Playlist
Show Playlist
Hide Playlist
Osteoarthritis (OA): Pathogenesis
-
Rheumatology I 01 Non-Autoimmune Arthritis.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
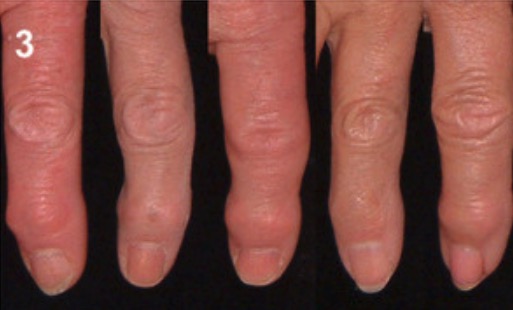
00:01 Pathogenesis. It's quite complex: biochemical, biomechanical, cytokine-mediated, to a certain extent, right? Because you do have WBCs, but it's < 2000 in the synovial fluid. 00:15 Now, commonly, the problem is obesity. 00:19 So you take a look at the patient who's obese. 00:21 Apart from Diabetes Type 2 and so on and so forth, that the patient has developed, metabolic syndrome as you know, the patient now is at risk of definitely developing osteoarthritis. 00:30 A lot of weight that the patient might… has to then put on the knees and such. 00:35 That incidence, unfortunately, osteoarthritis increases with age. You can't help it, right? But there are certain things that we can do to maybe protect ourselves. 00:43 Depends on our, well, genetics. 00:47 Signs and symptoms. Well, important here. 00:50 As I told you, as you move through osteoarthritis in your head, you're going to be comparing this with rheumatoid arthritis. 00:58 In rheumatoid arthritis… and that's the first time that I'm giving you a true comparison now. 01:03 In rheumatoid arthritis, as you know, it's a autoimmune issue, isn't it? Autoimmune most likely going to affect a female, no doubt. 01:11 Autoimmune diseases. 01:14 Here, we have a lot of information. 01:16 In rheumatoid arthritis, for example, the WBC count in the synovial fluid can exceed 2,000 cells per microliter. 01:24 They are generally in the range of 5,000 to 50,000. 01:28 Remember, what should be normal for synovial fluid? It's less than 200 cells per microliter. 01:34 Next, the patient says... 01:37 Who's your patient, a lady, young, maybe 35 or so? And she tells you, "Doc, I wake up in the morning and I'm having a hard time moving." "How long does it take before you get better?" "Hmm, maybe about an hour, hour and a half." That's a long time. 01:51 That's rheumatoid arthritis. 01:53 "And then upon moving, do your joints feel better or do they feel worse?" "Doc, actually, to tell you the truth, I mean, it just… When I start moving, it starts…they start feeling a lot better. So I like to move." Osteoarthritis doesn't do that. 02:07 Osteoarthritis, OA, worsens with use. Is that clear? It's wear and tear. And the more wear, the more tear. 02:15 Clinically, remind me the joints again? Reach out your hand, and you're going to give me your DIP. 02:22 When the DIP has undergone inflammatory or osteoarthritis, then it's called Heberden nodes. 02:29 HEB. 02:32 The one that will be proximal, go in alphabetical order. H will be distal, B will be your PIP. Those are called Bouchard, okay, at your PIP. 02:42 And then which finger did I have you put up? Not the middle finger, the thumb, yeah. 02:48 The thumb. That's called your carpometacarpal phalangeal joint. 02:51 That will be affected commonly in osteoarthritis. 02:55 Frequently, as I told you also, apart from that, the knees, the spine, the areas in which you'd expect dependency. 03:01 Now, there's a little bit of an exception. 03:06 Think about the metacarpophalangeal joint. 03:08 What are those? At times, don't you feel like you just want to punch me with your knuckles? Those knuckles are your metacarpophalangeal joints. 03:17 Notice, that is not affected here. Commonly, it's not. 03:22 The wrist is not commonly affected in osteoarthritis. 03:25 But what if you did have a patient who is an occupation, a welder, what have you, and deals with the hands as an occupation for decades. 03:37 Wear and tear. 03:38 And so, therefore, in that particular instance, in that occupation, whatever it may have been, has come to be known as your Missouri metacarpophalangeal joint. 03:49 Otherwise, osteoarthritis normally will not affect those joints. Keep that in mind. 03:55 And crepitus of affected, so a little bit of, let's say, noise. 04:00 In osteoarthritis, you'll notice here that the DIP is affected. What is that called again, please? Heberden. 04:07 What is it called if the PIP is affected? Good. The Bouchard. 04:11 Are your metacarpophalangeal joint commonly affected? Yes or no? No. Good. 04:18 Wrist commonly affected? No. 04:22 Could it be affected? Yes. 04:24 What's your patient doing? Occupation? Dealing with hands and wear and tear over a long period of time. 04:33 And then what about the thumb? Yes. 04:36 At what joint? Carpometacarpal joint, CMC. 04:41 Welcome to osteoarthritis. 04:45 On your examination, on X-ray, what are you going to find? Well, immediately, you'll notice the picture on the left of an X-ray of the knee. 04:56 And you'll notice that the joint space has indeed narrowed. 05:00 That's what happens with all that wear and tear taking place. 05:03 In addition, you might find areas that are a little bit… You see that? A little bit more opaqueness taking place? That area of being more bright white? The bright white area that you're seeing there, the bone is undergoing changes. 05:16 It's sclerotic changes. 05:18 And with that sclerosis, you might even find what's known as osteophytes, or bone spurs. 05:24 For example, you ride a horse with those boots, got the spurs sticking out of your boots. 05:30 Well, these are the spurs that are sticking out of a knee…of a bone called osteophytes. 05:34 That's your fun in osteoarthritis. 05:37 And what about the cartilage that's undergoing ulceration? And what do we call cartilage? Chondral, so subchondral sclerosis, subchondral type of cyst. 05:47 The joint capsule might become inflamed. 05:50 But be careful, though. Remember, the synovial fluid. 05:52 Is it…would you call it truly inflammatory or non-inflammatory? Good. Non inflammatory. Why? Because if you did check the synovial fluid in osteoarthritis, WBC count, < 2000. 06:06 So, by definition, not truly inflammatory. Is that understood? Now, once you have the cartilage which is being ulcerated, now it looks as though the bone is smooth. 06:18 A smooth bone is then called eburnation. 06:21 That's what we're seeing here on X-ray. 06:26 On labs, the sedimentation rate will be normal. 06:30 That's important. 06:32 Rheumatoid factor has nothing to do with rheumatoid arthritis, so it's not immune, remember? So, it's therefore, non-immune. 06:40 The X-ray, I showed you, subchondral sclerosis. 06:43 What does sclerosis mean? Thickening. 06:46 And with that thickening, what may then happen? Give formation to osteophytes, which are known as your bone spurs. 06:53 These osteophytes, if they're in the PIP, you would call them Bouchard. 06:58 If they're affecting the DIP you call them what? Heberden. Good. 07:02 What about management? NSAIDs, definitely a COX inhibitor. 07:06 Commonly, as I told you, obesity. 07:09 So, conservatively, tell your patient to exercise, physical therapy and such. 07:15 Worst-case scenario, maybe the knee is so far gone that surgery is recommended. 07:20 And there's really no role here for PO steroids. 07:24 Intraarticular, you could then inject, maybe, glucocorticoids, though. Keep that in mind. 07:29 Or perhaps, hyaluronic acid. Remember? The synovial lining, it's producing synovial fluid that's made up of hyaluronic type of fluid, isn't it?
About the Lecture
The lecture Osteoarthritis (OA): Pathogenesis by Carlo Raj, MD is from the course Introduction and Non-Autoimmune Arthritis. It contains the following chapters:
- The Pathogenesis of Osteoarthritis
- Examination and Treatment of Osteoarthritis
Included Quiz Questions
Which of the following is NOT a risk factor for the development of osteoarthritis?
- Diabetes
- Obesity
- Increasing age
- Joint overuse
- Joint injury or past trauma
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
2 customer reviews without text
2 user review without text