Playlist
Show Playlist
Hide Playlist
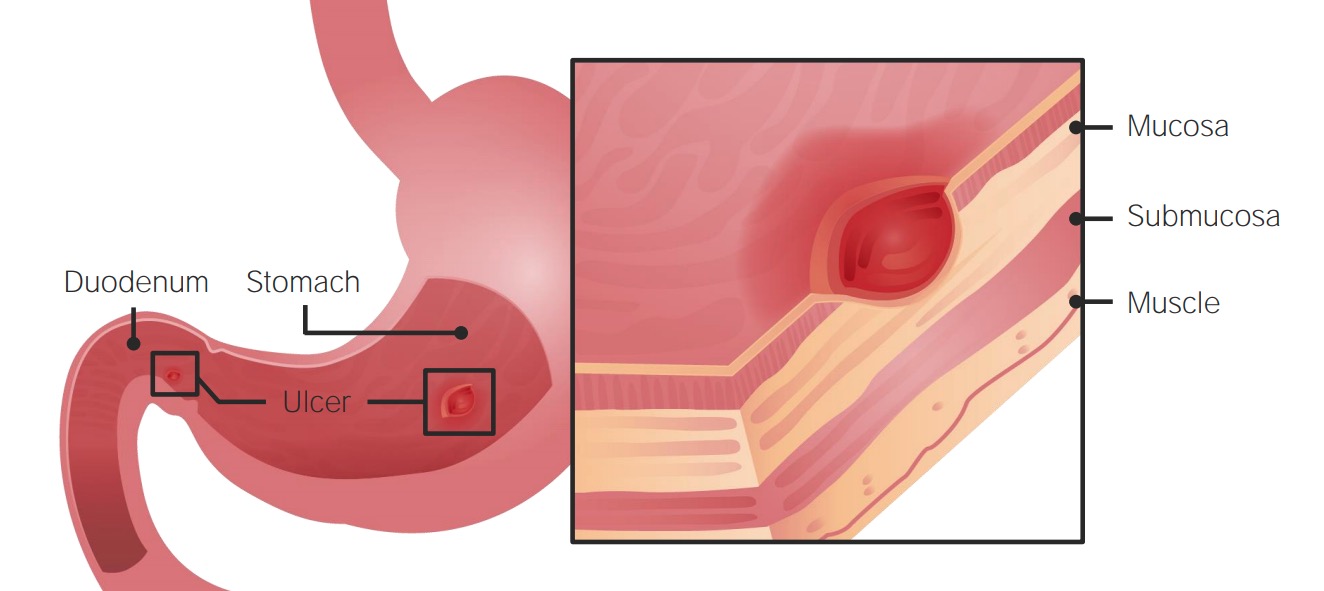
NSAIDs Induced Peptic Ulcer Disease
-
Slides Stomach and Duodenum.pdf
-
Download Lecture Overview
00:00 NSAID Associated Peptic Ulcer Disease. Your patient taking, let’s say NSAIDs for osteoarthritis or in general, just inflammation of the joints. Have been taking this over decades. 00:17 And with NSAIDs as we mentioned earlier, if the prostaglandins are then lost within the stomach, the lining of the stomach in fact now becomes vulnerable to the acid abuse and so therefore may bring about erosion of the lining resulting in peptic ulcer disease of the stomach. The first case that you’re going to find with peptic ulcer disease of the stomach but long term use, you consider this to be acute. 00:43 And it’s not like you take one aspirin or you take one ibuprofen and then all of a sudden the patient develops peptic ulcer disease. That makes no sense. You have to be taking these drugs over a long period of time. Also keep in mind, though, if NSAIDs are being taken over long period of time that in the kidney, with prostaglandins responsible for keeping the afferent arteriole open. 01:10 If NSAIDs are taken, you take out the prostaglandin, you’re at risk of vasoconstricting the afferent and over a long period of time, here as well, you’re worried about chronic kidney injury. 01:23 Is that clear? Two major organ systems that are extremely vulnerable to attack with NSAID use. 01:30 And really because of the easy accessibility of these drugs by the patient over the counter, you have to properly educate your patient because they’re going to be popping pills all of the time whenever they feel pain. And I’m talking popping pills excessively for long period of time. And they may or may not even tell you. Right? Increased risk of bleeding with low dose and high dose aspirin. 01:55 Further increased risk of dose dependencies which you’re worried about. Exactly what I was saying, the patients are in pain, they might be taking aspirin and they might be increasing the dosage without you ever knowing. It is important that you establish in your practice, excellent rapport with your patients. 02:15 So that they're being transparent between you and your patient. Enteric coating does not reduce the risk of bleeding. Do not allow the advertisements and the commercials to fool you. High rate of mortality for NSAID associated with GI bleeding. 02:35 Who is your patient with NSAID associated peptic ulcer disease. More than 70, higher dose of NSAIDs, often associated with H. pylori, and concomitant corticosteroids. Remember please, with NSAIDs, they might very well be in pain and if they are, they’re probably taking prednisone as well. 02:58 My goodness. A combination of NSAIDs and corticosteroids definitely compromises the production of your prostaglandin. Therefore increases the risk of peptic ulcer disease further. Also, anticoagulants. 03:13 Prior history of peptic ulcer disease. 03:16 NSAIDs what does it do? Inhibits your prostaglandin. Management. PPI and remove the NSAIDs. 03:24 At some point in time if peptic ulcer disease has kicked in, remove the offending agent. 03:30 Educate your patient properly and PPIs. Always treat your H. pylori. Highly indicated gastric or duodenum. 03:39 H. pylori, for the most part, you assume is present. 03:45 Prophylaxis. Misoprostol, a prostaglandin. It’s a prostaglandin E derivative and combats the effects of NSAIDs. Diarrhea is a dose limiting side effect however. And absolutely contraindicated in pregnancy. 04:06 Prophylaxis. PPI. Superior to H2 blockers we’ve talked about when it comes to acid control. 04:14 COX−2 inhibitors might be a possible alternative. Lacks cardiovascular protective effect. 04:22 And GI protective effect lost with concomitant baby aspirin use. So COX−2 inhibitors, you've heard of celecoxib, so on and so forth. Might be alternatives that you’re looking for when dealing with NSAID associated peptic ulcer disease.
About the Lecture
The lecture NSAIDs Induced Peptic Ulcer Disease by Carlo Raj, MD is from the course Stomach and Duodenum Diseases: Basic Principles with Carlo Raj.
Included Quiz Questions
What is the percentage of risk of a GI bleed seen in patients using long-term NSAIDs?
- 1.3%
- 1.6%
- 1.7%
- 1.9%
- 2.3%
How do NSAIDS that are used adversely affect the kidneys?
- By vasoconstriction
- By increased capillary permeability
- By vasodilation
- By lowering blood pressure
- By thinning of the blood
Which drug used in conjunction with NSAIDs can lead to an increase in NSAID-related peptic ulcers?
- Prednisone
- Thyroxine
- Codeine
- Morphine
- Lidocaine
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
such a good lecuture. Covers the topic in a broad sense. good clinical value.