Playlist
Show Playlist
Hide Playlist
Tachycardia: Wolff-parkinson White Syndrome: Definition and Pathogenesis
-
Slides Tachyarrhythmia MultifocalAtrialTachycardia CardiovascularPathology.pdf
-
Download Lecture Overview
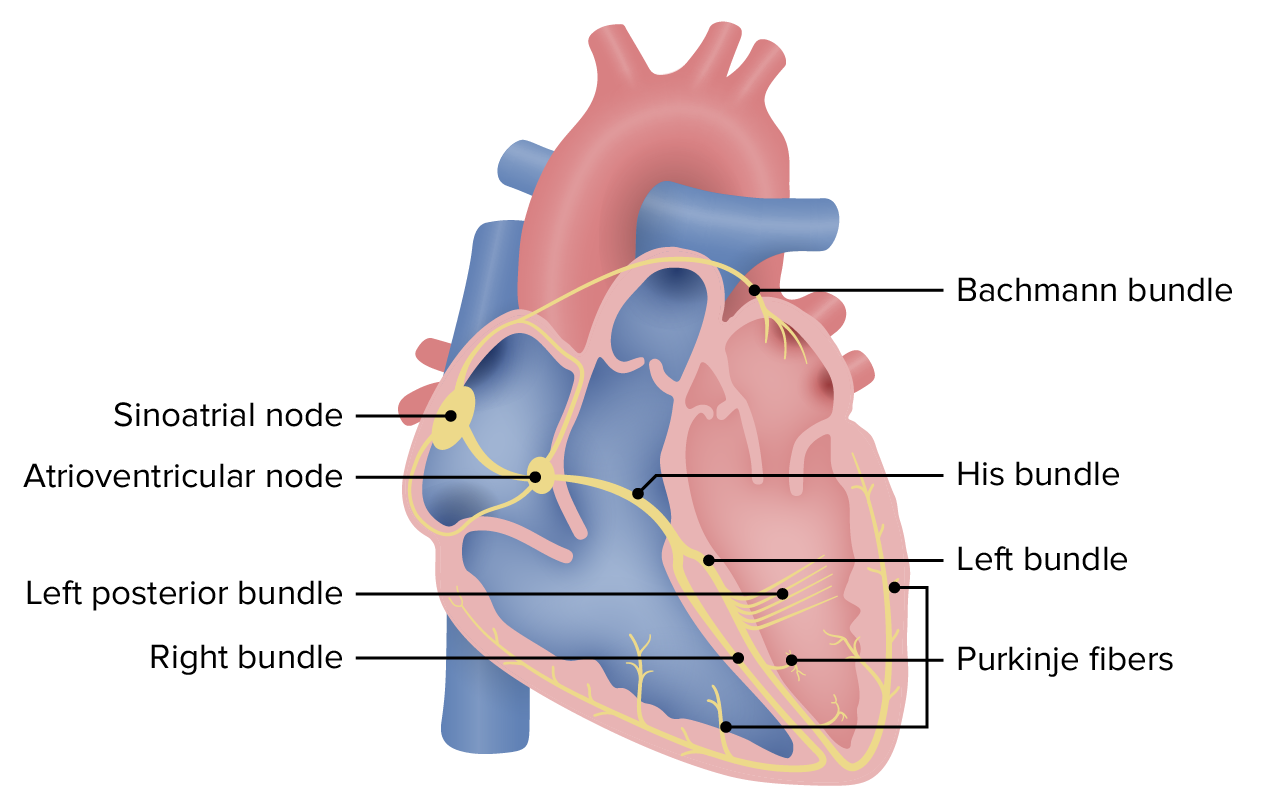
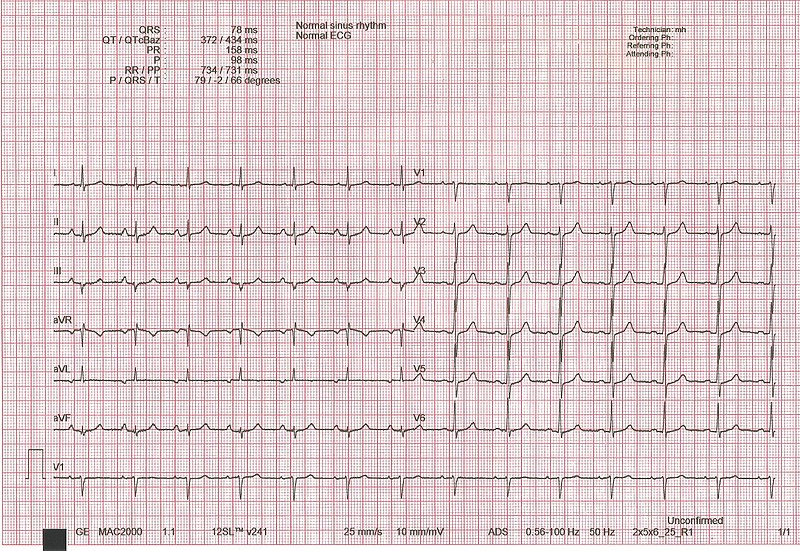
00:00 This particular SVT is WPW. So we have now completed our discussion of multifocal atrial tachycardia. I have noted to you the specific points that distinguish it from the others. In WPW, take a look at this heart and right off the bat, it explains everything that we need to know for WPW. We began this discussion some time ago. We will continue repeating this and now we have the following discussion. 00:28 First and foremost, you are paying attention to the green electrodes in the heart, in other words those nodal areas where the green becomes quite important. This is normal, the green of the SA node in the right atrium and then travels with the AV node. You see the cicuit right there. You see the green node. That green node represents the AV node. Every single impulse originating from the SA node should travel through there. There should be a little bit of delay. I am purposely emphasizing delay, why? In a little bit, there are certain drugs that you want to avoid at all costs in WPW and that point of me reiterating delay is huge. Now where the pathology is what you are seeing shaded in the brown. That is an accessory pathway. That pathway should not be existing ladies and gentleman because that pathway exists that pathway right there does not have the characteristic feature of being able to delay your impulse traveling from the atria down through your ventricle. Now what I am going to do is get straight to the clinical points because you can spend hours, days, weeks, what have you on WPW. We don't have the luxury of that kind of time. All we can do at this point is simply figure out this is my patient walking in. Take a look at the EKG, no doubt. It is WPW. And then after that, you get into as much detail as you wish. Education is as you know endless and it is absolutely enriching, but you must lay down the foundation first. So that pathway, accessory as you are seeing there in the brown shaded area is what you are paying attention to. It's not, it doesn't have the delay characteristics, so, therefore, any impulse have might then travel through it, guess what? It is going to go through it way too quick. Listen to what I just said. It passes through there too quickly. So what does that mean to you clinically? What does that mean to you in terms of an investigation known as your EKG? It is the fact that your electrocardiogram where an impulse from the SA node may then be traveling through your atria and then into the ventricle too quickly is what is that by definition? PR interval on EKG. So that PR interval once again you tell me what normal is. 03:00 The time is 0.12 seconds or 120 milliseconds to 200 milliseconds a.k.a. 0.2 seconds. Right? If it travels through that too quickly, what have you done to the PR interval? Good. Shortened it. Is that clear? Completely the opposite of what? AV block. All those AV blocks that we talk about ladies and gentleman that PR interval we know mostly those PR intervals in AV blocks were prolonged. What is the one big exception? Mobitz type II under second-degree AV block. 03:45 You remember that. If you don't my big attempt to make sure you review that. This is the time to solidify and distinguish each one of your arrhythmias. So far your focus is where? On that shaded area, that accessory pathway, impulse traveling through there too quickly, our first real diagnosis where the PR interval has been shortened. Are we good? Less than 0.12 and that is what you are looking for. Next well what is this called? It is called the bypass tract. You call this as a pre-excitation syndrome. So if by chance, you don't see the term WPW, Wolf-Parkinson-White, then the other names for this would be a pathologic accessory pathway disease or a pre-excitation syndrome, which is exactly what it is. Now, are we done? So far we have one component of WPW. There are going to be two others and those two will be related as we shall see moving forward. How would one develop WPW, Wolf-Parkinson-White? A congenital issue. What is happening? Instead of the impulses traveling through the AV, it will then bypass. Bundle of Kent is something that you want to keep in mind anatomically please, memorize that, causing earlier ventricular activation. What happens to your PR interval? It gets shortened. It is one pre-excitation syndrome. Keep in mind. As you move on into subspecialities or specialization in general, you will talk about many reentry, but, at least know one before this course is over and note well. It could be associated with afib. Imagine reentry, a circle. You are not going anywhere and you keep come back in the atria. The atria doesn't know how to respond. So, therefore, may lead into atrial fibrillation. 05:33 Atrial flutter or hypertrophic cardiomyopathy, so it could result in many issues, beginning with WPW. Ebstein's anomaly of the tricuspid valve, well with this especially with the lithium. 05:45 We have a patient who mighty have bipolarism is taking lithium. 05:51 Let us continue wtih WPW. So we have palpitations, dizziness, syncope. 05:57 I really could have repeat this any further. It is the fact that once your heart starts getting disregulated that you are not having proper cardiac output. There is no proper organization of blood flow. So, therefore, resulting in dizzziness, syncope, not good, palpitations.
About the Lecture
The lecture Tachycardia: Wolff-parkinson White Syndrome: Definition and Pathogenesis by Carlo Raj, MD is from the course Arrhythmias: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following statements is TRUE regarding Wolff-Parkinson-White syndrome?
- The PR interval is shortened.
- The PR interval is prolonged.
- Atrial pacemaker activity arises from different atrial locations.
- It is associated with a prolonged QT interval on ECG.
- It is associated with bradycardia.
Which of the following is associated with WPW?
- Atrial fibrillation
- AV block
- Congenital QT syndrome
- Dilated cardiomyopathy
- Mitral stenosis
Which of the following valves can be affected by lithium teratogenicity?
- Tricuspid valve
- Mitral valve
- Aortic valve
- Pulmonic valve
- Left-sided valves
What is the pathophysiological mechanism that defines Wolff-Parkinson-White syndrome?
- An alternative electrical pathway directly connects atria and ventricles and bypasses the AV node.
- An alternative electrical pathway directly connects atria and ventricles bypassing the SA node.
- The PR interval is prolonged.
- Normal conduction is preserved.
- Atrial pacemaker activity arises from different atrial locations.
Customer reviews
3,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
1 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
you seem to skip over Ebsteins anomaly and it kinda seems like you're saying it's a side effect of lithium. it isn't. it's a CONGENITAL anomaly that presents in neonates whose mother took lithium during pregnancy.