Playlist
Show Playlist
Hide Playlist
Case: 61-year-old Man with Headache
-
Slides CNS Infections Encephalitis.pdf
-
Download Lecture Overview
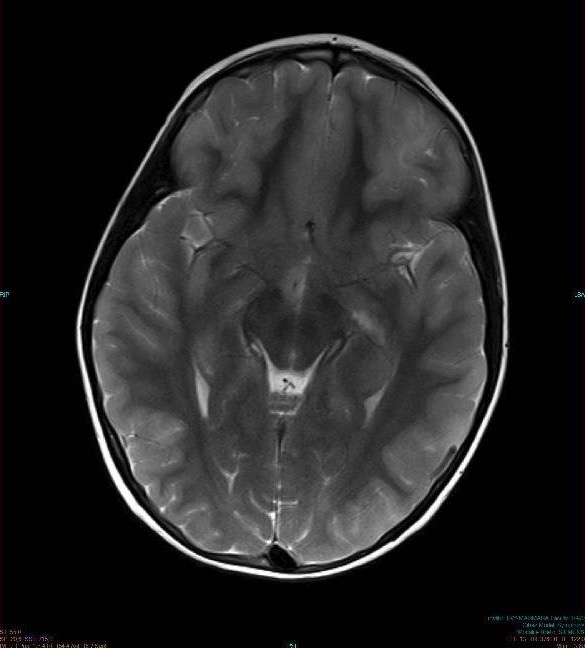
00:00 In this lecture, we're going to talk about encephalitis. So let's start with a case. A 61-year-old man with headache. This 61-year-old man has no past medical history and presents with a several-week history of personality changes and headache. The headache began 2 weeks ago and was mild at first, but has become slightly more severe with the pain that is 7/10 in severity everyday for the past 5 days. So this sounds like a subacute onset condition. His wife reports changes in his personality and he has been sleeping more, some alteration in his sensorium. He now presents abruptly today due to seizure-like activity or episode with left head turn, eye deviation, followed by jerking of the left arm and hand then spreading to the entire hemibody followed by generalized tonic clonic activity. So clearly, he has had a focal onset generalized seizure. He has no neck stiffness or meningismus and no rash. What about his workup? Laboratory assessment reveals normal routine studies except elevated transaminases, increased liver enzymes and normal renal function. And a spinal tap is performed to look for infection and the CSF analysis reveals significantly elevated white blood cells, a prominent pleocytosis 5000 white blood cells. The differential is 97% mononuclear, these are lymphocytes, which points us in the direction of a viral or maybe a fungal process. 01:33 The protein level is slightly elevated, the glucose is 91 and systemic glucose is 140. That's about 65% of the systemic glucose. So that signature points us towards possibly a viral process. So what's the diagnosis? Well, let's walk through some of the key features of the case. First of all, this is a 2-week onset, there's a prodrome with not feeling well and headache and generalized malaise as it sounds and this suggest a viral prodrome of what is likely a viral infectious process. He presents with a seizure, a focal onset seizure that suggest that there is some area of cortical irritation or dysfunction or pathology and specifically this left body or right brain focal onset seizure suggest that we need to look in the right hemisphere. And this is indicative of a possible encephalitis or cerebritis. There's no neck stiffness, no meningismus and so we're not favoring meningitis in favor of an encephalitis or cerebritis. 02:37 And the workup, the spinal tap, reveals a signature that is most suggestive of a viral process. 02:44 How about the imaging? Well here's the imaging for this patient. On the far left, we see the diffusion-weighted image followed by the flare or fluid-attenuated inversion recovery image and the T2 image. The images, the flare, and the T2 they show us swelling on the brain. The diffusion shows us swelling in cells that we call cytotoxic edema. Diffusion-weighted images can show us strokes, but this white area in the right temporal lobe doesn't look like a stroke. 03:14 It doesn't follow a vascular territory. This is white on all the gray matter cells, all the cortical surface of the right temporal lobe. And we see edema on the flare and the T2 in that area. 03:27 This suggests some type of edematous, infectious, or inflammatory process going on in the temporal lobes. So again, what's the diagnosis? Is this a meningitis or an encephalitis? Is it a cerebritis or a brain abscess? Well we don't like meningitis. There's not meningeal signs. No neck stiffness, no meningismus, no Brudzinski or Kernig sign that show evidence of meningeal irritation. A cerebritis typically is a focal infection of the brain, patients present with headache, fever, and a focal neurologic deficit. This patient has a focal onset seizure, but this process sounds like a more generalized process in the brain and we would favor cerebritis or brain abscess less. This patient has a typical presentation for encephalitis. An initial viral prodrome with headache, maybe some low grade chills or fevers followed by generalized cortical dysfunction culminating in a seizure.
About the Lecture
The lecture Case: 61-year-old Man with Headache by Roy Strowd, MD is from the course CNS Infections.
Included Quiz Questions
Which of the following is consistent with the presentation of viral encephalitis?
- Seizure
- Positive Kernig's sign
- Flaccid lower limb paralysis
- Positive Brudzinski's sign
- Nuchal rigidity
Which of the following MRI findings is characteristic of viral encephalitis?
- Temporal lobe edema
- Basal ganglia calcification
- Periventricular calcification
- Discrete lesion with a thin enhancing rim
- Ventriculomegaly
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |