Playlist
Show Playlist
Hide Playlist
Neuroepithelial Tumors: Medulloblastoma
-
Slides 08 Tumors of the CNS Neuropathology II.pdf
-
Download Lecture Overview
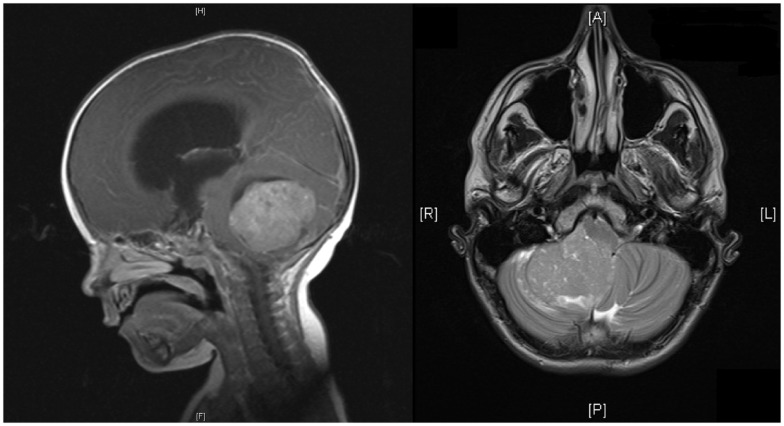
00:00 Here we'll take a look at a neuroepithelial tumor. This is called medulloblastoma. 00:06 Right off the bat and let me tell you medulloblastoma will be the most common primary CNS tumor in a child. Now with that said, let's take a look at what it's referring to. Sometimes you've seen their abbreviation when you're reading a journal, whatever. BMJ, Lancet, NEJM, what have you. And you might see their abbreviation PNET. In fact, you have or you will. It stands for primitive neuroectodermal tumor, PNET. You see it? Here, we want to think of this as being embryonal neoplasm. 00:47 Embryonal, I just began this discussion by calling this a primary CNS tumor in a child, the median age 7. 70% presented patients under age 20 and they make up 10% of all brain tumors in patients under the age of 19. Located where? Yet another one right in that area in the vicinity of the 4th ventricle in the cerebellum, right in that vicinity. So give me 3 right now in a child, they would be in that region, 3. Most common astrocytoma in a child, pilocytic. What about an ependymoma, could be located in the floor of the 4th ventricle. And here we have a medulloblastoma. 01:30 Where is it located? The midline of the cerebellum. All of these could cause what, obstructive non-communicating type of hydrocephalus. Clear. So as you can see here, there is a decent listed differentials causing non-communicating, rapid growth, rapid growth. May occlude flow of outflows of CSF resulting in hydrocephalus as we mentioned. Now, the small blue cells, see if you want from now on, medulloblastoma. 01:58 B blastoma, small blue cells is the histologic description. May then go in to the CSF. 02:08 Keep that in mind. If you take a look at this imaging study, you'll notice. Where are we? You see that structure where we have the cerebellum and you find that increased opacity which then represents a tumor. It looks like it's in the midline of this child's image of the brain and therefore you can notice that now as it moves anteriorly here that is then going to cause obstruction of the outflow of your CSF from the 4th ventricle most likely. This is medulloblastoma. A couple of things that I wish to bring to your attention under medulloblastoma, you want to know this in great detail because it is a primary CNS tumor in a child. Well-circumscribed gray and friable, microscopically sheaths of anaplastic cells. Take a look at these small cells with little cytoplasm and hyperchromatic nuclei that are elongated or crescent shaped and by hyperchromatic nuclei we are referring to this of being, take a look at these sheaths of small blue cells, medulloblastoma. Clinical presentation is important. 03:20 Increased intracranial pressure as you can imagine. Ataxia because we're referring to the cerebellum being affected. Clinical features, we have highly malignant tumor, highly malignant. Unfortunately may disseminate into the CSF. A common complication because of its increased aggressiveness. We call this drop metastasis. 03:40 Met stands for metastasis. Poor prognosis unfortunately in a child and that just makes me sad and it's radiosensitive but poor prognosis. Please make sure that you know medulloblastoma in great detail.
About the Lecture
The lecture Neuroepithelial Tumors: Medulloblastoma by Carlo Raj, MD is from the course Tumors of the CNS.
Included Quiz Questions
Which of the following is the most common malignant CNS tumor in a child?
- Medulloblastoma
- Oligodendroglioma
- Pilocytic astrocytoma
- Ependymoma
- Pleomorphic xanthoastrocytoma
What is the median age of presentation of a medulloblastoma?
- 7 years
- 17 years
- 8 years
- 6 years
- Lymphoma
Which of the following is true about medulloblastomas?
- They disseminate into the CSF via drop metastasis.
- They cause a decrease in intracranial pressure.
- They have a good prognosis.
- They are not radiosensitive.
- They cause a communicating type of hydrocephalus.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |