Playlist
Show Playlist
Hide Playlist
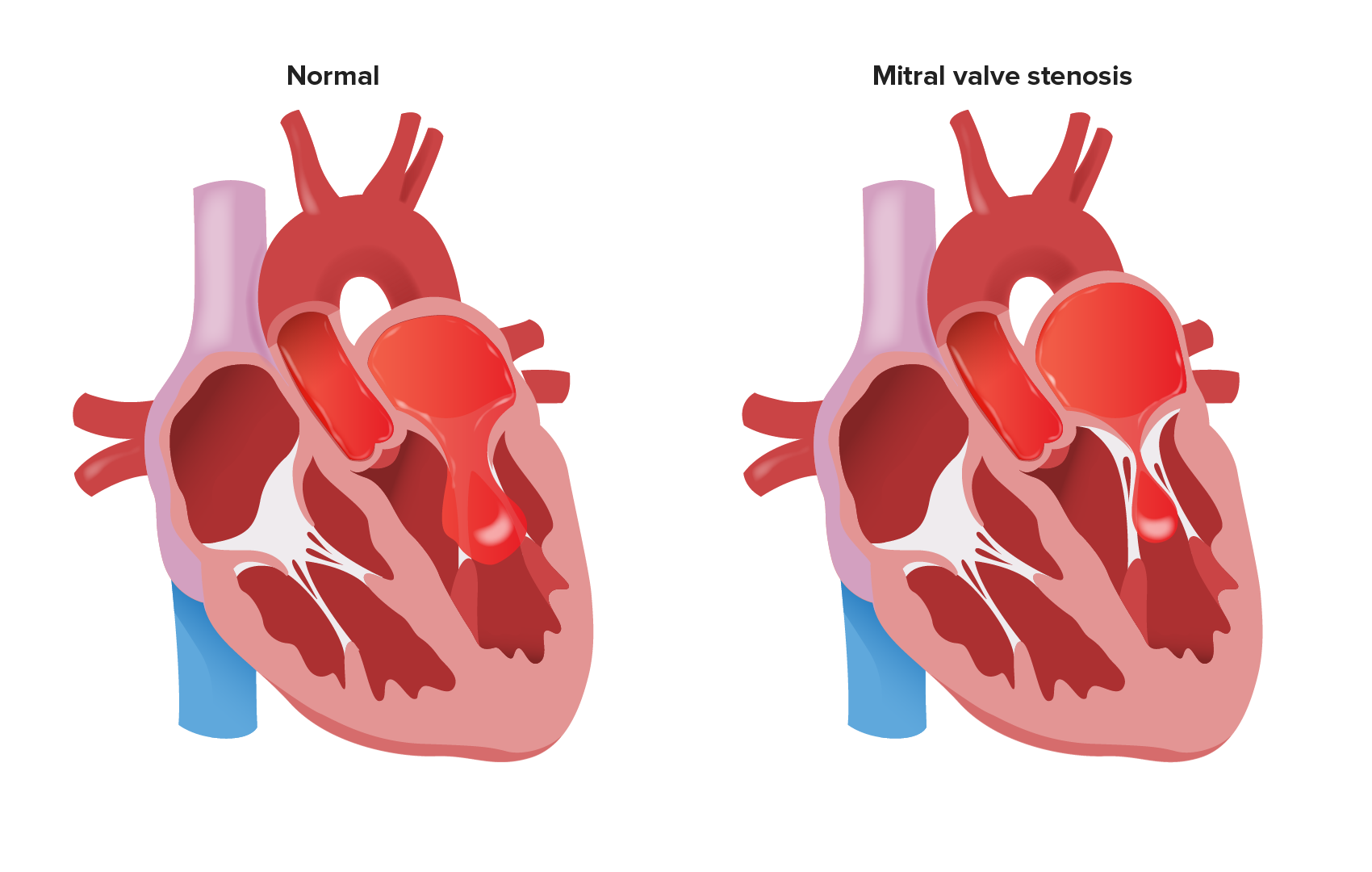
Mitral Stenosis: Signs and Symptoms
-
Slides ValvularHeart DiseaseMitralStenosis CardiovascularPathology.pdf
-
Download Lecture Overview
00:01 Mitral stenosis, progressive dyspnea on exertion, nonspecific for any valvular heart disease. 00:05 Hemotypsis, why? Why we are seeing this more so than any other valvular heart disease? It is the fact that the left atrium is not emptying. It back up to your pulmonary veins hence resulting in. Could you have increased RBCs in your lungs and such? Sure. Coughing up of blood, that is not good. Heart failure, late finding, once again a bad prognosis. It means what? Well the opening snap, we talked about how it will be after S2 called it as mid-diastolic murmur. The closer that your opening snap is to S2, the worse is the prognosis. Tell me the size of your left ventricle. Very very tiny. Eventually, what is going to happen? It become the pulmonary edema? Sure. We will talk about that increased hydrostatic pressure. Right? Then you have what? It may transmit this disease into the right ventricle. Might have right ventricular failure. Is this, very important question pay attention, is this cor pulmonale? Nope. "But Dr. Raj, right ventricular failure secondary to left-sided heart failure?" Yes. That is not cor pulmonale? No. So what is cor pulmonale? It is right ventricular failure secondary to a primary pulmonary disease such as maybe pneumonia, maybe pulmonary fibrosis so on and so forth. But when you have right ventricular failure here due to left-sided heart failure, that's not cor pulmonale. But if you do find it, mitral stenosis, not a good prognosis. Physical examination. Palpation, right ventricular heave. What does that mean? It means pulmonary hypertension. What about the PMI? Pay attention here. What is PMI? Point of maximal impulse. So I don't know that means. Ya you do. PMI is the apex of the heart and where is the apex? What chamber is that when you refer to the apex? Left ventricle. 01:54 What is the size of your left ventricle? Either normal or maybe decreased. It is never cardiomegaly. 02:01 It makes no sense. The left ventricle is not going to go laterally displaced. Is that clear? Every single statement that we have here has huge clinical relevance. 02:11 I have information that goes outside of the apparent slide and such, but it is only so that we have a complete story, so that we have more differentials, so that we integrate more material. 02:21 All this information at some point in time, is touched, will be touched, and forever will be part of your understanding. Mid-diastolic murmur is what we talked about occurs during diastole. Heard loudest well, we talked about this where, when it comes to mitral issues. 02:37 Where am I? Where are you upon cardiac auscultation? No issues between S1, S2. 02:48 So that will be wholly systolic. It is after S2, you have an opening snap and then you have it. It is after S2. It is after that "dadup". You are going to hear an opening snap, where you can hear this? Auscultation, fifth intercostal space, midclavicucular, apex is where you are. What kind of murmur? A mid-diastolic murmur. Afib is something that you want to worry about. What does afib mean to you? It means that you are going to mess up your conduction system. And with atrial fibrillation what might you be looking for? What wave? Are you paying attention? You tell me. Atria. If you say QRS complex, I will find a way to come there and slap you. No. But the P wave is what you are paying attention to, atria. What is the wrong with those P waves? They are not present, are they wavy? Not saw-tooth. That's atrial flutter. That is another discussion for another day.
About the Lecture
The lecture Mitral Stenosis: Signs and Symptoms by Carlo Raj, MD is from the course Valvular Heart Disease: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following explains the etiology of hoarseness in a patient with mitral stenosis?
- Compression of the left recurrent laryngeal nerve
- Increased hydrostatic pressure in the pulmonary veins
- Compression of the vagus nerve
- Compression of the right recurrent laryngeal nerve
- Pulmonary edema
Which of the following describes the murmur of mitral stenosis?
- Opening snap followed by a mid-diastolic rumble.
- Mid-systolic click with a mid-diastolic rumble
- Systolic crescendo-decrescendo murmur
- Early diastolic decrescendo murmur
- High-pitched holosystolic murmur
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
I like how he keeps me engaged and constantly asks me questions to keep me on my toes. I appreciate his jokes too because it makes studying a little bit more fun