Playlist
Show Playlist
Hide Playlist
The Acute Abdomen – General Principles
-
Slides AcuteAbdomen Surgery.pdf
-
Download Lecture Overview
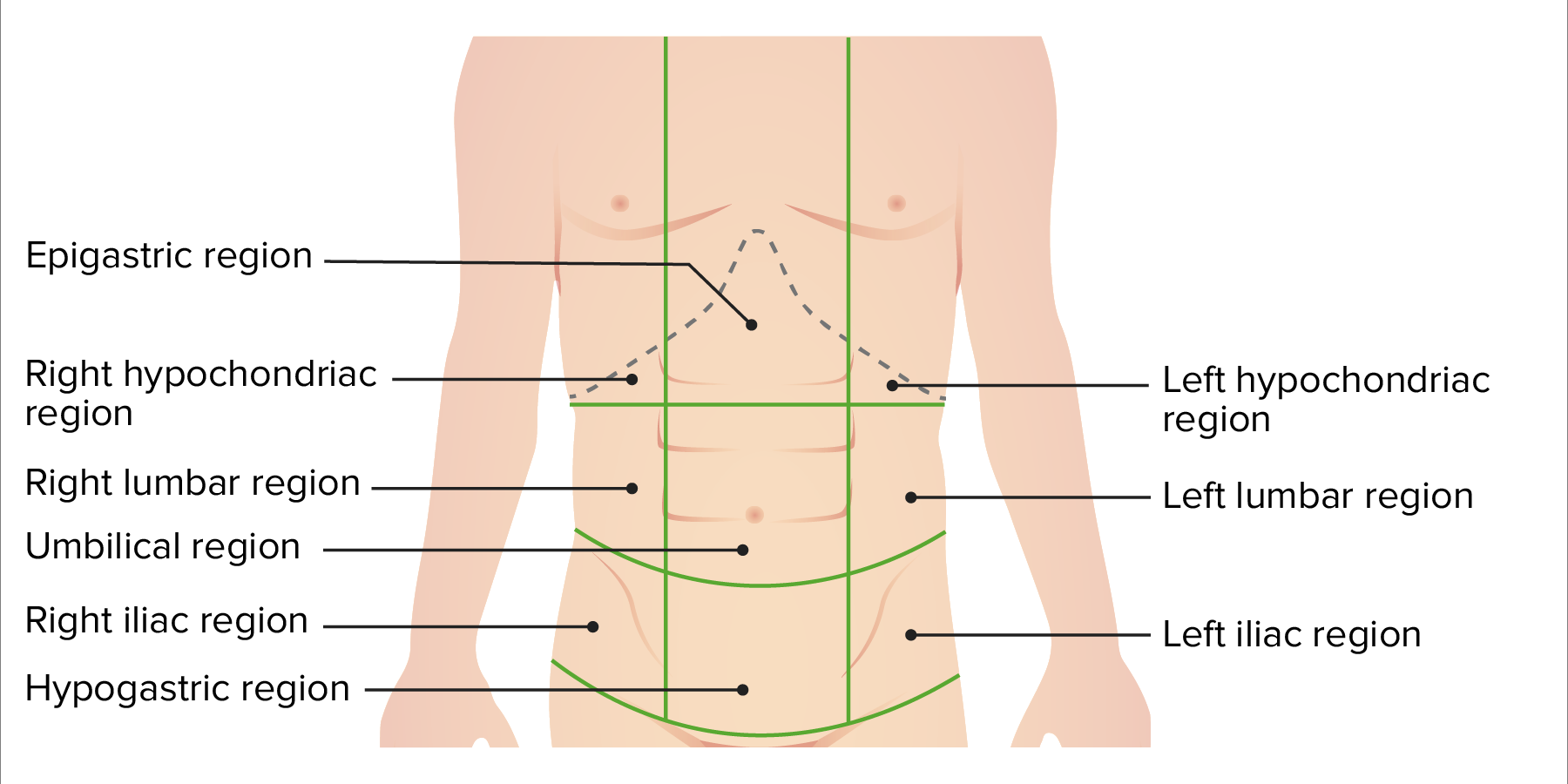
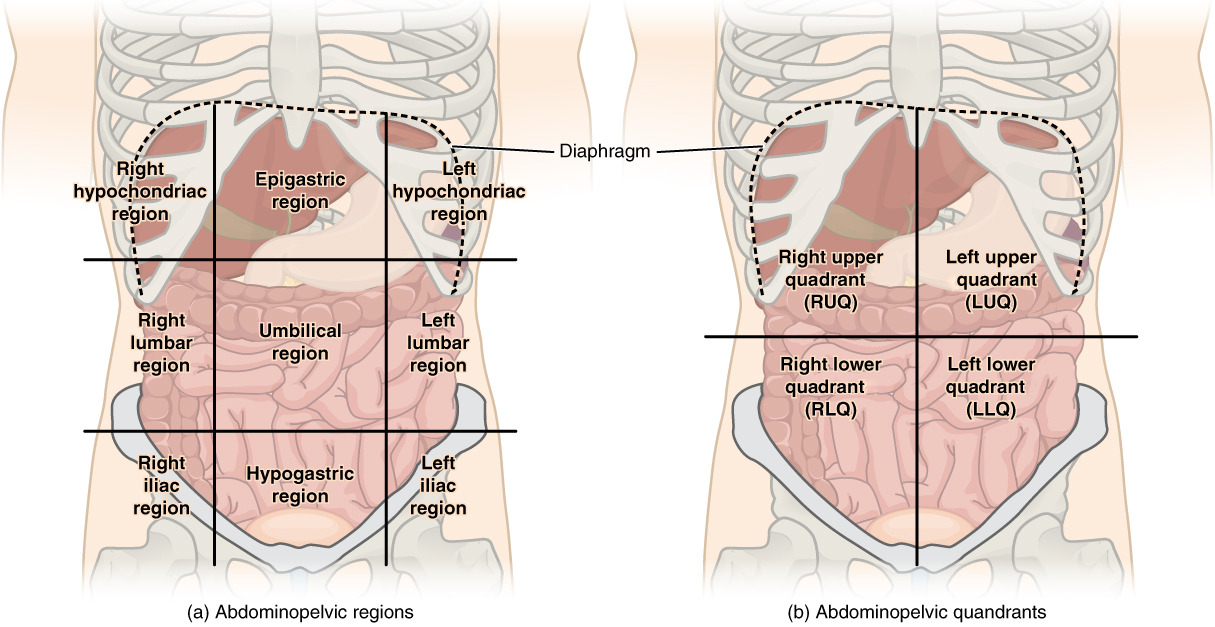
00:01 Merhaba. Tekrar hoşgeldiniz. Bugün, bu akut karın modülünde, bazı genel prensipleri tartışacağız. 00:08 Klinik bir senaryo ile başlayalım. Kendinizi acil serviste hayal edin. 00:15 üç günlük kramp ile acil servise başvuran 35 yaşında erkek hastanın karın ağrısı ve ishali var. Ateşi olduğunu söylüyor. Fizik muayenenizde, karnın tüm çeyreklerinde palpasyona yatkındır, ancak herhangi bir defans veya rebound göstermez. 00:32 Bunu bir saniyeliğine düşün. Bu hastanın cerrahi karnı var mı? Akut karın nedir? Bunlar bu modülde cevaplamayı umduğum bazı sorular. 00:53 Nedeni ne olursa olsun karın ağrısının ani başlangıcı akut karın olarak tanımlanır. 01:01 Peritonun farklı katmanları muhtemelen size çok tanıdık geliyor. Bu resme bir göz atın. Mavi anahat peritonun katmanlarını gösteriyor. 01:09 Peritonun parietal ve visseral olmak üzere iki katmanı vardır. 01:17 Karın ağrısı ve karın klasik olarak dokuz kadrana bölünmüştür. 01:24 Burada visseral ve parietal peritonun ağrısı arasındaki farkları biraz ayırt edeceğim . İlk olarak, viseral peritondan başlıyoum. 01:31 Enflamasyon viseral peritonu içeriyorsa ağrının yerini belirlemek zordur. Viseral ağrıya genellikle distansiyon ve iskemi aracılık eder ve ağrı büyük ölçüde karın orta hattında hissedilir. 01:45 Ancak parietal periton’un sinir lifleri omuriliğin bir tarafına veya diğer tarafına gider. 01:52 Bu karın ağrısının yerini lokalize etmemizi kolaylaştırır. 02:02 Burada, karnın konumuna göre çok çeşitli ayırıcı tanılar görüyorsunuz. 02:09 Bunları hızlıca gözden geçirelim. Karnın sağ kadranında akut kolesistit, kolanjit ve hatta hepatit düşünülmelidir. Karnın sağ alt çeyreğinde, apandisit düşünülür. Kadınlarda over torsiyonu / kistleri veya pelvik inflamatuar hastalık(PID) dahil jinekoloji patolojisini çok önemli bir şekilde göz önünde bulundurun. Karnın sol tarafına geçelim. 02:33 Sol üst kadranda, peptik ülser hastalığı düşünülmelidir. Mid-epigastrik ağrı tipik olarak pankreatit ile ilişkilidir. Yine, karnın sol üst çeyreğinde, dalak veya böbrek taşları ağrıya neden olabilir. Karın sol alt kadranına ne dersiniz? Divertikülit, kolon volvulus, kolon perforasyonunu düşünüyoruz. Belki de teşhis edilmesi en zor olanı klasik olarak ince bağırsak tıkanıklığı ile ilişkili ince bağırsaklar gibi orta hat yapıları ve bu durumda ince bağırsak perforasyonudur. Peki bir cerrah olarak hastaya yaklaşımımız nasıldır? 38 yaşındaki sağlıklı bir çocuğun klinik durumunu gördüğümde, kendime çok önemli üç soru soruyorum. 03:17 Öncelikle hastanın ameliyata ihtiyacı var mı? Sonra, hastanın ameliyata ne zaman ihtiyacı var? Son olarak, herhangi bir ek tetkik yapmak gerekli midir? Cerrahi dersleri boyunca genellikle bu üç soru üzerine çok düşündüğümüzü göreceksiniz. 03:39 Akut karın muayeneniz sırasında mümkün olduğunca erken zamanda bir cerraha başvurmanızı istememizin nedenlerinden biri budur. 03:45 Şimdi cerrahi gerektirebilecek ve aynı zamanda cerrahi karın olarak da bilinen bazı yaygın durumlara bir göz atalım. 03:52 Unutmayın, bunlar USMLE sınavı için çok önemli konulardır. 04:02 İlk olarak perforasyon; Batın grafisi çekerseniz ve bu görüntüde gösterildiği gibi diyaframın altında serbest hava varsa, bu hastanın daha fazla tetkik yapmadan acil bir keşif laparotomisine ihtiyacı vardır. 04:18 Ne yazık ki, serbest havanın veya pnömoperitonumun varlığı, size patolojinin ne olduğunu söyleyemez. 04:25 Şimdi iskemi hakkında konuşalım. Bağırsak iskemisi perforasyondan daha nadirdir, ancak yine de akut ve cerrahi karınların çok önemli bir nedenidir. 04:41 Klasik olarak parmak izi ve pnömatozis tanımlanır. Pnömatozis: bağırsak mukozasının iskemiye ilk ve en duyarlı katmanı olması nedeniyle oluşur. 04:50 Mukoza parçalandığında, hava daha sonra pnömatozis ile sonuçlanan ince bağırsak katmanlarına transmural olarak girmesine izin verilir. 04:58 Bunu bir abdominal röntgende parmak izi ve pnömatozis olarak göreceksiniz Şimdi kanama hakkında konuşalım. 05:12 Gastrointestinal kanamanın büyük çoğunluğu nonoperatif olarak tedavi edilmekle birlikte ve bunu operasyon dışı olarak yapmakta büyük başarı elde etmemize rağmen, hasta hipotansiyon gibi hemodinamik olarak instabil hale geldiğinde veya önemli miktarda kan transfüzyonu gerektirdiğinde, acil ameliyat için bir endikasyon teşkil eder. 05:30 Son olarak, ince bağırsak obstrüksiyonu; Amerika Birleşik Devletleri'ndeki en yaygın tanılardan biridir ve Amerika Birleşik Devletleri'ndeki en yaygın cerrahi tanılardan biridir. 05:44 Neyse ki bu hastaların çoğu için ameliyat gerekmiyor. 05:50 Daha sonraki bir ders modülünde tartışılacak olan bağırsak obstrüksiyonu genellikle önceki ameliyatlarla ilişkilidir. 05:55 Burada batın grafisinde, özellikle dik bir batın grafisinde, hava sıvı seviyelerini fark edeceksiniz. 06:04 Klinik inciler: Unutmayın, tüm akut karınlar ameliyat gerektirmez, ancak tüm cerrahi karınlar büyük olasılıkla akut karınlardır. 06:12 Muayeneniz için başka bir önemli gerçek, peritonit belirtileri, ister defans ister rebound olsun, daha fazla çalışma gerektirmeden cerrahi eksplorasyon gerektirir. 06:28 Akut karınla ilgili bu ders için bana katıldığınız için teşekkür ederim.
About the Lecture
The lecture The Acute Abdomen – General Principles by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
Where is visceral peritoneal pain usually felt?
- Diffusely in the abdomen
- At a distinct localized point
- In the lower abdominal quadrants
- In the lateral flanks
- In the pelvis
Which of the following combinations of the cause of abdominal pain and the clinical localization of the pain is INCORRECT?
- The right upper quadrant and mesenteric ischemia
- The left lower quadrant and diverticulitis
- The left upper quadrant/epigastric region and peptic ulcer
- The right upper quadrant and cholecystitis
- The right lower quadrant and appendicitis.
A 24-year-old woman presents with acute right lower quadrant pain. Which of the following pathologies MUST be included in your differential?
- Ovarian torsion
- Diverticulitis
- Hemorrhagic hemorrhoids
- Cholecystitis
- Peptic ulcer
Which of the following radiological signs does NOT suggest a surgical abdomen?
- Air in the rectum
- Pneumoperitoneum
- Thumb-printing
- Intestinal pneumatosis
- Air-fluid levels
Which of the following imaging findings is correctly paired with the clinical cause?
- Intestinal pneumatosis and ischemic bowel
- Foreign bodies and mesenteric ischemia
- Thumb-printing and uncomplicated small bowel obstruction
- Air-fluid levels and a bowel perforation
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
4 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Very simple and straightforward. Excellent use of the films to show each case - best example I've seen thus far. I always struggle with the radiology terms used in materials, especially if the accompanying graphic isn't clear.
It is perfectly explained, included important facts med students need to learn! Congratulations
His lecture is very cool mood.so My Brain can catch his speech easily.Hope these lectures will help me in my examination.
1 customer review without text
1 user review without text