Playlist
Show Playlist
Hide Playlist
Large Intestines: Diverticulitis
-
Slides Diverticulitis General Surgery.pdf
-
Download Lecture Overview
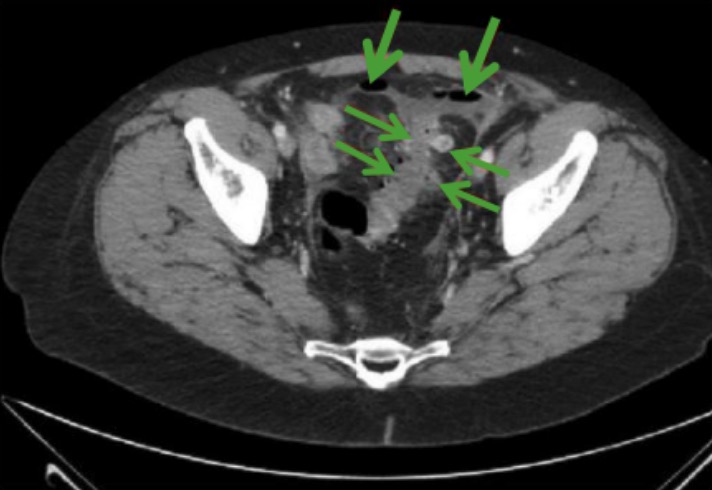
00:01 Welcome back. 00:02 Thank you for joining me on this discussion of diverticulitis in the section of general surgery. 00:10 Diverticulosis is a very common disease. 00:13 It's anatomically a herniation of mucosa to the wall of the colon via areas of inherent weakness called the VASA RECTA. 00:21 Where the vessels are coming into the intestines. 00:26 It can lead to secondary infection and microperforation, which is then diagnosed as diverticulitis. 00:33 Itis meaning inflammation of the osis. 00:35 So diverticulosis, can progress to diverticulitis It's typically associated with a low fiber, constipation and obesity. 00:47 There appears statistically left column and predominance, we think largely due to a high intraluminal pressures as a result of the solid stools heading to the left side of the colon. 01:00 What are some physical findings of diverticulosis? What's interesting because diverticulosis unlike diverticulitis may be very much asymptomatic. 01:08 One of the classic presentations of diverticulosis however, is bleeding. 01:14 Bleeding is not necessarily a for certain finding and diverticulosis, but when you have lower GI bleeding, one of the things to keep on the top of your differential diagnosis is diverticulosis. 01:29 When diverticulosis gets infected secondarily and leads to microperforation, we then have a situation of diverticulitis like we previously mentioned. 01:38 Well, what are some of the classic findings of diverticulitis once the diverticulosis has either been secondarily infected or progressed to microperforation? Well, typically, the patient presents with some form of abdominal pain, whether this be in a left lower quadrant of the abdomen, if it's likely due to a sigmoid diverticulitis. 01:56 In the superpubic region where sometimes patients often report the sensation of incomplete voiding. 02:03 Remember that the sigmoid colon is very floppy. 02:06 It can either be on the right side of the abdomen or the on the left side of the abdomen. 02:09 So right side or lower quadrant abdominal pain can also be either due to right side or diverticulitis or because you have a floppy sigmoid colon. 02:18 The classically it's been described as left lower quadrant abdominal pain. 02:23 This pain can become generalized with perforation. 02:26 Although by definition, diverticulitis is a microperforation. 02:30 The perforation where we're talking about generalized peritonitis is usually associated with a large perforation. 02:38 Oftentimes, patients also present with diarrhea. 02:40 This is likely local inflammatory response. 02:46 What laboratory findings were you thought? Well, you know, routine chemistry, maybe everything's pretty much normal. 02:52 On a CBC, you may see increased white blood cell count or leukocytosis. 02:57 Again, no specific lab finding is absolutely indicative of diverticulitis. 03:03 An index of suspicion is very important. 03:08 Here you'll see a CT abdomen pelvis, the green arrow points to a collection. 03:13 Notice that around the collection, it's a ring enhancing collection with both fluid and air level. 03:19 This is consistent with a pericolonic abscess. 03:24 You'll also notice that if you follow the sigmoid colon, you'll notice little pockets of air along the lining of the colon indicative of diverticulitis and microperforation specifically. 03:36 We have a standard classification for describing diverticulitis based on radiographic findings. 03:42 It's called the Hinchey classification. 03:44 Let's familiarize you with Hinchey classification. 03:47 Hinchey classification I is a phlegmon or pericolic abscess. 03:52 If a walled-off abscess develops in the abdomen or the pelvis, it becomes a Hinchey classification II. 03:59 This is very similar to the CAT scan that you just saw. 04:02 Hinchey classification III is generalized purulent peritonitis, And IV is fecal contamination.
About the Lecture
The lecture Large Intestines: Diverticulitis by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
Which one of the following statements about diverticular disease is FALSE?
- Diverticulitis is always asymptomatic.
- Diverticulitis is inflammation and infection of diverticula.
- Constipation is a risk factor for diverticulosis.
- Diverticulosis is predominantly located in the left colon.
- Diverticulitis can lead to micro-perforations.
Which of the following is a risk factor of diverticulosis?
- Low fiber diet
- Diarrhea
- Anorexia
- High fiber diet
- Regular, frequent bowel movements
A 55-year-old male with a history of diverticulosis and recurrent bouts of diverticulitis presents to the emergency room with a one-day history of fever and chills. Physical exam is significant for generalized abdominal pain and tenderness, peritoneal signs, and vitals show hemodynamic instability. Which one of the following is likely to be the cause of his symptoms?
- Colonic perforation
- Microperforation of the colon
- Enteritis
- Recurrent diverticulitis
- Small bowel obstruction
Which one of the following definitions of the various Hinchey classifications is INCORRECT?
- Class 3 --- Diverticulitis with pericolic abscess
- Class 1 --- Diverticulitis with phlegmon formation
- Class 2 --- Diverticulitis with walled-off pelvic abscess
- Class 3 --- Diverticulitis with generalized purulent peritonitis
- Class 4 --- Diverticulitis with generalized fecal peritonitis (fecal contamination)
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |