Playlist
Show Playlist
Hide Playlist
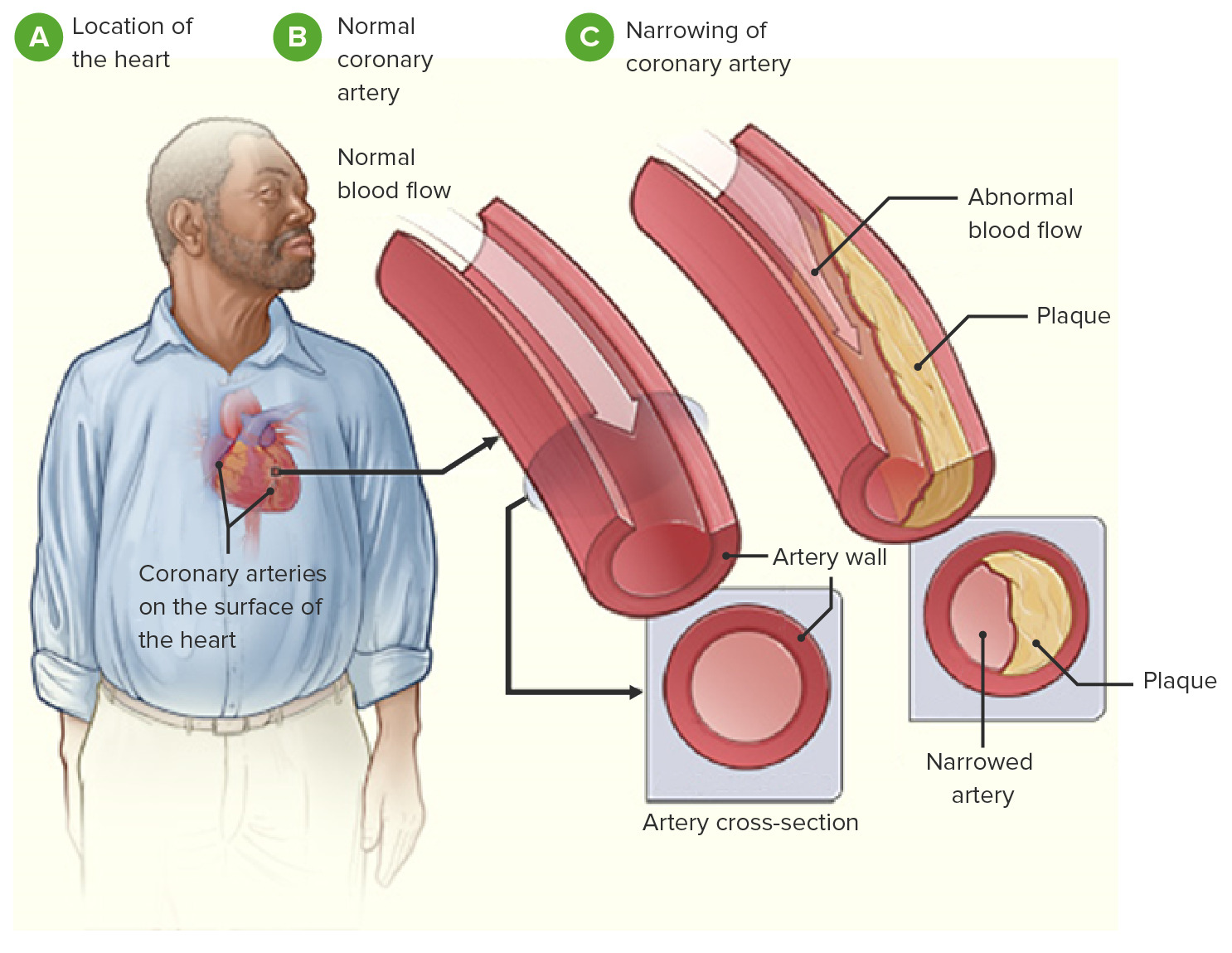
Atherosclerotic Cardiovascular Disease
-
Slides AtheroscleroticCardiovascularDisease ChronicCare.pdf
-
Download Lecture Overview
00:01 Let's talk about one of the most important and frightening diagnoses in primary care and that's atherosclerotic cardiovascular disease. 00:09 We have a case here to help set up our discussion. 00:12 You can see, ouch, my chest. 00:14 The patient is a 54-year-old male with a six-hour history of substernal chest pain which is constant. 00:20 It started after some heavy lifting and radiates up to his left shoulder. 00:24 Oh-oh! Let’s see. 00:26 He’s otherwise asymptomatic. 00:28 He has a history of obesity and hypertension, so a couple of cardiovascular risk factors there. 00:32 Plus, he’s a 54-year-old male. 00:34 That’s kind of in the sweet spot for getting typical angina symptoms. 00:40 So, what's the most important exam to order in the outpatient setting for this patient? Is it, A, chest radiography; B, an electrocardiogram; C, a serum creatinine kinase with an MB fraction; or D, serum troponin levels? Now, the answer is B, electrocardiogram. 01:01 This is the first step in the evaluation of most patients with chest pain beyond the history and physical examination. 01:08 But it does start with a history and physical. 01:10 And as the patient is describing the history of chest pain to me, I'm putting them in my mind in terms of how it corresponds with typical symptoms of angina and, therefore, their cardiac risk. 01:22 So, the type of pain with angina is usually a dull pressure. 01:27 So, that's a point against the patient unfortunately that they may have cardiac disease with that dull pressure. 01:34 Whereas a sharp pain or a more like lancinating pain like an electricity, those aren't often associated with angina or coronary artery disease and, therefore, that’s something that makes me think, oh good, this is not going to be coronary artery disease. 01:50 The duration of pain is important. 01:52 Most stable angina last for minutes and then disappears oftentimes associated with activity. 01:58 Patients just say, yeah, I get about two seconds. 02:00 It shoots through my chest and then it goes away. 02:03 Very unlikely angina. 02:04 And as well as a pain – yeah, it was there and it stayed from Sunday all the way through Tuesday. 02:10 36 hours of pain. 02:11 Also probably not angina. 02:14 Of course, with the angina, it’s going to be worse with physical activity, straining, particularly Valsalva where you’re really lifting and pulling something hard. 02:23 Alleviating factors, patients who say, like, well, I rub some cream on my chest and the pain goes away or I give myself a massage, I stretch out and it feels better, that's probably more musculoskeletal obviously than it would be angina and related to coronary artery disease. 02:41 Does the pain radiate anywhere? So, typical sites of radiation for angina include the shoulder, the arms, the jaw and the neck, that’s – and those are all concerning. 02:54 Sometimes with a musculoskeletal injury, like a bad injury over the lateral pectoral muscle, the shoulder might be involved too, but this is where it’s really kind of – with angina, it’s actually traveling over there, whereas in a musculoskeletal injury it’s just going to be a general soreness in this area. 03:11 And associated symptoms. 03:12 Musculoskeletal pain doesn't promote nausea, vomiting, numbness, tingling or diaphoresis. 03:20 And just to recall that musculoskeletal pain accounts for most patients with chest pain who present to primary care, musculoskeletal costochondritis. 03:30 Angina is actually pretty rare. 03:32 Also remember that there is a difference between sexes on this issue. 03:37 So, stable angina and angina symptoms are much more commonly encountered among men, although women have a higher rate of atherosclerotic cardiovascular disease overall. 03:52 And their disease among women is generally more deadly, partly because they don’t have typical symptoms that men have that show that there is an incipient event coming. 04:03 So, women will just present – they are more likely to present with a myocardial infarction as opposed to having stable angina or something they could have done about it prior to it becoming a critical situation where the heart has ischemia. 04:18 So, again, thinking back to the history and risk stratification, family history does count. 04:23 So, do take a family history of other cardiovascular events. 04:26 Past medical history certainly counts. 04:28 Do they have some of the big diagnoses that are known to promote a history of cardiac disease, diabetes, hypertension, hyperlipidemia? Are they smoking? Are they obese? And then looking at serum lipids is probably the most important lab. 04:46 If I have to flip through something to evaluate, okay, what is their risk stratification, lipids are the one lab value I’d hold on to more than any other.
About the Lecture
The lecture Atherosclerotic Cardiovascular Disease by Charles Vega, MD is from the course Chronic Care.
Included Quiz Questions
Which of the following is a LEAST characteristic of angina?
- Chest pain described as sharp
- Chest pain described as pressure
- Chest pain that lasts for several minutes
- Chest pain that radiates to the shoulder or arm
- Chest pain that is associated with numbness and tingling
Which of the following types of patients are more likely to present with atypical angina?
- Female, diabetic, and old
- Male, diabetic, and old
- Female, nondiabetic, and young
- Male, diabetic, and young
- Male, nondiabetic, and old
Which of the following is the initial investigation in a patient who presents with angina?
- Electrocardiogram
- Cardiac troponin
- Echocardiogram
- Chest X-ray
- Exercise electrocardiogram
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |