Playlist
Show Playlist
Hide Playlist
Infections of the Upper Pediatric Airway: Peritonsillar Abscess (Quinsy)
-
Slides Headandneckinfections Pediatrics.pdf
-
Download Lecture Overview
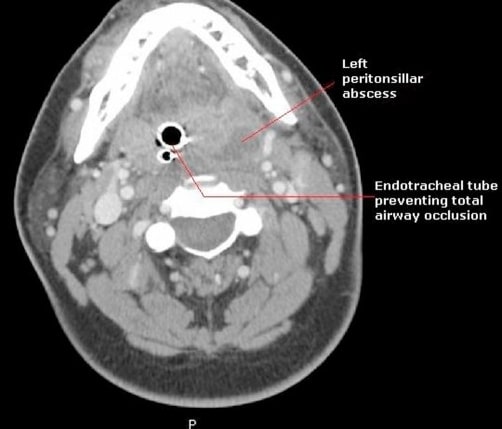
00:00 Let's switch gears to the next upper airway infection, which is a peritonsillar abscess. We're moving a little bit further back in the mouth now. This is an abscess that occurs in the peritonsillar space, just in the back of the throat. It may start as a cellulitis and then progress. 00:18 It's usually a polymicrobial infection including <i>Streptococcal</i> species, <i>Staph</i>, <i>Anaerobes</i> or maybe <i>Haemophilus</i>. So this is a mixed infection. What's key and the most important clinical pearl for you is trismus. If a patient doesn't want to open their mouth, there is a high likelihood they have a peritonsillar abscess. However, the trismus may make the exam difficult because it's harder to see back into the throat. Nonetheless, you really have to try because it's an exam that makes the diagnosis in most cases. Older patients will often report that they have a unilateral sore throat. It hurts on 1 side but not on the other. Younger patients often can't report this. When you look inside, you will notice a large fluctuant tonsil. It may have obvious need to rupture or it may just be red and swollen. One trick is you may see that the uvula is deviating towards the unaffected side. The swelling on 1 side pushes the uvula over. In severe cases, the airway may be uncompromised. Here's a CAT scan you can see of a patient with a peritonsillar abscess. We don't usually get a CAT scan. You can usually figure it out on physical exam alone but if it's complex you might need to do that. So, how do we manage these patients? There's no role for labs in a patient with peritonsillar abscess. A blood culture is almost always negative and we're going to drain this anyway. If you wanted to, you could certainly culture the pus that comes out when you drain it. If a deeper infection is suspected, we will get that CAT scan to make sure where is this going, what do we need. I've seen cases where it went extended through the back of the neck and all the way down into the mediastinum. If it's not yet drainable, if it appears to be more of a phlegmon or pre-abscess cellulitis, we're going to start off by treating with antibiotics. The antibiotic choice is ampicillin/sulbactam. It's a broad-spectrum agent that's going to kill <i>Staph</i> as well as many of the others. It will miss MRSA so if this is a rapidly progressive and aggressive peritonsillar abscess, you might want to do clindamycin instead. 02:41 Eventually if they are getting better on the ampicillin/sulbactam we will transition to amoxicillin/clavulanic acid. Second line is that clindamycin generally for coverage of MRSA. 02:55 Also, steroids are indicated but only if there's an acute airway obstruction. We don't want to blunt the immune response against infection. If it's drainable, the cure and the best treatment is to call the ear, nose, and throat doctors and ask them to do an incision and drainage. That's really how we're going to get these kids better faster and get them on their way home. We often might add antibiotics especially if there's a lot of cellulitis. If a patient keeps coming back in with recurrent tonsillar infections, you might consider down the road a tonsillectomy but that decision isn't made lightly because remember tonsillectomies are not only painful, they carry the risk of severe bleeding.
About the Lecture
The lecture Infections of the Upper Pediatric Airway: Peritonsillar Abscess (Quinsy) by Brian Alverson, MD is from the course Pediatric Infectious Diseases. It contains the following chapters:
- Pathology of Peritonsillar Abscess
- Management of Peritonsillar Abscess
Included Quiz Questions
Which of the following physical findings is most consistent with peritonsillar abscess?
- Inability to open the mouth
- Inability to tip the head to look up
- Inability to tip the head to look down
- Inability to move the head side to side
- Inability to close the mouth
Which of the following is NOT a common organism that causes peritonsillar abscess?
- Pseudomonas
- Staphylococcus
- Streptococcus
- Anaerobic species
- Haemophilus
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
3 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
very interesting assessment and thank you for the antibiotic regimen.
Excellent lecture with emphasis on most important clinical signs and clear categorization regarding management.
Great aproach It would be lovely if you indicated dose for drugs Thanks