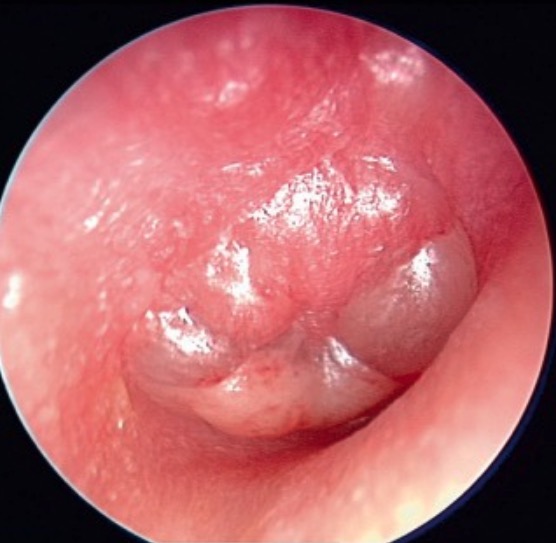
00:01 Now, what about therapy? It’s really difficult to study therapy in sinusitis because many patients who have bacterial sinusitis resolve spontaneously, they get better on their own. 00:17 After all, if you think about what’s going on, if they have pus in their sinuses and that pus will drain, symptoms should resolve and that they may resolve without any antibiotics at all. 00:33 There was a meta-analysis looking at placebo versus antibiotics. 00:41 And in that analysis they found that antibiotics reduced the clinical symptoms by just a relatively small percent. 00:50 So that the take home message is that antibiotics have only a modest effect and here are the data from that study. 01:00 In the antibiotic group, there was a cure or improvement in 64% and in the placebo group there was a cure or improvement in 32%. 01:12 So I think you can see that the effect of antibiotics is -- it’s real, but it’s very modest. 01:20 So what are our targets for antibiotics if we do think a patient has bacterial sinusitis? They are Streptococcus pneumoniae Gram-positive diplococci, Haemophilus influenzae pleomorphic Gram-negative coccobacilli. 01:41 So Moraxella is the third target and these are organisms that are Gram-negative cocci. 01:48 They actually kind of look like Neisseria on Gram stain. 01:53 And while I’m talking about the Gram stain, there is one trick that I have used in the treatment of bacterial sinusitis in my patients. 02:04 Believe it or not, I have had them blow their nose, blow these purulent secretions into a cellophane wrap. 02:13 Not into a Kleenex, but into a cellophane wrap so I can actually trap the secretions. 02:22 Then taking a little bit of the purulent secretions and doing a -- making a smear on a slide and doing a Gram stain, you can actually sometimes tell exactly what organism is causing bacterial sinusitis. 02:38 But I admit to being rather compulsive, but for example if you are in a situation, say, you’re doing missionary work or you’re working in a developing country, you could use a Gram stain to direct your antibiotics, you may be able to pick up that Streptococcus pneumoniae or Haemophilus influenzae. 03:01 So generally, we’re going to use amoxicillin plus or minus clavulanate and the clavulanate is a beta-lactamase inhibitor. 03:11 So the more concerned you are about a resistant organism or the possibility of anaerobes, you would use amox/clav, but amoxicillin alone is reasonable. 03:26 We generally give it in a higher dose in kids who are in daycare or in people aged under two or more than 65 years of age because resistant organisms are a little more common in those individuals. 03:44 Now if somebody has significant penicillin allergy, we generally use one of the cephalosporins, the oral cephalosporins, or a respiratory quinolone, but we do not give respiratory quinolones to children because of the possible adverse effects on connective tissue and tendons. 04:06 And prolonged quinolone therapy is also a concern in adults for the same reason. 04:14 The duration of therapy is widely variable and it’s difficult to do studies on duration of therapy. 04:25 Indeed, in many infectious diseases, we’re not certain how long to treat. 04:31 If it’s ten days recommended, would you believe eleven or would you believe nine? Would nine work as well as ten? You can see obviously how difficult it is to determine such a thing. 04:43 We may need to consider sinus surgery in patients who have serious complications as shown in this young lad. 04:50 He most likely has preseptal orbital cellulitis. 04:55 And this is a crucial examination if somebody presents like this. 05:00 You need to examine the extraocular muscles. 05:04 If the extraocular muscles are intact, if movement is perfectly normal, that’s an indication of preseptal and less serious orbital cellulitis. 05:16 But if the eyes don’t move, the infection is deep within the orbit and that’s an important physical examination technique. 05:27 So normally, this would occur with a severe acute infection refractory to antibiotics and the ENT surgeons would need to go in and open up the sinuses to allow them to drain. 05:46 A lot of people use corticosteroids because systemic steroids have been shown to have modest benefit. 05:57 But the studies do not permit us to recommend steroids and we know that topical steroids are of no benefit at all. 06:09 What about antihistamines? Antihistamines are not of benefit in absolutely normal individuals without a history of seasonal rhinitis, only in those patients would we use antihistamines because antihistamines can actually dry up the nasal secretions and may cause blockage of the ostia of the sinuses, which you’re trying to avoid. 06:34 Decongestants, like alpha-adrenergics, also are of modest benefit. 06:40 And if you decide to use those, you should be aware of the side effects, like increased blood pressure, CNS stimulation, insomnia, and the problem with these is after 24 to 48 hours, these agents may actually aggravate nasal congestion. 07:01 So if you’re going to recommend those for your patients, they should be used for a short time only and not in children. 07:10 One thing that is somewhat useful is that of saline irrigations. 07:16 And there are saline irrigations available and just gentle irrigation can loosen up some of the thick secretions. 07:28 They are better than the saline sprays that are commercially available. 07:32 However, you can imagine how difficult they are to study in children, so we don’t have good data about them in children. 07:44 Bottom line, topical steroids have not shown any benefit in treating sinusitis. 07:50 So despite how often they are given to patients, they’re really not indicated. 07:56 And that concludes my discussion with you today of sinusitis. 08:02 Thank you.
About the Lecture
The lecture Acute Sinusitis: Management by John Fisher, MD is from the course Upper Respiratory Infections. It contains the following chapters:
- Acute Sinusitis – Management
- Sinus Surgery and Adjunctive Measures
Included Quiz Questions
What is the recommended treatment for uncomplicated acute sinusitis?
- Symptomatic treatment for a upper respiratory infection
- Oral corticosteroids
- A 14-day course of amoxicillin/clavulanate
- A 10-day course of amoxicillin/clavulanate
- A 7-day course of amoxicillin
For a patient with sinusitis accompanied by eye-movement deficits, what is the recommended plan?
- Antibiotics and surgical consultation
- Intranasal corticosteroids and decongestants
- Hospitalization and intravenous antibiotic treatment
- Antibiotics and follow-up in 3 days
- Antibiotics and intranasal corticosteroids
Which of the following is the most appropriate next step in the management of a child with symptoms and signs of acute sinusitis and a foreign object in one nostril?
- Removal of foreign object and antibiotics
- High dose antibiotics
- Symptomatic management and nasal irrigation
- Removal of foreign object and inhaled corticosteroids
- Oral decongestants and high dose antibiotics
Which of the following adjunctive therapies for acute sinusitis has been shown to be most beneficial to patients?
- Saline irrigation
- Saline sprays
- Inhaled anticholinergics
- Inhaled beta agonists
- Systemic corticosteroids
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Dr Fisher has that ability that great lecturers have when lecturing. That plus proper use of multimedia results in a great lecture.