Playlist
Show Playlist
Hide Playlist
Response-to-Injury Hypothesis
-
Slides Pathogenesis of Plaque Formation.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
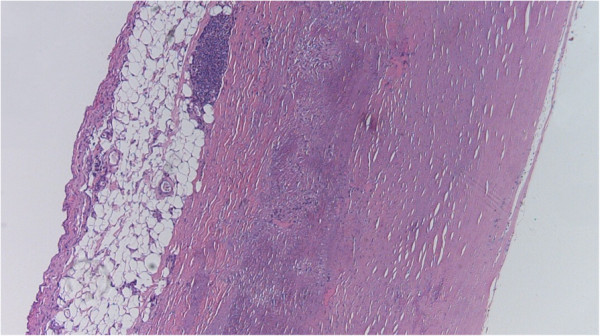
00:00 We've been discussing risk factors and kind of the general features of atherosclerosis. 00:06 Let's get a little bit down into the details about how the plaque actually forms because this also informs our thinking about how we can maybe inhibit that process and maybe even reverse the process. 00:21 So we're talking about pathogenesis. 00:24 Here we are, roughly halfway through the roadmap for atherosclerosis. 00:31 Again, by way of a review, remember that atherosclerosis is an interval based process. 00:38 It's composed of dysfunctional endothelial, a fibrous cap, overlying and atheromatous core and driven by macrophage and other inflammatory cells and processes. 00:54 That leads to narrowing of vessels or to destruction of the vessel wall. 00:59 Pretty straightforward. 01:01 Let's go now into greater detail. 01:04 How does this happen? And beginning in about the 60s, early 70s, we thought what was going on is that endothelium was damaged and that all of atherosclerosis was response to injury. 01:17 So that hypothesis, were showing a vessel cross section of the wall, the lavender cells on top endothelium, the orange cells in the middle media. 01:26 And we thought there was an injury to the endothelium, we would erode or denude the endothelium. 01:34 Platelets would bind, because we've exposed the underlying extracellular matrix. 01:40 We would then get the production of pro-inflammatory, pro-growth factors made by those activated platelets. 01:49 And we would do that over and over and over again. 01:53 And that would give us atherosclerosis. 01:57 Pretty straightforward. 01:58 A brilliant hypothesis, except it wasn't really accurate. 02:03 It turns out, because in this hypothesis, endothelial loss, denudation was a key feature, that turned out to be what was wrong. 02:12 And in fact, the endothelium is not lost in atherosclerosis. 02:17 So this is a transmission electron micrograph of a vessel wall, and the cell labelled at the top is endothelium. 02:26 The cell with the kind of the cleared areas is a macrophage. 02:29 And the underlying kind of white stripe is the internal elastic lamina. 02:38 And in this, in the internal elastic lamina allows us to demarcate everything above that is going to be the intima, everything below that is going to be the media. 02:47 And the macrophage is already there. 02:48 Remember, macrophages are going to be a major driving force, a pro-inflammatory innate immune response, that's going to be driving atherosclerosis, the macrophages already in the intima. 03:00 And yet the endothelium is perfectly fine. 03:04 It's still there. 03:05 So we never lose the endothelium and atherosclerosis in the typical way that atherosclerosis develops. 03:15 This gets back to thinking about the normal health and maintenance, the care and feeding of your endothelial cells, and normal tension, normal blood pressure, normal laminar flow, normal growth factor production by under line cells and epithelial cells, fibroblasts, macrophages, normal cytokine production and normal levels of oxygen NPH lead to a healthy state of the endothelium. 03:44 And that endothelial will make appropriate levels of growth factors and vasoactive mediators controlling whether the vessel tone is increased, or, relaxed, it will make appropriate levels of adhesion molecules and anticoagulant so that blood stays in a liquid phase. 04:02 So a healthy happy endothelial cell actually requires the input of a number of normal conditions to have normal outputs. 04:11 Let's talk about endothelial dysfunction. 04:14 So when we have turbulent flow, when we have hypertension, when we have increased inflammatory cytokines, when we have activated compliment, bacterial products, cholesterol and other lipid products, if we have advanced glycation end products as associated with diabetes, if we have too high level of hypoxia, or acid, if we have other inflammatory things like viruses and cigarette, smoke, we have endothelial cell dysfunction. 04:45 And now the endothelial cells make abnormal levels and different suites of growth factors and chemokines to recruit inflammatory cells, they make other cytokines, they are more pro-coagulant, they're going to be more likely to clot. 05:00 They're going to be more likely to be adhesives. 05:03 So to recruit inflammatory cells, they're going to make more vasoactive mediators so that we're going to tend to see vasospasm. 05:11 And we're going to see increased levels of histocompatibility molecules so that we have an increased inflammatory response. 05:19 So endothelial dysfunction not endothelial loss is what is going to be the primary initial driver for the development of atherosclerosis. 05:29 Just as an example of that, if we look on this, on this image, control blood vessel that is not inflamed and not activated. 05:40 Labelled inflammatory cells, in this case, neutrophils that have a fluorescent label built into them, do not stick to the vessel wall. 05:49 If we stimulate on the right hand side, those same blood vessels with various inflammatory cytokines, interleukin1 tumour necrosis factor, or other things such as certain cholesterol byproducts, we will now activate that endothelium. 06:05 It will become dysfunctional and will suddenly recruit a whole bunch of neutrophils, which will release their inflammatory mediators and will begin to drive the process of atherosclerosis development. 06:15 So, endothelial activation and dysfunction very much are the upstream drivers of atherosclerosis development.
About the Lecture
The lecture Response-to-Injury Hypothesis by Richard Mitchell, MD, PhD is from the course Atherosclerosis.
Included Quiz Questions
The primary cause of atherosclerotic plaque formation is...
- ...endothelial dysfunction.
- ...increased pro-inflammatory substances.
- ...endothelial loss.
- ...endothelial hyperplasia.
- ...chronic cell injury.
What is the normal flow in a blood vessel?
- Laminar flow
- Rotational flow
- Turbulent flow
- Unsteady flow
- Compressible flow
How does a dysfunctional endothelium stimulate plaque formation?
- Increases cytokines
- Prevents hypoxia
- Controls acidosis
- Maintains normotension
- Regulates growth factors
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |