Playlist
Show Playlist
Hide Playlist
Rabies Virus – Rhabdoviruses
-
02-46 Rhabdoviruses.pdf
-
Download Lecture Overview
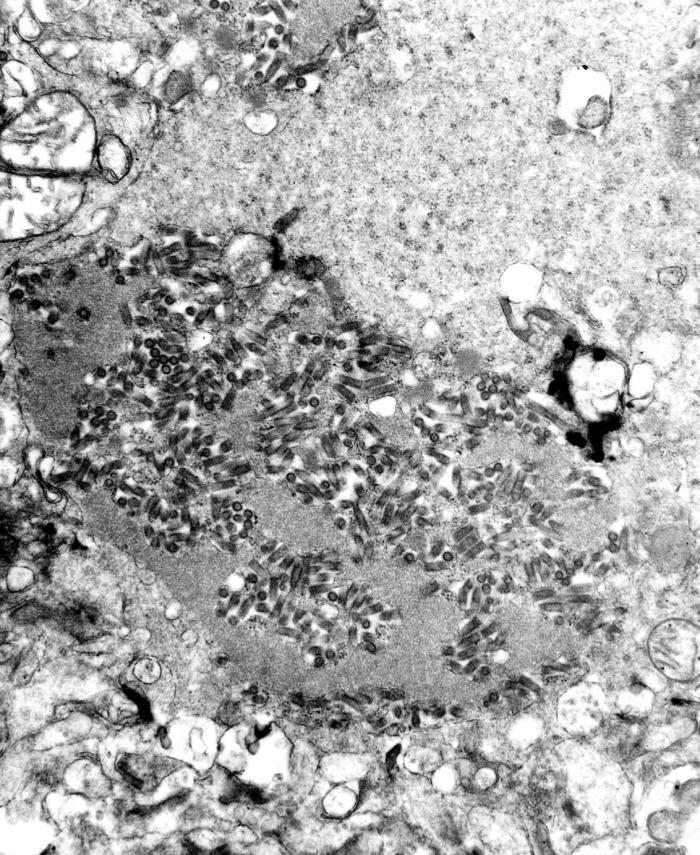
00:01 The rhabdoviridae, viruses. 00:05 Rhabdoviridae are mid-sized, enveloped viruses with a helical capsid, and they appear bullet-shaped. 00:11 You can actually see several of them on the transmission micrograph on the right side of the slide. 00:17 They contain a linear, single-stranded, negative-sense RNA genome, which means that they must also carry a RNA-dependent RNA polymerase, which they do to help them transcribe their genome. 00:31 The important virus here is the rabies virus, and we'll spend some time talking about what that looks like. 00:39 Rabies virus in the incubation period, so after exposure to rabies, can last silently, asymptomatically, up to a full year or so. 00:51 Now the exposure, as you'll probably remember from watching movies and hopefully, the literature, can come from exposure to a rabid animal. 01:01 nd depending on where the incubation or, excuse me, where the inoculation occurs, affects how long the duration of the asymptomatic incubation is. 01:11 Why is that so? Because the virus has to travel slowly, retrograde to the central nervous system. 01:19 So, if one is bitten, for example, on the first toe, it has the entire length of the body to travel to get way up here. 01:27 If one is bitten on the nose, well, say, "Goodbye, Charlie," because you're gonna be gone much sooner than a whole 365 days. 01:35 So, if one is lucky and there's been an exposure peripherally, then it'll be a longer duration of the incubation period. 01:42 If one is looking for the virus at that time, it'll be very difficult. 01:47 One might be able, on biopsy, to see viral effects by scanning electron microscope in the muscles surrounding the bite, but the patient won't have developed antibodies of a low titer of the virus. It would have to be a risk-based diagnosis. 02:03 When the disease actually starts, there is a 2-10 day prodrome, which includes nonspecific viral symptoms. 02:12 So fever, nausea, vomiting, very typical, patient has anorexia, headache, lethargy Again, you could think of this as, again, a flu-like illness. 02:22 However, if they're able to give you the history of the exposure, the history of the bite, or whatever the exposure was for the rabies, then one could actually, at the site of the exposure, be able to find a high titer of rabies virus. 02:39 And one could at least start to support the patient at that time. 02:44 How successfully would be, well, it's pretty much unknown. 02:48 There still won't be antibody because the immune system is still waking up to the fact that there has been this exposure to a foreign substance, to the rabies virus. 02:59 After the prodromal period, there is an inexorable progression to the neurologic component of rabies. 03:04 And this is the phase that everybody recognizes as classic rabies. 03:08 So the hydrophobia, fear of water, pharyngeal spasms, hyperactivity, anxiety, depression, altered consciousness, paralysis, delirium. 03:18 This is, sort of, the brain on drugs. 03:21 So, think of every part of the brain as sped up on caffeine or speed or something, and you get a picture of what these patients are like, completely out of control. 03:30 This lasts for 2-7 days, and at this time, you can finally start to make a very clear diagnosis after a clinical suspicion. 03:39 So, biopsing many highly innervated sites, so any of the glands, the skin, the eyes. 03:46 The classic spot is the hair follicles at the base of the neck, and one can see or one can demonstrate the rabies virus there. 03:54 One also can find the rabies' virions through saliva and antibodies now detectable in the serum and the central nervous system. 04:03 Ultimately, and despite medical attempts, the patients progress to coma. 04:07 And here is where they encounter death through cardiac arrest, hypoventilation, shock, sometimes secondary infections. 04:15 And this process may take from, you know, immediately following the neurologic complications, or up to 14 days, if there's a secondary infection. 04:25 So, where does rabies come from? Well, unvaccinated domestic animals, dogs and cats, or feral dogs and cats. 04:34 Also, skunks, raccoons, bats are classic. 04:37 The transmission, of course, is the bite from any of those infected animals, but so, too, aerosols. 04:44 So think about saliva or body fluids, excreta, urine, feces, from any of those. 04:51 This accounts for some of the reports from seeing a bat flying around the bedroom and then somebody acquiring rabies. 04:59 If the bat was dropping or exchanging saliva, it is possible for there to be transmission of that mechanism. 05:06 So, too, there are some reports of bats in the ceiling above a bed, above a hospital bed, in fact, and somehow, the saliva aerosolized through the ventilation system and the patient acquired it. 05:19 So, it's unfortunately very easy to acquire the rabies virus from excreta, saliva, urine, etc., from animals. 05:30 Diagnosis. 05:32 It's a neurologic, it's a clinical diagnosis. 05:34 Getting the history of the exposure if one is lucky, but again, as with the hospital bed and ceiling encounter, one may not actually see the animal or the bat which might have been the exposure. 05:47 So, with the diagnosis, one can do the biopsies as we mentioned in the previous slide. 05:53 One could also look pathologically on those biopsies for the presence of the Negri bodies in infected brain. 06:00 And the image on the slide shows you with several green arrows these highly eosinophilic collections. 06:06 Those are a collection of capsids, of virion capsids from the virus all together, as they're starting to exit cytoplasm in the process of making new virus. 06:18 So, clinical diagnosis, for sure, and the treatment. 06:25 Well, I don't have much to say about the treatment, so let's start with prevention, , because that's the best way to treat rabies, to avoid it in the first place. 06:32 So, pets require vaccinations. 06:35 High-risk personnel, perhaps Animal Control officers also require vaccination, and there is a very good vaccine out there. 06:43 However, most often, the prevention is actually a prophylactic approach after the exposure has occurred. 06:49 So, if there's a known bite, immediate attention in a medical personnel, cleaning the wound deeply with injection to try and get as much of the rabies-containing saliva out of the wound. 07:01 And then immunization with a killed rabies vaccine, and there will be continued immunizations at a specific series at day 3, 7, 14, 21. 07:12 Thankfully, the vaccine series is much less frequent, much less painful than it used to be, but it is still 5 separate shots. 07:21 Also importantly, because one wants to create an immune response at the immediate time of the exposure without waiting the 2 weeks for immuno- prophylaxis from the vaccine to develop, there is passive immunization with rabies immunoglobulin And that is injected if one knows where the bite occurred, half of the injection is at and around the site to the bite. 07:45 And the other half is in the contralateral, deltoid from which the vaccine was given because if you gave it at the same site, it's going to inactivate the vaccine's effect. 07:56 Treatment. 07:56 Unfortunately, there is no known effective treatment for symptomatic rabies, which is almost 100% fatal. 08:03 There are only 29 cases of confirmed survivors in the entire world, and most survived in neurologic sequelae. 08:10 Palliative therapy can be used to lessen symptoms including sedatives, antipsychotics and analgesics. 08:16 There are a few aggressive experimental treatments that have been attempted, typically in combination with each other These include immunotherapy, antiviral therapy, neuroprotective therapy such as ketamine and hypothermia, minocycline and medications that prevent cerebral vasospasms. 08:34 However, none of these therapies have been proven to be efficacious. 08:38 So, currently, there's no recommended use of the protocol. 08:42 It is simply support, support, support, and hope for the best. 08:46 So, the rabies virus, a very difficult one because there's truly no hope for the patients infected. 08:52 The best approach is to prophylax against it, and avoid, at all cost, the bite of a rabid animal.
About the Lecture
The lecture Rabies Virus – Rhabdoviruses by Sean Elliott, MD is from the course Viruses.
Included Quiz Questions
Which of the following corresponds with the typical shape of the rabies virus, as seen in transmission electron microscopic images?
- Bullet-shaped
- Brick-shaped
- Worm-like
- Spherical
- Polyhedral
Which of the following adequately describes the genome of the rhabdoviruses?
- Linear, single-stranded RNA
- Circular, single-stranded DNA
- Linear, double-stranded DNA
- Circular, single-stranded RNA
- Circular, double-stranded DNA
The non-specific prodromal phase of infection by the rabies virus typically lasts...?
- ...2–10 days.
- ...12–20 days.
- ...24–30 days.
- ...30–40 days.
- ...60–365 days.
Which of the following viral inclusion bodies do you expect to find upon histological evaluation of the diseased neurological tissue of a patient infected by the rabies virus?
- Negri bodies
- Guarnieri bodies
- Bollinger bodies
- Cowdry type A bodies
- Torres bodies
The type of vaccine used for the prevention and prophylaxis of infection by the rabies virus is which of the following?
- Inactivated/killed
- Live attenuated
- Recombinant
- Subunit
- Toxoid
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |