Playlist
Show Playlist
Hide Playlist
Epstein-Barr Virus (EBV) – Herpesviruses
-
Slides Herpesviridae.pdf
-
Download Lecture Overview
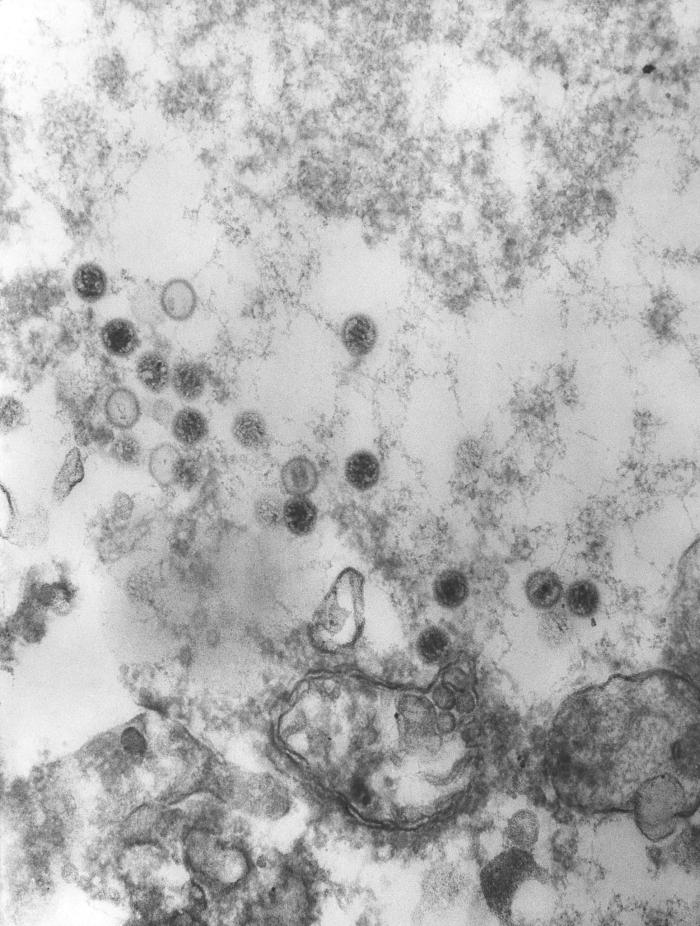
00:01 Okay, moving on to our fourth herpes virus, Epstein-Barr virus, EBV. 00:08 This is transmitted in multiple ways. 00:10 Through direct contact with saliva, through aerosolization of respiratory droplets, close contact with anything. 00:18 Also via transfusions, if a blood donor was actively infected with Epstein-Barr virus, certainly the same thing with a solid organ transplant. 00:27 There can be congenital transmission, and pretty much any body fluid. 00:33 Why? Because Epstein-Barr virus targets B lymphocytes, which you see on the image in front of you. 00:39 All those are lymphocytes, not necessarily actively infected with Epstein-Barr virus, but they at least are the proper target. 00:46 You may hear infectious mononucleosis caused by EBV, named the "kissing disease." It kind of says it all. 00:55 So, pathogenesis. 00:57 Epstein-Barr virus targets its B lymphocyte starting in the oropharynx, again, because many of these exposures will occur through the oral mucosa mechanism. 01:06 And from the oropharynx, then you get progression to and through saliva into lymphoid tissue, typically starting in the tonsils, in the pharynx. 01:17 And that's important because, as we'll see, one of the clinical symptoms with infectious mononucleosis is a pharyngitis, a sore throat. 01:25 Then we have production -- the Epstein-Barr virus is achieving latency in those lymphocytes, we have production of immunoglobulin M heterophile antibodies. 01:36 eterophile, meaning multiple forms, is because the lymphocytes are confused. 01:42 B lymphocytes produce immunoglobulin M and progressing to immunoglobulin G. 01:48 The immunoglobulin M is supposed to be specific to the infecting organism, but because these cells are being disrupted by EBV pathology, they're producing immunoglobulin M antibodies which may target anything and everything. 02:02 They're polyclonal. 02:04 But they can be detected by a test, as we'll see very shortly. 02:09 Latency. 02:10 As the Epstein-Barr virus achieves its latency, its quietness in the B lymphocytes, it persists there for life, which unfortunately means that those B cells can undergo increased turn over, increase mitoses And any proliferation, especially of a red blood cell or, in this case, a white blood cell can cause a neoplastic diseases. 02:33 So Epstein-Barr virus, infectious mononucleosis, also highly associated with malignancies. 02:40 So, let's look at our 2 most common diseases side by side. 02:44 Mononucleosis compared to hairy oral leukoplakia. 02:48 Patients at risk for mononucleosis, classically, are teenagers, and also young adults, but anybody and everybody can be infected with Epstein-Barr virus at any age. 02:59 In fact, by young adulthood, most say, 25, 26 years of age, 60% of us have been infected with Epstein-Barr virus, but we may not know it because it can cause a completely asymptomatic diseases. 03:14 So, teens and young adults, though, are the classic targets for Epstein-Barr mononucleosis. 03:19 The incubation period is up to 2 months. 03:22 This is again, it's a very slow process, which is great for the incubation to take that long, but not so great because the disease lasts similarly, very long. 03:31 Hairy oral leukoplakia is a problem for those patients who are immunosuppressed and classically those patients with HIV/AIDS because they've lost their suppressor function with the T lymphocyte, the CD4 T lymphocyte, and thus, those proliferating B lymphocytes can get out of control and cause many things, including the leukoplakia. 03:54 Clinical manifestations for infectious mononucleosis. 03:57 lassically, we have the exudative pharyngitis. It looks, smells, and feels, for all of the world, like streptococcal pharyngitis, but the testing for group A strep is negative. 04:09 The other parts of the infectious mononucleosis triad are pronounced cervical or, in fact, posterior cervical lymphadenopathy, so toward the back of the neck. 04:20 These patients come in with what's called a bowl neck, a thick neck which looks like the neck of a bowl. 04:26 And that, along with sore throat or pharyngitis and palpable splenomegaly, is screaming the diagnosis infectious mononucleosis. 04:35 It makes sense because Epstein-Barr virus targets B lymphocytes, and where do they live? The lymph nodes, the spleen, nd they came in through the tonsils in the back of the throat. 04:48 Patients with this triad all have extreme fatigue. 04:51 And anybody who has suffered from this, you have my deepest sympathies. 04:55 It may take days to weeks to months to get out of bed. 04:58 We're talking completely flattened. 05:00 Along with that fever, headache, if the patients receive ampicillin or amoxicillin, classically, they'll develop discrete erythematous papular rash. 05:11 In fact, that used to be the way that we diagnose Epstein-Barr virus prior to having our serologic testing. 05:18 We just gave them some amoxicillin and see if a rash developed. 05:21 There was an 80% attack rate with giving ampicillin or amoxicillin to a patient with Epstein-Barr virus to elicit that rash. 05:29 As I mentioned before, asymptomatic infections are very common. 05:34 In fact, and luckily, about 80% of Epstein-Barr virus infections are completely asymptomatic. 05:41 Looking now at the clinical parts for the hairy oral leukoplakia, these are lesions most often seen on the tongue, sometimes toward the back of the tongue, which are white. 05:52 They start off looking like thrush, the lesions caused by Candida albicans, a yeast in the mouth. 06:00 But, they rapidly go from white to sort of grayish, just sometimes even black, and they're fixed. 06:05 They don't scrape off. 06:08 So, clearly, seeing that kind of a lesion in the mouth of a patient who is immunocompromised, for whatever reason, should raise suspicions, both of an opportunistic yeast infection, but also of an Epstein-Barr virus leukoplakia. 06:23 Diagnosis. 06:24 So the diagnosis of Epstein-Barr virus infection, regardless of what it is causing, can be accomplished in several different ways. 06:32 The first is by blood smear with an astute hematopathologist. 06:36 The lymphocytes, the B lymphocytes of a patient with Epstein-Barr virus infection can look very atypical or reactive. 06:44 And so the hematopathologist or the lab may call you and say, "I'm seeing a whole bunch of reactive lymphocytes on the blood smear." These reactive lymphocytes are also called Downey cells, and you can see an image of one of those on the lower right. 06:59 The next test is the monospot test and this detects those heterophile, immunoglobulin M antibodies that we were talking about from early stages of Epstein-Barr virus infection, those disordered B lymphocytes producing anything they can. 07:15 And then, we have specific immunoglobulin M and G tests for Epstein-Barr virus antigens, and these can be from the cell wall, from the nuclear antigen, or early antigens themselves. 07:28 And based on the serologic pattern, one can tell at what stage the patient is infected: early, middle, or latent.
About the Lecture
The lecture Epstein-Barr Virus (EBV) – Herpesviruses by Sean Elliott, MD is from the course Viruses.
Included Quiz Questions
Which of the numerically labeled members of the Herpesviridae family correctly corresponds with the Epstein-Barr virus?
- Human herpesvirus 4
- Human herpesvirus 3
- Human herpesvirus 5
- Human herpesvirus 6
- Human herpesvirus 8
The Epstein-Barr virus primarily infects and achieves latency in which of the following?
- B lymphocytes
- T lymphocytes
- Neutrophils
- Eosinophils
- Basophils
Which of the following antibiotics is typically associated with induction of a hypersensitivity rash in a patient with infectious mononucleosis?
- Ampicillin
- Ciprofloxacin
- Cefixime
- Azithromycin
- Doxycycline
Downey cells appreciated on the blood smear of a patient suffering from Epstein-Barr virus-induced infectious mononucleosis are best described by which of the following?
- Atypical lymphocytes
- Atypical basophils
- Atypical macrophages
- Atypical neutrophils
- Atypical eosinophils
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |