Playlist
Show Playlist
Hide Playlist
Cutaneous Fungal Infections
-
03-57 Microsporidia.pdf
-
Download Lecture Overview
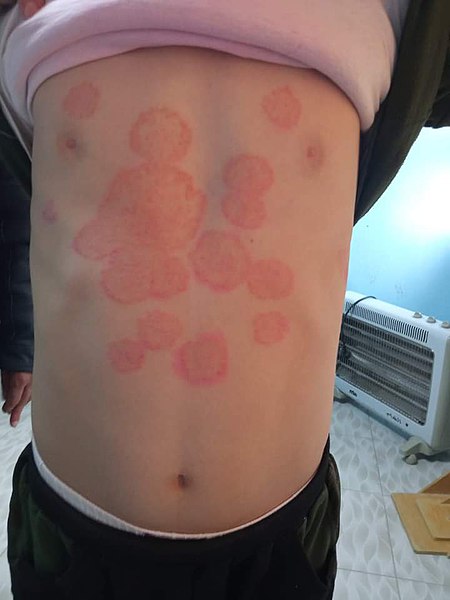
00:00 Dermatophyte infections are fungal infections of the skin, hair, and nails, which are caused by spore-forming, single-cell, filamentous fungi. 00:08 The three main genera are: Trichophyton, Microsporum, and Epidermophyton. 00:13 They metabolize and survive upon keratin. 00:16 These infections also have general names including Tinea, Dermatophytoses, Ringworm, and Cutaneous mycoses, as well as site specific names, which we will describe later. 00:27 Other fungal infections of the skin include: Yeast such as Candida, and nondermatophyte molds such as Fusarium, and Aspergillus. 00:36 They cause what we call cutaneous mycoses, which again is a reference to the fungal appearance of mycotic infection. 00:45 But in fact, the common name for this is ringworm or to the dermatologist these are dermatophytoses. 00:53 So, let us look as you can see, with a classic picture on the right side of the slide at what a ringworm does a raised red spot with some scaly nature on top of it. 01:05 Transmission of these organisms is unfortunately quite common because they are ubiquitous, they live everywhere. 01:13 So all of us, at any point in time, at many parts of our body are colonized with these organisms. 01:20 Fortunately, infection only occurs when there is a disruption of our normal defenses. 01:26 What is our most common normal defense? Our skin. 01:29 And so any breaks in the skin whether they're microscopic or even more significant, such as an abrasion or a laceration will allow for these infections to gain entry, even to the slight superficial component of the skin and begin to start their action. 01:46 The incubation period is unknown, because we don't exactly know when to start the clock from ticking that these organisms, all of them are on the skin at any point in time. 01:56 So just imagine that it takes simply a break in skin of some sort, and then at some point in time, a cutaneous mycoses will develop. 02:17 The target for these the pathogenesis it really has to do with the fact that these organisms especially are focusing on getting access to keratin. 02:26 They actually process keratin. 02:28 So, they will start at the very surface on top of the stratum corneum. 02:33 And then once they're given access to deeper layers of the epidermis to get access to the keratin containing layers of that epidermis. 02:42 So side of the inoculation will be somewhere on somebody's stratum corneum and then they'll invade deeper to pursue the keratin. 02:51 The organisms all produce keratinase, an enzyme which will break down keratin, and that allows them to feast if you will on the keratin as their nutritional source. 03:02 Interestingly, when it's time for the organisms to replicate, they will actually be able to place fungal spores from the cells, typically onto hair shaft forming an ecotothrix, which is in a way for those of you who study or have seen lice, where the eggs of the lice will also bind to that bottom of the hair shaft. 03:22 So to with these organisms, their fungal spores will be attached to the exterior of the hair shaft. 03:29 So diagnosis. 03:30 Well, if a clinical picture is not worth a thousand words, then we have the ability to look even more specifically with a Wood's lamp: a bright fluorescent light, which when shown on an active mycotic lesion due to these organisms will shine white. 03:47 Now, the picture you see in front of you is a Wood's lamp brightening picture of the ear and sort of posterior neck of a patient. 03:57 On top of the picture is the hair, which normally luminousness. 04:00 But if you look at the ear lobe, the pinna itself as well as parts of the neck, you'll see multiple areas of these white luminescent areas. 04:10 Those would all be areas of cutaneous infection with these organisms. 04:15 In addition, so the picture being worth a thousand words is great, but of course we like proof. 04:21 So one can scrape these lesions gently with the razor blade onto a glass slide and then put a drop of potassium hydroxide. 04:30 One will then be able to see the branching septate hyphae and one could also do a blue fungal stain to further identify them. 04:39 So let's now look at the different types of clinical diseases related to the different type of these organisms which are commonly called tinea. 04:47 The first one is Tinea capitis. 04:50 Capitis for head, and as you would expect, this causes skin lesions on the head and the scalp. 04:57 The picture to the right side of the slide shows you that classic appearance with significant secondary alopecia. 05:04 You can see bare areas or bare patches on this patient's scalp. 05:09 And in those bare areas, you can see scaly lesions that will be a classic tinea capitis. 05:15 Now, as an interesting side note, patients with tinea capitis will frequently also present with a kerion, K-E-R-I-O-N Kerion is going to be an extremely swollen nodule underneath that site of the tinea capitis infection, and it represents a sterile id reaction. 05:37 A sterile hypersensitivity immunologic reaction to antigens expressed by the tinea capitis. 05:43 And those patients with tinea capitis and a kerion will frequently also have very enlarged occipital lymph nodes. 05:52 So, those three all go together. 05:54 You can make a clinical diagnosis in a heartbeat just by visualizing such a patient. 06:00 Next, tinea corporis. 06:02 Corporis or corpus for body. 06:04 These lesions are found anywhere in the body, most often on the extremities but sometimes on the trunk, the back, the buttocks, etc. 06:13 The tinea corporis lesions are slightly more erythematous and you will see with the other tinea that we're talking about, and they're slightly less circumscribed. 06:23 The appearance on this picture is of a somewhat serpiginous bordered lesion, which is so scaly but which also has various discrete erythematous papules raised upon its surface. 06:35 Regardless, there will be areas of some central clearing such as you also see expressed on this picture. 06:43 Tinea cruris commonly called jock itch. 06:46 Now, not just in the inguinal, or peritoneal regions but also in the axilla areas where one typically sees secondary sexual characteristics with pubic hair is where this tinea loves to hang out, pardon <inaudible>. 07:01 Tinea cruris also is going to be slightly erythematous and raised typically though without the central clearing. 07:09 Now, many patients will come to you complaining of a burning, or an irritation in either the antecubital fossa, the axilla, or the perinatal region that the groin and then that complaint along with the clinical appearance should be able to give you the diagnosis. 07:28 Tinea pedis. 07:29 Pedis for feet, but also to be seen on the hands will be typically and most oftenly seen in the interdigital space. 07:38 So in the hands between the fingers right there. 07:41 Some might think, "Oh, it's just skin breakdown because my hands are dry, they're cracked, it's cold outside. 07:48 I've been washing my hands diligently because I'm a good health care provider." But these will... 07:53 in addition to that cracked appearance you have erythema and also that scaly appearance. 08:00 The moccasin distribution, well, that sort of makes sense if you happen to wear moccasins, you know that they're sort of low slung and they typically don't cover the anterior portion of the foot as well. 08:12 Occasionally, and not all the time, but occasionally, tinea pedis lesions also appear to be somewhat vesicular. 08:20 But trust me, they're not herpetic, they're all due to this cutaneous mycotic infection. 08:26 And then finally, Tinea unguium is absolutely to do with the nails of the the fingers and the toes. 08:34 Another name for this would be onychomycosis. 08:37 And there again that mycoses there's that fungally sounding name again, these all behave very much like a slow growing fungal infection would. 08:45 Tinea unguium or onychomycosis can absolutely cause destruction of the nail itself. 08:51 It frequently looks brittle or fragile, very much like this picture shows with the appearance that it could just sort of chip off, and indeed, that's a scaly appearance, but of the toenails. 09:03 Occasionally, these lesions will appear green. 09:06 Other times there appear yellow, gray, bronze, you name it. 09:10 It depends on the subspecies of the tinea causing the disease. 09:15 So the cutaneous mycoses caused by the tinea organisms. 09:20 Location, location, location is probably your best friend and identifying what organisms causing what where? But the diagnosis is still the same. 09:28 Clinical, perhaps a skin scraping, and your good friend the Wood's lamp.
About the Lecture
The lecture Cutaneous Fungal Infections by Sean Elliott, MD is from the course Fungi.
Included Quiz Questions
The cutaneous manifestation known as ringworm is caused by which of the following types of parasites?
- Unicellular fungi
- Flagellates
- Ciliates
- Sarcodines
- Helminths
Which of the following enzymes is most likely to be produced by the unicellular parasites causing cutaneous mycoses?
- Keratinase
- Ribonuclease
- Proteoglycanase
- Elastase
- Collagenase
During infection of the scalp by Microsporidia, which of the following terms best describes the attachment of spores to the hair shaft?
- Ectothrix
- Ectosarc
- Ectoproct
- Ectotroph
- Ectozoan
Which of the following is used for the microscopic evaluation of a specimen obtained from a ringworm lesion?
- Potassium hydroxide
- Gram stain
- Ziehl-Neelsen stain
- Methylene blue
- Wright’s stain
A dermatophytosis involving the skin between the digits of the toes is termed...?
- ...tinea pedis.
- ...tinea capitis.
- ...tinea corporis.
- ...tinea cruris.
- ...tinea unguium.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |