Playlist
Show Playlist
Hide Playlist
Acute Otitis Media (Middle Ear Infection): Signs and Symptoms
-
Slides OtitisMedia InfectiousDiseases.pdf
-
Reference List Infectious Diseases.pdf
-
Download Lecture Overview
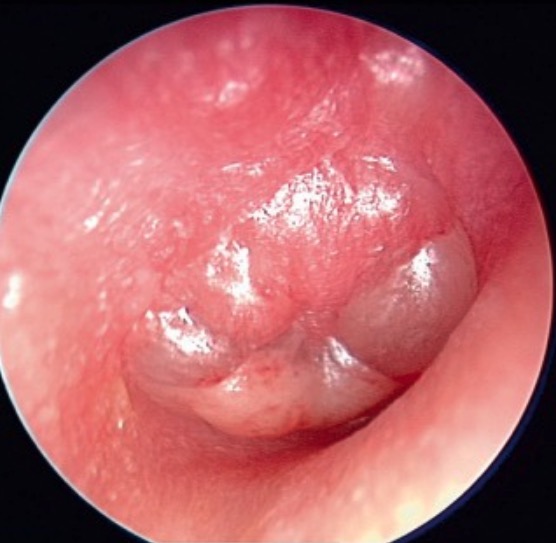
00:01 So an acute otitis media is a challenge for all physicians, especially pediatricians because the children may not be able to tell you that they have ear pain. 00:16 So ear pain and hearing loss, at least transient hearing loss, are fairly common in acute otitis media. 00:28 This is part of the challenge of identifying babies who have acute otitis media, sometimes it’s very difficult to examine them. 00:37 You definitely need a good assistant to hold the patient still. 00:45 There’s always the danger of injuring their external auditory canal with the otoscope. 00:52 A wiggling, screaming child is difficult to evaluate and the pediatricians are notorious for being very patient and it’s a very wonderful calling. 01:08 But what they’re looking for is marked tympanic membrane erythema and the eardrum can look red when a child is having forceful Valsalva maneuvers such as when they’re crying. 01:26 They’re also looking for a bulge in the tympanic membrane where it seems to be coming toward the observer. 01:36 That’s difficult to see. 01:39 Also, difficult to see is impaired mobility of the tympanic membrane, you really need a cooperative patient to do that. 01:48 And normally, the eardrum is supposed to be very mobile. 01:55 If it’s not mobile, there’s probably fluid behind it. 02:02 Some of the nonspecific clinical features that pediatricians think about are ear pulling, irritability, fever, decreased appetite, and sleep disturbance. 02:15 So I think you can see why a lot of kids get antibiotics because the physician just can’t be sure whether they have otitis media or not. 02:26 There is a number of possible complications with Otitis media. 02:29 This includes mastoiditis, tympanic membrane perforation, brain abscess and permanent hearing loss. 02:37 There’s a curious finding called bullous myringitis. 02:43 And to describe it to you, it would be a tympanic membrane with a bleb on it, a bulla. 02:53 And when I was in training, I was taught that that was pathognomonic of Mycoplasma pneumoniae ear infection. 03:03 But it turns out that it probably can be caused by any of the common pathogens and it’s not specific to Mycoplasma pneumoniae. 03:16 But the problem is just on the tympanic membrane, there is a bleb on it. 03:23 It presently is just a manifestation of severe acute otitis media, and other bugs can do it. 03:32 So the normal tympanic membrane moves and it moves like a flapping flag, it’s very sensitive to the least movement. 03:45 Well, it has to be for hearing. 03:47 So when it doesn’t move, there’s usually fluid behind it. 03:53 So it’s obvious that the clinical picture is the way we make this diagnosis. 04:02 In most instances, we are not going to be using a needle to get middle ear fluid. 04:11 That was done in days gone by, but we don’t do myringotomies anymore in most patients. 04:21 You would do a myringotomy and get some middle ear fluid, your ENT physician would generally do that, in somebody who had otitis media and was critically ill, and I think you can see why we would need to know what bug is making the patient critically ill. 04:37 In an extremely toxic individual with no response to antibiotics within 48 to 72 hours, we need to find out what’s there. 04:48 And in an immunocompromised patient, they can have funny bugs. 04:53 And I know of a patient that had actually tuberculous otitis media that was missed and missed and missed again until finally, one of the ENT physicians did a biopsy of some tissue around the middle ear and was able to make the diagnosis. 05:14 So we need to think of strange organisms in immunocompromised patients.
About the Lecture
The lecture Acute Otitis Media (Middle Ear Infection): Signs and Symptoms by John Fisher, MD is from the course Upper Respiratory Infections. It contains the following chapters:
- Acute Otitis Media – Signs/Symptoms
- Acute Otitis Media – Diagnosis
Included Quiz Questions
Which of the following best defines bullous myringitis?
- Bullae or vesicles on the tympanic membrane, without affecting the contents of the external or middle ear
- Bullae or vesicles on the tympanic membrane, affecting the contents of the external and middle ear
- Bullae or vesicles on the tympanic membrane, affecting the contents of the middle ear without affecting the external ear
- Bullae or vesicles on the tympanic membrane, affecting the contents of the external ear without affecting the middle ear
Which of the following patients with signs and symptoms of otitis media should receive tympanocentesis and culture?
- A 4-year-old on chemotherapeutic agents for leukemia
- A 5-month-old infant
- A 3-year-old girl with a second episode of otitis media
- Any patient with bullous myringitis
- Young children with non-specific symptoms of an ear infection
What is the most likely cause of bilateral erythema of the tympanic membranes in a seemingly healthy toddler?
- Crying
- Traumatic intracranial bleed
- Mastoid process injury
- Bilateral acute otitis media
- A viral upper respiratory infection
Which of the following is NOT a typical symptom of acute otitis media in a young child?
- Rash
- Ear pain
- Ear rubbing
- Hearing loss
- Ear drainage
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |