Playlist
Show Playlist
Hide Playlist
Retinoblastoma
-
03 Retinal Disorders V2.pdf
-
Download Lecture Overview
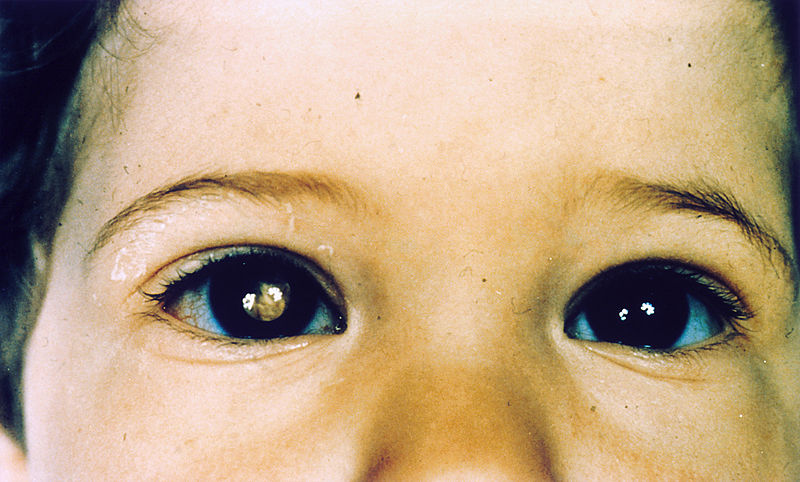
00:01 The topic here within the retina, this time would be a cancer. 00:04 Let's say that you have a child. 00:07 And in the child you notice upon fundoscopic examination, a white lesion, a huge white mass that you find on the retina. 00:18 We have occurrence of this in 1 in 14,000. 00:21 And as you remember, retinoblastoma is a tumor suppressor gene, is it not? And so when chromosome 13 is involved, and there's mutation of the retinoblastoma. 00:31 Anytime that you have a mutation, in which a tumor suppressor gene has been removed, there is increase or inhibit proliferation of your cells. 00:40 It promotes proliferation. Welcome to cancer, correct? Let's take a look a little bit of molecular pathology that you must know. A quick review. 00:48 We'll talk about in a second. If you take a look at the eye itself. 00:53 Look from the outside, the naked eye. What color is that? White. 00:58 We call this cat's eye reflex. We call that leuko. 01:01 Leuko meaning white, coria. 01:07 The review of molecular pathology for retinoblastoma is the following. 01:10 Whenever we talk about RB, then you're referring to which part of your cell cycle down here? Between G1 and S phase, correct? So before we go into DNA replication, you're in G1. 01:24 And here between G1 and S, think of having yourself security guards. 01:29 The security guards are then maintaining or preventing garbage from coming in. 01:33 What may then happen, every once in a while, is that there might be a disguise that the criminal might then take on in which unbeknownst to the security guard, allows for the criminal to come in. 01:43 What retinoblastoma is normally? Is the normal security guard. 01:48 And therefore maintains the quality of the type of cell that goes from G1 to S phase. 01:54 So what now happens when you have a retinoblastoma type of mutation? Is that the brakes have now been removed. 02:01 Removing the brakes by mutation that might be taking place of retinoblastoma. 02:06 When you remove the brake off of E2F, That E2F will then allow for that cell of whatever kind, and by that I mean, neoplastic cells or cancer cells, what have you, mutated cells. 02:19 From moving from G1 to S Phase and I make this motion because you know, that a cell never, if it's going to give rise to retinoblastoma or a cancer, right? In general, that cell is never going to come out of the cell cycle, or it doesn't want to. 02:36 So therefore when there is a mutation taking place in retinoblastoma, you do this by phosphorylating, don't you? Maybe by chance remember that name of that phosphorylation enzyme? Yeah, I get it. It is kinase, sure. But what kind of kinase? It's a Cyclin D Cdk4, remember that? Cyclin D Cdk4. 02:58 That kinase will then phosphorylate that RB normally to remove the brake so that E2F then allows for the cell to go from G1 to S Phase, correct? But what if there's a mutation taking place for which the retinoblastoma is forever mutated? Then E2F will allow, always allow for that cell, that criminal that to go from G1 to S phase giving rise to in this case, Retinoblastoma. 03:26 Now, once you notice that retinoblastoma, leukocoria in that child, then what may then happen years down the road? What other kind of cancer may then develop? Let's say, oh, maybe in the knee. Good. Osteosarcoma. 03:38 Retinoblastoma rise from primitive retinoblast. 03:44 Now, the picture here, is then pointing to what is known as your Flexner-Winstersteiner rosette. 03:50 Do you see that arrow there? Have a closer look, near that white arrow. 03:53 That then represents the rosette. 03:55 Well, what the rosette is an inner lumen there and around the lumen would then be your cancer cells. 04:03 You can have two types of rosettes here, Flexner-Winstersteiner, and possibly Homer Wright. 04:09 We focus here Flexner-Winstersteiner. 04:11 And there's every possibility that the retinoblastoma and the cancer cells may then move into your nerves. 04:19 Keep that in mind. We walk in through this. 04:25 On the left, showed you a picture in the previous discussion, what we have a Flexner-Winstersteiner rosette. 04:32 And in cross-examination, we notice in the orbit a huge retinoblastoma. 04:37 In this then would appear, if you will take a look at the patient, as being, what? Leukocoria or cat's eye reflex. 04:45 Compare the retinoblastoma type of cancer that's taking place in a child to what is going on here in the ocular region, specifically, do you see the area down at the bottom over to the left a little bit, area that's pigmented. 05:02 That's definitely not white. 05:04 It's not retinoblastoma, this is ocular melanoma. 05:09 Therefore could involve the conjunctiva, or the uvea. 05:13 And that's where we are in that region. 05:18 Primary intraocular neoplasia is what this is. 05:20 This is not, I repeat, not metastasis from somewhere. 05:24 And primary neoplastic overall, if it does go on to metastasis, for some interesting reason, which unknown to me, and really at this point we're still trying to figure out signally, but the point is, if there is metastasis from ocular melanoma, it has a predisposition of going to a liver. 05:46 Fascinating. Ocular melanoma. 05:50 A melanoma metastasis target, liver. Keep that in mind. 05:54 And the type of spread that you're looking for in melanoma, is what you are worried about will be through your blood vessels, hematogenous, not lymphatics. 06:05 It is moving to the liver via hematogenous route not lymphatics. 06:10 Kind of behaves like a sarcoma, doesn't it? Welcome to ocular melanoma. 06:17 The picture on the left that you see on fundoscopic examination, you can't miss that, a huge pigmented region. 06:25 Here we have orbital cellulitis. 06:28 This is not a stye. This is not ophthalmia neonatorum. 06:32 But what happens here is the fact that it is periorbital redness that you're seeing, but swelling. 06:36 Secondary to sinusitis. 06:39 The pathogens commonly Strep pneumo or Haemuphilus influenza. 06:43 You are looking for fever, apoptosis, bulging of the eyes, periorbital swelling as you see here, and the retina however is normal. 06:52 So there's nothing really going on with the retina, right? This is orbital, orbital cellulitis. 06:56 Management would be Nafcillin, ceftriaxone, and metronidazole perhaps. 07:03 Orbital cellulitis, be careful. 07:04 Just because you see puffy eyes does not always mean that you have issues within the eye, but this is a type of cellulitis.
About the Lecture
The lecture Retinoblastoma by Carlo Raj, MD is from the course Retinal Disorders. It contains the following chapters:
- Retinoblastoma
- Ocular Melanoma
Included Quiz Questions
What is the most common intraoccular malignant lesion in childhood?
- Retinoblastoma
- Melanoma
- Capillary hemangioma
- Rhabdomyosarcoma
- Dermoid cyst
In young children, retinoblastoma typically presents as which of the following?
- Leukocoria
- Anisocoria
- Retinal detachment
- Coloboma
- Aniridia
What is the most common primary intraocular neoplasm in adults?
- Ocular melanoma
- Retinoblastoma
- Dermoid cyst
- Capillary hemangioma
- Rhabdomyosarcoma
Metastasis from ocular melanoma most commonly targets which organ?
- Liver
- Lungs
- Brain
- Heart
- Kidneys
Customer reviews
4,5 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
He takes into consideration the most important points. One of the greatest teachers in this platform.
i rated this presentation because it is well prepared and well summarised medical students and residents should go through it.