Playlist
Show Playlist
Hide Playlist
Acne Vulgaris
-
Slides Disorders of sebaceous and apocrine glands.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
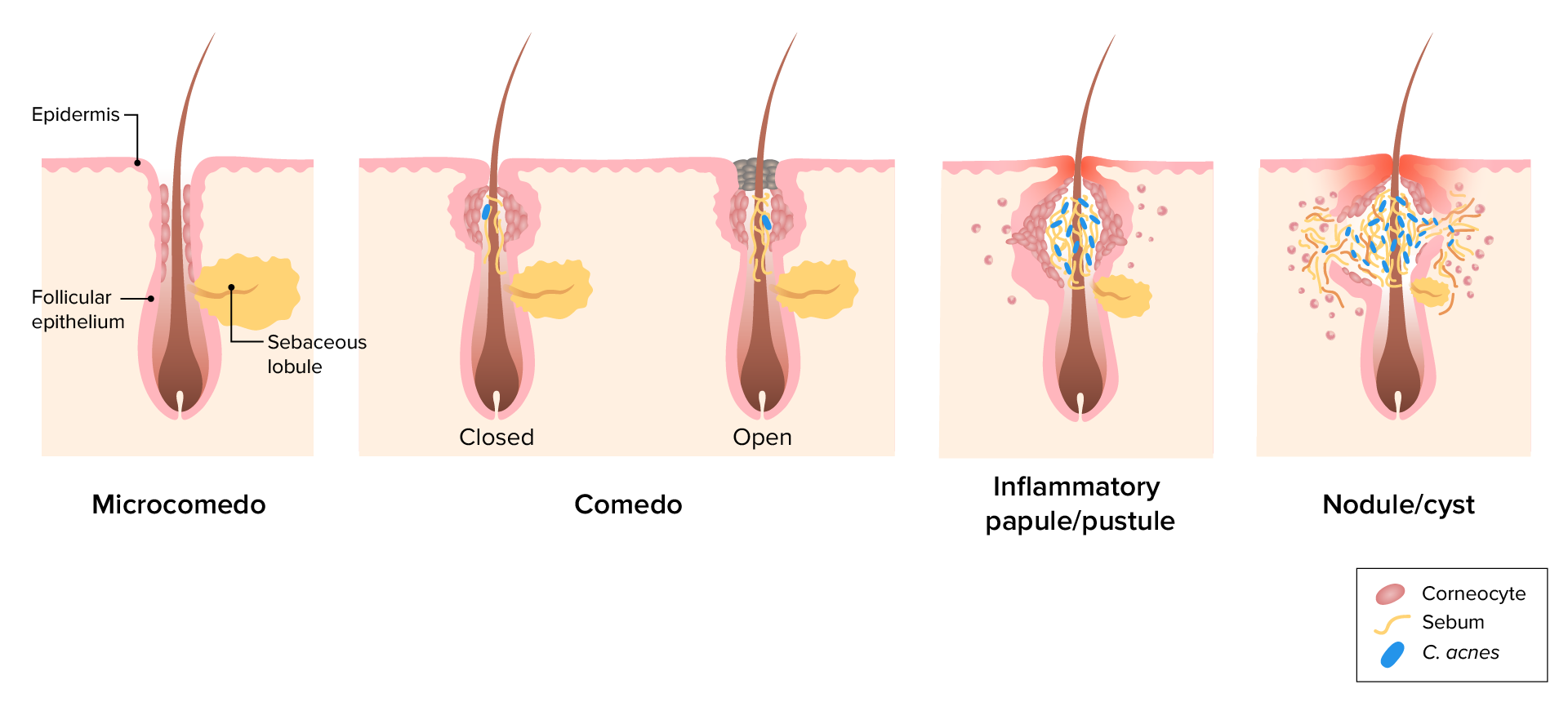
00:01 Ok, so as I've said, this is the most common skin disease of young persons and it occasionally develops in adulthood but most often folks have experienced it during their adolescence. 00:12 It's associated with significant psychological morbidity because that's a difficult time for everybody growing up in their adolescent years. 00:21 The etiology has to do with increased sebum production which tends to accompany puberty. 00:27 Essentially, with that increased sebum production, proprionibacterium acnes starts to colonize the hair follicles. 00:34 Now, this is an anaerobic diptheroid that thrives on the nutirent rich sebaceous glands so you start to increase sebum, this otherwise benign pathogen, starts to colonize those follicles. 00:45 It's unfortunately a very inflammatory type of bacteria and leads to a local immune response which causes follicular hyperkeratinization and ultimately, papules start to form and there's some downstream manifestations. 00:58 There are a number of different factors which have been associated with developing acne vulgaris. 01:03 Genetics is definitely one of them, we know that patients who have parents who had acne are more likely to develop acne themselves. 01:09 There have been a myriad of different factors that have been associated with diet that have been described. 01:14 One of the ones that keeps coming up is potentially, dairy exposure. 01:17 In addition there's a number of medications which have been implicated. 01:20 Glucocorticoids to be one of the primary ones. 01:22 But in addition, things like lithium and phenytoin have also been shown to be associated with the development of acne. 01:28 Eventually what happens is those papules that we talked about with follicular hyperkeratinizations can progress, become more inflammatory and then you're developing what's called comedones. 01:38 Open comedones called black heads and closed comedones called white heads. 01:43 These are essentially clogged keratin and sebum-filled hair follicles. 01:48 Ultimately overtime, those can progress to pustules and nodules. 01:53 Now importantly, acne vulgaris is not really associated with either telangiectasias or any of this eyelid involvement that we're getting from our patient. 02:05 Moving on though to talk about the management of acne vulgaris, typically we wanna try and minimize frictions. 02:10 So if somebody wears a helmet and it has a chin strap, that could contribute to the flares of acne. 02:15 You wanna avoid any particular triggers and there may be some idiosyncrasies about which patients are susceptible to which triggers but avoiding topical corticosteroids, avoiding oral contraceptive pills, and medications like lithium and phenytoin can help. 02:28 And ultimately, in terms of treating the disease, we start off with basic things like topical retinoids, benzoyl peroxides, mixtures of topical antibiotics like erythromycin and clindamycin can help. 02:39 For more advanced disease, we start to add oral antibiotics like tetracycline. 02:44 And lastly, for severe cases we can use isotretinoin. 02:48 A quick comment about isotretinoin, this drug is remarkably effective for acne vulgaris but there's a catch. 02:56 Isotretinoin is notoriously teratogenic, so you have to make sure if you're prescribing this medication that your patient is in two forms of birth control. 03:04 In fact, in many countries, you have to get special licensure in order to even prescribe this medication. 03:10 So there are certainly some features that support acne vulgaris but it still doesn't quite seem to fit the bill. 03:16 So I'm comfortable taking that one off and let's move on to systemic lupus erythematosus.
About the Lecture
The lecture Acne Vulgaris by Stephen Holt, MD, MS is from the course Miscellaneous Skin Disorders.
Included Quiz Questions
Which of the following is involved in the pathogenesis of acne vulgaris?
- Follicular hyperkeratinization
- Autoimmune reaction to gliadin proteins
- Colonization of aerobic bacteria within the hair follicles
- An adverse effect of tetracycline antibiotics
- Increased production of melanin
Which of the following statements is correct regarding the management of acne vulgaris?
- Sexually active female patients must use two forms of contraception before starting isotretinoin.
- Eyelid lesions are treated with topical antibiotics.
- Benzoyl peroxide is contraindicated in pregnancy due to its severe teratogenicity.
- Local skin friction is usually not a concern.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
great lecture! Dr. Holt makes it so simple to understand. I would recommend this lecture for any medical student